
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
BRIEF RESEARCH REPORT article
Front. Psychol. , 03 April 2025
Sec. Psychology for Clinical Settings
Volume 16 - 2025 | https://doi.org/10.3389/fpsyg.2025.1411908
Introduction: As social relationships are intertwined with mental health recovery, it is important to address a client’s social support network during mental health interventions. This seems even more important for autistic clients, because research suggests they have on average smaller networks and experience more loneliness than non-autistic individuals. Therefore, an interview assessing the social support network in relation to intervention goals was co-created together with stakeholders (autistic clients, mental healthcare professionals and a mother of an autistic client). In addition, the psychometric properties and acceptability of this Network-in-Action-Interview (NiA-I) were studied as pre-registered (AsPredicted #59767).
Methods: The Nominal Group Technique was used to co-create the NiA-I with stakeholders and it was administered to autistic clients (n = 44) recruited in a highly specialized mental health facility.
Results: Network-in-Action-Interview social support scores were significantly correlated with the Multidimensional Scale of Perceived Social Support, indicating sufficient convergent validity. Clients and professionals reported that the NiA-I provided the therapist with greater insight into the client’s social support network. Professionals reported the NiA-I could be improved regarding administration duration.
Discussion: This cross-sectional study shows that the NiA-I is a solid and helpful tool for including the social network in clinical practice. Addressing and including a client’s social support network is important for recovery-focused mental health treatment. The NiA-I can assist professionals in taking such actions.
A person’s social support network can either promote or hinder recovery from mental health problems (Reupert et al., 2015). For example, on the one hand having meaningful social connections is one of the core aspects of personal recovery (Tew et al., 2012), while on the other hand distancing oneself from certain others who are disempowering or overprotective can also promote recovery (Reupert et al., 2015). Therefore, it is important to pay attention to a client’s social support network during mental health interventions and how this support relates to the individual’s intervention goals. In this study, we focus on developing and studying a co-created interview that assesses social support aspects in relation to intervention goals.
Regarding social support, autistic individuals appear more vulnerable. For example, autistic adults experience more loneliness (Moseley et al., 2021; Tobin et al., 2014) and lower levels of social support (e.g., Moseley et al., 2021) compared to non-autistic individuals, with the latter being associated with lower quality of life (Charlton et al., 2022). Moreover, wishes related to their social networks were reported by the majority of autistic adults recruited via a mental health facility (van den Heuvel et al., 2022). This strengthens the need of considering the social support network during mental health interventions in autistic individuals, a group known to have an elevated prevalence of mental health problems such as depression and anxiety disorders (Hollocks et al., 2019; Hudson et al., 2019).
However, social network interventions are not a one-size-fits-all solution, as everyone has different needs which differ along the journey of recovery (Tew et al., 2012). Using a social network mapping tool can assist the mental healthcare professional and the autistic individual in discovering collaboratively what could help the client regarding their network in several ways. For example, social network mapping can help to gain a broader understanding of the client’s daily life including their social interactions (Brooks et al., 2022). Also, it opens a conversation to empower the client (Sweet et al., 2018) which suits within a contextual-focused, recovery-oriented mental healthcare. In addition, such a tool facilitates the identification of strengths and resources within one’s social environment (Tew et al., 2012), which might serve as a first step in assisting clients to mobilize support within their network. Lastly, it can help in identifying suitable network members for involvement during mental health interventions, which is associated with better client-reported intervention outcomes and higher satisfaction with care in clients with psychiatric conditions (Svendsen et al., 2021).
Based on these arguments plus a lack of suitable existing instruments for clinical practice, we developed the Network in Action-Questionnaire (NiA-Q) (van den Heuvel et al., 2022). This is a digital questionnaire assessing both functional (e.g., perceived social support and interpersonal distress) and structural aspects (e.g., network size) of the social support network. These aspects are assessed in relation to the individual’s treatment goals, so the information from the NiA-Q is directly applicable to the individual’s mental health intervention. Therefore, it is expected this instrument will be more suitable for use in clinical practice compared to other instruments that lead to a more general impression of someone’s social network. However, using the NiA-Q in clinical practice revealed that both clients and professionals encountered some challenges. That is, some clients considered their social network a too sensitive topic for an anonymous, digital questionnaire without the opportunity to discuss this directly with their practitioner. In addition, the professionals missed opportunities to respond to the client’s needs, for example, by explaining if something was unclear or by asking further questions on specific topics to gather as much relevant information as possible.
Therefore, in this study, we transformed the NiA-Q into an interview version, the Network in Action-Interview (NiA-I), in collaboration with stakeholders using a structural group technique. In addition, this study investigated (1) the first psychometric properties of the newly developed NiA-I; and (2) the acceptability of the instrument to autistic clients and professionals.
Throughout the study, a project group was involved consisting of two autistic clients, a mother of an autistic client and five healthcare professionals from diverse backgrounds working in an autism mental healthcare center. They provided input during the development of the NiA-I, on recruitment strategies, and on content of the acceptability measures.
The development process of the NiA-I consisted of three steps. In the first step, the NiA-Q (van den Heuvel et al., 2022), was transformed into a first draft version by the researchers. A limited number of questions that were considered relevant based on literature on social network concepts were added. For example, a question about the relationships between network members was added to the interview to obtain a measure of network density. Next, this version was presented to the project group using the Nominal Group Technique (NGT; Delbecq and Van de Ven, 1971; McMillan et al., 2014) during an online meeting (duration: 120 min). NGT facilitates the generation of ideas about a specified topic, by structuring group discussion in four phases to reach a collaborative decision (McMillan et al., 2016). NGT minimizes possible adverse effects of intragroup dynamics and encourages openness and contributions from all group members (Hatch et al., 2021). The researchers participated as facilitators. Following NGT procedure, during the Silent Generation phase, all members silently wrote down their suggestions for modifications to the proposed interview. Subsequently, during the Round Robin phase, members named their suggestions. In the Clarification phase, members could discuss and group double or overlapping suggestions. The last phase, Ranking, was conducted by e-mail: all members voted for each suggestion whether they considered this a useful suggestion or not. Votes from the autistic individuals and the mother of an autistic client counted double to create more balance in the votes of clinical professionals versus experts by experience. Suggestions that more than half of the group voted as being beneficial were implemented by the researchers in a new version of the NiA-I.
In the second step, the NiA-I as it emerged from the NGT meeting was presented to other professionals (n = 10) and autistic clients (n = 4) in individual feedback sessions with a researcher (duration: 45 min). Participants were asked how item wording could be improved and what topics were missing.
In the third step, feedback gathered in the second step was presented to the project group in a second NGT session (duration: 120 min). Therefore, the Silent Generation and Round Robin phases were not applicable. Clarification and Ranking phases proceeded in the same manner as the first NGT session, resulting in a version of the NiA-I that was pilot tested by four autistic clients and their therapists. Based on their experiences, final adjustments were made to the NiA-I in consultation with the project group. Examples of adjustments were changes in the order of questions and improvements in layout. Also, the suggestion for therapists to look up some information (i.e., on treatment goals and current care providers) before interview administration was added, as this decreased the administration time and load to clients. See Table 1 of the topics covered in the final version of the NiA-I. As part of the interview, participants make a sociogram of their current and desired situation regarding their social network. The network members are placed in one of four concentric circles around the client, with the innermost circle representing the most supportive or significant individuals. This structure helps to visualize the perceived closeness or importance of each network member and desired changes.
All autistic clients and their therapists were recruited via a highly specialized autism mental health facility in Netherlands. The client population is characterized by having co-occurring conditions besides a clinical diagnosis of an autism spectrum disorder (ASD) and they have often had previous treatment that was unsuccessful. Data collection took place in 2021 and 2022. Inclusion criteria for the autistic individuals were (1) ASD diagnosis based on DSM-5 (American Psychiatric Association, 2013); (2) being a client of the specialized autism center; and 3) aged 14 years or older. There were no specific inclusion criteria for therapists.
The study was classified as not falling under the Dutch Act on Medical Research Involving Human Subjects (WMO) (reference number W20_358 # 20.397) by the Medical Ethics Committee of Amsterdam University Medical Center, and was approved by the Ethics Committee of the Psychology Department of the University of Amsterdam (2020-EXT-12318; 2021-EXT-13059). Recruitment took place through multiple strategies: clients were asked to participate either (1) by their therapist during treatment, who approached clients they deemed eligible; (2) by a therapist after the intake procedure; (3) by the researcher in a therapeutic group meeting. The NiA-I was administered by either a therapist of the client as part of ongoing treatment (n = 19) or the researcher (n = 25). The interview was conducted face-to-face (n = 41), online (n = 2) or mixed (n = 1) in one or two sessions. The administration of the NiA-I lasted between 30 and 120 min (M = 69.9; SD = 25.6; median = 60), with 5–30 min (M = 17.2; SD = 9.5; median = 15) of preparation time for the professional. The client and therapist completed the acceptability measure directly after NiA-I administration. The client completed the Multidimensional Scale of Perceived Social Support (MSPSS), Autism Quotient (AQ) and Social-Responsiveness Scale (SRS) via a secured online platform within the following week.
The NiA-I consisted of nine main questions on various aspects of the social network, which were divided into sub-questions (see Table 1). Of these, question 3 assesses perceived social support through a quantitative score. The scores of the sub-questions of question 3 were averaged to determine a NiA-I social support score that is used for analyses of convergent validity and internal consistency. In this question, four aspects of social support were asked for a maximum of three separate treatment goals. If clients had fewer than three current goals, the four items were answered only for these goals. Answers were scored on a five-point scale (1 = not at all; 5 = very much) or as “not applicable.” The NiA-I is freely available upon request from the first author (NB the instrument is in Dutch). No additional training is needed prior to administration by a clinical professional.
The MSPSS (Zimet et al., 1988) measures the perceived level of social support from friends, family and significant other/special person. It consists of 12 items measured on a seven-point scale. Higher scores indicate a higher level of social support. The psychometric properties of the MSPSS have been demonstrated in a range of studies, including its reliability and validity of the Dutch version (Pedersen et al., 2009) and in both adolescent and adult samples (e.g., Bruwer et al., 2008; Zimet et al., 1990).
To measure client’s and therapist’s experience with the NiA-I, we developed acceptability ratings with the project group. The five-item client-version and the six-item therapist-version largely overlapped in content (see Table 3) and both versions were measured on a five-point scale (1 = very strongly disagree; 5 = very strongly agree).
Depending on the participant’s age, the caregiver-report SRS-2 (Constantino and Gruber, 2005) or its adult version, the self-report SRS-A (Constantino, 2002), was used. It measures autistic traits in 64 (SRS-A) or 65 (SRS-2) items, which are answered on a four-point Likert scale and lead to scores between 0 and 3. The total scores range from 0 to 192 for SRS-A and from 0 to 195 for SRS-2. Higher scores indicate more autism traits. We used the cut-off score of 57 for the SRS-2 and 54 for the SRS-A. Mean scores for non-autistic people have shown to range between 37.7 and 76.5 (Bezemer et al., 2020). The validity and reliability of the Dutch version of the SRS-2 and SRS-A have shown to be adequate (Noens et al., 2012; Roeyers et al., 2011). The SRS-2/SRS-A score was used for descriptive purposes and for subgroup analyses, see section “2.6 Data analysis.”
The AQ (Baron-Cohen et al., 2001; Hoekstra et al., 2008) measures characteristics indicative for autism with a cut-off score of 32. It consists of 50 items answered on a four-point Likert scale. A higher score indicates more autism characteristics. Answers are dichotomized into 0 (not indicative of ASD) or 1 (indicative of ASD) (Baron-Cohen et al., 2001), leading to a possible score range of 0–50. Mean scores for non-autistic people have shown to range between 16.4 and 22.2 in the general population and between 20.9 and 33.1 in psychiatric samples (Bezemer et al., 2020). The Dutch version of the AQ is reliable and valid (Hoekstra et al., 2008). The AQ score was used for descriptive purposes and for subgroup analyses, see section “2.6 Data analysis.”
Only in three of 19 NiA-I takings by therapists (16%) audio recording succeeded. Therefore, the recordings were not formally evaluated. No problems with administration occurred in these three recordings. Additionally, no problems were reported by clients or therapists during other, non-recorded administrations, nor did clients express objections to specific items.
The study design and analyses were pre-registered on AsPredicted (#597671). To investigate convergent validity, Pearson correlation between the NiA-I question 2 mean score and MSPSS mean score was calculated. Both a frequentist approach (i.e., leading to a p-value) in R Core Team (2017) and Bayesian statistics in JASP version 0.13.1 (JASP Team, 2020) were applied. For the latter, the prior was kept at the default (i.e., 0.707). We report the Bayes Factor10 (BF10), which indicates the probability that the alternative hypothesis is true compared to the null hypothesis. The correlation analysis was repeated including only participants scoring above either the AQ cut-off (i.e., 32) or SRS-2 (i.e., 57)/SRS-A cut-off (i.e., 54) to check whether this changed the results. In addition to the correlation analysis, a Bland–Altman plot was used to inspect systematic differences across the range of scores (Bland and Altman, 1986), such as whether differences in scores tend to occur at lower or higher score ranges. First, the NiA-I and MSPSS scores were transformed into z-scores to enable cross-measure comparison. Second, the difference value of each NiA-I-MSPSS pair was plotted on the y-axis and the mean value for each NiA-I-MSPSS rating pair was plotted on the x-axis. A positive mean difference score indicates a pair where the NiA-I score is higher than the MSPSS value.
Internal consistency for the social support scores of the NiA-I was presented in Cronbach’s alpha. Since some participants had less than three treatment goals and not applicable was a valid answer option if a social support aspect did not apply to a certain intervention goal, we followed the procedure described by Arifin (2018) that takes not applicable answer options into account.
Acceptability ratings of clients and professionals were presented in descriptive statistics. As professionals could administer the NiA-I for multiple clients and therefore complete the acceptability measure multiple times, we calculated intraclass correlations (ICC) for the ratings of professionals.
Lastly, we briefly describe the responses on the final, open-ended question of the NiA-I for explorative purposes.
As pre-registered, 44 clients participated in the study. Clients were between 14 and 58 years old (M = 23.8, SD = 8.8). Regarding gender, 17 (38.6%) clients identified as female, 25 (56.8%) as male and two (4.5%) as other. See for further characteristics Table 2.
Social support items on the NiA-I and MSPSS were moderately positively correlated, r(31) = 0.36, p = 0.042, BF10 = 1.57. The Bayes factor indicates anecdotal evidence that the two scores are correlated (Wagenmakers et al., 2011). Conform pre-registration, we planned to repeat the correlation analysis with solely those participants scoring above cut-off score on either AQ or SRS-2/SRS-A. However, no participants had to be excluded based on this restriction. The Bland-Altman plot showed no systematic differences across the range of social support scores of the NiA-I and MSPSS (see Figure 1).
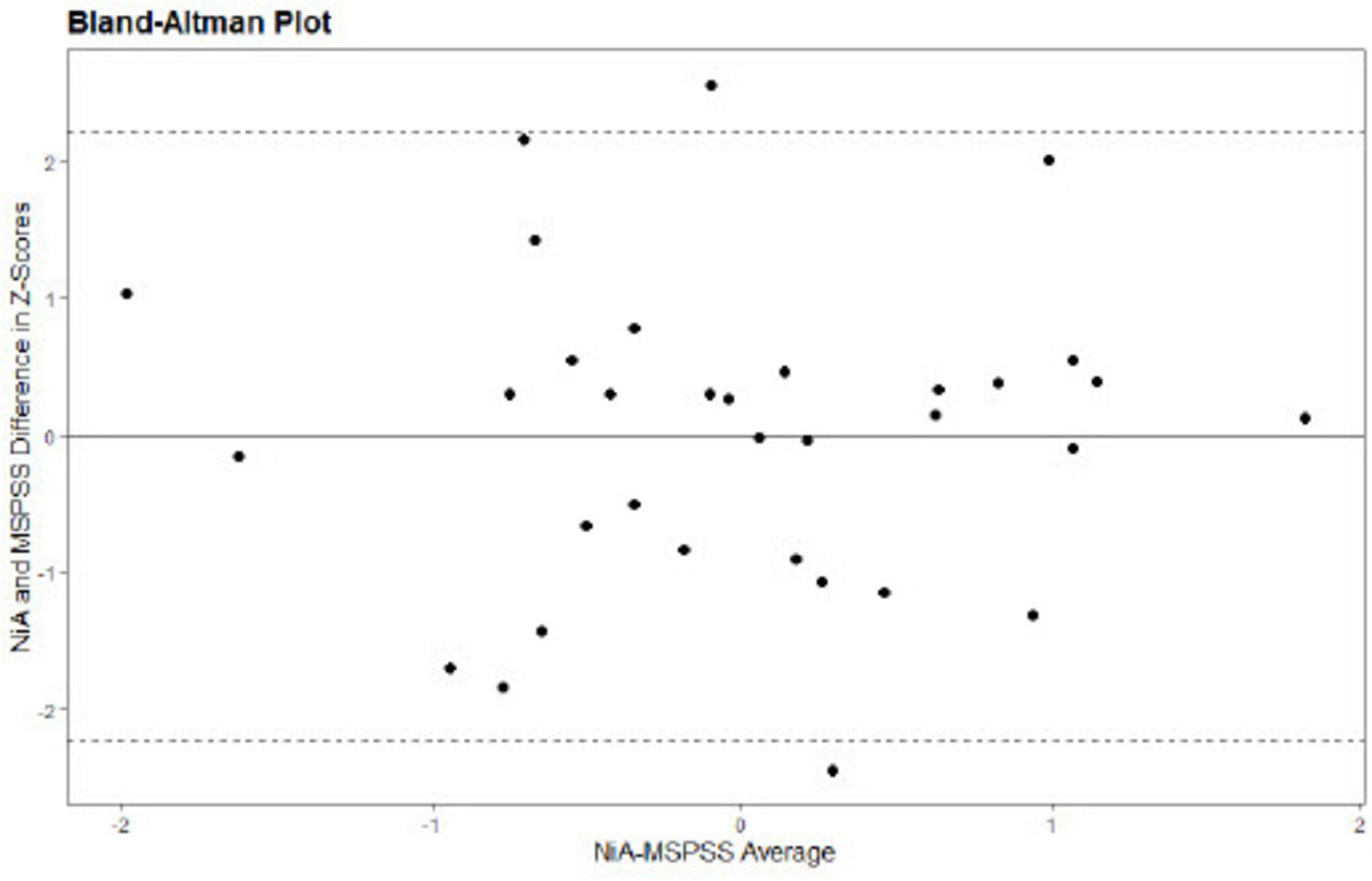
Figure 1. Bland-Altman plot shows no systematic differences between Network in Action-Interview and Multidimensional Scale of Perceived Social Support Scale.
The social support items of the NiA-I had a good internal consistency (Evers et al., 2009), α = 0.85.
Acceptability ratings of clients and professionals are presented in Table 3. As three professionals participated two or three times, ICCs were calculated (see Table 3). For three items (i.e., duration, clarity of questions, and compatibility with clinical practice) ICCs showed that all variance could be attributed to variance between different raters, so the professionals who participated more than once were consistent in their scoring across clients. For the other items, ratings of professionals varied when they administered the NiA-I to multiple clients.
In order to obtain qualitative information, we examined the open-ended, final question of the NiA that asked clients what they thought was the most important topic discussed during the interview. Around a quarter of participants (n = 12) described their desired changes regarding their social network as the most important topic. Some clients (n = 6, 14%) explicitly referred to the network circles of question 2 and 9 and how it helped to formulate their wishes:
“Placing people in the circle (from step 2). I realized that I feel I have to approach everyone in the same way and meet all their expectations, but this may not be as necessary with people who are a bit more distant from me.” (23 years-old woman)
Other participants (n = 9, 20%) mentioned that answering concrete questions about their network provided them with insight:
“It’s kind of unusual to look at my network in such a focused way. But it gives me a different angle and helps me think about it more broadly” (23 years-old man)
Other examples of insights or topics that clients referred to in their answers to this question are:
“The question about who you want to involve; I would like my parents to listen to me more when I am struggling with something.” (21 years-old woman)
“The most important thing: family comes first. I also want to evaluate each of my contacts to see whether it drains or gives me energy.” (40 years-old man)
“I thought at first that I’d need to find people, but there are already enough people I can go to.” (21 years-old man)
Eight clients (18%) did not answer this question.
The purpose of this study was to co-create an interview based on the NiA-Q (van den Heuvel et al., 2022) with various stakeholders so that clinicians could use it to gain insight into an autistic client’s social support network. The results indicate that the NiA-I is a sufficiently valid, reliable, and acceptable instrument to assess the social support network in clinical practice in autistic individuals.
The results of acceptability ratings from clients and professionals showed that the NiA-I was considered relevant by the majority of both clients and therapists. Still, we have two suggestions to increase the usefulness of the NiA-I. First, it would be interesting to further explore the characteristics of clients for whom the NiA-I might be most beneficial, in order to better predict to whom and when this instrument is indicated. Second, the perceived usefulness for clients could be improved by adding a more comprehensive explanation of how the social support system can contribute to mental health recovery so that individuals could more easily relate the NiA-I outcomes to their own situation.
The NiA-I provided the therapist with more insight into the client’s social support network, which is an important goal of the instrument. However, the acceptability ratings of professionals also indicated that the NiA-I could be improved regarding administration duration and how the interview fits within current clinical practice. Therefore, shortening the NiA-I could be considered in future research, allowing the professional and/or client to choose between a full or shortened version based on the individual’s needs.
The convergent validity analysis indicates that the NiA-I and MSPSS (Zimet et al., 1988) social support scores are sufficiently associated but do also differ. A first explanation is that the MSPSS might focus more on emotional aspects of social support than on concrete or informational support, as previously noted by others (Tracy and Whittaker, 1990), whereas the NiA-I explicitly asks about both emotional, informational and practical support in relation to intervention goals. Although there were several reasons to choose for the MSPSS in this study (e.g., good psychometric properties, a validated Dutch version, suitable for use in both adolescents and adults), the difference in broadness of included social support features in the two measures could explain the moderate correlation.
However, another explanation is that social support related to intervention goals is considerably different from the construct of general social support, which is one of the reasons why the NiA-I was developed in the first place. For example, not all network members perceived as supportive in general are relevant for certain intervention goals. This leads to the more fundamental question of which aspects within the broad concept of social support contribute most to mental health recovery (Priebe et al., 2014), which might even be different for autistic individuals. Social interactions and subjective social support appeared related to psychological health aspects of quality of life in autistic adults, but not instrumental social support (Charlton et al., 2022). Future studies should explore such influences on mental health recovery in autistic adults, so that we can better understand which aspect of social support we can try to act on to improve outcomes for autistic individuals, a group with high prevalence of mental health problems (Hollocks et al., 2019; Hudson et al., 2019).
An advantage of the NiA-I is that it supports the strong motivation of clinicians2 to include the social network of an autistic client. Moreover, the tool offers a practical solution to working network- and recovery-oriented, for example, by incorporating it into a mental healthcare team’s working routine. This is relevant for practice, because research on family involvement in mental healthcare has pointed at the role of organizational policy and working routine for successful implication (Eassom et al., 2014; see text footnote 2).
Besides assisting professionals in using a network-oriented approach during mental health interventions, there are at least two other specific applications of the NiA-I. First, the information resulting from the NiA-I can provide a starting point for a personalized social support intervention. Social support interventions for persons with mental health problems are effective only if they have a personalized approach (Beckers et al., 2022), so if they take into account the needs of the individual client as is done with the NiA-I. The finding that social support interventions are effective is promising, because these have been suggested as an approach to increase wellbeing in autistic individuals (Bishop-Fitzpatrick et al., 2018; Moseley et al., 2021). As a second application, the NiA-I can help the client nominate members of a resource group (Nordén et al., 2012): a client-chosen group of key network members and professionals that meets regularly and supports the achievement of the client’s goals. Further research can explore what role the NiA-I can play in these two applications.
There are some limitations to keep in mind when interpreting the results of this study. First of all, this study included a relatively limited number of participants, so the psychometric properties of the NiA-I should also be evaluated in a larger sample. Future studies could assess other psychometric properties besides convergent validity and internal consistency. An interesting avenue for further research would be to explore predictive validity, for instance, by examining whether NiA-I scores are associated with recovery progress or perceived loneliness over time. A second limitation is that participants were not randomly selected, but were approached if their therapist expected a NiA-I to be relevant to them or if the client was interested in participating. This might have influenced the acceptability results. However, a nuance here is that a clinician in regular clinical practice will also first make a clinical judgment before administering the NiA-I to a client.
Strengths of the study are that different types of stakeholders were involved in the development of the interview. Additionally, we used a structured group approach in the development process using NGT (Delbecq and Van de Ven, 1971), which encouraged all participants of the project group to give their input in an equal manner.
To conclude, it is important to provide attention to social support and involve the social network during mental health interventions, especially in autistic clients given vulnerabilities in this area. The NiA-I provides a tool to practically implement this aim into the clinical working routine, resulting in greater understanding of wishes, needs and opportunities within the client’s social support network for both therapist and client.
The datasets presented in this article are not readily available because they involve privacy-sensitive data that may be identifiable to individuals. Requests to access the datasets should be directed to RMvdH, ci52YW5kZW5oZXV2ZWxAbGVva2FubmVyaHVpcy5ubA==.
The studies involving humans were approved by Ethics Committee of the Psychology Department of the University of Amsterdam (2020-EXT-12318; 2021-EXT-13059). The study was classified as not falling under the Dutch Act on Medical Research Involving Human Subjects (WMO) (reference number W20_358 # 20.397) by the Medical Ethics Committee of Amsterdam University Medical Center. The studies were conducted in accordance with the local legislation and institutional requirements. Written informed consent for participation in this study was provided by the participants or the participants’ legal guardians/next of kin.
RMvdH: Conceptualization, Formal Analysis, Investigation, Writing – original draft. HMG: Conceptualization, Writing – review and editing. MW: Conceptualization, Writing – review and editing. J-PT: Conceptualization, Writing – review and editing.
The author(s) declare that no financial support was received for the research and/or publication of this article.
Study design and analyses were pre-registered at AsPredicted (#59767; https://aspredicted.org/5CS_Q32). Data, materials and analysis code are available from the first author upon request. We thank the participants for their time and effort in participating in the study. We are also grateful to our project group for their contributions to the study.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders: DSM-5. Washington, DC: American Psychiatric Association.
Arifin, W. N. (2018). Calculating the Cronbach’s alpha coefficients for measurement scales with ‘not applicable’ Option. Pulau Pinang: Universiti Sains Malaysia. doi: 10.13140/RG.2.2.16955.87843
Baron-Cohen, S., Wheelwright, S., Skinner, R., Martin, J., and Clubley, E. (2001). The Autism-Spectrum Quotient (AQ): Evidence from asperger syndrome/high-functioning autism, malesand females, scientists and mathematicians. J. Autism Dev. Disord. 31, 5–17. doi: 10.1023/A:1005653411471
Beckers, T., Maassen, N., Koekkoek, B., Tiemens, B., and Hutschemaekers, G. (2022). Can social support be improved in people with a severe mental illness? A systematic review and meta-analysis. Curr. Psychol. 42, 14689–14699. doi: 10.1007/s12144-021-02694-4
Bezemer, M. L., Blijd-Hoogewys, E. M. A., and Meek-Heekelaar, M. (2020). The Predictive Value of the AQ and the SRS-A in the diagnosis of ASD in adults in clinical practice. J. Autism Dev. Disord. 51, 2402–2415. doi: 10.1007/s10803-020-04699-7
Bishop-Fitzpatrick, L., Mazefsky, C. A., and Eack, S. M. (2018). The combined impact of social support and perceived stress on quality of life in adults with autism spectrum disorder and without intellectual disability. Autism 22, 703–711. doi: 10.1177/1362361317703090
Bland, J. M., and Altman, D. G. (1986). Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 327, 307–310.
Brooks, H., Devereux-Fitzgerald, A., Richmond, L., Bee, P., Lovell, K., Caton, N., et al. (2022). Assessing the effectiveness of social network interventions for adults with a diagnosis of mental health problems: A systematic review and narrative synthesis of impact. Soc. Psychiatry Psychiatr. Epidemiol. 57, 907–925. doi: 10.1007/s00127-022-02242-w
Bruwer, B., Emsley, R., Kidd, M., Lochner, C., and Seedat, S. (2008). Psychometric properties of the multidimensional scale of perceived social support in youth. Compr. Psychiatry 49, 195–201. doi: 10.1016/j.comppsych.2007.09.002
Charlton, R. A., McQuaid, G. A., and Wallace, G. L. (2022). Social support and links to quality of life among middle-aged and older autistic adults. Autism 27, 92–104. doi: 10.1177/13623613221081917
Constantino, J. N. (2002). The Social Responsiveness Scale—Adult Version. Torrance, CA: Western Psychological Services.
Constantino, J. N., and Gruber, C. P. (2005). The Social Responsiveness Scale Manual. Torrance, CA: Psychological Services.
Delbecq, A. L., and Van de Ven, A. H. (1971). A group process model for problem identification and program planning. J. Appl. Behav. Sci. 7, 466–492. doi: 10.1177/002188637100700404
Eassom, E., Giacco, D., Dirik, A., and Priebe, S. (2014). Implementing family involvement in the treatment of patients with psychosis: A systematic review of facilitating and hindering factors. BMJ Open 4:e006108. doi: 10.1136/bmjopen-2014-006108
Evers, A., Lucassen, W., Meijer, R., and Sijtsma, K. (2009). COTAN beoordelingssysteem voor de kwaliteit van tests (geheel herziene versie). Amsterdam: NIP.
Hatch, M. R., Carandang, K., Moullin, J. C., Ehrhart, M. G., and Aarons, G. A. (2021). Barriers to implementing motivational interviewing in addiction treatment: A nominal group technique process evaluation. Implement. Res. Pract. 2:26334895211018400. doi: 10.1177/26334895211018400
Hoekstra, R. A., Bartels, M., Cath, D. C., and Boomsma, D. I. (2008). Factor structure, reliability and criterion validity of the Autism-Spectrum Quotient (AQ): A study in Dutch population and patient groups. J. Autism Dev. Disord. 38, 1555–1566. doi: 10.1007/s10803-008-0538-x
Hollocks, M. J., Lerh, J. W., Magiati, I., Meiser-Stedman, R., and Brugha, T. S. (2019). Anxiety and depression in adults with autism spectrum disorder: A systematic review and meta-analysis. Psychol. Med. 49, 559–572. doi: 10.1017/S0033291718002283
Hudson, C. C., Hall, L., and Harkness, K. L. (2019). Prevalence of depressive disorders in individuals with autism spectrum disorder: A meta-analysis. J. Abnorm. Child Psychol. 47, 165–175. doi: 10.1007/s10802-018-0402-1
JASP Team (2020). JASP (Version 0.13.1)[Computer software]. Available online at: https://jasp-stats.org/2020/07/21/jasp-0-13-1-small-fixes/ (accessed July 21, 2020).
McMillan, S. S., Kelly, F., Sav, A., Kendall, E., King, M. A., Whitty, J. A., et al. (2014). Using the Nominal Group Technique: How to analyse across multiple groups. Health Serv. Outcomes Res. Methodol. 14, 92–108. doi: 10.1007/s10742-014-0121-1
McMillan, S. S., King, M., and Tully, M. P. (2016). How to use the nominal group and Delphi techniques. Int. J. Clin. Pharm. 38, 655–662. doi: 10.1007/s11096-016-0257-x
Moseley, R. L., Turner-Cobb, J. M., Spahr, C. M., Shields, G. S., and Slavich, G. M. (2021). Lifetime and perceived stress, social support, loneliness, and health in autistic adults. Health Psychol. 40, 556–568. doi: 10.1037/hea0001108
Noens, I., Steyaert, J., De la Marche, W., and Scholte, E. (2012). Handleiding SRS-A—Screeningslijst Voor Autismespectrumstoornissen [SRS-A Social Responsiveness Scale, Professional Manual]. Stockholm: Hogrefe.
Nordén, T., Malm, U., and Norlander, T. (2012). Resource Group Assertive Community Treatment (RACT) as a tool of empowerment for clients with severe mental illness: A meta-analysis. Clin. Pract. Epidemiol. Ment. Health 8, 144–151. doi: 10.2174/1745017901208010144
Pedersen, S. S., Spinder, H., Erdman, R. A. M., and Denollet, J. (2009). Poor perceived social support in implantable cardioverter defibrillator (ICD) patients and their partners: Cross-validation of the multidimensional scale of perceived social support. Psychosomatics 50, 461–467. doi: 10.1016/S0033-3182(09)70838-2
Priebe, S., Omer, S., Giacco, D., and Slade, M. (2014). Resource-oriented therapeutic models in psychiatry: Conceptual review. Br. J. Psychiatry 204, 256–261. doi: 10.1192/bjp.bp.113.135038
R Core Team (2017). R: A Language and Environment for Statistical Computing. Vienna: R Foundation for Statistical Computing.
Reupert, A., Maybery, D., Cox, M., and Scott Stokes, E. (2015). Place of family in recovery models for those with a mental illness. Int. J. Ment. Health Nurs. 24, 495–506. doi: 10.1111/inm.12146
Roeyers, H., Thys, M., Druart, C., De Schryver, M., and Schittekatte, M. (2011). Screeninglijst Voor Autismespectrumstoornissen (SRS) Handleiding. Stockholm: Hogrefe uitgevers.
Svendsen, M. L., Ellegaard, T., Jeppesen, K. A., Riiskjær, E., and Nielsen, B. K. (2021). Family involvement and patient-experienced improvement and satisfaction with care: A nationwide cross-sectional study in Danish psychiatric hospitals. BMC Psychiatry 21:190. doi: 10.1186/s12888-021-03179-1
Sweet, D., Byng, R., Webber, M., Enki, D. G., Porter, I., Larsen, J., et al. (2018). Personal well-being networks, social capital and severe mental illness: Exploratory study. Br. J. Psychiatry 212, 308–317. doi: 10.1192/bjp.bp.117.203950
Tew, J., Ramon, S., Slade, M., Bird, V., Melton, J., and Le Boutillier, C. (2012). Social factors and recovery from mental health difficulties: A review of the evidence. Br. J. Soc. Work 42, 443–460. doi: 10.1093/bjsw/bcr076
Tobin, M. C., Drager, K. D. R., and Richardson, L. F. (2014). A systematic review of social participation for adults with autism spectrum disorders: Support, social functioning, and quality of life. Res. Autism Spectr. Disord. 8, 214–229. doi: 10.1016/j.rasd.2013.12.002
Tracy, E. M., and Whittaker, J. K. (1990). The social network map: Assessing social support in clinical practice. Fam. Soc. 71, 461–470. doi: 10.1177/104438949007100802
van den Heuvel, R. M., Wensing, M., Geurts, H. M., and Teunisse, J.-P. (2022). The social support network of adults with an autism spectrum condition: An exploration using the network in action-questionnaire. J. Autism Dev. Disord. 53, 1974–1988. doi: 10.1007/s10803-022-05467-5
Wagenmakers, E. J., Wetzels, R., Borsboom, D., and van der Maas, H. L. (2011). Why psychologists must change the way they analyze their data: The case of Psi: Comment on Bem (2011). J. Pers. Soc. Psychol. 100, 426–432. doi: 10.1037/a0022790
Zimet, G. D., Dahlem, N. W., Zimet, S. G., and Farley, G. K. (1988). The multidimensional scale of perceived social support. J. Pers. Assess. 52, 30–41. doi: 10.1207/s15327752jpa5201_2
Keywords: autism, adults, mental healthcare, social network, social support
Citation: van den Heuvel RM, Geurts HM, Wensing M and Teunisse J-P (2025) Measuring the social support network in autistic clients: development and validation of the Network in Action-Interview. Front. Psychol. 16:1411908. doi: 10.3389/fpsyg.2025.1411908
Received: 03 April 2024; Accepted: 17 March 2025;
Published: 03 April 2025.
Edited by:
Gianluca Castelnuovo, Catholic University of the Sacred Heart, ItalyReviewed by:
Catherine Caldwell-Harris, Boston University, United StatesCopyright © 2025 van den Heuvel, Geurts, Wensing and Teunisse. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Rinske M. van den Heuvel, ci52YW5kZW5oZXV2ZWxAbGVva2FubmVyaHVpcy5ubA==
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.