- 1American University of the Caribbean School of Medicine, Cupecoy, Sint Maarten
- 2Graduate College of Biomedical Sciences and College of Dental Medicine, Western University of Health Sciences, Pomona, CA, United States
Despite many initiatives over more than 4 decades, the diversity of United States physicians still does not reflect the diversity of the United States population. The present study undertakes a literature review of the last 30 years to investigate barriers and protective factors underrepresented college students encounter as applicants for medical school. Known barriers that influence matriculation into medical school were analyzed such as academic metrics and test scores. Additionally, elements that are less well studied were investigated such as factors perceived as barriers by underrepresented applicants in addition to protective factors that allow them to persist in their journey in the face of difficulties and adversity.
Introduction
It has been known for many years that the United States is facing a significant physician shortage in particular in the primary care field (Zhang et al., 2020; Association of American Medical Colleges, 2021c) and this has been exacerbated by the COVID-19 pandemic (Dill, 2021; Frogner and Dill, 2022). Furthermore, there is a continuing inequity between the diversity of healthcare providers and population trends in the United States. In the 1960s, the importance of these provider inequities was first investigated and the federal government along with organizations such as the Association of American Medical College (AAMC) eventually created initiatives and programming to expose and prepare underrepresented populations for careers in healthcare (Petersdorf, 1992; Nickens et al., 1994; Hayes-Bautista et al., 2000; Smedley et al., 2003; Sullivan, 2011; Bennett et al., 2021). A similar situation is seen in other health professions such as dentistry and pharmacy (Campbell et al., 2021; Nalliah et al., 2021; Bradley-Guidry et al., 2022; Chisholm-Burns et al., 2022). The AAMC describes those underrepresented in medicine (URiM) as “racial and ethnic populations that are underrepresented in the medical profession relative to their numbers in the general population” (Association of American Medical Colleges, 2004). As of 2020, 5.3% of physicians identified as Black or African American, 5.4% identified as Hispanic, Latino, or of Spanish origin, 1.9% identified as Other race or ethnicity, and less than 1% identified as American Indian or Alaska Native or as Native Hawaiian or Other Pacific Islander (0.4 and 0.2%, respectively; Association of American Medical Colleges, 2021a). By comparison, the census bureau reported that Black and African-American citizens accounted for 13.6% of the population and Hispanic/Latino/Latina/Latinx for 18.9% (U.S. Census Bureau, 2021).
There are many reasons that it is important to increase diversity in health professions. For example, studies have shown that URiM graduates are more likely to become primary care providers and serve the underrepresented and underserved communities, often coming from these communities themselves (Komaromy et al., 1996; Xu et al., 1997; Andriole and Jeffe, 2011; Lupton et al., 2012; Kuczewski and Brubaker, 2014; Larson and Frogner, 2019). Additionally, racial concordance and patient compliance has been explored and it has been shown that patients are more likely to comply with their medications and health directives when the race and experiences of their provider matches their own, leading to improved health outcomes (Street et al., 2008; Strumpf, 2011; Alsan et al., 2019; Mindlis et al., 2020; Schoenthaler and Ravenell, 2020; Takeshita et al., 2020). The recent social unrest in the United States, the pandemic which disproportionately affected minorities and calls by various organizations declaring racism a public health threat (American Medical Association, 2020; American Public Health Association, 2021; American Psychiatric Association, 2022) have most recently highlighted the importance of having a socially, ethnically, and culturally diverse healthcare workforce.
Nevertheless, despite a nearly 60% increase in enrollment in US medical schools in the last two decades (Association of American Medical Colleges, 2021b), and a concomitant rise of URiM and low socioeconomic applicants, the representation of these applicants in medical school classes has not kept pace with changes in population distribution (Grumbach et al., 2001; Smedley et al., 2003; Sanchez et al., 2015; Laurencin and Murray, 2017; Pfeffinger et al., 2020; Morris et al., 2021). Of particular concern, the growth of Black and African-American applicants, matriculants, and graduates has significantly lagged behind other groups (Koenig et al., 1998; Rodriguez and Campbell, 2015; Cloutier et al., 2021; Morris et al., 2021; Nakae and Subica, 2021).
There has been considerable discussion of the factors that contribute to the underrepresentation of minorities and marginalized individuals in all of the health fields, which has led to the concept of a “leaky pipeline” from college to medical school with some inclusion of K–12 (Barr et al., 2008; Upshur et al., 2018). Many contributory factors that are barriers to movement through the pipeline at the level of undergraduate education as well as at the admissions level of the professional schools have been identified. These factors include poor academic preparation (including the K-12 experience), lack of exposure to healthcare, lack of training for standardized examinations, admissions committee compositions, racist attitudes, and such. Perhaps the most studied of these is the observed score gaps among members of different racial and ethnic groups and different socioeconomic groups in regard to GPA and on standardized tests including the Graduate Record Examination, Law School Admission Test and the Medical College Admissions Test (MCAT; Koenig et al., 1998; Camara and Schmidt, 1999; Davis et al., 2013). Despite this, MCAT scores and GPA are used by medical schools to determine the readiness of applicants for success in the curriculum as studies continue to show that these metrics are correlated with passing the level 1 licensure exams, the United States Medical Licensing Examination (USMLE), and the Comprehensive Osteopathic Medical Licensing Examination (COMLEX; Casey et al., 2016; Ghaffari-Rafi et al., 2019; Zhong et al., 2021). This emphasis on academic metrics has led to the term “academic redlining” to describe the “systematic exclusion of qualified applicants from underrepresented racial and economic backgrounds” due to the use of MCAT data (Nakae and Subica, 2021). An overhaul of the MCAT in 2015 aimed to remove some of these barriers but, as with the “old” test, URiM students still perform on average below the 50th percentile (Thomas and Dockter, 2019; Association of American Medical Colleges, 2022c) and one study showed that nearly 30% of the applicants who had scores in the middle third of the MCAT (495–504) were URiM (Terregino et al., 2020). A major component of these unchanging scores especially in the CARs section likely relates to issues associated with underfunded and disinvested K-12 schools leading to a well-documented achievement gap for Black and Latinx children (Reardon, 2016; Goode and Landefeld, 2018; Orfield et al., 2019; Jones et al., 2021). On-going long-term assessment of the validity of the MCAT test is aimed at progression through medical school and will thus naturally focus only on matriculated students rather than students who did not get the scores necessary to be admitted.
In an attempt to mitigate the emphasis on these metrics, the AAMC developed a guide for the holistic review of applicants, through which admissions committees use, in addition to metrics, non-academic aspects (Experiences and Attributes) of an application to ensure that candidates from diverse backgrounds and experiences are reviewed (Association of American Medical Colleges, 2016; Grbic et al., 2019; Bates et al., 2020). However, while holistic review is encouraged by the AAMC, there are differences across schools as to the extent to which holistic review practices are implemented (Glazer et al., 2014) and each school still uses their own algorithms to set threshold cutoffs for GPA and MCAT below which an applicant is automatically rejected (Glazer et al., 2014; Goode and Landefeld, 2018). One reason for this is that pressure still exists on admissions committees to matriculate students with a strong likelihood of success (Glazer et al., 2014) since publications such as U.S. News & World Report continue to base rankings of medical schools on research funding, school reputation, and student selectivity factors not the number of diverse graduates (Ko et al., 2023). Another is a lack of a common definition and implementation of the practice (Artinian et al., 2017) and this is confounded by a high degree of variation in the institutional climate and declared social mission of US medical schools (Thomas and Dockter, 2019). Holistic review is also under threat by legal challenges to race-conscious admissions (Thomas and Dockter, 2019). Although the use of race as a factor in admissions has been ruled as legal by the Supreme Court [Regents of the University of California vs. Bakke (1978), Grutter vs. Bollinger (2003), and Fisher vs. University of Texas (2013)], the fate of existing admissions policies which support student diversity is currently (2023) again under consideration by the US Supreme Court (Curfman, 2022). The effect of a reversal of race-conscious admissions policies can be extrapolated from the observation that in the six states (California, Washington, Florida, Nebraska, Texas, and Michigan) who have state-wide bans of using race in admissions there has been a significant decline in the enrollment of historically minoritized and marginalized students in public medical schools (Steinecke and Terrell, 2008; Garces and Mickey-Pabello, 2015).
A further issue that contributes to continuing inequities in the matriculation of URiM students is the lack of diversity in academic medicine. Data from the AAMC shows that in allopathic medical schools over 83% of the medical school faculty is white or Asian and almost 90% of this same group hold the rank of Professor (Association of American Medical Colleges, 2022a). This lack of URiM faculty could potentially lead to admissions committees that have a different perspective and may demonstrate unconscious racial bias (Corrice, 2009). The lack of faculty diversity also results in a lack of role models, and this is especially an issue with Black males in medicine (Association of American Medical Colleges, 2015). Clearly, with a more diverse faculty, it is likely that the higher level of cultural humility would be a benefit to the educational experience (Odom et al., 2007; Joseph O. R. et al., 2021).
Looking at the financial cost of medical school, in 2019 the average 4-year cost of medical school was $250,222 at a state institution and $330,180 at a private medical school (Youngclaus and Fresne, 2020). Costs like these will disproportionately affect the lower socioeconomic applicants who may already have considerable undergraduate debt. Indeed, looking at the rates of matriculation into medical school as reported by the AAMC (Youngclaus and Roskovensky, 2018), approximately 76–79% of matriculants belonged to the top two highest quintiles in which yearly parental income is greater than $121,000, while only 5% come from the lowest household income quintile. With such clear household income inequities among matriculants, the influence of financial barriers is obvious and will disproportionally affect particularly Black and Hispanic or Latino applicants as a result of the persistent racial wealth gap and the effects of structural racism (Porter et al., 2020).
It is increasingly understood that various social determinants are paramount to the lack of diversity in medicine since social factors have long-term effects. These include several aspects that are unique in certain ways, but all relate to the marginalization of individuals in society, such as stereotype threat, minority status stress, and racial discrimination. Impostor phenomenon (Clance and Imes, 1978) is described as self-doubt of intellect, skills, or accomplishments. Although this is not a pathological condition, imposterism does correlate with burnout, psychological stress, depression, and adverse mental health (Bravata et al., 2020; Cawcutt et al., 2021). An interesting point of view from some individuals in higher education (Nadal et al., 2021; Ramos and Wright-Mair, 2021) suggests that impostor phenomenon is a direct byproduct of systemic oppression of marginalized groups. In addition, the lack of institutional diversity and shortage of role models in higher education and professional school increases the notion of “not belonging” (Stone et al., 2018). The negative feelings and doubt that come from impostor phenomenon especially in the competitive science, technology, engineering, and math (STEM) courses can lead to higher stress levels, anxiety, depression, poor attendance, lower course grades, and less persistence in STEM and beyond (Canning et al., 2019a).
In direct contrast to impostor phenomenon, self-efficacy is a key attribute for pre-medical and medical students (Artino, 2012). Self-efficacy as defined by Bandura (1977) is “…an individual’s belief in his or her own ability to organize and implement action to produce the desired achievements and results.” This confidence will be critical for success at all levels of learning and those with higher self-efficacy will be more likely to persist in STEM and onward to medical school (MacPhee et al., 2013). Additionally, social support systems and mentoring are important for students to provide continued motivation to carry on with their pursuit of a healthcare career (McNeill et al., 2014).
Given that many of the initiatives to remove or reduce the barriers to success for URiM students have not made significant changes to the diversity of medical schools, it may be time instead to take a critical look at what can be done to facilitate success by supporting the inherent qualities of URiM applicants. Thus, we aimed to explore the factors underrepresented students face as applicants for medical school and to answer the following research question: What are the factors and barriers that influence the matriculation of URiM students into medical school?
2. Methods
2.1. Design
Online databases, PubMed, and EBSCO were used to identify papers published in English between 1995 and 2023 regarding matriculation of students to US medical schools. Results were screened using a two-phase system, title and abstract review, with subsequent full text review by both CT and CAG to determine if articles met the inclusion or exclusion criteria.
2.2. Search strategy
The search strategy focused on factors that may influence the matriculation of URiM applicants into medical school. Barriers and protective factors to investigate were initially identified by CT through her personal experiences as a first-generation Latina. These were modified and extended by discussions with other URiM pre-medical students and refined as the literature review was performed. The development of categories was an iterative process as the manuscript was prepared and revised.
The initial search took place in October 2020 with a subsequent search performed in March 2023. From December 2022 to April 2023, citation alerts were reviewed for any additional relevant publications. Employing the use of the supplemental Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist (Page et al., 2021), a combination of the following search terms and keywords were used: matriculants, underrepresented, resiliency, self-efficacy, medical school, barriers, impostor, African-American, Black, Hispanic, Latino, successful, and health profession school. These search terms were initially determined by the personal and educational experiences of CT and CAG. Limits were set to publications and results confined to those available in English between 1995 and 2023.
2.3. Inclusion and exclusion criteria
Both researchers screened the literature with specific inclusion and exclusion criteria, which were modified throughout the study selection process to narrow the focus of the selected articles.
To be included in the review, papers needed to specifically discuss or focus on factors that either supported or reduced the pool of underrepresented applicants to US medical schools. The target participants were URiM high school and college students. Articles discussing strategies for retention of matriculants in medical school or strategies for increasing enrollment in other health professions were not included. Additionally, papers were excluded if they discussed factors that did not match one of the theme areas we had identified, were not published in English, or pertained to schools other than those in the United States.
Screening took place in two phases. Phase 1 consisted of screening title and abstract of articles retrieved during the search of keywords. The screening was for specific terminology related to URiM admissibility and/or matriculation into medical school in the United States. In Phase II, full-text articles were assessed for eligibility and relevance to the goals of the study and research question.
3. Results
3.1. Included studies
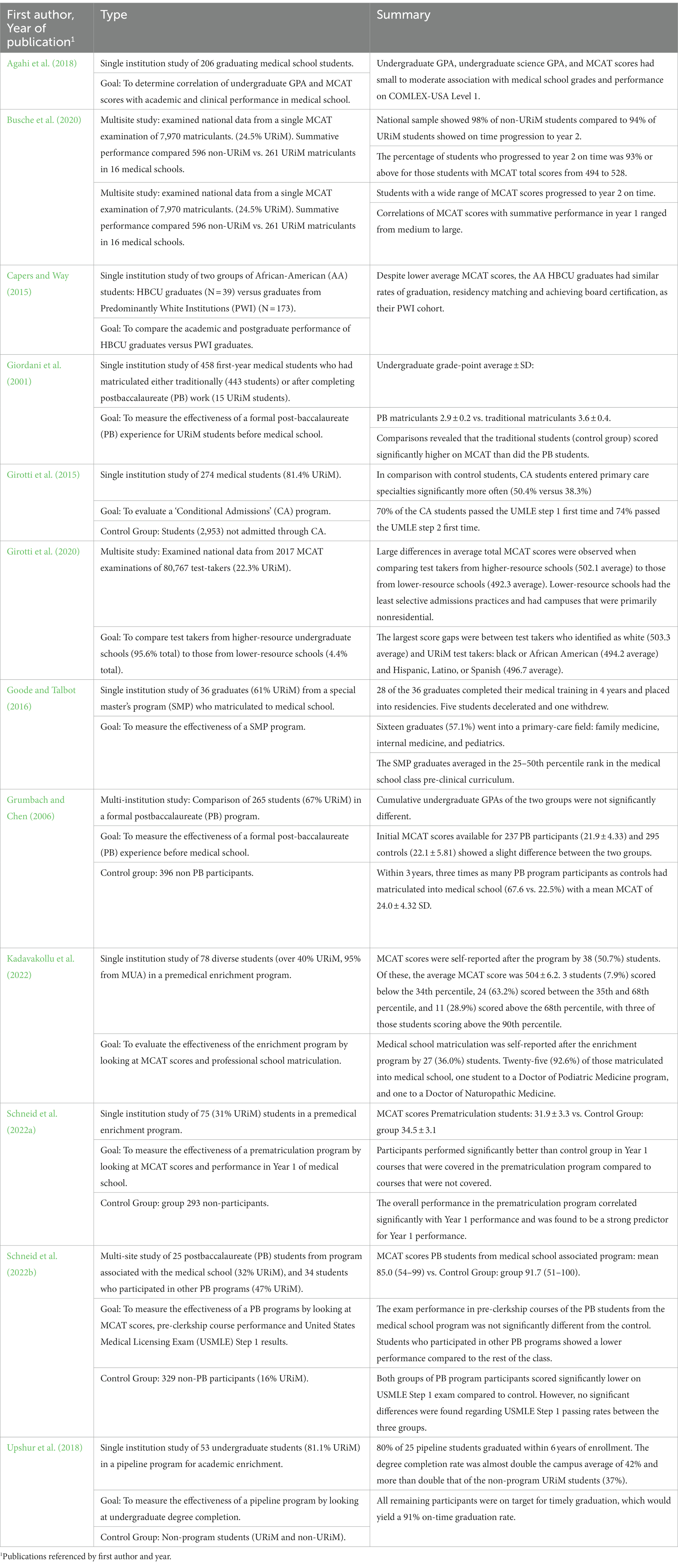
Initial search results were exported to EndNote and duplicates removed for a total of 196 citations. Upon further exploration and browsing of appropriate foundation websites, citation alerts, and review of cited references, 30 additional publications were added for a total of 226 citations. Phase I screening excluded 78 articles and 148 were deemed appropriate for full review by both authors. After Phase II, full text review confirmed that 66 articles met all criteria. A flow diagram was adapted from the PRISMA guidelines (Supplementary Figure 1 in Supplementary material) and used during the screening process. Several of the studies discussed multiple factors. Articles included presentations, scholarly perspectives, qualitative surveys, and data reports. Most of the studies were single institution, and many included a control group or a comparison to national data. The literature was grouped into broad categories by CT and CAG based on the barriers or protective factors discussed. Tables 1–5 summarize each article reviewed by describing the type, and size of study and the goal, and the results.
3.1.1. Academic metrics
A significant and much studied barrier for increasing diversity is academic metrics since medical schools rely heavily on MCAT scores and undergraduate GPA to determine admission, but data continue to show a persistent score gap for URiM and low SES applicants (Table 1). There is some evidence that standardized test scores and GPA do not necessarily correlate with progression through medical school. Indeed, students with midrange and lower MCAT scores also proceed successfully through their pre-clinical curriculum and pass their first licensure exams (USMLE and COMLEX; Capers and Way, 2015; Girotti et al., 2015, 2020; Agahi et al., 2018; Busche et al., 2020; Schneid et al., 2022a,b). A reduced emphasis on MCAT would capture more URiM students; however, the key role of the medical school must be recognized in supporting students with lower scores—a collaborative learning environment, diverse peers, and an experiential curriculum have all been highlighted as critical. The demonstrated success of diversity-targeted pipeline and postbaccalaureate programs in preparing students for degree completion and success in medical school additionally points to the critical importance of improving study-methods and test-taking skills (Giordani et al., 2001; Grumbach and Chen, 2006; Goode and Talbot, 2016; Upshur et al., 2018; Kadavakollu et al., 2022; Schneid et al., 2022b).
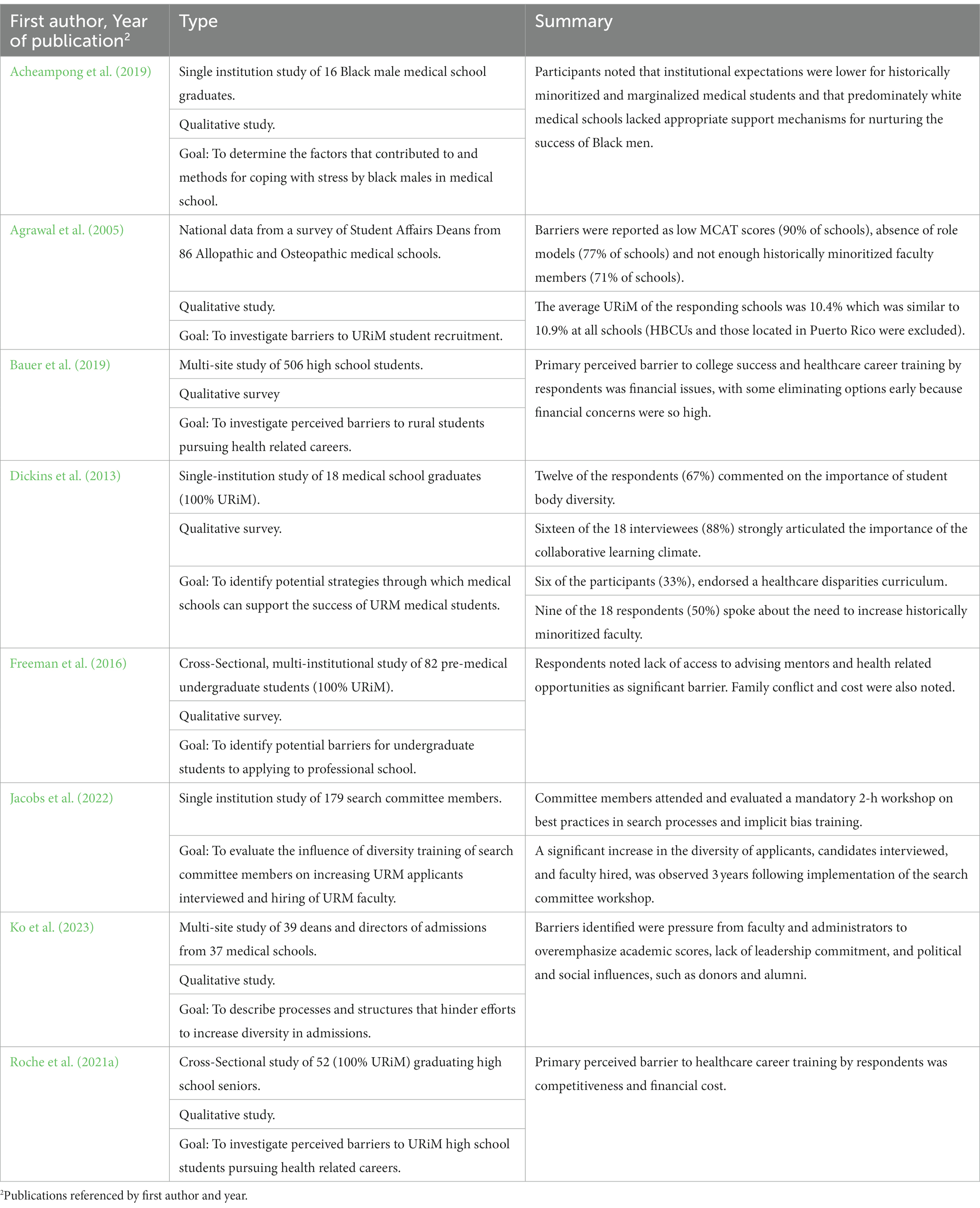
3.1.2. Faculty diversity
One issue, stemming from the previously mentioned lack of faculty diversity in academic medicine, is that admissions committees may have different perspectives of the barriers that URiM students will face in acceptance to, and success in, medical school (Table 2). To demonstrate this, when surveyed, admissions leaders viewed academic performance as measured by undergraduate GPA and MCAT as the most significant measure of academic attainment and hence a key barrier for URiM applicants (Agrawal et al., 2005; Ko et al., 2023). In contrast, diverse students when asked the same question were more likely to identify financial concerns, feelings of academic inadequacy, and lack of racially concordant faculty and mentors (Dickins et al., 2013; Freeman et al., 2016; Acheampong et al., 2019; Bauer et al., 2019; Roche et al., 2021a). Improving faculty diversity in academic medicine is obviously critical but in the short-term admissions committee members may benefit from unconscious bias mitigation training and workshops including taking implicit association tests (Jacobs et al., 2022). Although the long-term effects of this training are not clear, especially with the frequent turn-over of admissions committees’ members, increasing individuals’ knowledge of their implicit racial biases would likely positively impact their review of historically minoritized and marginalized applicants.
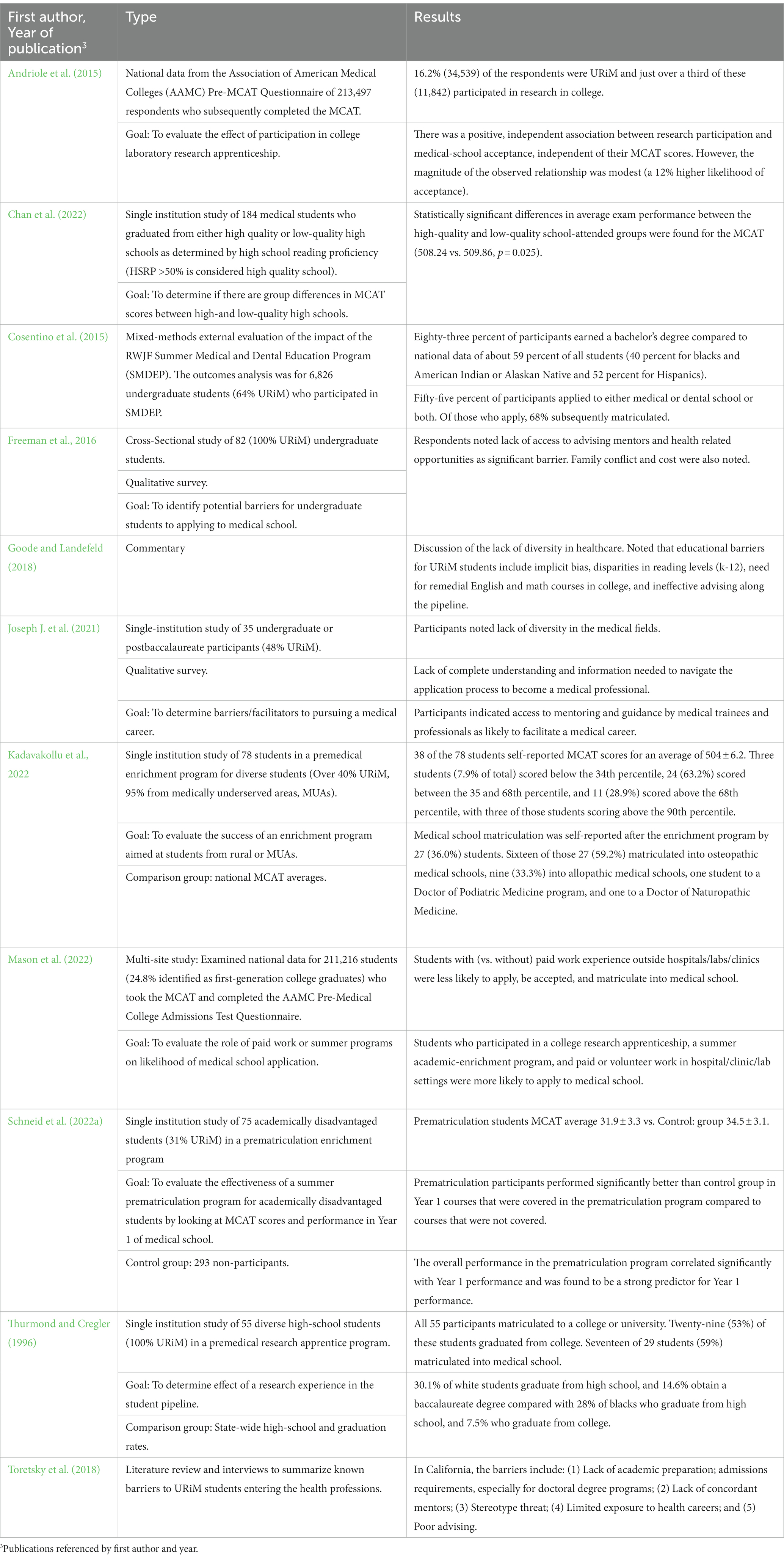
3.1.3. Educational
Many URiM applicants come from lower socioeconomic backgrounds and attend underfunded and disinvested schools and institutions, significantly limiting the number of resources available to these students which can result in lower rates of college attendance, undergraduate degree completion, and lower MCAT scores (Freeman et al., 2016; Goode and Landefeld, 2018; Chan et al., 2022; Table 3). The lack of informed academic advisors and less familiarity with the university and medical school application processes is also a significant barrier for URiM students to overcome, particularly those that are first-generation (Joseph J. et al., 2021).
Underrepresented in medicine applicants are also less likely to have access to positive educational opportunities such as research experience, exposure to healthcare career opportunities or have a family member who is a healthcare provider (Freeman et al., 2016; Goode and Landefeld, 2018; Toretsky et al., 2018). An early association was noted by Thurmond showing that participants in an URiM student research apprenticeship program were more likely to choose a science major and later choose a healthcare career (Thurmond and Cregler, 1996). This has been further reinforced by additional studies demonstrating that URiM students who obtained health professions exposure, and participated in healthcare career opportunities and other summer enrichment programs, had higher MCAT scores and were more likely to apply to medical school (Andriole et al., 2015; Cosentino et al., 2015; Kadavakollu et al., 2022; Mason et al., 2022; Schneid et al., 2022a).
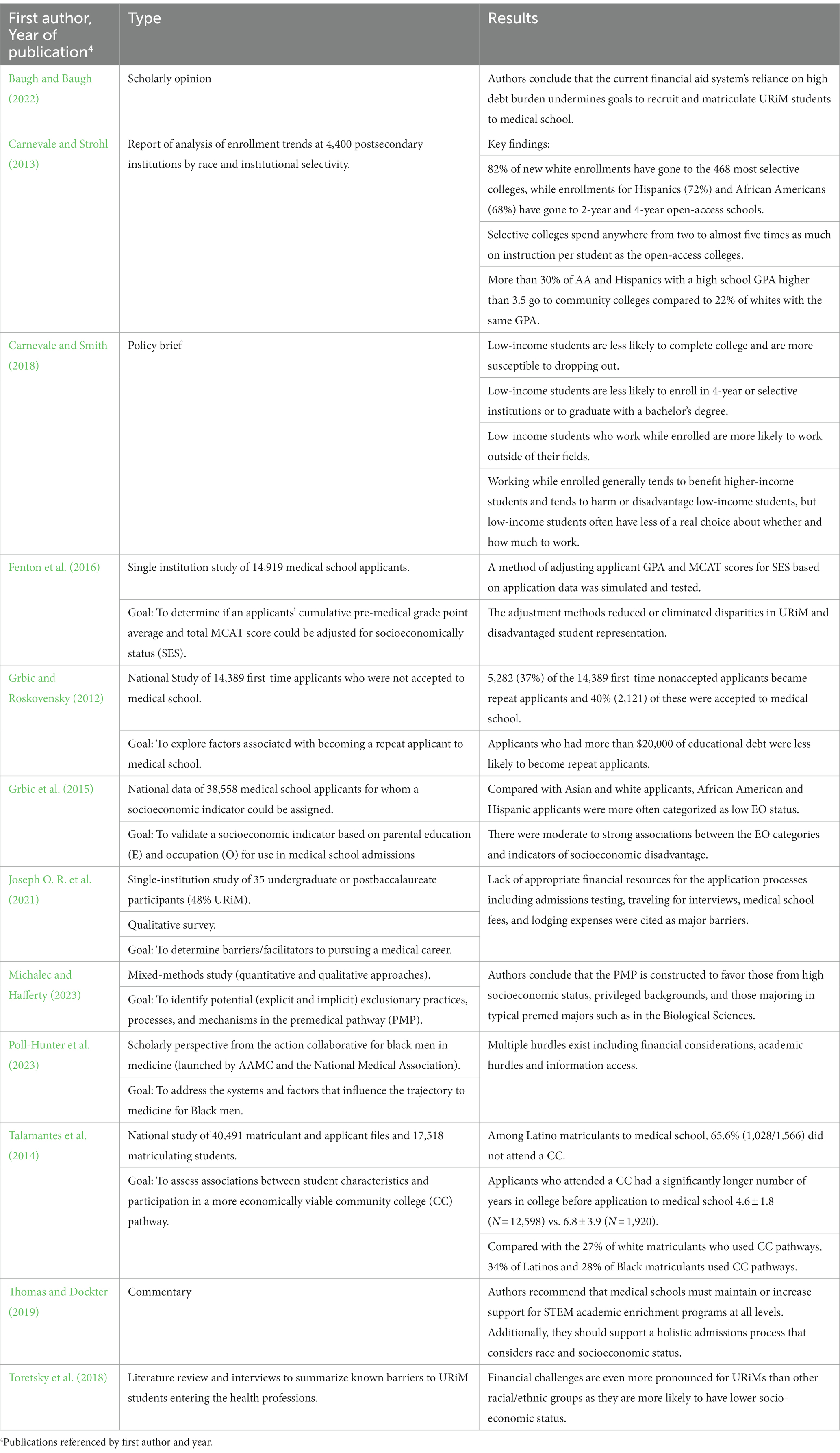
3.1.4. Financial
In addition to the obvious concerns of the cost of medical school (Baugh and Baugh, 2022), financial barriers are evident as URiM students are more likely to come from low socioeconomic backgrounds, experience financial stress during their undergraduate education and are more likely to need to work through college (Carnevale and Smith, 2018; Toretsky et al., 2018; Table 4). This leads to a myriad of results: reduced study time resulting in a less than competitive GPA, no opportunity for extra-curricular and volunteer activities, and the inability to pay for MCAT preparatory classes or even the exam itself. Indeed, the pre-medical pathway has been referred to as an example of discriminatory design based on the disadvantages it poses for applicants who come from low socioeconomic status (SES) backgrounds (Michalec and Hafferty, 2023). Unsuccessful first-time applicants to medical school with high pre-existing debt are further shown to be less likely to reapply (Grbic and Roskovensky, 2012). The additional cost of other programs such as postbaccalaureate courses to increase preparation, meet prerequisites or raise GPA becomes an added financial stressor (Talamantes et al., 2014; Toretsky et al., 2018; Joseph J. et al., 2021; Poll-Hunter et al., 2023). Even pipeline programs that are meant to increase matriculation of URiM students to health profession schools, come at a cost, directly or indirectly through loss of summer wages, and are likely to increase debt. There has been some discussion that low SES is actually the primary barrier to diversifying schools and that it should be considered in admissions instead of race (Carnevale and Strohl, 2013; Grbic et al., 2015; Fenton et al., 2016). However, this would not account for systemic marginalization of URiM applicants related to issues such as education, employment and criminal justice. Indeed, it has been reported that an admissions process that considers SES in place of race does not admit the same numbers of Black and Hispanic/Latina/Latino/Latinx applicants as a process that considers race (Thomas and Dockter, 2019).
3.1.5. Psychosocial factors
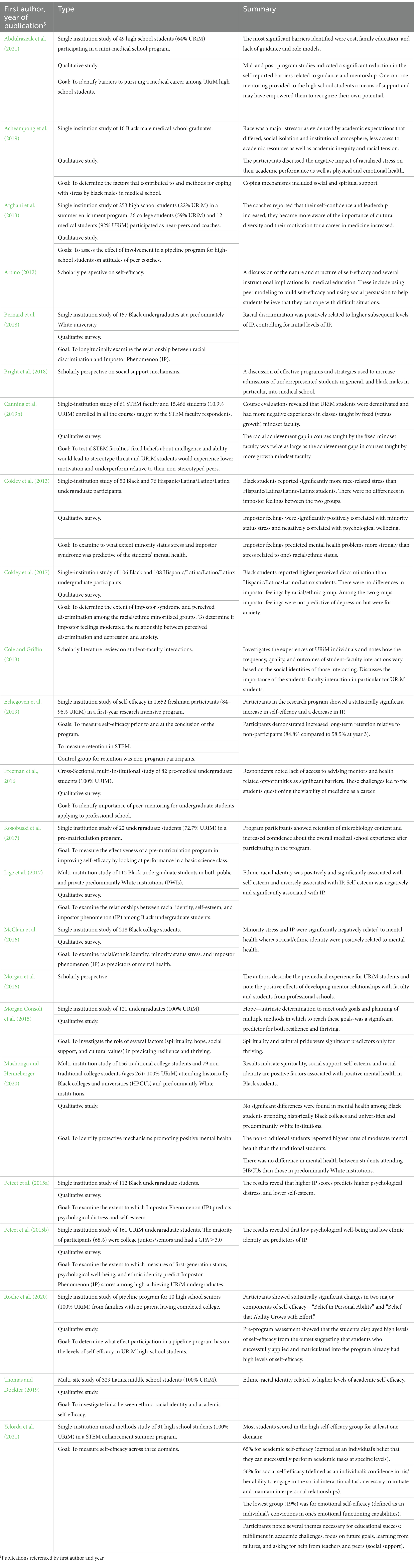
In this category, which covers the highest percentage of the citations, we looked at psychosocial factors which are less studied but are clearly significant for historically minoritized and marginalized students (Table 5). We have included the negative factor of impostor phenomenon and the more positive facilitators of self-efficacy and social/spiritual support.
Underrepresented and first-generation students often experience feeling like impostors in college and this can negatively influence their academic performance, their confidence in their abilities, and ultimately their success. The feeling of additional pressure to prove others wrong and the experience of microaggressions and perceived racism is particularly prevalent in minoritized and marginalized communities (Peteet et al., 2015b; Toretsky et al., 2018; Acheampong et al., 2019). An interesting point of view from some individuals in higher education (Ramos and Wright-Mair, 2021) suggests that impostor phenomenon is a direct byproduct of systemic oppression (e.g., racism, sexism) and is exacerbated by bias and microaggressions (Bernard et al., 2018). As an example, in courses taught by STEM faculty with a belief in fixed ability, the racial achievement gap was large, the URiM students experienced stereotype threat, were demotivated and this contributed to the feelings of impostorism (Canning et al., 2019b). Indeed, it is clear that impostor phenomenon, minority status stress, and race related stressors such as racial microaggressions are interconnected and all contribute to poor mental health, psychological stress, and low self-efficacy (Cokley et al., 2013, 2017; Peteet et al., 2015a; McClain et al., 2016; Bernard et al., 2018). Of importance though is that racial identity, the importance of race/ethnicity to an individual’s overall sense of self, may mitigate the feelings of impostor phenomenon (McClain et al., 2016) by increasing self-efficacy (Echegoyen et al., 2019), and self-esteem (McClain et al., 2016; Lige et al., 2017). In contrast, lower racial/ethnic identity is a predictor of impostor phenomenon (Peteet et al., 2015b).
Self-efficacy as defined by Bandura (1977) is “an individual’s belief in his or her own ability to organize and implement action to produce the desired achievements and results.” The literature suggests that although many URiM students may need additional assistance for successful matriculation, those that apply to and participate in pipeline programs or research experiences possess high levels of confidence in their ability to succeed and their participation in these programs reinforces this quality of self-efficacy (Artino, 2012; Turan et al., 2013; Miller, 2014; Kosobuski et al., 2017; Echegoyen et al., 2019; Roche et al., 2020; Yelorda et al., 2021). As mentioned, racial identity is also related to higher self-efficacy and targeted pipeline programs may provide an environment to foster and improve this ethnic centrality. Indeed, Bright et al. (2018) have suggested the development of programs to specifically target these positive qualities by increasing the opportunities for academic nurturing and mentoring to increase application and matriculation of URiM applicants.
To provide continued motivation to carry on with their pursuit of medical school, URiM and marginalized applicants rely on social support systems and mentoring (Afghani et al., 2013; Acheampong et al., 2019; Abdulrazzak et al., 2021; Roche et al., 2021b). For some students, in the face of adversity and stress, connecting with others decreased the negative effects and helped them stay motivated (Morgan Consoli et al., 2015; Acheampong et al., 2019). Relating to other students with experience in similar paths, perhaps through peer-mentoring programs, helps to mitigate negative experiences associated with being a marginalized pre-medical student perhaps by increasing or reinforcing racial/ethnic identity. With regard to medical school applications, as URiM applicants look at the grades needed and statistics for acceptance, the impostor phenomenon may lead them to believe that they are not competitive and this may be enough to deter them from moving forward in their endeavor if they are not actively supported at multiple points in their journey (Freeman et al., 2016; Morgan et al., 2016). The student-faculty relationship in particular has been shown to be one of the most influential and important social relationships for students, especially for students of color (Cole and Griffin, 2013). In this regard, undergraduate research experiences can provide long-lasting mentor-student relationships. Additionally, for some URiM students, having faith and/or practicing spirituality seems to decrease stress associated with the pre-medical journey and provides the support to successfully continue moving forward in academics (Acheampong et al., 2019; Mushonga and Henneberger, 2020).
4. Discussion
The lack of physician diversity in the US has been investigated extensively and the vast majority of literature is aimed at investigating barriers that negatively affect URiM students matriculating to and graduating from medical school. This review, which focused on the application and matriculation of URiM applicants to medical school, reinforced the known barriers of academic criteria, educational disadvantages, lack of faculty diversity, and financial considerations. For a low SES applicant, which encompasses many URiM applicants, healthcare experience opportunities, involvement in research, summer enrichment programs, and even co-curricular activities are often out of reach due to the need to work to support themselves and their families (Clement, 2016). Lack of these opportunities may make an applicant’s file less competitive especially in light of the AAMC experiences-attributes-metrics model (Association of American Medical Colleges, 2020). An alternative may be encouraging admissions officers and committee members to recognize the inherent value of paid healthcare experience as compared to medical volunteerism and clinical shadowing (Association of American Medical Colleges, 2022b) especially given the observation that these experiences may improve success in the clerkship environment (Strowd et al., 2020). A commitment of all levels of administration in medical schools to full implementation of holistic admissions practices will certainly allow for a better evaluation of the various aspects of an applicant’s files including the barriers that they have faced. Diversifying the admissions committee membership will also be key (Robinett et al., 2021) as well as recognizing and mitigating unconscious bias at all levels. The emphasis on objective academic criteria such as GPA and standardized testing should be tempered by the realization that these metrics are the end result of a number of interrelated factors such as school district funding, study time, educational support and financial ability to participate in opportunities such as advanced placement courses and test-preparation (Allegretto et al., 2022). More investigation must be done to delineate these relationships and address the issues at the source. In addition, these metrics do not provide information on the quality of the healthcare professional an applicant may become, and non-cognitive variables are critical in addressing this component of the application (Strowd et al., 2020). A promising new initiative, the AAMC PREview professional readiness exam (Association of American Medical Colleges, 2023), aims to objectively assess certain key core competencies and skills for pre-medical students such as resilience, service orientation, ethics teamwork, and cultural competence. The efficacy of this exam is currently being tested in 18 allopathic schools.
In addition to the obvious barriers, there are also a number of psychological, cultural, and social factors that contribute to the premedicine journey of URiM students. Impostor phenomenon is increasingly reported in historically minoritized and marginalized communities and is considered by some as a consequence of structural racism (McGee et al., 2021) and lack of campus and professional diversity. In the absence of role models, historically minoritized and marginalized students may feel like they do not belong, and this can lead to feelings of inadequacy, incompetency, and self-doubt—all criteria of impostor phenomenon. In the STEM educational pipeline where there is a clear lack of racial diversity these feelings of impostor syndrome can and do lead to negative experiences, lack of motivation, burn-out, and ultimately a lack of persistence and/or retention (Goode and Landefeld, 2018; Tao and Gloria, 2019). In contrast, positive racial (and STEM) identity is a protective factor against impostor phenomenon and again highlights the need to increase diversity and racially concordant mentors and role-models at all points in the pipeline, including through residency and into academic medicine.
Other facilitators of URiM students to continue their journey to medical school include self-efficacy and/or self-belief, which is developed in many pipeline programs and research experiences. Clearly to support the cultural wealth of historically minoritized and marginalized students, the involvement of strong role models through high-school and college and social support networks which can foster this development must be nurtured and encouraged. In addition, spirituality and high levels of racial or ethnic centrality have been seen to be important in giving historically marginalized students the tools to deal with perceived and real racism. Finally, any attempts to increase the matriculation of URiM students into medical school must be coupled with a commitment from the institutions that they will provide the climate that will support the persistence and success of those students.
This review was not meant to be exhaustive but instead focused on several factors that we identified that effect underrepresented students on the premedicine pathway. Limitations of this review were that much of the literature discussed came from qualitative reports and from self-reported data and surveys, information which is subjective. In many cases, the cohorts under study were small and were from a single institution or single program. The primary focus was on the racial and ethnic minorities of Black/African American and Hispanic/Latinx, since although Native Americans and Alaskan Natives are also underrepresented in medicine, we were unable to find sufficient literature to speak on additional factors related to this population. The expectation is that the same factors will apply to these groups. In addition, in some regions, Southeast Asians are considered URiM but data reports and most literature aggregate Asian populations. We also did not include other historically minoritized and marginalized groups such as sex assigned at birth/gender/gender identity (LGBTQ+) or disabled. Although diversity initiatives extend back over four decades, this review focused on the last 30 years to cover only two iterations of the MCAT. Finally, our grouping of articles was largely subjective and based on the broad categories, and the articles themselves may not have used the same terms and/or language when discussing the various barriers or protective factors.
To conclude, if the diversity of US physicians is ever to approach the diversity of the US population, all factors should be investigated to increase the academic success and eventual matriculation of historically minoritized and marginalized students to medical school. The emphasis on barriers to success should be balanced with promoting protective factors, in particular, those that diverse students rely on for persistence in their education.
Author contributions
CT and CG contributed to conception and design of the study. CT proposed the factors and barriers based largely on her experiences as a first-generation Latina and wrote the first draft of the manuscript. CG organized the database. All authors contributed to the article and approved the submitted version.
Acknowledgments
We would like to acknowledge the input of Alissa Craft in the early phases of the writing. CG would like to thank Thomas Landefeld for many spirited and productive conversations.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fpsyg.2023.1141045/full#supplementary-material
References
Abdulrazzak, A., Chandler, A., Lu, R., Mobarakai, O., Lebron, B., Ingram, N., et al. (2021). Mini-medical school programs decrease perceived barriers of pursuing medical careers among underrepresented minority high school students. J. Osteopath. Med. 121, 883–890. doi: 10.1515/jom-2021-0125
Acheampong, C., Davis, C., Holder, D., Averett, P., Savitt, T., and Campbell, K. (2019). An exploratory study of stress coping and resiliency of black men at one medical school: a critical race theory perspective. J. Racial Ethn. Health Disparities 6, 214–219. doi: 10.1007/s40615-018-0516-8
Afghani, B., Santos, R., Angulo, M., and Muratori, W. (2013). A novel enrichment program using cascading mentorship to increase diversity in the health care professions. Acad. Med. 88, 1232–1238. doi: 10.1097/ACM.0b013e31829ed47e
Agahi, F., Speicher, M. R., and Cisek, G. (2018). Association between undergraduate performance predictors and academic and clinical performance of osteopathic medical students. J. Am. Osteopath. Assoc. 118, 106–114. doi: 10.7556/jaoa.2018.025
Agrawal, J. R., Vlaicu, S., and Carrasquillo, O. (2005). Progress and pitfalls in underrepresented minority recruitment: perspectives from the medical schools. J. Natl. Med. Assoc. 97, 1226–1231.
Allegretto, S., Garcia, E., and Weiss, E. (2022). Public education funding in the U.S. needs an overhaul. How a larger Federal Role Would Boost Equity and Shield Children from Disinvestment during Downturns. Available at: https://www.epi.org/publication/public-education-funding-in-the-us-needs-an-overhaul/ (Accessed December 12, 2022).
Alsan, M., Garrick, O., and Graziani, G. (2019). Does diversity matter for health? Experimental evidence from Oakland. Am. Econ. Rev. 109, 4071–4111. doi: 10.1257/aer.20181446
American Medical Association (2020). New AMA policy recognizes racism as a public health threat [online]. American Medical Association. Available at: https://www.ama-assn.org/press-center/press-releases/new-ama-policy-recognizes-racism-public-health-threat (Accessed November 16, 2020).
American Psychiatric Association (2022). APA's apology to black, indigenous and people of color for its support of structural racism in psychiatry [online]. American Psychiatric Association. Available at: https://www.psychiatry.org/newsroom/apa-apology-for-its-support-of-structural-racism-in-psychiatry (Accessed December 21, 2022).
American Public Health Association (2021). Structural racism is a public health crisis: Impact on the black community [online]. American Public Health Association. Available at: https://www.apha.org/policies-and-advocacy/public-health-policy-statements/policy-database/2021/01/13/structural-racism-is-a-public-health-crisis (Accessed December 21, 2022).
Andriole, D. A., and Jeffe, D. B. (2011). Characteristics of medical school Matriculants who participated in Postbaccalaureate premedical programs. Acad. Med. 86, 201–210. doi: 10.1097/ACM.0b013e3182045076
Andriole, D. A., Jeffe, D. B., and Tai, R. H. (2015). Participation in college laboratory research apprenticeships among students considering careers in medicine. Med. Educ. Online 20:27231. doi: 10.3402/meo.v20.27231
Artinian, N. T., Drees, B. M., Glazer, G., Harris, K., Kaufman, L. S., Lopez, N., et al. (2017). Holistic admissions in the health professions: findings from a National Survey. Coll. Univ. 92, 65–68.
Artino, A. R. (2012). Academic self-efficacy: from educational theory to instructional practice. Perspect. Med. Educ. 1, 76–85. doi: 10.1007/S40037-012-0012-5
Association of American Medical Colleges (2004). Underrepresented in medicine definition [online]. Available at: https://www.aamc.org/initiatives/urm (Accessed December 12, 2022).
Association of American Medical Colleges (2015). Altering the course, black males in medicine [online]. Washington, DC. Available at: https://store.aamc.org/altering-the-course-black-males-in-medicine.html (Accessed March 29, 2023).
Association of American Medical Colleges (2016). Best practices for recruitment and retention of a diverse student body [online]. Available at: https://www.aamc.org/media/23151/download (Accessed December 12, 2022).
Association of American Medical Colleges (2020). Holistic review in medical school admissions: An introduction [online]. Available at: https://www.aamc.org/media/45551/download (Accessed April 1, 2023).
Association of American Medical Colleges (2021a). 2021 state physician workforce data report [online]. AAMC. Available at: https://store.aamc.org/downloadable/download/sample/sample_id/506/ (Accessed February 13, 2023).
Association of American Medical Colleges (2021b). AAMC medical school enrollment survey: 2020 results [online]. Available at: https://www.aamc.org/media/9936/download (Accessed January 12, 2023).
Association of American Medical Colleges (2021c). The complexities of physician supply and demand: Projections from 2019 to 2034 [online]. Washington, DC: IHS Markit Ltd. Available at: https://www.aamc.org/media/54681/download (Accessed January 12, 2023).
Association of American Medical Colleges (2022a). Faculty roster: U.S. medical school faculty. Table 3. Rank and race/ethnicity [online]. Available at: https://www.aamc.org/data-reports/faculty-institutions/interactive-data/2022-us-medical-school-faculty (Accessed February 8, 2023).
Association of American Medical Colleges (2022b). Table 1. Using MCAT data in 2023 medical student selection. [online]. Available at: https://www.aamc.org/system/files/2020-07/services_mcat_using-mcat-data-in-2021-medical-student-selection-guide_07082020_0.pdf (Accessed January 10, 2023).
Association of American Medical Colleges (2022c). Table A-18. MCAT scores and GPAs for applicants and matriculants to U.S. MD-granting medical schools by race/ethnicity, 2022–2023 [online]. Available at: https://www.aamc.org/media/6066/download (Accessed March 29, 2023).
Association of American Medical Colleges (2023). AAMC PREview™ professional readiness exam [online]. Available at: https://students-residents.aamc.org/aamc-preview/aamc-preview-professional-readiness-exam (Accessed April 1 2023).
Bandura, A. (1977). Self-efficacy: toward a unifying theory of behavioral change. Psychol. Rev. 84, 191–215. doi: 10.1037/0033-295X.84.2.191
Barr, D. A., Gonzalez, M. E., and Wanat, S. F. (2008). The leaky pipeline: factors associated with early decline in interest in premedical studies among underrepresented minority undergraduate students. Acad. Med. 83, 503–511. doi: 10.1097/ACM.0b013e31816bda16
Bates, T., Mutha, S., and Coffman, J. (2020). Practicing holistic review in medical education [Online]. UCSF: Healthforce Center. Available: https://healthforce.ucsf.edu/publications/practicing-holistic-review-medical-education (Accessed December 12, 2022).
Bauer, H. H., Anderson, C. B., Hirko, K., and Wendling, A. (2019). Barriers to college and health care careers among US students from a rural community. PRiMER 3:10. doi: 10.22454/PRiMER.2019.828405
Baugh, A. D., and Baugh, R. F. (2022). How financial aid policy shortchanges American healthcare. Teach. Learn. Med. 34, 322–328. doi: 10.1080/10401334.2021.1977135
Bennett, C. L., Yiadom, M., Baker, O., and Marsh, R. H. (2021). Examining parity among black and Hispanic resident physicians. J. Gen. Intern. Med. 36, 1722–1725. doi: 10.1007/s11606-021-06650-7
Bernard, D. L., Hoggard, L. S., and Neblett, E. W. (2018). Racial discrimination, racial identity, and impostor phenomenon: a profile approach. Cult. Divers. Ethn. Minor. Psychol. 24, 51–61. doi: 10.1037/cdp0000161
Bradley-Guidry, C., Burwell, N., Dorough, R., Bester, V., Kayingo, G., and Suzuki, S. (2022). An assessment of physician assistant student diversity in the United States: a snapshot for the healthcare workforce. BMC Med. Educ. 22:680. doi: 10.1186/s12909-022-03717-9
Bravata, D. M., Watts, S. A., Keefer, A. L., Madhusudhan, D. K., Taylor, K. T., Clark, D. M., et al. (2020). Prevalence, predictors, and treatment of impostor syndrome: a systematic review. J. Gen. Intern. Med. 35, 1252–1275. doi: 10.1007/s11606-019-05364-1
Bright, C. M., Price, M. A., Morgan, R. C. Jr., and Bailey, R. K. (2018). The report of the W. Montague Cobb /NMA Health Institute Consensus Panel on the plight of underrepresented minorities in medical education. J. Natl. Med. Assoc. 110, 614–623. doi: 10.1016/j.jnma.2018.03.012
Busche, K., Elks, M. L., Hanson, J. T., Jackson-Williams, L., Manuel, R. S., Parsons, W. L., et al. (2020). The validity of scores from the new MCAT exam in predicting student performance: results from a multisite study. Acad. Med. 95, 387–395. doi: 10.1097/ACM.0000000000002942
Camara, W., and Schmidt, A. (1999). Group differences in standardized testing and social stratification. College board report [online], 99. Available at: https://files.eric.ed.gov/fulltext/ED562656.pdf (Accessed December 12, 2022).
Campbell, H. E., Hagan, A. M., and Gaither, C. A. (2021). Addressing the need for ethnic and racial diversity in the pipeline for pharmacy faculty. Am. J. Pharm. Educ. 85:8586. doi: 10.5688/ajpe8586
Canning, E. A., Lacosse, J., Kroeper, K. M., and Murphy, M. C. (2019a). Feeling like an imposter: the effect of perceived classroom competition on the daily psychological experiences of first-generation college students. Soc. Psychol. Personal. Sci. 11, 647–657. doi: 10.1177/1948550619882032
Canning, E. A., Muenks, K., Green, D. J., and Murphy, M. C. (2019b). STEM faculty who believe ability is fixed have larger racial achievement gaps and inspire less student motivation in their classes. Sci. Adv. 5:eaau4734. doi: 10.1126/sciadv.aau4734
Capers, Q. T., and Way, D. P. (2015). Academic and post-graduate performance of African American medical students by category of premed institution: historically Black vs. predominantly White institutions. J. Health Care Poor Underserved 26, 617–630. doi: 10.1353/hpu.2015.0082
Carnevale, A.P., and Smith, N. (2018). Balancing work and learning: Implications for low-income students [online]. Washington, DC: Center on Education and the Workforce, Georgetown University. Available at: https://cew.georgetown.edu/cew-reports/LearnAndEarn/ (Accessed December 15, 2022).
Carnevale, A.P., and Strohl, J. (2013). Separate and unequal [online]. Washington, DC: Georgetown Public Policy Institute. Available at: https://cew.georgetown.edu/cew-reports/separate-unequal/ (Accessed December 12, 2022).
Casey, P. M., Palmer, B. A., Thompson, G. B., Laack, T. A., Thomas, M. R., Hartz, M. F., et al. (2016). Predictors of medical school clerkship performance: a multispecialty longitudinal analysis of standardized examination scores and clinical assessments. BMC Med. Educ. 16:128. doi: 10.1186/s12909-016-0652-y
Cawcutt, K.A., Clance, P., and Jain, S. (2021). "Bias, burnout, and imposter phenomenon: the negative impact of under-recognized Intersectionality" in Womens Health Rep. New Rochelle. 643–647.
Chan, L. J., Patel, D., Khalid, A., Ely, K., Lagasca, G., and Simanton, E. (2022). Impact of high school quality on academic performance throughout medical school. Cureus 14:e31496. doi: 10.7759/cureus.31496
Chisholm-Burns, M. A., Spivey, C. A., and Tipton, N. G. (2022). A diversity index to measure underrepresented minority enrollment in United States colleges and schools of pharmacy. Curr. Pharm. Teach. Learn. 14, 1340–1347. doi: 10.1016/j.cptl.2022.09.025
Clance, P. R., and Imes, S. A. (1978). The imposter phenomenon in high achieving women: dynamics and therapeutic intervention. Psychotherapy: theory. Res. Pract. 15, 241–247. doi: 10.1037/h0086006
Clement, L. (2016). External and internal barriers to studying can affect student success and retention in a diverse classroom. J. Microbiol. Biol. Educ. 17, 351–359. doi: 10.1128/jmbe.v17i3.1077
Cloutier, R. L., Bumsted, T., and Mejicano, G. (2021). The MCAT was a barrier to diversity long before COVID-19. Acad. Med. 96, e22–e23. doi: 10.1097/ACM.0000000000004196
Cokley, K., McClain, S., Enciso, A., and Martinez, M. (2013). An examination of the impact of minority status stress and impostor feelings on the mental health of diverse ethnic minority college students. J. Multicult. Couns. Dev. 41, 82–95. doi: 10.1002/j.2161-1912.2013.00029.x
Cokley, K., Smith, L., Bernard, D., Hurst, A., Jackson, S., Stone, S., et al. (2017). Impostor feelings as a moderator and mediator of the relationship between perceived discrimination and mental health among racial/ethnic minority college students. J. Couns. Psychol. 64, 141–154. doi: 10.1037/cou0000198
Cole, D., and Griffin, K. A. (2013). “Advancing the study of student-faculty interaction: a focus on diverse students and faculty” in Higher Education: Handbook of Theory and Research. ed. M. Paulson (Springer Science and Business Media), 561–611.
Corrice, A. (2009). "Unconscious bias in faculty and leadership recruitment: a literature review" in Analysis in Brief. Washington, DC: Assocation of American Medical Colleges.
Cosentino, C., Speroni, C., Sullivan, M., and Torres, R. (2015). Impact evaluation of the RWJF summer medical and dental education program (SMDEP). Available at: https://www.mathematica.org/publications/impact-evaluation-of-the-rwjf-summer-medical-and-dental-education-program-smdep (Accessed February 11, 2023).
Curfman, G. (2022). A new supreme court challenge to affirmative action in university admissions. JAMA Health Forum 3:e220767. doi: 10.1001/jamahealthforum.2022.0767
Davis, D., Dorsey, J. K., Franks, R. D., Sackett, P. R., Searcy, C. A., and Zhao, X. (2013). Do racial and ethnic group differences in performance on the MCAT exam reflect test Bias? Acad. Med. 88, 593–602. doi: 10.1097/ACM.0b013e318286803a
Dickins, K., Levinson, D., Smith, S. G., and Humphrey, H. J. (2013). The minority student voice at one medical school: lessons for all? Acad. Med. 88, 73–79. doi: 10.1097/ACM.0b013e3182769513
Dill, M. (2021). We already needed more doctors. Then Covid-19 hit [online]. Washington, DC. Available at: https://www.aamc.org/news-insights/we-already-needed-more-doctors-then-covid-19-hit (Accessed December 21 2022).
Echegoyen, L. E., Aley, S. B., Garza, J. P., Ramos, C., Oviedo, S. L., and Corral, G. (2019). Impact of open enrollment in course-based undergraduate research experiences with at-risk student populations. EDULEARN Proc 2019, 6580–6588.
Fenton, J. J., Fiscella, K., Jerant, A. F., Sousa, F., Henderson, M., Fancher, T., et al. (2016). Reducing medical school admissions disparities in an era of legal restrictions: adjusting for applicant socioeconomic disadvantage. J. Health Care Poor Underserved 27, 22–34. doi: 10.1353/hpu.2016.0013
Freeman, B. K., Landry, A., Trevino, R., Grande, D., and Shea, J. A. (2016). Understanding the leaky pipeline: perceived barriers to pursuing a career in medicine or dentistry among underrepresented-in-medicine undergraduate students. Acad. Med. 91, 987–993. doi: 10.1097/ACM.0000000000001020
Frogner, B. K., and Dill, J. S. (2022). Tracking turnover among health care workers during the COVID-19 pandemic: a cross-sectional study. JAMA Health Forum 3:e220371. doi: 10.1001/jamahealthforum.2022.0371
Garces, L. M., and Mickey-Pabello, D. (2015). Racial diversity in the medical profession: the impact of affirmative action bans on underrepresented student of color matriculation in medical schools. J. Furth. High. Educ. 86, 264–294. doi: 10.1353/jhe.2015.0009
Ghaffari-Rafi, A., Lee, R. E., Fang, R., and Miles, J. D. (2019). Multivariable analysis of factors associated with USMLE scores across U.S. medical schools. BMC Med. Educ. 19:154. doi: 10.1186/s12909-019-1605-z
Giordani, B., Edwards, A. S., Segal, S. S., Gillum, L. H., Lindsay, A., and Johnson, N. (2001). Effectiveness of a formal post-baccalaureate pre-medicine program for underrepresented minority students. Acad. Med. 76, 844–848. doi: 10.1097/00001888-200108000-00020
Girotti, J. A., Chanatry, J. A., Clinchot, D. M., Mcclure, S. C., Swan Sein, A., Walker, I. W., et al. (2020). Investigating group differences in Examinees' preparation for and performance on the new MCAT exam. Acad. Med. 95, 365–374. doi: 10.1097/ACM.0000000000002940
Girotti, J. A., Park, Y. S., and Tekian, A. (2015). Ensuring a fair and equitable selection of students to serve Society's health care needs. Med. Educ. 49, 84–92. doi: 10.1111/medu.12506
Glazer, G., Bankston, K., Clark, A., and Ying, J. (2014). “Holistic admission in the health professions: findings from a National Survey.” Urban Universities for Health Report [Online]. Available at: https://www.aplu.org/wp-content/uploads/holistic-admissions-in-the-health-professions.pdf (Accessed March 12, 2020).
Goode, C. A., and Landefeld, T. (2018). The lack of diversity in healthcare: causes, consequences, and solutions. J. Best Pract. Health Profess. Divers. Educ. Res. Policy 11, 73–95.
Goode, C. A., and Talbot, C. (2016). A Special Master’s program as a pipeline to increase diversity at an osteopathic medical college. J. Best Pract. Health Profess. Divers. Educ. Res. Policy 9, 1198–1216.
Grbic, D., Jones, D. J., and Case, S. T. (2015). The role of socioeconomic status in medical school admissions: validation of a socioeconomic Indicator for use in medical school admissions. Acad. Med. 90, 953–960. doi: 10.1097/ACM.0000000000000653
Grbic, D., Morrison, E., Sondheimer, H. M., Conrad, S. S., and Milem, J. F. (2019). The association between a holistic review in admissions workshop and the diversity of accepted applicants and students matriculating to medical school. Acad. Med. 94, 396–403. doi: 10.1097/ACM.0000000000002446
Grbic, D., and Roskovensky, L. B. (2012). Which factors predict the likelihood of reapplying to medical school? An analysis by gender. Acad. Med. 87, 449–457. doi: 10.1097/ACM.0b013e3182494e54
Grumbach, K., and Chen, E. (2006). Effectiveness of University of California Postbaccalaureate Premedical Programs in increasing medical school matriculation for minority and disadvantaged students. JAMA 296, 1079–1085. doi: 10.1001/jama.296.9.1079
Grumbach, K., Coffman, J., Rosenoff, E., and Muñoz, C. (2001). “Trends in underrepresented minority participation in health professions schools,” in The right thing to do, the smart thing to do enhancing diversity in the health professions. Summary of the symposium on diversity in health professions in honor of Herbert W. Nickens, M.D. (eds.) B.D. Smedley, A.Y. Stith, L. Colburn and C.H. Evans. Washington, DC, National Academy Press.
Hayes-Bautista, D. E., Hsu, P., Hayes-Bautista, M., Stein, R. M., Dowling, P., Beltran, R., et al. (2000). Latino physician supply in California: sources, locations, and projections. Acad. Med. 75, 727–736. doi: 10.1097/00001888-200007000-00018
Jacobs, N. N., Esquierdo-Leal, J., Smith, G. S., Piasecki, M., and Houmanfar, R. A. (2022). Diversifying academic medicine: one search committee at a time. Front. Public Health 10:854450. doi: 10.3389/fpubh.2022.854450
Jones, A. C., Nichols, A. C., McNicholas, C. M., and Stanford, F. C. (2021). Admissions is not enough: the racial achievement gap in medical education. Acad. Med. 96, 176–181. doi: 10.1097/ACM.0000000000003837
Joseph, J., Dao, D., Hwang, S. M., Dotzler, S. M., Chesak, S. S., Weiskittel, T. M., et al. (2021). Perceptions of barriers and facilitators to becoming a medical professional among underrepresented undergraduate and Postbaccalaureate learners. Mayo Clin. Proc. Innov. Q. Outcomes 5, 347–358. doi: 10.1016/j.mayocpiqo.2021.01.003
Joseph, O. R., Flint, S. W., Raymond-Williams, R., Awadzi, R., and Johnson, J. (2021). Understanding healthcare Students' experiences of racial Bias: a narrative review of the role of implicit Bias and potential interventions in educational settings. Int. J. Environ. Res. Public Health 18. doi: 10.3390/ijerph182312771
Kadavakollu, S., Lund, K. S., Swamy, V., Kim, W. D., Llenado, R. A., Nunes, T. F., et al. (2022). Promoting cultural competency and osteopathic medicine awareness among premedical students through a summer premedical rural enrichment program. J. Osteopath. Med. 122, 553–561. doi: 10.1515/jom-2022-0002
Ko, M., Henderson, M. C., Fancher, T. L., London, M. R., Simon, M., and Hardeman, R. R. (2023). US medical school admissions Leaders' experiences with barriers to and advancements in diversity, equity, and inclusion. JAMA Netw. Open 6:e2254928. doi: 10.1001/jamanetworkopen.2022.54928
Koenig, J. A., Sireci, S. G., and Wiley, A. (1998). Evaluating the predictive validity of MCAT scores across diverse applicant groups. Acad. Med. 73, 1095–1106. doi: 10.1097/00001888-199810000-00021
Komaromy, M., Grumbach, K., Drake, M., Vranizan, K., Lurie, N., Keane, D., et al. (1996). The role of Black and Hispanic physicians in providing health Care for Underserved Populations. N. Engl. J. Med. 334, 1305–1310. doi: 10.1056/NEJM199605163342006
Kosobuski, A. W., Whitney, A., Skildum, A., and Prunuske, A. (2017). Development of an interdisciplinary pre-matriculation program designed to promote medical Students' self efficacy. Med. Educ. Online 22:1272835. doi: 10.1080/10872981.2017.1272835
Kuczewski, M., and Brubaker, L. (2014). Medical education for "dreamers": barriers and opportunities for undocumented immigrants. Acad. Med. 89, 1593–1598. doi: 10.1097/ACM.0000000000000399
Larson, E. H., and Frogner, B. K. (2019). Characteristics of physician assistant students planning to work in primary care: a National Study. J. Phys. Assist. Educ. 30, 200–206. doi: 10.1097/JPA.0000000000000275
Laurencin, C. T., and Murray, M. (2017). An American crisis: the lack of black men in medicine. J. Racial Ethn. Health Disparities 4, 317–321. doi: 10.1007/s40615-017-0380-y
Lige, Q. M., Peteet, B. J., and Brown, C. M. (2017). Racial identity, self-esteem, and the impostor phenomenon among African American college students. J. Black Psychol. 43, 345–357. doi: 10.1177/0095798416648787
Lupton, K., Vercammen-Grandjean, C., Forkin, J., Wilson, E., and Grumbach, K. (2012). Specialty choice and practice location of physician alumni of University of California premedical Postbaccalaureate programs. Acad. Med. 87, 115–120. doi: 10.1097/ACM.0b013e31823a907f
MacPhee, D., Farro, S., and Canetto, S. S. (2013). Academic self-efficacy and performance of underrepresented STEM majors: gender, ethnic, and social class patterns. Anal. Soc. Issues Public Policy 13, 347–369. doi: 10.1111/asap.12033
Mason, H. R. C., Ata, A., Nguyen, M., Nakae, S., Chakraverty, D., Eggan, B., et al. (2022). First-generation and continuing-generation college graduates' application, acceptance, and matriculation to U.S. medical schools: a National Cohort Study. Med. Educ. 27:2010291. doi: 10.1080/10872981.2021.2010291
McClain, S., Beasley, S. T., Jones, B., Awosogba, O., Jackson, S., and Cokley, K. (2016). An examination of the impact of racial and ethnic identity, impostor feelings, and minority status stress on the mental health of black college students. J. Multicult. Couns. Dev. 44, 101–117. doi: 10.1002/jmcd.12040
McGee, E. O., Botchway, P. K., Naphan-Kingery, D. E., Brockman, A. J., Houston, S., and White, D. T. (2021). Racism camouflaged as Impostorism and the impact on black STEM doctoral students. Race Ethn. Educ. 25, 487–507. doi: 10.1080/13613324.2021.1924137
McNeill, K. G., Kerr, A., and Mavor, K. I. (2014). Identity and norms: the role of group membership in medical student wellbeing. Perspect. Med. Educ. 3, 101–112. doi: 10.1007/S40037-013-0102-Z
Michalec, B., and Hafferty, F. W. (2023). Examining the U.S. premed path as an example of discriminatory design & exploring the role(s) of capital. Soc. Theory Health 21, 70–97. doi: 10.1057/s41285-022-00175-7
Miller, C. J. (2014). Implementation of a study skills program for entering at-risk medical students. Adv. Physiol. Educ. 38, 229–234. doi: 10.1152/advan.00022.2014
Mindlis, I., Livert, D., Federman, A. D., Wisnivesky, J. P., and Revenson, T. A. (2020). Racial/ethnic concordance between patients and researchers as a predictor of study attrition. Soc. Sci. Med. 255:113009. doi: 10.1016/j.socscimed.2020.113009
Morgan Consoli, M. L., Delucio, K., Noriega, E., and Llamas, J. (2015). Predictors of resilience and thriving among Latina/o undergraduate students. Hisp. J. Behav. Sci. 37, 304–318. doi: 10.1177/0739986315589141
Morgan, H. K., Haggins, A., Lypson, M. L., and Ross, P. (2016). The importance of the premedical experience in diversifying the health care workforce. Acad. Med. 91, 1488–1491. doi: 10.1097/ACM.0000000000001404
Morris, D. B., Gruppuso, P. A., McGee, H. A., Murillo, A. L., Grover, A., and Adashi, E. Y. (2021). Diversity of the National Medical Student Body—four decades of inequities. N. Engl. J. Med. 384, 1661–1668. doi: 10.1056/NEJMsr2028487
Mushonga, D. R., and Henneberger, A. K. (2020). Protective factors associated with positive mental health in traditional and nontraditional black students. Am. J. Orthop. 90, 147–160. doi: 10.1037/ort0000409
Nadal, K. L., King, R., Sissoko, D. R. G., Floyd, N., and Hines, D. (2021). The legacies of systemic and internalized oppression: experiences of microaggressions, imposter phenomenon, and stereotype threat on historically marginalized groups. New Ideas Psychol. 63:100895. doi: 10.1016/j.newideapsych.2021.100895
Nakae, S., and Subica, A. M. (2021). Academic redlining in medicine. J. Natl. Med. Assoc. 113, 587–594. doi: 10.1016/j.jnma.2021.05.008
Nalliah, R. P., Timothe, P., and Reddy, M. S. (2021). Diversity, equity, and inclusion interventions to support admissions have had little benefit to black students over past 20 years. J. Dent. Educ. 85, 448–455. doi: 10.1002/jdd.12611
Nickens, H. W., Ready, T. P., and Petersdorf, R. G. (1994). Project 3000 by 2000. Racial and ethnic diversity in U.S. N. Engl. J. Med. 331, 472–476. doi: 10.1056/NEJM199408183310712
Odom, K. L., Roberts, L. M., Johnson, R. L., and Cooper, L. A. (2007). Exploring obstacles to and opportunities for professional success among ethnic minority medical students. Acad. Med. 82, 146–153. doi: 10.1097/ACM.0b013e31802d8f2c
Orfield, G., Frankenberg, E., Ee, J., and Ayscue, J. (2019). Harming our common future: America’s segregated schools 65 years after Brown. [online]. Available at: https://escholarship.org/uc/item/23j1b9nv (Accessed March 29, 2023).
Page, M. J., Moher, D., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., et al. (2021). Prisma 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ 372:n160. doi: 10.1136/bmj.n160
Peteet, B. J., Brown, C. M., Lige, Q. M., and Lanaway, D. A. (2015a). Impostorism is associated with greater psychological distress and lower self-esteem for African American students. Curr. Psychol. 34, 154–163. doi: 10.1007/s12144-014-9248-z
Peteet, B. J., Montgomery, L., and Weekes, J. C. (2015b). Predictors of imposter phenomenon among talented ethnic minority undergraduate students. J. Negro Educ. 84, 175–186. doi: 10.7709/jnegroeducation.84.2.0175
Petersdorf, R. G. (1992). Not a choice, an obligation. Acad. Med. 67, 73–79. doi: 10.1097/00001888-199202000-00003
Pfeffinger, A., Fernández, A., Tapia, M., Rios-Fetchko, F., and Coffman, J. (2020). Recovery with limited progress: Impact of California proposition 209 on racial/ethnic diversity of California medical school matriculants, 1990 to 2019. Available at: https://healthforce.ucsf.edu/publications/recovery-limited-progress-impact-california-proposition-209-racialethnic-diversity (Accessed December 12, 2022).
Poll-Hunter, N. I., Brown, Z., Smith, A., Starks, S. M., Gregory-Bass, R., Robinson, D., et al. (2023). Increasing the representation of Black men in medicine by addressing systems factors. Acad. Med. 98, 304–312. doi: 10.1097/ACM.0000000000005070
Porter, S. R., Jones, M. R., Hendren, N., and Chetty, R. (2020). Race and economic opportunity in the United States: an intergenerational perspective. Q. J. Econ. 135, 711–783. doi: 10.1093/qje/qjz042
Ramos, D., and Wright-Mair, R. (2021). Imposter syndrome: a buzzword with damaging consequences. Diverse Issues in Higher Education [Online]. Available at: https://www.diverseeducation.com/tenure/article/15109066/imposter-syndrome-a-buzzword-with-damaging-consequences (Accessed December 15, 2022).
Reardon, S. F. (2016). School segregation and racial academic achievement gaps. RSF: the Russell Sage Foundation. J. Soc. Sci. 2, 34–57. doi: 10.7758/RSF.2016.2.5.03
Robinett, K., Kareem, R., Reavis, K., and Quezada, S. (2021). A multi-pronged, antiracist approach to optimize equity in medical school admissions. Med. Educ. 55, 1376–1382. doi: 10.1111/medu.14589
Roche, R., Manzi, J., Baker, S., and Ndubuizu, T. (2021a). Under-represented minority students and identification of obstacles to a career in medicine. Clin. Teach. 18, 186–190. doi: 10.1111/tct.13312
Roche, R., Manzi, J., and Kruithoff, B. C. (2021b). The benefits of being a "buddy": exploring the medical student experience as mentor to minority high-school students. Health Equity 5, 1–7. doi: 10.1089/heq.2020.0060
Roche, R., Manzi, J., Ndubuizu, T., and Baker, S. (2020). Self-efficacy as an Indicator for success in a premedical curriculum for underrepresented minority high school students. J. Med. Educ. Curric. Dev. 7:238212052094066. doi: 10.1177/2382120520940661
Rodriguez, J. E., and Campbell, K. M. (2015). Does the continued use of the MCAT hinder care for minority patients? J. Immigr. Minor. Health 17, 981–982. doi: 10.1007/s10903-014-0054-3
Sanchez, G., Nevarez, T., Schink, W., and Hayes-Bautista, D. E. (2015). Latino physicians in the United States, 1980-2010: a thirty-year overview from the censuses. Acad. Med. 90, 906–912. doi: 10.1097/ACM.0000000000000619
Schneid, S. D., Fricovsky, E. S., Loehr, P. G., and Kim, J. G. (2022a). A pipeline for health systems science in Postbaccalaureate premedical programmes. Med. Educ. 56, 568–569. doi: 10.1111/medu.14757
Schneid, S. D., Kelly, C. J., and Brandl, K. (2022b). Relationships between preadmission variables and academic outcomes for Postbaccalaureate students in medical school. Adv. Health Sci. Educ. Theory Pract. 27, 1033–1048. doi: 10.1007/s10459-022-10129-3
Schoenthaler, A., and Ravenell, J. (2020). Understanding the patient experience through the lenses of racial/ethnic and gender patient-physician concordance. JAMA Netw. Open 3:e2025349. doi: 10.1001/jamanetworkopen.2020.25349
Smedley, B., Stith, A., and Nelson, A., Institute of Medicine (US) Committee on Understanding and Eliminating Racial and Ethnic Disparities in Health Care (2003). Unequal treatment: Confronting racial and ethnic disparities in health care. Washington (DC), National Academies Press (US).
Steinecke, A., and Terrell, C. (2008). “After affirmative action: diversity at California medical schools” in Analysis in Brief. Washington, DC, American Association of Medical Colleges.
Stone, S., Saucer, C., Bailey, M., Garba, R., Hurst, A., Jackson, S. M., et al. (2018). Learning while black: a culturally informed model of the impostor phenomenon for black graduate students. J. Black Psychol. 44, 491–531. doi: 10.1177/0095798418786648
Street, R. L., O'Malley, K. J., Cooper, L. A., and Haidet, P. (2008). Understanding concordance in patient-physician relationships: personal and ethnic dimensions of shared identity. Ann. Fam. Med. 6, 198–205. doi: 10.1370/afm.821
Strowd, L. C., Gao, H., Obrien, M. C., Burns, C., Freischlag, J. A., Strowd, R. E., et al. (2020). Prematriculation healthcare employment predicts success in clerkship environment. Med. Sci. Educ. 30, 211–217. doi: 10.1007/s40670-019-00859-2
Strumpf, E. C. (2011). Racial/ethnic disparities in primary care: the role of physician-patient concordance. Med. Care 49, 496–503. doi: 10.1097/MLR.0b013e31820fbee4
Sullivan, L. W. (2011). “Introduction: an overview of the US healthcare system and US health disparities at the beginning of the twenty-first century” in Healthcare Disparities at the Crossroads With Healthcare Reform. ed. R. A. Williams (New York, NY: Springer), 3–6.
Takeshita, J., Wang, S., Loren, A. W., Mitra, N., Shults, J., Shin, D. B., et al. (2020). Association of racial/ethnic and gender concordance between patients and physicians with patient experience ratings. JAMA Netw. Open 3:e2024583. doi: 10.1001/jamanetworkopen.2020.24583
Talamantes, E., Mangione, C. M., Gonzalez, K., Jimenez, A., Gonzalez, F., and Moreno, G. (2014). Community college pathways: improving the U.S. Acad. Med. 89, 1649–1656. doi: 10.1097/ACM.0000000000000438
Tao, K. W., and Gloria, A. M. (2019). Should I stay or should I go? The role of imposterism in STEM persistence. Psychol. Women Q. 43, 151–164. doi: 10.1177/0361684318802333
Terregino, C. A., Saguil, A., Price-Johnson, T., Anachebe, N. F., and Goodell, K. (2020). The diversity and success of medical school applicants with scores in the middle third of the MCAT score scale. Acad. Med. 95, 344–350. doi: 10.1097/ACM.0000000000002941
Thomas, B. R., and Dockter, N. (2019). Affirmative action and holistic review in medical school admissions: where we have been and where we are going. Acad. Med. 94, 473–476. doi: 10.1097/ACM.0000000000002482
Thurmond, V. B., and Cregler, L. L. (1996). College majors and career choices of minority high school student research apprentices. J. Assoc. Acad. Minor. Phys. 7, 22–24.
Toretsky, C., Mutha, S., and Coffman, J. (2018). Breaking barriers for underrepresented minorities in the health professions. Available at: https://healthforce.ucsf.edu/publications/breaking-barriers-underrepresented-minorities-health-professions (Accessed December 21, 2022).
Turan, S., Valcke, M., Aper, L., Koole, S., and Derese, A. (2013). Studying self-efficacy beliefs in medical education. Procedia Soc. Behav. Sci. 93, 1311–1314. doi: 10.1016/j.sbspro.2013.10.034
U.S. Census Bureau (2021). Population estimates, July 2021 [online]. Available at: https://www.census.gov/quickfacts/fact/dashboard/US/RHI225221#RHI225221 (Accessed December 15 2022).
Upshur, C. C., Wrighting, D. M., Bacigalupe, G., Becker, J., Hayman, L., Lewis, B., et al. (2018). The health equity scholars program: innovation in the leaky pipeline. J. Racial Ethn. Health Disparities 5, 342–350. doi: 10.1007/s40615-017-0376-7
Xu, G., Fields, S. K., Laine, C., Veloski, J. J., Barzansky, B., and Martini, C. J. (1997). The relationship between the race/ethnicity of generalist physicians and their care for underserved populations. Am. J. Public Health 87, 817–822. doi: 10.2105/AJPH.87.5.817
Yelorda, K., Bidwell, S., Fu, S., Miller, M. O., Merrell, S. B., Koshy, S., et al. (2021). Self-efficacy toward a healthcare career among minority high school students in a surgical pipeline program: a mixed methods study. J. Surg. Educ. 78, 1896–1904. doi: 10.1016/j.jsurg.2021.04.010
Youngclaus, J., and Fresne, J.A. (2020). Physician education debt and the cost to attend medical school: 2020 update [online]. Washington, DC: AAMC. Available at: https://store.aamc.org/downloadable/download/sample/sample_id/368/ (Accessed December 12 2022).
Youngclaus, J., and Roskovensky, L. (2018). An Updated Look at the Economic Diversity of U.S. Medical Students, in: Analysis in Brief. Washington, DC: Association of American Medical Colleges.
Zhang, X., Lin, D., Pforsich, H., and Lin, V. W. (2020). Physician workforce in the United States of America: forecasting nationwide shortages. Hum. Resour. Health 18:8. doi: 10.1186/s12960-020-0448-3
Keywords: underrepresented, underrepresented in medicine (URiM), diversity, matriculation, professional school, impostor phenomenon, self-efficacy, barriers
Citation: Tello C and Goode CA (2023) Factors and barriers that influence the matriculation of underrepresented students in medicine. Front. Psychol. 14:1141045. doi: 10.3389/fpsyg.2023.1141045
Edited by:
Mark Guiberson, University of Wyoming, United StatesReviewed by:
William Burton, Albert Einstein College of Medicine, United StatesLeon McDougle, The Ohio State University, United States
Copyright © 2023 Tello and Goode. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Christine A. Goode, Y2dvb2RlQHdlc3Rlcm51LmVkdQ==
 Cynthia Tello1,2
Cynthia Tello1,2 Christine A. Goode
Christine A. Goode