
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Public Health , 02 April 2025
Sec. Aging and Public Health
Volume 13 - 2025 | https://doi.org/10.3389/fpubh.2025.1569119
This article is part of the Research Topic Atopic March and Atopic Multimorbidity View all 6 articles
Background: With the aging global population, older adult atopic dermatitis (AD) is emerging as an increasingly significant health challenge. This study aimed to evaluate the global burden of older adult AD from 1990 to 2021 and to project its change to 2050.
Methods: The estimates and 95% uncertainty intervals of prevalence, incidence, and disability-adjusted life-years (DALYs) attributable to AD among individuals aged over 60 years were extracted from the Global Burden of Diseases (GBD) Study 2021. We used joinpoint regression analysis, decomposition analysis, cross-country inequality analysis, frontier analysis and prediction model to epidemiological analysis.
Results: From 1990 to 2021, the global prevalence of older adult AD increased to 11,009,630 cases (95% UI: 9,915,829 to 12,170,941), even as ASRs declined, which were primarily driven by population growth. It was observed that females and 75–79 years old had higher incidence rates. SDI relative and frontier analysis exhibited that incidence, prevalence and DALYs rates were positively correlated with SDI levels, while SDI-related inequalities had a significant decrease. Predictions up to 2050 anticipated increasing older adult AD incidence, prevalence, and DALYs numbers, while only age-standardized disability-adjusted life-year rates (ASDRs) were expected to decline.
Conclusion: The burden of older adult AD varied by genders, age groups, regions, countries and climatic conditions. Although the ASRs had shown a decline over time, the burden of older adult AD remained significant, especially in regions with high SDI levels. In the future, the burden of older adult AD was projected to continue rising until 2050, thereby targeted interventions and public health strategies were needed to address this trend.
Atopic dermatitis (AD) is a chronic inflammatory skin disease primarily characterized by dry, itchy, and eczematous skin (1), significantly impacting individual social interactions and quality of life. AD arises in genetically susceptible individuals when environmental factors interact with compromised skin barrier function, leading to immune dysregulation (2). It’s the heaviest burden among skin diseases, affecting at least 230 million people globally (3). While AD is commonly observed in childhood, it can have long-term effects into adulthood. As aging intensifies, the older adult AD gradually attracts more and more attention. Among the older adult, trunk involvement is more common, and the percentage of moderate to severe AD is higher (4), which has a huge impact on their quality of life and disease burden. In addition, due to the uniqueness of the older adult population, they often have more comorbidities and are prone to worsening due to systemic medication for AD. Although children represent a key population for AD prevention and treatment, the condition in the older adult cannot be overlooked. Compared with young AD patients, decreased barrier functionalities due to aging may elevate the vulnerability to environmental stimuli, potentially resulting in systemic sensitization and predisposing older adult individuals with AD to type 2 immune reactions (5, 6). Therefore, it’s important to present the burden estimates for older adult AD.
The Global Burden of Diseases (GBD) dataset is recognized as a potent tool widely utilized in disease burden research (7–9). Currently, there is a lack of detailed global burden information specific to AD in the older adult. Therefore, our objective is to analyze the GBD database to report the global, regional, and national burdens and trends related to older adult AD from 1990 to 2021, encompassing prevalence, incidence, and disability-adjusted life years (DALYs). Furthermore, we also discuss the spatiotemporal trends associated with socioeconomic development at the national level and forecast these three indicators until 2050, which inform future public health interventions.
The GBD 2021 study offers an exhaustive evaluation of health losses due to 371 diseases, injuries, and impairments across 204 countries and regions. It employs the latest epidemiological data and advanced standardized methodologies (10). The GBD database uses advanced techniques to handle missing data and correct for confounding variables. Comprehensive descriptions of the study design and methodologies of GBD studies can be found in the existing GBD literature (10). The Global Health Data Exchange query tool1 provides access to the data.
We sought data from the GBD study tool on incidence, prevalence, and disability-adjusted life years (DALYs) of AD in people aged 60 years and older from 1990 to 2021. To facilitate a significant comparison of rates across various global populations, age standardization was employed in the GBD study to adjust a country’s prevalence rates for different risk factors against a consistent standard population. Disability-adjusted life years (DALYs) quantified the aggregate healthy years forfeited from disease onset to demise, which were determined by summing the years lived with disability (YLDs) and the years of life lost (YLLs). YLDs were derived by multiplying the patient’s count by the time until remission or demise, incorporating the disability weight. YLLs were figured by multiplying the death toll by the standard life expectancy from a reference table. Furthermore, we also included a socio-demographic index (SDI) for analyzing the correlation between diseases and development levels, which was a comprehensive metric encompassing income, education, and fertility, and measuring the sociodemographic advancement level of a nation or region (11).
The burden of older adult AD was measured across different periods and segmented by region, nation, SDI, sex, and age, employing absolute numbers and age-standardized rates (ASRs) with their 95% uncertainty interval (UI). Within the GBD database, these metrics were derived based on the global population’s age distribution, determined by a specific formula: (ai: the age-specific rate in the ith age group; w i : the number of people in the corresponding i-th age group among the standard population; A: the number of age groups). These initiatives considered variations in the demographic age structures of populations. The objective of age standardization was to mitigate the influence of demographic age structures and facilitate the comparability of research metrics. In addition, we used a joinpoint regression model (selecting the log-linear model: lny = xb) to assess rates trend (12). This model allowed us to compute the annual percent change (APC) along with its 95% confidence interval (CI), and illustrate the trend across the specified time period. Subsequently, we derived the average annual percent change (AAPC) by analyzing the trend of APC. To evaluate the correlations between the SDI and age-standardized older adult AD rates, we utilized the Spearman correlation coefficient, and statistical significance was set at p < 0.05. In order to gain deeper insights into the explanatory factors influencing older adult AD burden from 1990 to 2021, decomposition analyses were conducted, taking into account population size, age structure, and epidemiological shifts (13). Moreover, to examine the relationship between older adult AD burden and sociodemographic development levels, we employed frontier analysis and cross-country inequality analysis to quantify the distributive inequality of older adult AD burden across nations, in which the slope index of inequality and the concentration index represent absolute and relative gradient inequality, respectively. Additionally, we projected future trends in older adult AD burden using a Bayesian age-period-cohort (BAPC) model, incorporating integrated nested Laplace approximations. Data analysis was conducted using R software, specifically version 4.3.3.
In 2021, older adult AD continued to pose a significant global burden, totaling 11,009,630 cases (95% UI: 9,915,829 to 12,170,941), with a remarkable 106.98% increase since 1990 (Table 1). Notably, despite this substantial increase in case numbers, the age-standardized prevalence rates (ASPRs) exhibited a slight decline, from 1117.11 cases per 100,000 population (95% UI: 1005.84 to 1234.26) in 1990 to 1016.99 cases per 100,000 population (95% UI: 915.91 to 1124.40) in 2021.
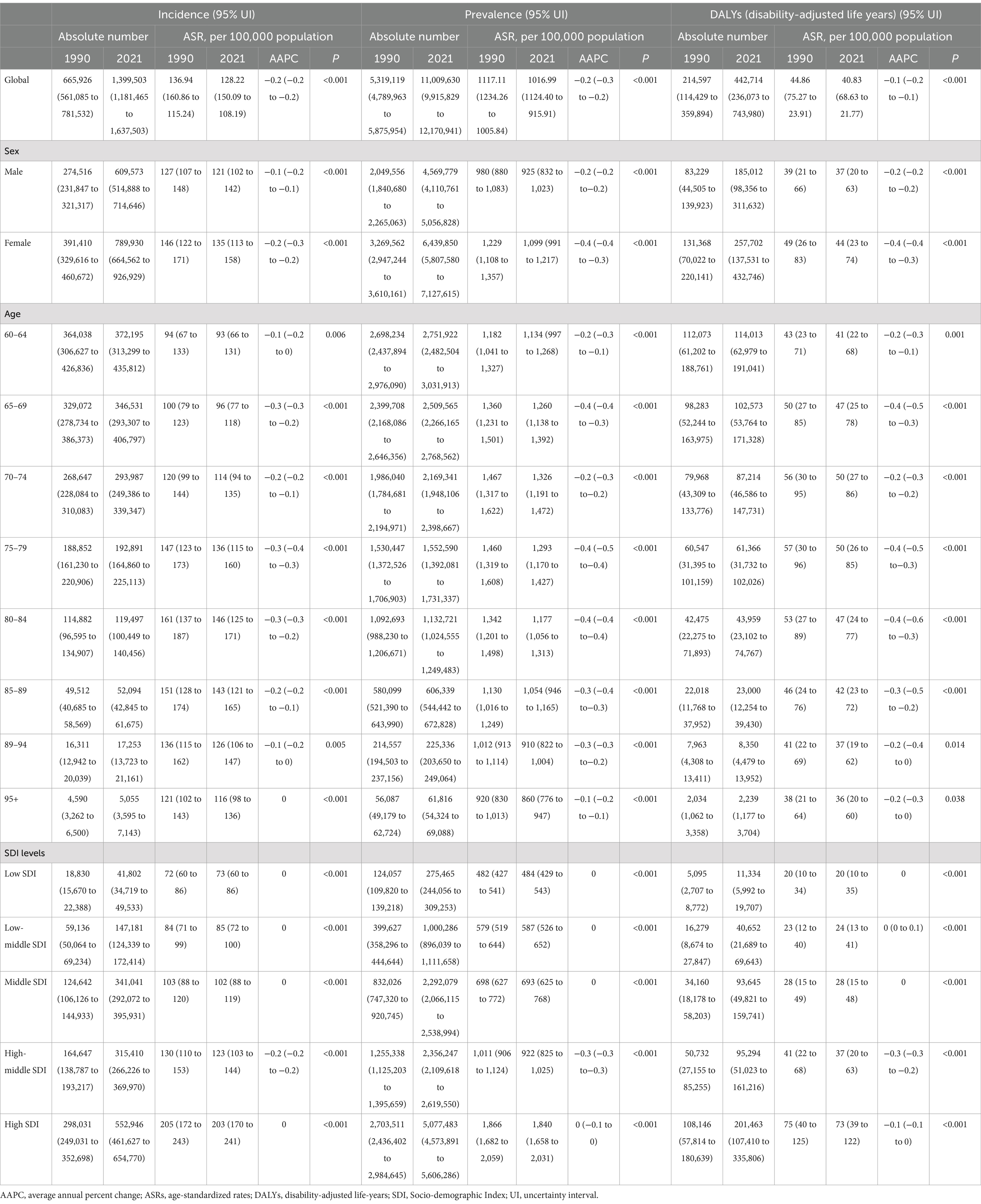
Table 1. Numbers and ASRs per 100,000 cases of incidence, prevalence and DALYs of older adult atopic dermatitis in 1990 and 2021, along with the AAPC in ASRs per 100,000 cases from 1990 to 2021, categorized by global, sex, age and SDI regions.
Regarding incidence, the global number of new older adult AD cases reached 1,399,503 in 2021 (95% UI: 1,181,465 to 1,637,503), representing a 110.16% surge compared to 1990. The age-standardized incidence rates (ASIRs) of older adult AD declined from 136.94 cases per 100,000 people (95% UI: 115.24 to 160.86) in 1990 to 128.22 cases per 100,000 (95% UI: 108.19 to 150.09) in 2021.
Furthermore, the DALYs due to older adult AD in 2021 amounted to 442,714 (95% UI: 236,073 to 743,980), with an age-standardized disability-adjusted life-year rates (ASDRs) of 40.83 per 100,000 population (95% UI: 21.77 to 68.63) and an AAPC of −0.1% (95% CI: −0.2 to −0.1). Notably, incidence, prevalence, and DALY rates exhibited a consistent downward trend with AAPCs < 0% (Figure 1).
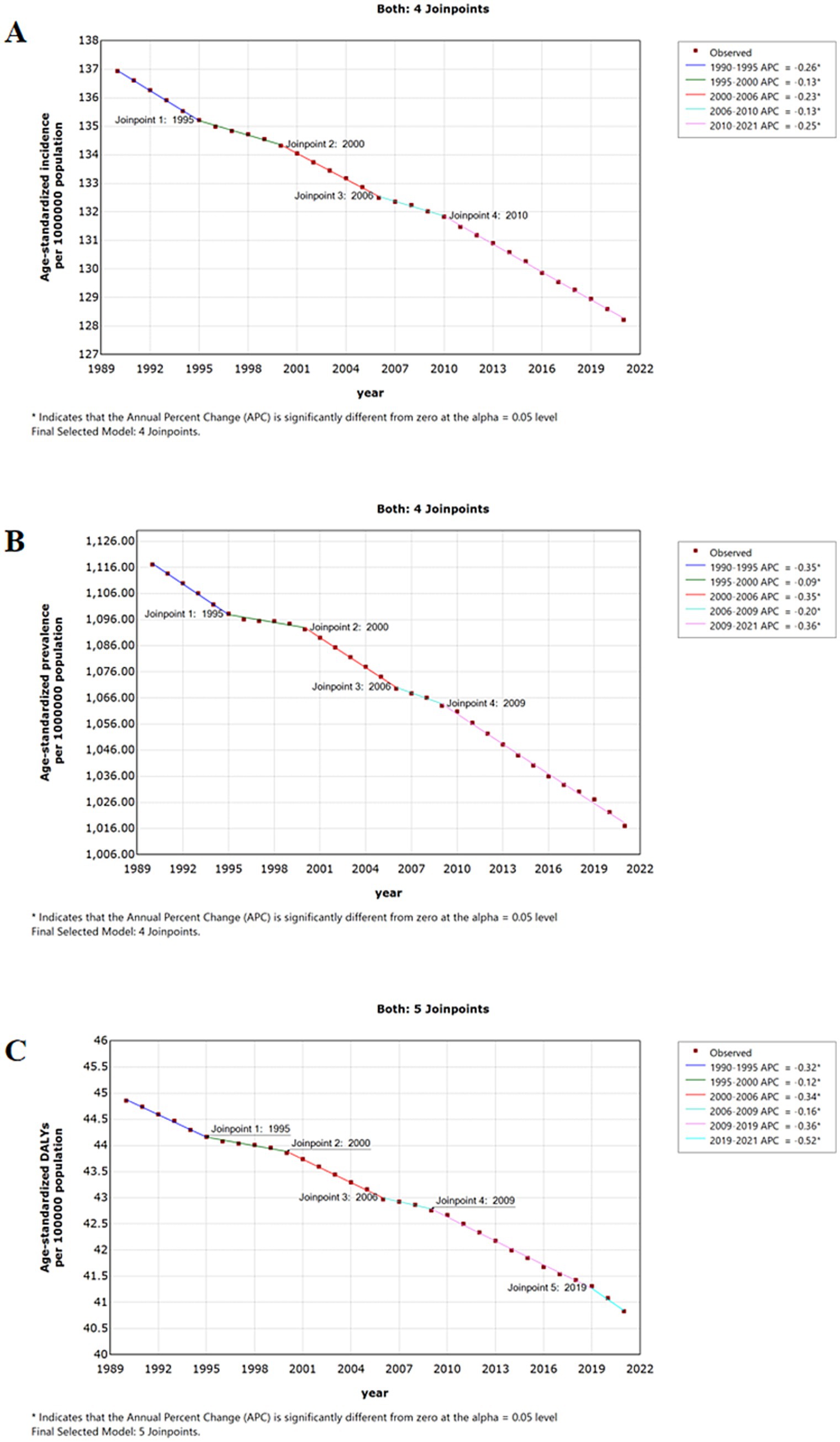
Figure 1. Jointpoint regression analysis of global incidence (A), prevalence (B) and DALYs (C) of older adult atopic dermatitis from 1990 to 2021. DALYs, disability-adjusted life-years.
In 2021, globally, the number of older adult AD cases amounted to 4,569,779 in males and 6,439,850 in females, with females being more affected (Table 1). Although the rates of both genders displayed comparable downward trends between 1990 and 2021, females consistently maintained higher rates across all categories. However, sex-specific analysis of older adult AD incidence, prevalence, and DALYs revealed a slight decline in ASRs from 1990 to 2021, with AAPCs approaching 0%.
Incidence of older adult AD increased, with a particularly sharp rise between the ages of 75–79. Similarly, prevalence rates climbed with age, peaking in the 85–89 age bracket. The trend in DALYs followed a similar pattern, reaching its maximum in the 80–84 age group. Across these metrics, females consistently demonstrated slightly higher rates than males in all age categories (Supplementary Figure S1).
Predominantly, the majority of older adult AD cases, including incidence, prevalence, and DALYs, were concentrated in regions with high SDI levels. Upon examining older adult AD indicators across 21 regions, a positive association with SDI became apparent. Specifically, ASRs for incidence, prevalence, and DALYs exhibited robust positive correlations with SDI levels (R = 0.673, p < 0.001; R = 0.659, p < 0.001; R = 0.660, p < 0.001). Notably, eight regions, such as Southern Latin America, Tropical Latin America, and Eastern Europe, surpassed the global averages for prevalence, incidence, and DALYs (Supplementary Figure S2). Consistently, a broader examination encompassing 204 countries and territories reinforced that ASRs for incidence, prevalence, and DALYs positively correlated with SDI levels (R = 0.593, p < 0.001; R = 0.556, p < 0.001; R = 0.555, p < 0.001), respectively (Figure 2).
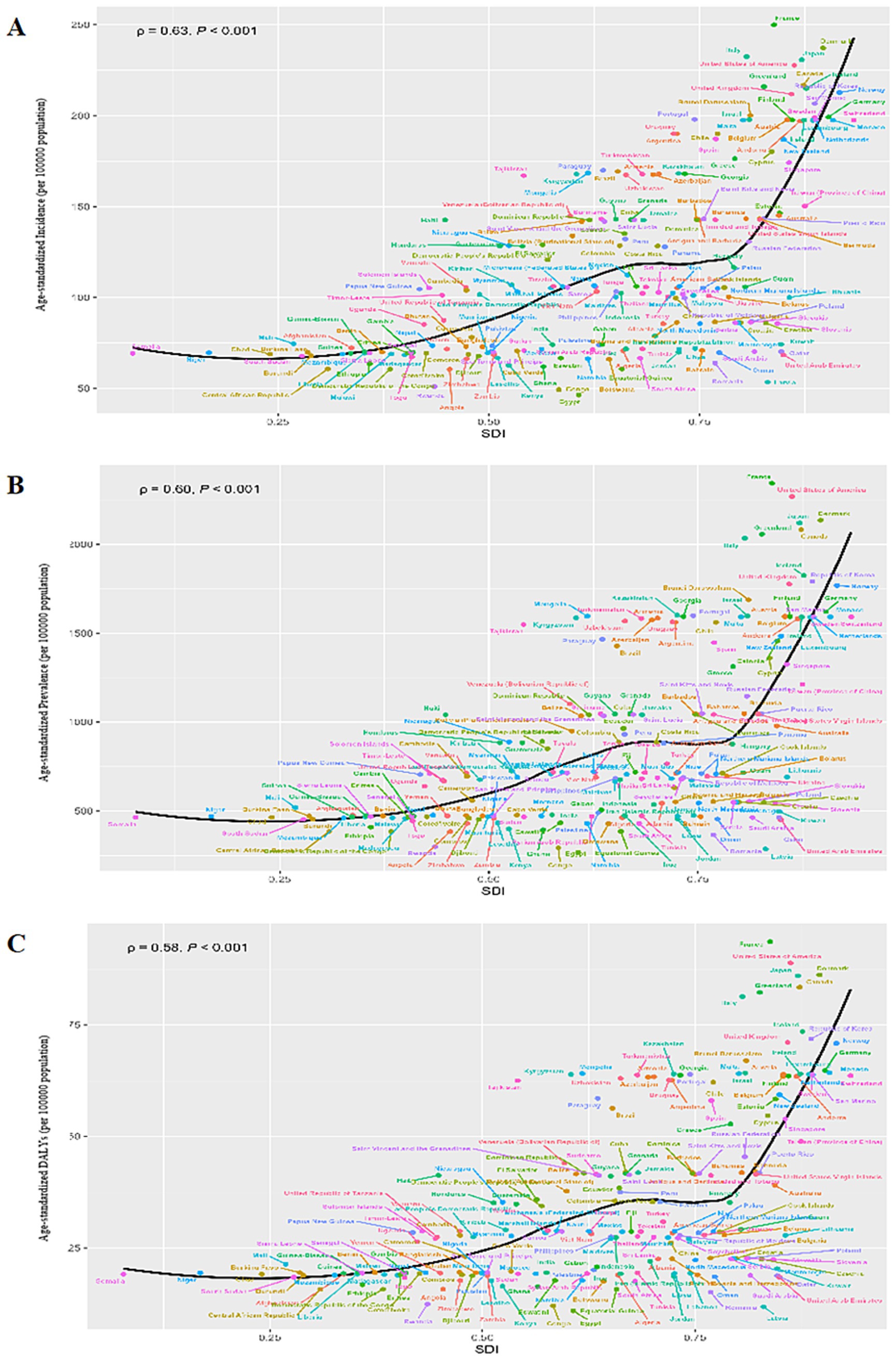
Figure 2. Pearson correlation analysis between the SDI and ASRs of incidence (A), prevalence (B), and DALYs (C) for older adult atopic dermatitis across 204 countries and territories levels in 2021. The expected ASRs in 2021 based solely on SDI were represented by the black line. For each country, points depict estimates in 2021. ASRs, age-standardized rates; DALYs, disability-adjusted life-years; SDI, Socio-demographic Index.
In 2021, the five regions with the highest older adult AD incidence were high-income North America, high-income Asia Pacific, Western Europe, Southern Latin America, and Tropical Latin America (Supplementary Table S1). Among these, high-income North America reported the peak ASIRs for older adult AD, which stood at 226.55 cases per 100,000 population (95% UI: 194.53 to 262.24). Western Europe exhibited the highest number of prevalence, estimated at 2,188,764.91 (95% UI: 1,917,994.06 to 2,479,578.21). In terms of ASPRs, high-income Asia Pacific topped the list with 2027.35 cases per 100,000 population (95% UI: 1,816.82 to 2,246.17). Consistent with the prevalence trends, Western Europe also reported the highest DALYs, totaling 86,960.81 (95% UI: 46,501.71 to 146,619.17). Regarding the ASDRs for older adult AD, high-income North America led with 88.27 cases per 100,000 population (95% UI: 47.32 to 145.35). Across all regions, the AAPCs in ASIRs, ASPRs, and ASDRs for older adult AD remained relatively stable, approaching 0%.
In 2021, three countries reporting the highest incidence of older adult AD were China (270,331.98, 95% UI: 232354.22 to 312366.65), the United States Virgin Islands (179,007.14; 95% UI: 154,561.43 to 206577.38), and India (108,337.77; 95% UI: 92,763.57 to 12,5951.47). Gabon (237.31 per 100,000 population, 95% UI: 177.39 to 304.67), Cabo Verde (249.97 per 100,000 population, 95% UI: 189.38 to 321.84), and Guam (232.53 per 100,000 population, 95% UI: 196.06 to 274.15) exhibited the highest ASIRs for AD (Supplementary Table S2; Figure 3A).
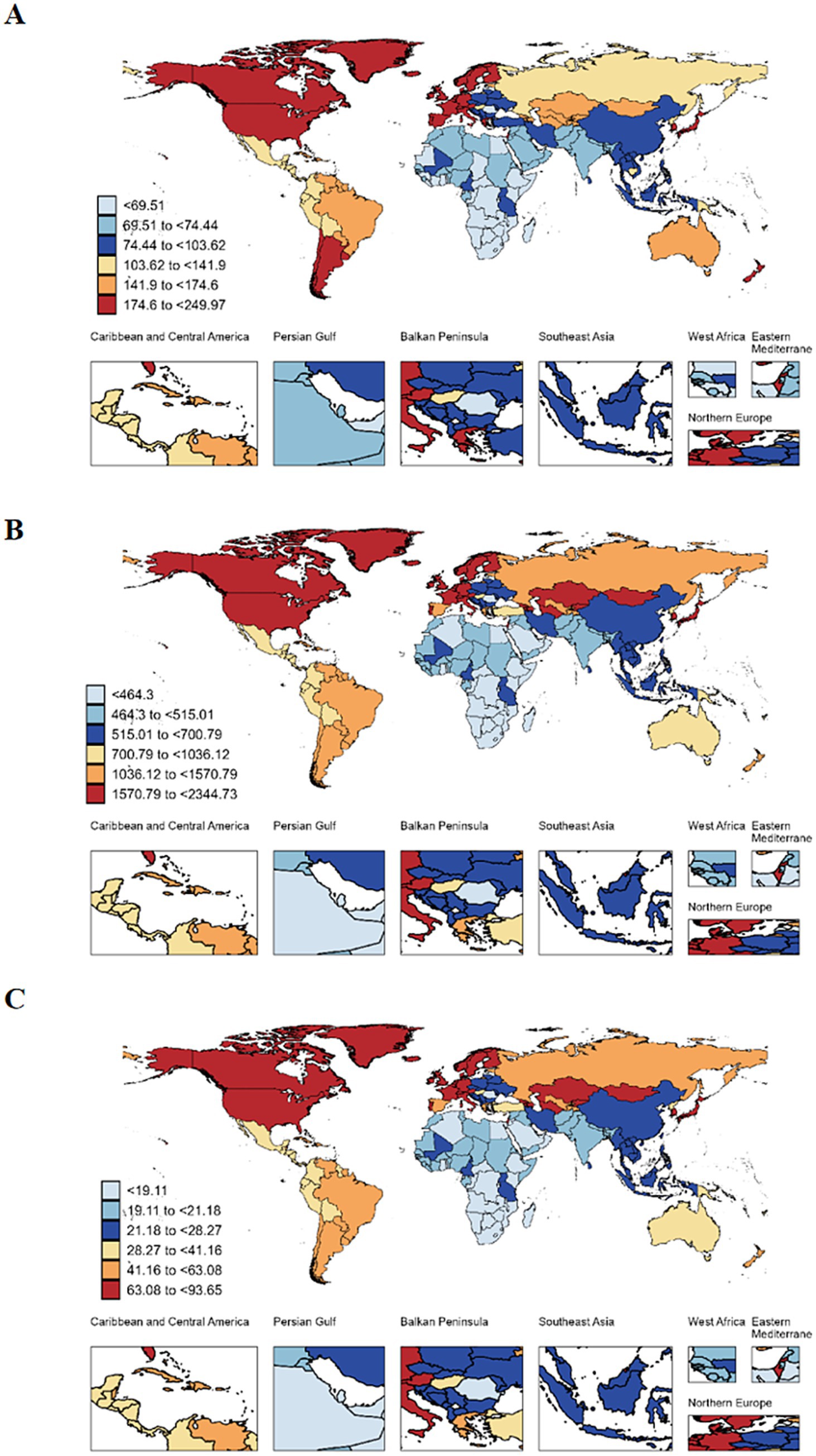
Figure 3. The global incidence (A), prevalence (B) and DALYs (C) of older adult atopic dermatitis in 204 countries and territories. DALYs, disability-adjusted life-years.
Regarding prevalence, China (1,700,330.02, 95% UI: 1,52,4724.81 to 1,88,8313.9) and the United States Virgin Islands (1,78,5263.55, 95% UI: 1,63,9173.64 to 1942483.31) topped the list in 2021. Cabo Verde (2344.73 per 100,000 population, 95% UI: 1969.09 to 2756.95), Hungary (2270.04 per 100,000 population, 95% UI: 2084.45 to 2469.8), and Gabon (2136.61 per 100,000 population, 95% UI: 1766.51 to 2552.22) had the highest ASPRs for AD (Figure 3B).
The highest DALYs due to older adult AD were recorded in China (70598.84, 95% UI: 37190.42 to 122155.3), the United States Virgin Islands (69810.16, 95% UI: 37347.43 to 114650.94), and Japan (38832.09, 95% UI: 20760.05 to 64776.46). Cabo Verde (93.65 per 100,000 population, 95% UI: 49.64 to 156.92), Hungary (88.86 per 100,000 population, 95% UI: 47.55 to 145.98), and Gabon (86.21 per 100,000 population, 95% UI: 45.18 to 148.21) demonstrated the highest ASDRs for older adult AD (Figure 3C). Notably, the incidence, prevalence, and DALYs rates remained relatively stable, with AAPCs approaching 0% (Supplementary Figure S3).
Over the past three decades, there had been a remarkable surge in incidence, prevalence, and DALYs number worldwide, with the highest elevation noted in the high SDI quintile, primarily attributed to population growth (Supplementary Table S3). Intriguingly, adverse epidemiological shifts were discernible globally, as well as in the high-middle and high SDI quintiles, with the most significant manifestation observed in the high-middle SDI quintile. When examined by gender, females exhibited a higher burden compared to males across all subgroups (Figure 4).
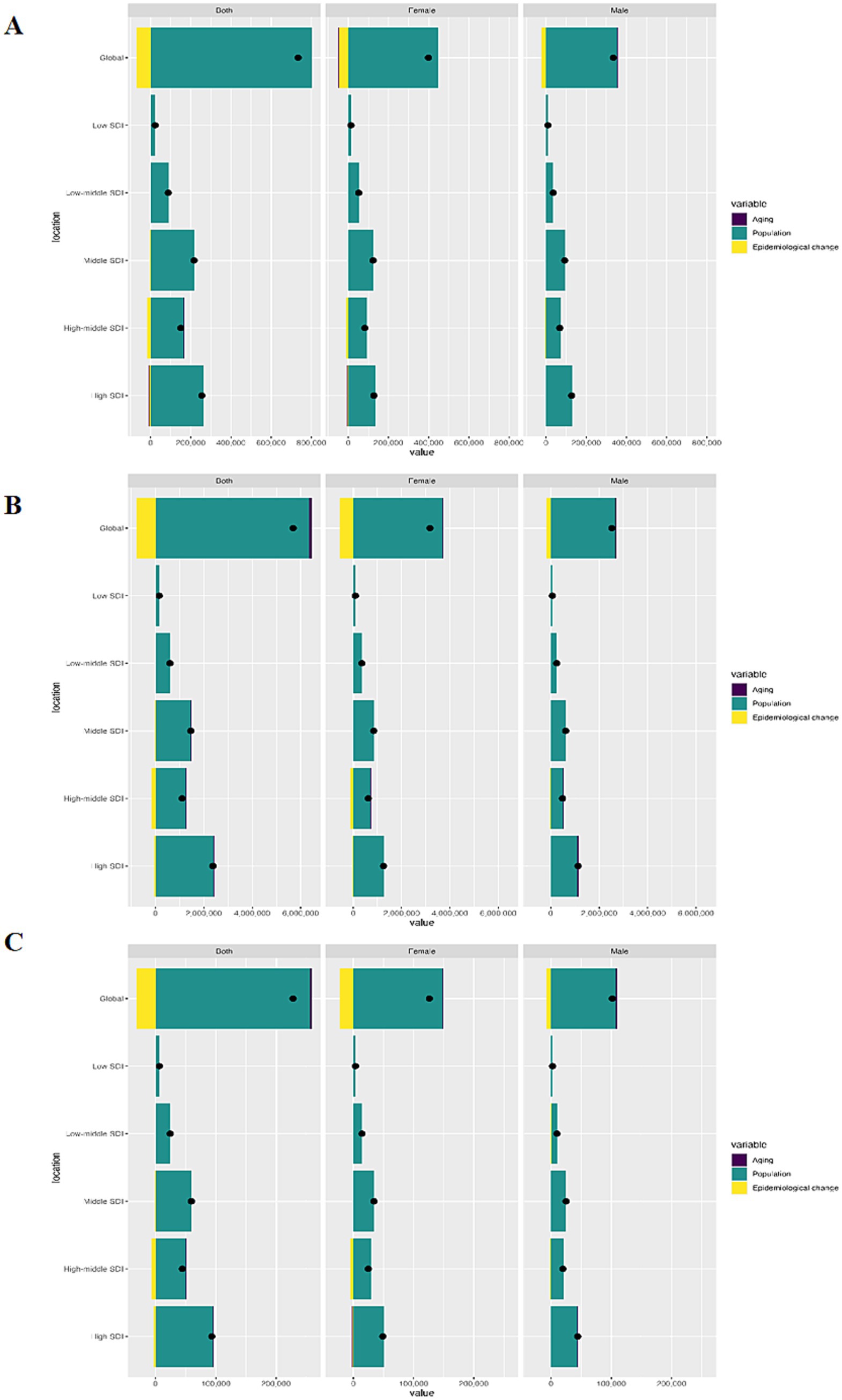
Figure 4. Decomposition analysis of changes in incidence (A), prevalence (B) and DALYs (C) rates by sex and SDI regions. DALYs, disability-adjusted life-years; SDI, Socio-demographic Index.
Considerable absolute and relative disparities related to the SDI levels were noted in the distribution of older adult AD burden across 204 countries (Supplementary Table S4). Notably, DALYs were disproportionately concentrated in countries with high SDI levels. According to the slope index of inequality, the disparity in DALYs between countries with the highest and lowest SDI was 45.46 (95%CI: 38.14 to 52.77) in 1990 and 35.6 (95%CI: 28.98 to 42.22) in 2021. Additionally, the concentration index underwent a significant decline, from 0.29 (95%CI: 0.26 to 0.31) in 1990 to 0.26 (95%CI: 0.23 to 0.3) in 2021 (Supplementary Figure S4).
In our extensive frontier analysis, spanning from 1990 to 2021 across 204 countries and territories, and utilizing SDI and ASDRs for older adult AD, subtle trends emerged (Supplementary Table S5). As SDI increased from 0.0 to 1.0, a gradual decline in older adult AD’s ASDRs was observed, evident in the shifting density from darker to lighter shades over the years, signifying an overall decrease in DALYs. Examining the 2021 frontier analysis results, clear distinctions among nations and territories were depicted visually. Notably, 10 countries, including France, high-income North America, and Denmark, exhibited notably higher rates, placing them substantially away from the frontier. Conversely, Somalia, Rwanda, the Central African Republic, and Niger were positioned nearer to the frontier, indicating favorable outcomes relative to their SDI levels (Supplementary Figure S5).
The estimated number of cases and ASRs of incidence, prevalence, and DALYs for older adult AD up to 2050 were depicted in Supplementary Figure S6. On a global scale, an increase in the number of cases and ASRs for both incidence and prevalence was anticipated. In contrast, for DALYs, while the number of cases was projected to rise, the annual ASRs was forecasted to decline until 2050. The comprehensive figures for the number of cases and ASRs for incidence, prevalence, and DALYs were provided in Supplementary Table S6.
This research presented the latest data on the burden of older adult AD at the global, regional, and national levels, spanning the period from 1990 to 2021. Although there were variations in incidence, prevalence and DALYs of older adult AD across countries, the burden older adult AD increased overall from 1990 to 2021. SDI relative and cross-country inequality analysis revealed high SDI countries shouldering a disproportionate older adult AD burden. Decomposition analysis found population growth as a major factor driving the changes in older adult AD burden. Of note, although the ASRs of DALYs were predicted to slightly decrease annually from 2022 to 2050, the absolute numbers of incidence, prevalence and DALYs were predicted to keep increasing, suggesting a huge challenge in the control and management of older adult AD remained in the next decades.
Prior studies have indicated that the ASPRs and ASIRs remained relatively stable between 1990 and 2019 (14), while our study reported a slight decrease. It may be attributed to advancements in treatment modalities, enhanced prevention and control measures, environmental and lifestyle changes, genetic factors, birth cohort effects, as well as shifts in diagnostic criteria and research methodologies (15). Additionally, the rise in overall incidence, prevalence, and DALYs was primarily due to population growth rather than an actual expansion in the proportion of affected individuals, suggesting that improvements in healthcare and public health initiatives may have contributed to mitigating the burden of AD among the older adult.
Older adult AD incidence peaked in the 75–79 age group. Notably, many trials have restricted the participation of older adults by imposing upper age limits (ranging from 40 to 70 years) or by establishing eligibility criteria that disproportionately exclude this population, thereby hindering the assessment of the efficacy and safety of novel therapies in the older adult, which ultimately limits their utilization in this demographic.
Our study indicated that the incidence of AD was higher in older adult females than in older adult males. However, existing research on the incidence of AD in males and females remains controversial (16, 17). Significant changes occur in hormone homeostasis and the immune system of older adult females, making them more susceptible to skin barrier dysfunction and immune disturbances, which may account for the higher incidence of AD in this demographic (18, 19). Additionally, this disparity may also be attributed to variations in the surveyed regions and populations.
The ASIRs, ASPRs, and ASDRs of AD exhibited regional and national differences, remained relatively stable across 21 regions and 204 countries from 1990 to 2021. As previously reported in international studies, higher levels of the SDI tend to be associated with higher prevalence rates of AD (20), which increases with rising SDI. The high-income areas such as North America, Western Europe and high-income Asia Pacific exhibited higher incidence and prevalence rates, potentially linked to the rapid pace of urbanization and economic development, where older adult individuals may experience lifestyle alterations and exposure to environmental pollutants, both known risk factors for AD (21, 22). Furthermore, countries with higher SDI typically possess better healthcare systems and greater awareness of older adult AD, leading to improved diagnosis and reporting of the disease (23, 24). This disparity underscores the multifaceted determinants of healthcare outcomes, indicating that while SDI is a significant factor, other underlying elements (environmental, genetic, or healthcare system complexities) also play crucial roles in shaping AD trends. Heterogeneity in the burden of older adult AD across SDI regions and countries underscores the importance of tailored interventions and public health strategies.
We also presented the global burden of older adult AD until 2050. Our findings indicated that the incidence and prevalence of older adult AD were anticipated to rise by 2050, posing an even greater societal burden globally. Consequently, healthcare systems will continue to bear a significant burden due to this disease in the future. These trends underscore the urgency for the formulation of nuanced health policies that focus on reducing the incidence and improving the long-term prognosis for older adult patients with AD.
This study also has several limitations. Firstly, there was considerable variation in the quality and accessibility of healthcare data across different regions, which may introduce biases or inaccuracies in the results. Secondly, similar to all analyses utilizing GBD data, this study was constrained by limitations in case ascertainment. The identification of older adult AD cases in the GBD study hinges on a range of data sources and coding systems, potentially leading to either underestimation or overestimation of older adult AD prevalence and burden in specific regions or populations. Additionally, this study lacked a classification analysis of older adult AD severity.
Globally, AD represented an underestimated public health concern primarily affecting individuals aged 60 and older, with variations observed across genders, age groups, regions, and nations. Between 1990 and 2021, the burden of older adult AD remained high varied by gender, age and countries. Those within the 80–89 age bracket, particularly females, bore a heavier burden of AD and thus warrant greater attention. Consequently, targeted strategies for the effective prevention and management of AD in the older adult are needed to address the impending challenge.
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding authors.
YO: Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Software, Visualization, Writing – original draft. XYS: Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Software, Writing – original draft. JBZ: Funding acquisition, Methodology, Visualization, Writing – review & editing. JC: Conceptualization, Funding acquisition, Writing – review & editing.
The author(s) declare that financial support was received for the research and/or publication of this article. This study was supported by the Natural Science Foundation of Chongqing (2023NSCQ-MSX0321); China Postdoctoral Science Foundation (grant number: 2024M763893).
We appreciate the works by the Global Burden of Diseases, Injuries, and Risk Factors Study (GBD) 2021 collaborators.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The authors declare that no Gen AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fpubh.2025.1569119/full#supplementary-material
AD, Atopic dermatitis; AAPC, Average annual percent change; APC, Annual percent change; ASRs, Age-standardized rates; ASDRs, Age-standardized disability-adjusted life-year rates; ASIRs, Age-standardized incidence rates; ASPRs, Age-standardized prevalence rates; BAPC, Bayesian age-period-cohort; CI, Confidence interval; DALYs, Disability-adjusted life-years; GBD, Global burden of diseases; SDI, Socio-demographic index; Th, T helper; UI, Uncertainty intervals; YLDs, Lived with disability; YLLs, Years of life lost.
1. Langan, SM, Irvine, AD, and Weidinger, S. Atopic dermatitis. Lancet. (2020) 396:345–60. doi: 10.1016/s0140-6736(20)31286-1
2. Maurelli, M, Chiricozzi, A, Peris, K, Gisondi, P, and Girolomoni, G. Atopic dermatitis in the elderly population. Acta Derm Venereol. (2023) 103:adv13363. doi: 10.2340/actadv.v103.13363
3. Ali, F, Vyas, J, and Finlay, AY. Counting the burden: atopic dermatitis and health-related quality of life. Acta Derm Venereol. (2020) 100:adv00161. doi: 10.2340/00015555-3511
4. Chan, LN, Magyari, A, Ye, M, Al-Alusi, NA, Langan, SM, Margolis, D, et al. The epidemiology of atopic dermatitis in older adults: a population-based study in the United Kingdom. PLoS One. (2021) 16:e0258219. doi: 10.1371/journal.pone.0258219
5. Bozek, A, Fisher, A, Filipowska, B, Mazur, B, and Jarzab, J. Clinical features and immunological markers of atopic dermatitis in elderly patients. Int Arch Allergy Immunol. (2012) 157:372–8. doi: 10.1159/000329150
6. Chiricozzi, A, Maurelli, M, Calabrese, L, Peris, K, and Girolomoni, G. Overview of atopic dermatitis in different ethnic groups. J Clin Med. (2023) 12:2701. doi: 10.3390/jcm12072701
7. Liu, J, Liu, T, Burkart, KG, Wang, H, He, G, Hu, J, et al. Mortality burden attributable to high and low ambient temperatures in China and its provinces: results from the global burden of disease study 2019. Lancet Reg Health West Pac. (2022) 24:100493. doi: 10.1016/j.lanwpc.2022.100493
8. GBD 2021 Gout Collaborators. Global, regional, and national burden of gout, 1990-2020, and projections to 2050: a systematic analysis of the global burden of disease study 2021. Lancet Rheumatol. (2024) 6:e507–17. doi: 10.1016/s2665-9913(24)00117-6
9. Wang, F, Ma, B, Ma, Q, and Liu, X. Global, regional, and national burden of inguinal, femoral, and abdominal hernias: a systematic analysis of prevalence, incidence, deaths, and DALYs with projections to 2030. Int J Surg. (2024) 110:1951–1967. doi: 10.1097/JS9.0000000000001071
10. GBD 2019 Diseases and Injuries Collaborators. Global burden of 369 diseases and injuries in 204 countries and territories, 1990-2019: a systematic analysis for the global burden of disease study 2019. Lancet. (2020) 396:1204–22. doi: 10.1016/s0140-6736(20)30925-9
11. GBD 2019 Demographics Collaborators. Global age-sex-specific fertility, mortality, healthy life expectancy (HALE), and population estimates in 204 countries and territories, 1950-2019: a comprehensive demographic analysis for the Global Burden of Disease Study 2019. Lancet. (2020) 396:1160–203. doi: 10.1016/s0140-6736(20)30977-6
12. Kim, HJ, Fay, MP, Feuer, EJ, and Midthune, DN. Permutation tests for joinpoint regression with applications to cancer rates. Stat Med. (2000) 19:335–51. doi: 10.1002/(sici)1097-0258(20000215)19:3<335::aid-sim336>3.0.co;2-z
13. Cheng, X, Yang, Y, Schwebel, DC, Liu, Z, Li, L, Cheng, P, et al. Population ageing and mortality during 1990-2017: a global decomposition analysis. PLoS Med. (2020) 17:e1003138. doi: 10.1371/journal.pmed.1003138
14. Faye, O, Flohr, C, Kabashima, K, Ma, L, Paller, AS, Rapelanoro, FR, et al. Atopic dermatitis: a global health perspective. J Eur Acad Dermatol Venereol. (2024) 38:801–11. doi: 10.1111/jdv.19723
15. Bieber, T. Atopic dermatitis: an expanding therapeutic pipeline for a complex disease. Nat Rev Drug Discov. (2022) 21:21–40. doi: 10.1038/s41573-021-00266-6
16. Nix, DE, Lebsack, ME, Chapelsky, M, Sedman, AJ, Busch, J, and Norman, A. Effect of oral antacids on disposition of intravenous enoxacin. Antimicrob Agents Chemother. (1993) 37:775–7. doi: 10.1128/aac.37.4.775
17. Shin, YH, Hwang, J, Kwon, R, Lee, SW, Kim, MS, Shin, JI, et al. Global, regional, and national burden of allergic disorders and their risk factors in 204 countries and territories, from 1990 to 2019: a systematic analysis for the global burden of disease study 2019. Allergy. (2023) 78:2232–54. doi: 10.1111/all.15807
18. Johansson, EK, Bergström, A, Kull, I, Melén, E, Jonsson, M, Lundin, S, et al. Prevalence and characteristics of atopic dermatitis among young adult females and males-report from the Swedish population-based study BAMSE. J Eur Acad Dermatol Venereol. (2022) 36:698–704. doi: 10.1111/jdv.17929
19. Kanda, N, Hoashi, T, and Saeki, H. The roles of sex hormones in the course of atopic dermatitis. Int J Mol Sci. (2019) 20:4660. doi: 10.3390/ijms20194660
20. GBD 2019 IMID Collaborators. Global, regional, and national incidence of six major immune-mediated inflammatory diseases: findings from the global burden of disease study 2019. EClinicalMedicine. (2023) 64:102193. doi: 10.1016/j.eclinm.2023.102193
21. Nutten, S. Atopic dermatitis: global epidemiology and risk factors. Ann Nutr Metab. (2015) 66:8–16. doi: 10.1159/000370220
22. Yue, H, Umehara, Y, Trujillo-Paez, JV, Peng, G, Nguyen, HLT, Chieosilapatham, P, et al. Exogenous factors in the pathogenesis of atopic dermatitis: irritants and cutaneous infections. Clin Exp Allergy. (2021) 51:382–92. doi: 10.1111/cea.13820
23. Gatmaitan, JG, and Lee, JH. Challenges and future trends in atopic dermatitis. Int J Mol Sci. (2023) 24:11380. doi: 10.3390/ijms241411380
Keywords: atopic dermatitis, the older adult, global burden of disease study, disability-adjusted life years, incidence
Citation: Ou Y, Shao X, Zhang J and Chen J (2025) Global, regional, and national burden of older adult atopic dermatitis in 204 countries and territories worldwide. Front. Public Health. 13:1569119. doi: 10.3389/fpubh.2025.1569119
Received: 31 January 2025; Accepted: 20 March 2025;
Published: 02 April 2025.
Edited by:
Lizette M. Lorenz, North Carolina State University, United StatesReviewed by:
Lea Alice Kiefer, Charité University Medicine Berlin, GermanyCopyright © 2025 Ou, Shao, Zhang and Chen. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Jingbo Zhang, NDk1NTQ1NTZzYW1hZWxAZ21haWwuY29t; Jin Chen, Y2hlbmppbjc3OTFAMTYzLmNvbQ==
†These authors have contributed equally to this work
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.