
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Public Health , 18 February 2025
Sec. Aging and Public Health
Volume 13 - 2025 | https://doi.org/10.3389/fpubh.2025.1446862
This article is part of the Research Topic Exploring the Interplay of Aging, Obesity, and Oral Health in Elderly Populations View all articles
Background: With the development of the economy and society, people pay more and more attention to oral health. Oral frailty can limit nutritional intake and make an individual physically weak, which is detrimental to people’s health. Therefore, it is urgent to identify oral frailty and their associated risk factors. In this study, we aimed to evaluate the oral frailty and its influencing factors in Chinese middle-aged and older hospitalized patients.
Methods: A cross-sectional study was conducted from May 2023 to February 2024 in 2 tertiary hospitals in Wuhu City, Anhui Province, China. The self-designed sociodemographic information, the Oral Frailty Index-8, the 2-item Connor–Davidson resilience scale (CD-RISC-2), the sarcopenia screening questionnaire, and the three-item short literacy survey were used in this study.
Results: A total of 914 middle-aged and older adults patients were recruited. The prevalence of oral frailty was 48.7% (445/914). In the univariate analysis, oral frailty was significantly associated with age, education, place of residence, monthly income, sarcopenia, resilience, and health literacy. Correlation analysis showed that oral frailty was significantly negatively correlated with sarcopenia, resilience, and health literacy. In the binary logistic regression analysis, oral frailty was significantly associated with sarcopenia, and health literacy. Health literacy was a protective factor of oral frailty.
Conclusion: This study aimed to investigate the prevalence of oral frailty and identify the associated influencing factors among middle-aged and older adults patients in Anhui Province, China. This study identified several factors influencing oral frailty in middle-aged and older adults patients. Therefore, the government and relevant departments should implement targeted interventions to improve middle-aged and older adults patients’ oral frailty.
In recent decades, life expectancy has increased worldwide and the proportion of middle-aged and older adults people in other age groups has continued to increase, resulting in an aging society. As China’s aging population intensifies and lifestyle changes, the disease problems of middle-aged and older adults people have received widespread attention from society. The Japanese Dental Association defines oral frailty as a series of age-related phenomena and processes that lead to changes in various oral conditions (number of teeth, oral hygiene, oral function, etc.) and are accompanied by a decrease in interest in a healthy oral cavity. It is defined as decreased physical and mental performance, oral weakness leading to weight gain and eating disorders. The overall impact is reduced physical and mental performance (1). Oral health is one of the important components that affect the high quality of life of the older adults (1). Oral health is essential in maintaining good general health (2).
Studies have shown that poor oral health is associated with age-related physiological stress, frailty (3), sarcopenia (4), cognitive decline (5), and the accumulation of multiple diseases (6). Over and above all, oral frailty increases the risk of hospitalization for illness in middle-aged and older adults. People have recently become aware of the risk of periodontal disease in patients with chronic diseases such as diabetes (7), coronary heart disease (8), respiratory disease (9), and osteoporosis (10). Oral frailty may be an essential risk factor for systemic diseases, so timely oral health management is crucial to prevent non-communicable chronic diseases (11). A study found that people with oral frailty were at higher risk for physical frailty, sarcopenia, serious illness requiring care, and death than people without oral weakness (12). Poor oral health could affect the ability to eat, taste, swallow, and speak, reduce self-confidence, and significantly impact quality of life (13). Hihara et al. (14) assumed that oral frailty was an early sign of physical frailty.
Sarcopenia is a pathological condition of “muscle failure,” defined as “the progressive loss of muscle strength (muscle deficiency), mass (quantity), and function (quality), resulting in the decreased physical performance and increased disability, risk of falls, and death Rate (15). Sarcopenia is a multifaceted age-related disorder involving biological, environmental, socioeconomic, and genetic factors that combine to cause loss of muscle mass and function (16). Sarcopenia is an essential symbol of the aging process and is closely related to adverse outcomes such as falls, disability, and death, seriously affecting the physical health and quality of life of middle-aged and older adults people. The development of sarcopenia is related to unique molecular mechanisms such as aging, chronic disease, malnutrition, and inactivity (16). Sarcopenia is a reversible disease that can be reversed with early intervention (17).
Rutter (18) proposed psychological resilience in 1987 and defined it as the positive impact of individual differences on responses to stress and adversity. Psychological resilience can affect people’s emotions directly or indirectly through reactions. The study proposed that greater resilience is related to better-coping behaviors, and coping behaviors are related to better cognitive functions (19). At the same time, psychological resilience could protect against the harmful effects of chronic stress (20). Resilience is a dynamic process that allows people with chronic illness to adapt more positively when faced with unpleasant experiences in their lives, which allows them to manage better situations that cause anxiety and stress (21). Resilience can improve a person’s self-esteem, personal strength, and emotional stability. People with high levels of resilience have an extraordinary ability to cope with disease-related challenges (22).
Health literacy (HL) is a set of personal skills for acquiring, processing, understanding, and using health information to maintain health (23). Health literacy is essential for healthy living but is especially important when making disease-related decisions. These skills will help people prevent illness but also help people make informed decisions when they become ill, allowing them to manage their illness and the self-care that comes with it. Factors associated with health literacy include patient characteristics (24), physician-patient communication (25), the way information is presented ((26), and the way an individual receives information about their disease (also known as organizational HL). People with sufficient HL can identify and access reliable sources of information, distinguish misinformation, identify risks, and analyze data about their situation (27). In general, adequate HL relates to the patient’s ability to manage disease, communicate effectively with healthcare professionals, and participate in medical decision-making (28). Therefore, appropriate LH can guide and ultimately help patients on the right treatment path.
Oral frailty is an important feature of unhealthy aging, with serious negative effects on quality of life and an increased risk of malnutrition and death in middle-aged and older hospitalized patients. Early intervention and improvement of oral health are critical to the physical health of middle-aged and older adults and to reducing future adverse health events. Exploring the current status and influencing factors of oral frailty in middle-aged and older adults people, as well as factors that prevent the negative effects of oral frailty (e.g., resilience and social support), are essential for developing future guidelines for the prevention of oral frailty. However, the prevalence data of oral frailty in middle-aged and older hospitalized patients with chronic diseases in China are still lacking. Therefore, it is of great academic and practical significance to explore the status quo of oral frailty and related influencing factors in middle-aged and older hospitalized patients. The purpose of this study is to enrich the research on oral frailty by analyzing the prevalence and related influencing factors of oral frailty in middle-aged and older hospitalized patients in Anhui province. The results of this study can provide reference for medical institutions to improve the quality of life of middle-aged and older hospitalized patients with oral frailty in Anhui province.
All investigators composed of undergraduate students from Wannan Medical College, and they received systematic training before the start of the survey to improve the scientific nature of the investigation and questioning skills, and reduce investigation errors. When the patient’s vital signs and conditions were relatively stable, the researcher carefully explained the purpose of this study to middle-aged and older adults patients with chronic diseases who met the inclusion criteria. Our investigators, supported by hospital nursing staff, conducted face-to-face interviews with participants using a structured questionnaire. Verbal informed consent was obtained from all participants. After excluding patients with extremely serious conditions and those who could not fully understand the oral explanation, 981 valid samples were finally included. The investigators fully ensured participant’s privacy, confidentiality, voluntary participation, and their unconditional right to withdraw from the study at any point of data collection without causing any harm. This was a multicenter cross-sectional study, and participants were recruited from 2 tertiary hospitals in Wuhu City using convenience sampling. The inclusion criteria are: (1) age ≥ 45 years or over, (2) Chronic diseases such as diabetes, hypertension, stroke, and coronary heart disease were diagnosed in secondary hospitals and above, (3) Participants who have the ability to complete the questionnaire independently or can do so with the face-to-face assistance of the investigator.
The exclusion criteria are (1) the participants were diagnosed with severe mental illnesses, and neurological diseases by professional medical institutions; (2) those with a certain degree of cognitive impairment and unable to complete the questionnaire; (3) middle-aged and older adults patients with severe cardiovascular and cerebrovascular diseases, severe liver and kidney diseases, malignant tumors and other end-stage diseases; (4) severe vision or hearing impairment, unable to cooperate in completing the questionnaire.
The general demographic characteristics questionnaire was developed by searching the relevant literature through databases such as web of science and Pubmed and the clinical experience of the researchers.
This scale was compiled by Tanaka et al. (29), and was used to screen patients for oral frailty. The scale includes 5 aspects: whether to use dentures, swallowing function, social participation, oral health-related behaviors and chewing ability, with a total of 8 items, The OFI-8 total score was 0–8 points, and the higher the score, the worse the oral frailty, with ≥4 points indicating oral frailty. Moreover, its effectiveness has been verified through multiple cross-sectional surveys (30). The scale has good reliability and validity, with Cronbach’s alpha coefficient is 0.84 in this study.
The 2-item Connor–Davidson resilience scale (CD-RISC-2) is a self-assessment tool used to measure psychological resilience (31). The CD-RISC-2 consists of 2 questions, questions include “I can adapt when people and things around me change” and the responses are on a five-point Likert scale ranging from 0 (“never”) to 4 (“always”), generating total scores from 0 to 8, with higher scores indicating more higher degree of psychological resilience. The Cronbach’s alpha of the scale was 0.82 in this study.
Sarcopenia was assessed using the Sarcopenia Screening Questionnaire developed by Saint Louis University in the United States (32). It is currently widely used in many clinical studies because it is easy to operate and does not require other auxiliary equipment. SARC-F questionnaire components five components: strength, assistance walking, rise from a chair, climb stairs, and falls. Each item ranges between 0 and 2, and the total score ranges between 0 and 10.The higher the total SARC-F score, the more severe the sarcopenia. A score of 4 or greater predicts sarcopenia. The Cronbach’s alpha of the scale was 0.83 in this study.
The “Three-item Short Literacy Survey” scale was used. It was verified by McNaughton et al. (33) that this form has the characteristics of simplicity, speed, and good reliability and validity. This form is suitable for the health literacy assessment of middle-aged and older adults inpatients. The content includes: (1) Do you often need someone (such as family, friends, medical workers, caregivers, etc.) to help you understand written medical information? (2) Do you feel confident filling out medical forms on your own? (3) Do you need help interpreting written medical information to better understand your medical condition?”. The answers to each question are divided into 5 levels, each assigned a score of 1–5, with a total score of 15. A score of ≤10 indicates health literacy, and a score of >10 indicates a lack of health literacy. The Cronbach’s α coefficient is 0.792.
All the collected data were stored in the Questionnaire Star database and later imported into the Statistical Package for Social Sciences (SPSS) V22.0 software for data analysis. The participants’ oral frailty status was classified as oral frailty or non-oral frailty. Data were expressed as means and standard deviations or frequencies and percentages, and χ2 tests were performed to assess the relationships between factors and outcomes. Chi-square test was used to identify statistically significant factors affecting oral frailty. Independent variables with p-values less than 0.05 were used in binary regression analysis to identify variables which were independently associated with oral frailty. All statistical analyses were two-tailed, and statistical significance was set at p < 0.05 (Two-tailed).
This study was approved by the Nursing Department of the First Affiliated Hospital of Wannan Medical College (Yijishan Hospital), China (YJYYYHLB-2023-09-07). The survey was in line with the principles outlined in the latest edition of the Declaration of Helsinki. Participation in the study was voluntary, and all participants received verbal informed consent and signed a paper informed consent form at the beginning of the study.
A total of 943 middle-aged and older adults patients were invited to participate this study, of which 29 participants were excluded due to incomplete answer. The final sample recruited 914 patients, with the mean age being (65.73 ± 10.56) years old, of whom 312 (34.1%) patients aged between 45 and 59 years old, 246 (26.9%) patients aged between 60 and 69 years old, 250 (27.4%) patients aged between 70 and 79 years old, and 106 (11.6%) patients aged 80 years or older. 527 (57.5%) were male, and 388 (42.5%) were female. 316 (34.6%) patients resided in countryside, 332 (36.3%) resided in town, and 266 (29.1%) resided in city. The socio-demographic information is showed in Table 1.
In this study, 445 (48.7%) middle aged and older adults patients were identified as oral frailty. The result of univariate analysis showed that age, education, place of residence, monthly income, sarcopenia, resilience, and health literacy were inverse (Table 2).
As shown in Table 3, sarcopenia had positive correlation with oral frailty (p < 0.01), in contrast, resilience and health literacy had negative correlations (p < 0.01).
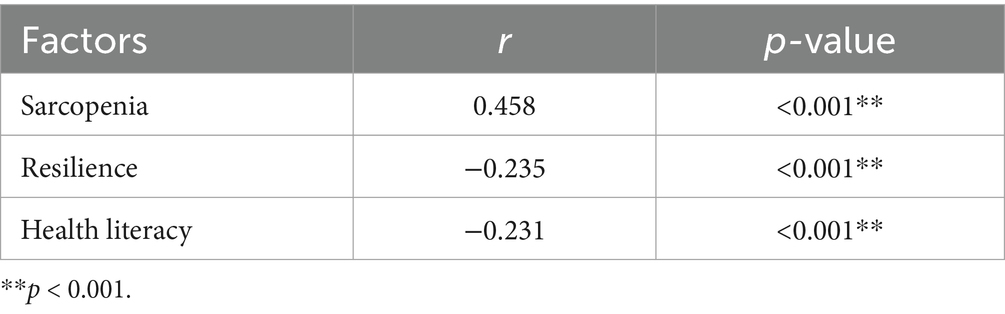
Table 3. Correlation between oral frailty and relevant indicators in middle-aged and older adults patients.
Binary logistic regression analysis was performed to explore the influencing factors of oral frailty, in which age, education, place of residence, monthly income, sarcopenia, resilience and health literacy were used as independent variables and oral frailty (grouping, 0 = non-oral frailty, 1 = oral frailty) were used as dependent variables. The result displayed that middle-aged and older adults patients with the age increasing, the risk of oral frailty increased (OR = 1.745, 95% CI 1.502–2.026). Compared with non-sarcopenia middle-aged and older adults patients, patients with sarcopenia more likely to experience oral frailty (OR = 2.994, 95% CI 1.998–4.485). Besides, our findings showed that health literacy (OR = 0.937, 95% CI 0.890–0.987) and resilience (OR = 0.874, 95% CI 0.778–0.981) were protective factors for oral frailty among middle-aged and older adults patients. The result of binary logistic regression analysis is displayed in Figure 1 and Table 4.
With the aging process, middle-aged and older populations are increasingly susceptible to oral frailty, which manifests as tooth loss, poor oral hygiene, and swallowing difficulties. These issues contribute to the deterioration of general health. While extensive research has examined oral frailty in community-dwelling older adults, there is a significant research gap regarding hospitalized middle-aged and older patients in China. This limitation hinders medical professionals in detecting and implementing effective preventive measures against oral frailty. To address this gap, our study utilized the Oral Frailty Index-8 questionnaire to investigate the prevalence and influencing factors of oral frailty among hospitalized patients.
Our findings revealed that 48.7% of patients aged 45 years and older in China are at risk of oral frailty, a prevalence significantly higher than the annual incidence reported among community-dwelling Chinese older adults (30.3%) (34). This discrepancy likely arises from the higher prevalence of physical frailty, sarcopenia, and malnutrition among hospitalized patients (35), which may lead them to rate their oral health more poorly. These results underscore the need for targeted interventions for this vulnerable population.
The study confirmed that advancing age is a critical risk factor for oral frailty, consistent with previous research by Iwasaki et al. (36). Age-related factors such as increased tooth loss, reliance on dentures, reduced diet quality, and difficulties in eating or chewing solid foods are well-documented contributors to poor oral health (37, 38). Additionally, older adults in China exhibit low levels of oral hygiene and infrequent dental visits (39), exacerbating the risk of oral frailty. Furthermore, advancing age is often accompanied by physical and social frailty as well as reduced social engagement, all of which elevate the risk of oral frailty (40). These findings highlight the importance of implementing standardized oral frailty screening during hospital admissions and initiating preventative measures, particularly for older patients.
Our study also identified sarcopenia as a significant risk factor for oral frailty in middle-aged and older patients, aligning with previous research (12). Sarcopenia, an age-related syndrome, adversely affects occlusal force (41), masticatory ability (42), tongue pressure (43), and swallowing function (44), resulting in diminished oral functionality. Kugimiya et al. (45) demonstrated that older adults with sarcopenia are more likely to exhibit low oral function. This emphasizes the need for patients with sarcopenia to receive regular dental care and targeted interventions to maintain oral functionality.
Additionally, we found that patients with higher health literacy scores were more likely to experience oral frailty. Although health literacy is critical for disease management, self-care, and the effective use of preventive services (46), its role in oral frailty has not been previously studied. Given that health literacy is vital in preventing general frailty (47), it may also play a key role in improving and preventing oral frailty. Future studies should explore the mechanisms underlying this relationship to inform interventions aimed at improving oral health outcomes.
Lastly, our results revealed a positive relationship between resilience and oral frailty. Resilience, defined as a reserve capacity to overcome stress and adversity (48), has been shown to promote healthy behaviors and mitigate the impact of disease (49). However, a high level of resilience has also been associated with poor self-rated oral health and oral health problems (50), possibly due to a greater awareness of health issues. Previous studies have suggested that resilience mediates the relationship between depression and oral health (51). These findings suggest that enhancing resilience may be beneficial for addressing poor oral health, and targeted psychosocial interventions should be considered.
This study highlights the high prevalence of oral frailty among hospitalized middle-aged and older patients in China and identifies key risk factors, including advancing age, sarcopenia, health literacy, and resilience. These findings underscore the importance of standardized oral frailty screening and targeted interventions to improve oral health outcomes in this vulnerable population. Future research should further investigate the mechanisms linking these factors to oral frailty to develop evidence-based strategies for prevention and management.
The current study has several limitations concerning the generalizability of the results: first, this study is cross-sectional and cannot infer causal relationships between influencing factors and oral frailty. Secondly, this study was conducted only in two tertiary hospitals in Wuhu City, Anhui Province, and this geographical limitation reduces the external validity of the study results. Third, self-report survey methods are susceptible to subject recall bias and social desirability bias, which may affect the accuracy of reported information. Fourth, potential sampling bias is also an unavoidable limitation. Therefore, this study will further expand the scope of the survey and conduct a series of longitudinal surveys in the future to verify and expand the relevant results.
The prevalence of oral frailty among middle-aged and older hospitalized patients was notably higher compared to community-dwelling older adults, indicating a critical need for targeted interventions in this population. Age and sarcopenia were identified as significant risk factors for oral frailty, while health literacy and resilience emerged as protective factors. These findings underscore the importance of routine screening for oral frailty in hospitalized patients, particularly those at higher risk, such as individuals with sarcopenia, low health literacy, low resilience, and advanced age. Health care professionals should implement comprehensive programs to identify and manage oral frailty early, incorporating strategies to enhance health literacy, improve resilience, and address the underlying causes of sarcopenia. Such measures are essential to mitigate the progression of oral frailty and improve overall patient outcomes.
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
The studies involving human/animal participants were reviewed and approved by the Nursing Department of the First Affiliated Hospital of Wannan Medical College (Yijishan Hospital), China (YJYYYHLB-2023-09-07). The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
J-kD: Conceptualization, Data curation, Funding acquisition, Investigation, Methodology, Resources, Software, Supervision, Validation, Writing – original draft, Writing – review & editing. HL: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. JM: Investigation, Writing – original draft, Writing – review & editing. YL: Investigation, Writing – original draft, Writing – review & editing. QL: Investigation, Writing – original draft, Writing – review & editing. X-zS: Investigation, Project administration, Software, Validation, Writing – original draft, Writing – review & editing. XT: Conceptualization, Investigation, Resources, Software, Validation, Visualization, Writing – original draft, Writing – review & editing. MZ: Conceptualization, Investigation, Methodology, Resources, Software, Supervision, Validation, Writing – original draft, Writing – review & editing.
The author(s) declare that financial support was received for the research, authorship, and/or publication of this article. This research was supported by Anhui Provincial University Scientific Research Key Project (2023AH051733 and 2023AH051730), the National Natural Science Fund of China (32371112), the teaching Quality Engineering Project in Anhui Province (2023jcjs116), the New Era Education Quality Project in Anhui Province (Graduate Education) (2023cxcy js021), the Anhui Province Educational Science Research Project (JK23173), the Key Laboratory of Philosophy and Social Science of Anhui Province on Adolescent Mental Health and Crisis Intelligence Intervention (SYS2023B09), the Industry-University Cooperation Collaborative Education Project of the Ministry of Education (220905875062412), the Anhui Provincial College Outstanding Young Talents Support Program (gxyq2022045), the Teaching Quality and teaching reform project of Wannan Medical College (2020jyxm58), and the Key Project Research Fund of Wannan Medical College (WK2023SZD03).
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
1. Watanabe, Y, Okada, K, Kondo, M, Matsushita, T, Nakazawa, S, and Yamazaki, Y. Oral health for achieving longevity. Geriatr Gerontol Int. (2020) 20:526–38. doi: 10.1111/ggi.13921
2. Baniasadi, K, Armoon, B, Higgs, P, Bayat, AH, Mohammadi Gharehghani, MA, Hemmat, M, et al. The Association of Oral Health Status and socio-economic determinants with Oral health-related quality of life among the elderly: a systematic review and meta-analysis. Int J Dent Hyg. (2021) 19:153–65. doi: 10.1111/idh.12489
3. Slashcheva, LD, Karjalahti, E, Hassett, LC, Smith, B, and Chamberlain, AM. A systematic review and gap analysis of frailty and oral health characteristics in older adults: a call for clinical translation. Gerodontology. (2021) 38:338–50. doi: 10.1111/ger.12577
4. Takahashi, M, Maeda, K, and Wakabayashi, H. Prevalence of sarcopenia and association with oral health-related quality of life and oral health status in older dental clinic outpatients. Geriatr Gerontol Int. (2018) 18:915–21. doi: 10.1111/ggi.13279
5. Gil-Montoya, JA, Sánchez-Lara, I, Carnero-Pardo, C, Fornieles-Rubio, F, Montes, J, Barrios, R, et al. Oral hygiene in the elderly with different degrees of cognitive impairment and dementia. J Am Geriatr Soc. (2017) 65:642–7. doi: 10.1111/jgs.14697
6. Ahmadi, B, Alimohammadian, M, Yaseri, M, Majidi, A, Boreiri, M, Islami, F, et al. Multimorbidity: epidemiology and risk factors in the Golestan cohort study, Iran: a cross-sectional analysis. Medicine. (2016) 95:e2756. doi: 10.1097/MD.0000000000002756
7. Liccardo, D, Cannavo, A, Spagnuolo, G, Ferrara, N, Cittadini, A, Rengo, C, et al. Periodontal disease: a risk factor for diabetes and cardiovascular disease. Int J Mol Sci. (2019) 20:1414. doi: 10.3390/ijms20061414
8. Humphrey, LL, Fu, R, Buckley, DI, Freeman, M, and Helfand, M. Periodontal disease and coronary heart disease incidence: a systematic review and meta-analysis. J Gen Intern Med. (2008) 23:2079–86. doi: 10.1007/s11606-008-0787-6
9. Azarpazhooh, A, and Leake, JL. Systematic review of the association between respiratory diseases and oral health. J Periodontol. (2006) 77:1465–82. doi: 10.1902/jop.2006.060010
10. Wang, CJ, and McCauley, LK. Osteoporosis and periodontitis. Curr Osteoporos Rep. (2016) 14:284–91. doi: 10.1007/s11914-016-0330-3
11. Li, X, Kolltveit, KM, Tronstad, L, and Olsen, I. Systemic diseases caused by oral infection. Clin Microbiol Rev. (2000) 13:547–58. doi: 10.1128/CMR.13.4.547
12. Tanaka, T, Takahashi, K, Hirano, H, Kikutani, T, Watanabe, Y, Ohara, Y, et al. Oral frailty as a risk factor for physical frailty and mortality in community-dwelling elderly. J Gerontol A Biol Sci Med Sci. (2018) 73:1661–7. doi: 10.1093/gerona/glx225
13. Wallace, K, Shafique, S, and Piamjariyakul, U. The relationship between Oral health and hemodialysis treatment among adults with chronic kidney disease: a systematic review. Nephrol Nurs J. (2019) 46:375–94.
14. Hihara, T, Goto, T, and Ichikawa, T. Investigating eating behaviors and symptoms of oral frailty using questionnaires. Dent J. (2019) 7:66. doi: 10.3390/dj7030066
15. Sanchez-Rodriguez, D, Marco, E, and Cruz-Jentoft, AJ. Defining sarcopenia: some caveats and challenges. Curr Opin Clin Nutr Metab Care. (2020) 23:127–32. doi: 10.1097/MCO.0000000000000621
16. Damluji, AA, Alfaraidhy, M, AlHajri, N, Rohant, NN, Kumar, M, al Malouf, C, et al. Sarcopenia and cardiovascular diseases. Circulation. (2023) 147:1534–53. doi: 10.1161/CIRCULATIONAHA.123.064071
17. Trevisan, C, Vetrano, DL, Calvani, R, Picca, A, and Welmer, AK. Twelve-year sarcopenia trajectories in older adults: results from a population-based study. J Cachexia Sarcopenia Muscle. (2022) 13:254–63. doi: 10.1002/jcsm.12875
18. Rutter, M. Psychosocial resilience and protective mechanisms. Am J Orthopsychiatry. (1987) 57:316–31. doi: 10.1111/j.1939-0025.1987.tb03541.x
19. Ma, Y, Leung, P, Wang, Y, and Wang, L. Psychological resilience, activities of daily living, and cognitive functioning among older male Tekun adults in rural long-term care facilities in China. Soc Work Health Care. (2022) 61:445–67. doi: 10.1080/00981389.2022.2147628
20. Franks, KH, Bransby, L, Cribb, L, Buckley, R, Yassi, N, Chong, TTJ, et al. Associations of perceived stress and psychological resilience with cognition and a modifiable dementia risk score in middle-aged adults. J Gerontol B Psychol Sci Soc Sci. (2023) 78:1992–2000. doi: 10.1093/geronb/gbad131
21. Kisomi, ZS, Taherkhani, O, Mollaei, M, Esmaeily, H, Shirkhanloo, G, Hosseinkhani, Z, et al. The moderating role of social support in the relationship between death anxiety and resilience among dialysis patients. BMC Nephrol. (2024) 25:100. doi: 10.1186/s12882-024-03533-x
22. Amirkhani, M, Shokrpour, N, Bazrafcan, L, Modreki, A, and Sheidai, S. The effect of resilience training on stress, anxiety, depression, and quality of life of hemodialysis patients: a randomized controlled clinical trial. Iran J Psychiatry Behav Sci. (2021) 15:e104490. doi: 10.5812/ijpbs.104490
23. Ishikawa, H, and Kiuchi, T. Association of Health Literacy Levels between Family Members. Front Public Health. (2019) 7:169. doi: 10.3389/fpubh.2019.00169
24. Sheridan, SL, Lohr, KN, Lux, L, et al. Literacy and health outcomes. Evid Rep Technol Assess. (2004) 87:1–8.
25. Street, RL. How clinician-patient communication contributes to health improvement: modeling pathways from talk to outcome. Patient Educ Couns. (2013) 92:286–91. doi: 10.1016/j.pec.2013.05.004
26. Arcia, A, Bales, ME, Brown, W, Bales, ME, et al. Method for the development of data visualizations for community members with varying levels of health literacy. AMIA Annu Symp Proc. (2013) 2013:51–60.
27. Levin-Zamir, D, and Bertschi, I. Media health literacy, eHealth literacy, and the role of the social environment in context. Int J Environ Res Public Health. (2018) 15:1643. doi: 10.3390/ijerph15081643
28. Sørensen, K, Makaroff, LE, Myers, L, Robinson, P, Henning, GJ, Gunther, CE, et al. The call for a strategic framework to improve cancer literacy in Europe. Arch Public Health. (2020) 78:60. doi: 10.1186/s13690-020-00441-y
29. Tanaka, T, Hirano, H, Ohara, Y, Nishimoto, M, and Iijima, K. Oral frailty Index-8 in the risk assessment of new-onset oral frailty and functional disability among community-dwelling older adults. Arch Gerontol Geriatr. (2021) 94:104340. doi: 10.1016/j.archger.2021.104340
30. Hu, S, and Li, X. An analysis of influencing factors of oral frailty in the elderly in the community. BMC Oral Health. (2024) 24:260. doi: 10.1186/s12903-024-03946-y
31. Zhang, M, Chi, C, Liu, Q, Zhou, N, Zhou, Z, Tao, X, et al. Prevalence and associated factors of insomnia symptoms after ending China’s dynamic zero-COVID policy: a cross-sectional survey of frontline nursing staff in Chinese hospitals. Front Public Health. (2024) 12:1363048. doi: 10.3389/fpubh.2024.1363048
32. Yao, R, Yao, L, Yuan, C, and Gao, BL. Accuracy of calf circumference measurement, SARC-F questionnaire, and Ishii’s score for screening stroke-related sarcopenia. Front Neurol. (2022) 13:880907. doi: 10.3389/fneur.2022.880907
33. McNaughton, C, Wallston, KA, Rothman, RL, Marcovitz, DE, and Storrow, AB. Short, subjective measures of numeracy and general health literacy in an adult emergency department. Acad Emerg Med. (2011) 18:1148–55. doi: 10.1111/j.1553-2712.2011.01210.x
34. Li, T, Shen, Y, Leng, Y, Zeng, Y, Li, L, Yang, Z, et al. The prevalence of oral frailty among older adults: a systematic review and meta-analysis. Eur Geriatr Med. (2024) 15:645–55. doi: 10.1007/s41999-023-00930-7
35. Ligthart-Melis, GC, Luiking, YC, Kakourou, A, Cederholm, T, Maier, AB, and de, M. Frailty, sarcopenia, and malnutrition frequently (co-)occur in hospitalized older adults: a systematic review and Meta-analysis. J Am Med Dir Assoc. (2020) 21:1216–28. doi: 10.1016/j.jamda.2020.03.006
36. Iwasaki, M, Shirobe, M, Motokawa, K, Tanaka, T, Ikebe, K, Ueda, T, et al. Prevalence of Oral frailty and its association with dietary variety, social engagement, and physical frailty: results from the Oral frailty 5-item checklist. Geriatr Gerontol Int. (2024) 24:371–7. doi: 10.1111/ggi.14846
37. Roberto, LL, Silveira, MF, de, A, Ferreira, FE, Martins, A, and Haikal, D. Contextual and individual determinants of tooth loss in adults: a multilevel study. BMC Oral Health. (2020) 20. doi: 10.1186/s12903-020-1057-1
38. Xu, KH, Li, L, Jia, SL, Li, Q, Hao, JX, Ma, S, et al. Association of Tooth Loss and Diet Quality with acceleration of aging: evidence from NHANES. Am J Med. (2023) 136:773–779.e4. doi: 10.1016/j.amjmed.2023.04.008
39. Ye, S, and Chen, L. Oral health knowledge, beliefs and practices among community-dwelling older adults in Shanghai, China: a cross-sectional analysis. Gerodontology. (2020) 37:191–9. doi: 10.1111/ger.12460
40. Hironaka, S, Kugimiya, Y, Watanabe, Y, Motokawa, K, Hirano, H, Kawai, H, et al. Association between oral, social, and physical frailty in community-dwelling older adults. Arch Gerontol Geriatr. (2020) 89:104105. doi: 10.1016/j.archger.2020.104105
41. Umeki, K, Watanabe, Y, Hirano, H, Edahiro, A, Ohara, Y, Yoshida, H, et al. The relationship between masseter muscle thickness and appendicular skeletal muscle mass in Japanese community-dwelling elders: a cross-sectional study. Arch Gerontol Geriatr. (2018) 78:18–22. doi: 10.1016/j.archger.2018.05.014
42. Horibe, Y, Ueda, T, Watanabe, Y, Motokawa, K, Edahiro, A, Hirano, H, et al. A 2-year longitudinal study of the relationship between masticatory function and progression to frailty or pre-frailty among community-dwelling Japanese aged 65 and older. J Oral Rehabil. (2018) 45:864–70. doi: 10.1111/joor.12700
43. Maeda, K, and Akagi, J. Decreased tongue pressure is associated with sarcopenia and sarcopenic dysphagia in the elderly. Dysphagia. (2015) 30:80–7. doi: 10.1007/s00455-014-9577-y
44. Cha, S, Kim, WS, Kim, KW, Han, JW, Jang, HC, Lim, S, et al. Sarcopenia is an independent risk factor for dysphagia in community-dwelling older adults. Dysphagia. (2019) 34:692–7. doi: 10.1007/s00455-018-09973-6
45. Kugimiya, Y, Iwasaki, M, Ohara, Y, Motokawa, K, Edahiro, A, Shirobe, M, et al. Association between sarcopenia and oral functions in community-dwelling older adults: a cross-sectional study. J Cachexia Sarcopenia Muscle. (2023) 14:429–38. doi: 10.1002/jcsm.13145
46. Li, H, Wu, Y, Bai, Z, Xu, X, Su, D, Chen, J, et al. The association between family health and frailty with the mediation role of health literacy and health behavior among older adults in China: Nationwide cross-sectional study. JMIR Public Health Surveill. (2023) 9:e44486. doi: 10.2196/44486
47. Uemura, K, Tsukasa, K, Watanabe, A, Okamoto, H, and Yamada, M. Association between community-level health literacy and frailty in community-dwelling older adults. Aging Clin Exp Res. (2023) 35:1253–61. doi: 10.1007/s40520-023-02405-y
48. Connor, KM, and Davidson, JR. Development of a new resilience scale: the Connor-Davidson resilience scale (CD-RISC). Depress Anxiety. (2003) 18:76–82. doi: 10.1002/da.10113
49. Finlayson, TL, Williams, DR, Siefert, K, Jackson, JS, and Nowjack-Raymer, R. Oral health disparities and psychosocial correlates of self-rated oral health in the National Survey of American life. Am J Public Health. (2010) 100:S246–55. doi: 10.2105/AJPH.2009.167783
50. Wu, B, Pei, Y, Zhang, W, and Northridge, M. Immigrant status, resilience, and perceived Oral health among Chinese Americans in Hawaii. Res Aging. (2020) 42:186–95. doi: 10.1177/0164027520912493
Keywords: comorbidities, frailty, social frailty, cognitive, medication compliance
Citation: Dou J-k, Liu H, Min J, Luo Y, Liu Q, Shi X-z, Tao X and Zhang M (2025) Prevalence and associated factors with oral frailty in middle-aged and older hospitalized patients: a cross-sectional study. Front. Public Health. 13:1446862. doi: 10.3389/fpubh.2025.1446862
Received: 10 June 2024; Accepted: 13 January 2025;
Published: 18 February 2025.
Edited by:
Sumit Yadav, UCONN Health, United StatesReviewed by:
Mihaela-Simona Naidin, University of Medicine and Pharmacy of Craiova, RomaniaCopyright © 2025 Dou, Liu, Min, Luo, Liu, Shi, Tao and Zhang. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Xue-zhi Shi, Mjc5ODk4NDAwM0BxcS5jb20=; Xiubin Tao, MTMyNTYwOTU2OEBxcS5jb20=; Ming Zhang, d255eHl6aGFuZ21pbmdAZm94bWFpbC5jb20=
†These authors have contributed equally to this work and share first authorship
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.