
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
REVIEW article
Front. Psychiatry , 04 April 2025
Sec. Social Psychiatry and Psychiatric Rehabilitation
Volume 16 - 2025 | https://doi.org/10.3389/fpsyt.2025.1431798
This article is part of the Research Topic Mental Health Recovery: Engaging and Empowering People Living With Mental Illness and Their Families View all 5 articles
Introduction: Mental health is influenced by how we perceive ourselves and others. A person’s conceptual structure and how he/she understands and makes sense of the world can be explored using the repertory grid technique (RGT), an assessment tool derived from personal construct theory. This review aimed to a) draw together relevant literature that had implemented the RGT to explore the conceptual system of a person diagnosed with a mental health condition necessitating psychiatric admission, b) synthesise research findings related to the structure and content of the conceptual system, and c) provide insights into how inpatient service users construed themselves and others to inform therapeutic practice.
Methods: A systematic search of five electronic databases (MEDLINE, EMBASE, PsycINFO, CINAHL, and Web of Science) and thesis databases (EThOS and ProQuest), alongside manual searches in relevant articles and Google Scholar, was conducted. Included studies were appraised for methodological quality using the Quality Assessment Tool for Studies with Diverse Designs.
Results: Twenty-one studies were identified and analysed using narrative synthesis. Of these 21 studies, 12 intentionally used a comparison group and compared the conceptual systems of people with different mental health diagnoses or compared conceptual systems of people with and without a diagnosed mental health condition. Findings from comparison group studies suggested that the self-esteem of a person diagnosed with a mental health condition was lower, compared to a person with no identified mental health diagnoses. Other people were typically idealised by people experiencing mental ill health; however, this finding was not observed in the experience of depression. Cognitive complexity, conceptual structure, and construing were variable across mental health conditions. Conceptual structures that were “simple” and characterised by “tight” construing were consistent with the profile of people with a mental health diagnosis, except for people with schizophrenia spectrum and psychotic disorders.
Conclusions: The structure of a conceptual system differed in people with and without a mental health condition and across mental health diagnoses. Considerations for how the review findings could inform psychological therapy and suggestions for future research are offered.
The World Health Organization (1) estimates that one in eight people is experiencing a mental health condition. Depression and anxiety disorders are the most common mental health conditions, with approximately 322 million and 264 million people living with these conditions, respectively (2). Mental health conditions are a pervasive public health concern. For example, approximately 14% of people in India (3), approximately 20% of people in Australia (4), and up to 25% of people in the UK (5) experience a mental health condition at some point in their lives. Depressive disorders are a major contributor to non-fatal loss in health and functioning worldwide (2). For example, in the UK and regions of the USA, depression is the single greatest cause of years lived with disability (2, 6). Indeed, in these two countries, the incidences of mental health conditions among children and adults are increasing (7–9).
Mental health conditions can be of such severity and/or significantly impact a person’s safety, wellbeing, and functioning that a person may require admission to an inpatient psychiatric hospital for care and treatment (10). Proportionately most people who experience a mental health condition can be safely supported in the community; however, for some, community-based services are deemed insufficient. For instance, approximately 3% of people in the UK required an inpatient psychiatric admission between 2020 and 2021 (11). Therefore, those admitted into inpatient psychiatric care are often people who present with the highest complexity and severity of mental ill health. It could be inferred that once a threshold is reached when inpatient psychiatric admission becomes necessary, a person’s mental health condition is notably more prominent or “active”, in comparison to someone residing in the community. It is imperative that people accessing inpatient psychiatric care receive purposeful admissions, inclusive of therapeutic, personalised, and timely assessment, intervention, and treatment (10). Without access to psychologically driven assessment and intervention, inpatient service users become increasingly vulnerable to longer inpatient stays (12). Prolonged inpatient psychiatric admissions have been shown to have detrimental consequences for inpatient service users including increased negative emotional states, an increased sense of shame, and worsening symptomology, such as depression, anxiety, and suicidality (13). Additionally, inpatient psychiatric stays are a high financial cost for healthcare systems; for instance, during the 2019/2020 financial year, £9 billion was spent on inpatient mental health care in the UK (14).
The nature of mental health conditions is complex and multifaceted. Personal construct theory (PCT) (15) is grounded in constructivist epistemology (16), which was presented with the term constructive alternativism (coined by Kelly, 15). This approach theorises that people construct their comprehension of the world and possess the capability to reconstruct their understanding following new experiences (17). The premise of PCT is that, through personal experience, people engage in a continuous process of forming subjective representations (i.e., “constructs”) of self-states (e.g., ideal self) and others (e.g., mother and father), which are referred to as “elements”. According to Kelly (15), a person uses his/her unique, and intricate, construct system to understand and interpret the world around him/her, a process termed construing, to make sense of and anticipate the behaviour of other people and thus sequentially his/her own behaviour. Kelly (18) postulates that a person’s personal construct system both enables and restricts his/her actions and has a pivotal role in shaping self-concept, an integral factor of our mental health. Kelly’s theory (15) also depicts the process by which construing occurs and posits that the nature of any person’s construing can be described along a “loose–tight” dimension. It is theorised that “loose” construing is when an element is positioned on opposing ends of construct poles on different occasions, resulting in changeable, vague predictions. The reverse pattern is the case in “tight” construing, which leads to consistent, unvarying, precise predictions (15). Kelly (15) further proposed that should a person construe extremely, either excessively “loosely” or “tightly”, it poses a risk to his/her psychological wellbeing.
Kelly (15) derived the complementary methodological approach of the repertory grid technique (RGT) from PCT. RGT is an assessment tool that allows for the exploration of a person’s views about the self and others through idiosyncratic language (19). A semi-structured interview is used to develop the repertory grid, and the procedural steps taken to form the grid can vary slightly. Typically, a person is asked to rate or rank various “elements” (e.g., actual self and ideal self; (20)) along several bipolar construct poles (e.g., “aggressive-easy going”; (21), p. 299) to determine the construct pole with which the person aligns the element more closely. Bipolar construct poles are often yielded from the person himself/herself through a method of elicitation carried out by the interviewer (e.g., triadic difference method; 15) and illustrated as numerical rating scales (e.g., 1–5 Likert scale; (22)).
The RGT yields both quantitative data, including the numerical rating given to an element along the bipolar construct pole, and qualitative data, such as elicited constructs. Consequently, both quantitative analytical approaches, for instance, principal component analysis (PCA; (23)), and qualitative analytical approaches, such as content analysis of elicited constructs [e.g (24).,], can be conducted (17, 25). A strength of RGT is that it facilitates the objective reporting and analysis of what is essentially subjective data (26) and therefore exceeds other methodological approaches with regard to minimising the risks of social desirability bias (27) and interviewer bias (28). Commonly, RGT analysis intends to reveal the degree of similarity construed between a particular pair of elements (e.g., by calculating the Euclidean distance between actual self and ideal self; (29)), the degree to which an element is construed as preferred or non-preferred (e.g., by calculating the mean ranked position of the actual self element along all construct poles within the repertory grid, with respect to the preferred pole (20);), and construing (e.g., by calculating the percentage of variance accounted for by the first principal component by conducting PCA; (30)). Therefore, by employing the RGT and appropriate analyses, a person’s self-concept, his/her self-esteem (e.g., discrepancy between actual self and ideal self), how he/she views himself/herself relative to others (e.g., discrepancy between actual self and significant other), and his/her construing (e.g., cognitive complexity, cognitive organisation, and cognitive articulation) can be deciphered.
Given that these aforementioned concepts can be deduced from an RGT, this illustrates the advantageous nature of this instrument in measuring important concepts in mental health. Self-discrepancy theory (31) offers one understanding of how a person can experience subjectively negative affect, a central facet of mental health conditions (32, 33). According to self-discrepancy theory, how a person views himself/herself, relative to other aspects of the self, has a formative and perpetuating role in his/her mental health. The theory postulates that emotional distress, across mental health diagnoses, can result from an incongruence perceived between a person’s actual self, ideal self, and ought self (34), with one’s self-esteem being negatively impacted when greater discrepancy between the actual self and ideal self arises (31). Self-esteem has been defined as a component of self-concept by Carl Rogers (35), a pioneer in the study of self-concept and self-esteem. For the purpose of this review, self-concept is defined as a person’s knowledge structure about himself/herself, who and what the self is (36), and self-esteem as an individual’s overall positive or negative evaluation of the self (37).
Low esteem has a causal role in the development of some mental health conditions, including depression and anxiety (38, 39), and in the development of complex feelings of sadness and disappointment (40). Hence, people with mental health conditions are found to experience a greater prevalence of discrepancies between the actual self and ideal self (34, 41), low self-esteem, and a negative view of the self (42, 43). Conversely, psychological wellbeing, in particular higher self-esteem, has been associated with greater congruence between actual and ideal self-concepts (44). Reducing the discrepancy between the actual self and ideal self has been shown to positively impact a person’s mental health (45, 46) and can be achieved through psychological interventions, including cognitive behavioural therapy and interpersonal psychotherapy (47).
A person’s self-concept, self-esteem, and mental health can also be influenced by the perception he/she holds about the self in relation to others and the response he/she receives from others towards the self. A process that is important to acknowledge when thinking about this is self-stigma, which occurs when a person experiencing a mental health condition accepts the prevailing negative attitudes, prejudices, and stereotypes about people with mental health conditions and then internalises or directs these towards himself/herself, resulting in a negative self-perception (48–50). Stereotypes held by the public about people with mental health conditions include being viewed as “dangerous”, “incompetent”, and “to be blamed” [(51), p. 343]. According to Link and Phelan (52), self-stigma can result in people who experience a mental health condition, perceiving themselves negatively or disadvantaged or even alienated, relative to other people. In their systematic review of 272 studies, Dubreucq et al. (53) noted that people who endorsed high levels of self-stigma were more likely to experience lower self-esteem and self-efficacy, greater psychiatric symptoms, higher sense of loneliness, poorer recovery, and poorer quality of life.
There is only one systematic review of studies that employed the RGT to explore the construing of self and others. In their systematic review of 15 studies focusing on psychosis only, García-Mieres et al. (54) found that people experiencing psychosis displayed high levels of actual–ideal and self–significant other discrepancies, fragmentation of self, and a rigid construct system. Although García-Mieres et al. (54) noted valuable insights into the content and construing demonstrated by people experiencing psychosis, the authors did not provide conclusions about the conceptual system beyond the experience of psychosis to other mental health conditions. Therefore, no systematic review to date has summarised, across mental health conditions, for people who require psychiatric hospitalisation, the content and process of self and other construing, captured by RGT. Through the identification, synthesis, and appraisal of existing RGT literature, this systematic review specifically aimed to address the question “How do people experiencing mental health conditions construe themselves and others, when the severity of their condition necessitates admission to a mental health hospital?”
This systematic review and narrative synthesis were conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (55). The protocol for this review was registered with Prospero International Prospective Register of Systematic Reviews (Ref: CRD42024498543, https://www.crd.york.ac.uk/PROSPERO/display_record.php?RecordID=498543) in January 2024.
The search strategy was developed through consultation with the University of Manchester library services. Categories from the PICO tool (Population, Intervention, Comparison and Outcome (56); were used to guide the development of the search strategy. A search for relevant literature was conducted in five electronic databases—MEDLINE, EMBASE, PsycINFO, CINAHL, and Web of Science—February 2024. These databases were selected because they included published research related to mental health conditions: RGT and PCT. To ensure the identification of all relevant studies that met the inclusion criteria, additional searches were undertaken using ProQuest, EThOS, Google Scholar, and Google in February 2024, and the top 200 results on each platform were screened. Furthermore, reference lists of all included articles were also reviewed (57).
The search terms were informed by the titles, abstracts, and keywords of key reviews and papers. Initial pilot searches were completed to support the development of the final search strategy, which were categorised into “mental health patient”, “mental health inpatient hospital”, and “repertory grid technique” (see Table 1). In addition, Medical Subject Headings (MeSH) terms were used to identify synonyms and added as search terms to the relevant key search category. All the terms and concepts were combined with Boolean operators (“AND” and “OR”), and the search strategy implemented is illustrated in Table 1.
Studies had to meet the following inclusion criteria: 1) implementation of “standard” RGT as opposed to a derived version (e.g., Bannister–Fransella Grid Test of Thought Disorder); 2) 50% or above of the total sample being people presenting with a mental health condition as broadly defined by recognised diagnostic manuals [e.g., Diagnostic and Statistical Manual of Mental Disorders, fifth edition revised (DSM-5-TR), American Psychiatric Association (APA) (58), or well-established instruments as the diagnostic categories of schizophrenia spectrum and other psychotic disorders, bipolar and related disorders, depressive disorders, anxiety disorders, obsessive-compulsive and related disorders, trauma- and stressor-related disorders, dissociative disorders, and personality disorders, and were described within the study by diagnosis or reaching clinical cutoff scores on an appropriate clinical tool; 3) 50% or above of the total sample were people admitted to an inpatient mental health service; 4) construing was primarily with reference to themselves, themselves and another element (person), and/or the person’s internal experience or lived experience in relation to their mental health; 5) the study had to report specific examples of elements used but did not have to state each element individually; 6) the study discussed the content and/or structure of the person’s construct system and/or construing; 7) the text was written in or translated into English; 8) the study was published peer-reviewed research or grey literature, including doctoral dissertations/theses (59); and 9) the study reported original data.
Studies were excluded if 1) they were review papers and/or book chapters; 2) RGT was completed within a forensic setting due to their specialist nature; 3) RGT was completed with person(s) presenting with a condition that came under a broad diagnostic category not listed in the inclusion criteria (e.g., neurodevelopmental disorders, eating disorders, somatic symptoms and related disorders, and substance-related and addictive disorders) due to their specialist nature and use of unique elements, which were distinct to their studies; 4) RGT was primarily employed to explore the construal of person(s) presenting with a physical health condition, in which the physical health condition was the primary focus, to enable sole focus on the construal of person(s) experiencing a mental health condition; 5) RGT was used to derive another, idiosyncratic variable (e.g., therapy success); and 6) construing was primarily with reference to specific external aspects of their mental health or externalities in general (e.g., practical aspects of their mental health care such as observation levels, or externalities such as observable behaviour and death).
Records identified from database searches were exported into the EndNote software (60), and any duplicate records were removed. The first author screened all remaining records by assessing the titles, keywords, and abstracts against the predefined inclusion and exclusion criteria. Any studies that did not meet the criteria were excluded. If eligibility was unclear, the record was retained at this stage. A second reviewer (IS) independently screened a sample of 10% (n = 1,046) of the total number of records identified from database searches (n = 10,467), with substantive agreement between the two reviewers (99.52%, kappa = 0.78), with any discrepancies being settled through discussion. The first author then conducted a full-text screening of all remaining articles and excluded studies that did not meet eligibility. Any disagreements were resolved in discussions with all authors. If a full text could not be obtained, it was removed. All remaining studies were included in the review.
Following the identification of articles, the first author completed data extraction into Microsoft Word. Extracted data were tabulated and included pertinent information, such as the study aims, demographic data of the sample, and main findings. A narrative synthesis (61) was performed to facilitate the structured extraction and synthesis of the findings across several studies to draw broad and robust conclusions on how people with mental health conditions that necessitated inpatient psychiatric admission construed themselves and others. The synthesis process was assessed for robustness through assessment and critical reflection of the methodological quality of the included studies and the analytical methods utilised within the synthesis (61).
Narrative synthesis enables the story of the literature to be told. It requires immersion in the literature, achieved through the process of reading and re-reading the included papers, to enable themes and patterns across the studies to emerge (61). Narrative synthesis permits the inclusion, comparison, and combining of heterogeneous quantitative, qualitative, and mixed-methods studies (62) and is useful to employ when the area of literature is underdeveloped (61).
The methodological quality of the studies was critically appraised using the Quality Assessment Tool for Studies with Diverse Designs (QATSDD (63)), a tool that evaluates studies with diverse designs, including qualitative, quantitative, or mixed methodological approaches. The QATSDD was deemed appropriate for the current review, as repertory grid methodology incorporates both qualitative and quantitative elements (64). As the QATSDD was originally developed for use in the discipline of psychology (65), it was easily modifiable to meet the aims of this review (64). It has been effectively employed in more than 80 reviews (65), and most specifically, it has been utilised successfully in the systematic review of repertory grid literature (66). The QATSDD was selected over other mixed- and multi-methods methodological quality assessments such as the Quality Assessment with Diverse Studies (QuADS (65)).
The QATSDD assesses 16 areas including consideration of the sample size and representativeness, description of the data collection procedure, justification for the analytical approach employed, and critical discussion of the strengths and limitations. Typically, all 16 items are applied to studies of mixed methodology, and some items are omitted when reviewing a study that adopts a purely quantitative or qualitative methodological approach. However, the QATSDD generates a percentage rating for each study, which enables comparison of all studies, irrespective of methodological approach (63). For this review, the following four items, “rationale for choice of data collection tool(s)”, “statistical assessment of reliability and validity of measurement tool(s)”, “fit between stated research question and method of data collection”, and “assessment of reliability of analytic process”, were omitted because they were not considered meaningful in a review of studies that all employed repertory grid methodology. For example, the reliability of the repertory grid analytical process is not assessed equivalently to other qualitative and quantitative methods (19).
Across the relevant 12 dimensions, each study was rated on a 4-point scoring scale: 3 (complete), 2 (moderately), 1 (very slightly), or 0 (not at all). Total scores were calculated and then presented as a percentage rating. A higher percentage rating implied stronger methodological quality (63). In accordance with other reviews that used the QATSDD (67, 68), methodological quality was categorised as poor (0%–24%), moderate (25%–49%), good (50%–75%), or high (76%–100%). To ensure the reliability of quality appraisal ratings, a second reviewer (IS) independently rated 10 of the identified papers (47.62%). Between raters, an agreement rating of 80.00% was achieved for overall quality rating, and an agreement rating of 70.83% was accomplished for identical individual domain ratings. Any discrepancies were resolved following discussion. No studies were excluded from the review based on quality.
A total of 19,833 records from database searches (n = 19,773) and other methods (n = 60) were initially identified (see Figure 1). After the removal of 9,306 duplicates, the titles and abstracts of the remaining 10,467 records were screened against eligibility criteria, and 10,333 were removed. Following database and additional method searches, 194 records were sought for retrieval, of which 20 were not obtained. A full-text review was undertaken of the remaining records (n = 174), of which 153 were excluded. Thus, 21 papers were included in the final review.
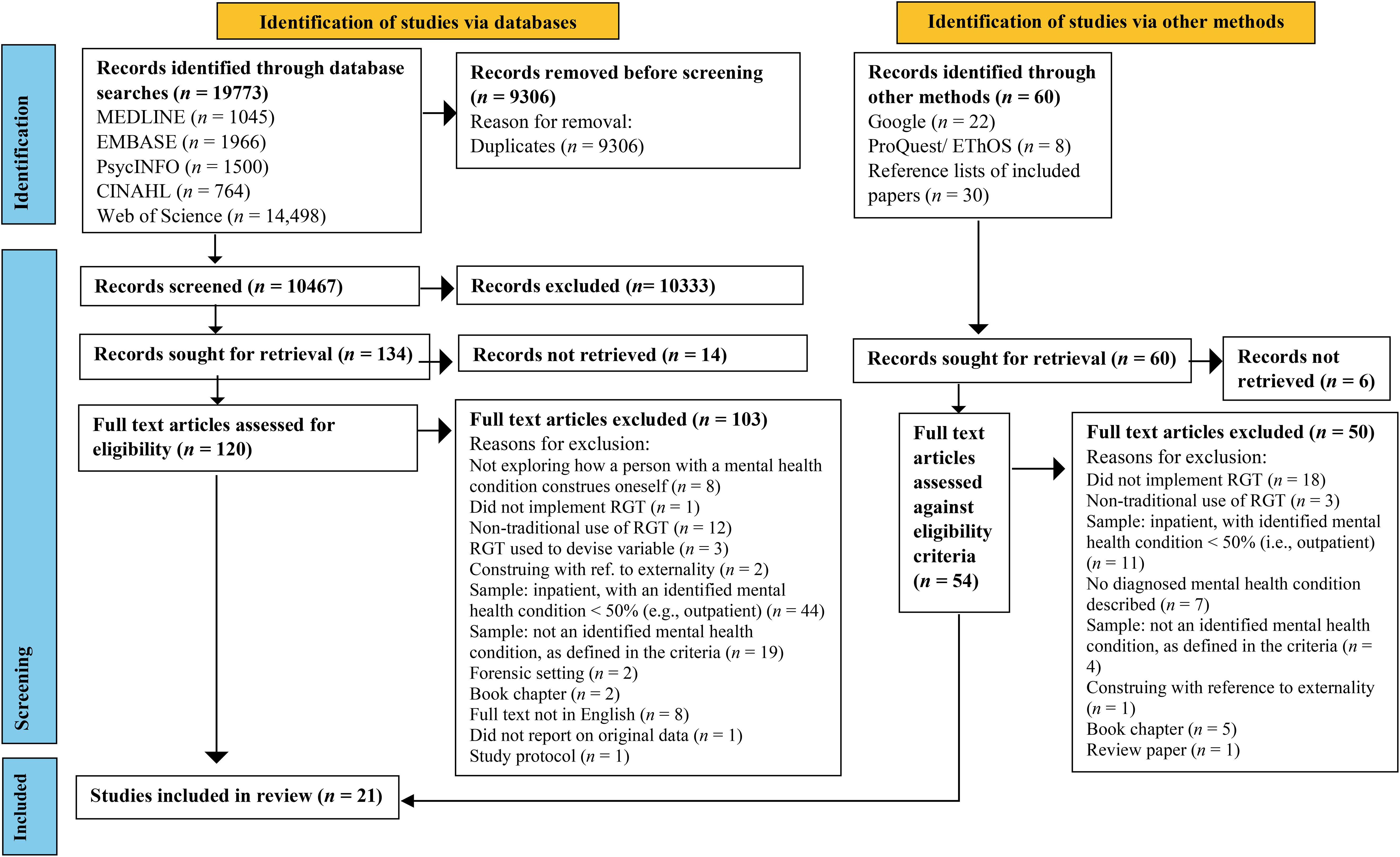
Figure 1. PRISMA flow diagram illustrating the review search strategy. PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-Analyses.
The characteristics of the included studies are summarised in Table 2. Conducted between 1969 and 2014, studies originated from the UK (n = 9), the USA (n = 6), France (n = 2), and Germany (n = 4). Sample sizes ranged from N = 1 to N = 161 participants, with two studies (9.52%) implementing a single-case design (21, 72). All studies included a clinical group that comprised one or more participants with an identified mental health condition in an inpatient setting. In total, the studies collectively presented data from 579 participants with an identified mental health condition being supported in an inpatient setting, a further 25 participants who had an identified mental health condition but were residing in the community, and 156 participants with no identified mental health condition. Most studies reported about age (n = 18, 85.71%) and gender (n = 18, 85.71%). However, fewer studies reported on other socio-demographic factors including ethnicity (n = 3, 14.29%), employment status (n = 6, 28.57%), relationship status (n = 2, 9.52%), and education level (n = 6, 28.57%). The specific diagnoses of participants were detailed in 18 studies (85.71%).
Across 21 studies, participants in the clinical groups were predominately diagnosed with a depressive disorder (n = 7), a schizophrenia spectrum and other psychotic disorders (n = 6), or an anxiety disorder (n = 4). Specific diagnoses were unclear in four studies (19.05%): examples of diagnoses were provided, or diagnoses were generalised and reported as a psychiatric condition. A validation of diagnosis method was reported in 12 studies (57.14%), such as being diagnosed by the treating clinician (n = 3), the International Classification of Diseases, 10th edition (ICD-10; WHO (88); n = 1), or an edition of the DSM (n = 1, DSM-II, APA, 71; n = 2, DSM-III, APA (89); n = 4, DSM-III-R, APA, 73) or by reaching clinical cutoff on an appropriate questionnaire or measure (n = 4).
Regarding the implementation of the RGT, all studies provided a pre-determined list of elements to the participants. In 18 studies (85.71%), idiosyncratic constructs were elicited from participants through a range of methods. In three studies (14.29%), participants were provided with at least one construct, and two studies (9.52%) failed to specify whether constructs were elicited or pre-determined. The repertory grid was implemented on a single occasion for each participant in 16 studies (76.19%), while five studies (23.81%) repeated the application of the repertory grid at least once. Twelve studies (57.14%) utilised at least one comparison group.
Overall, the methodological quality of the 21 studies was considered to be good (n = 17) or moderate (n = 3), with one study rated as being high quality ((22); see Supplementary Table 1). Irrespective of the rating, limitations were identified across all studies. However, given the scarcity of relevant studies in this research field, the collective perspective among the authors was that all included studies would meaningfully contribute to the review question, and hence, no studies were excluded on the grounds of methodological rigour.
Studies rated as moderate (21, 72, 77) lacked thorough consideration or description of various aspects of research design, including an explicit statement of aims, research setting, recruitment data, sample size and analysis, sample representativeness, data collection procedure, justification of analysis method, service user involvement, and strengths and limitations. However, it should be noted that some authors seemed to observe limited word counts, which resulted in papers lacking adequate detail (21, 72, 84).
Overall, 16 studies (76.19%) scored highly in relation to providing an explicit statement concerning the theoretical framework, and 14 studies (66.67%) were rated “complete” regarding an explicit statement of aims/objectives. Two studies [ (21, 79); 9.52%] failed to be assigned the highest rating on “fit between research question and format and content of data collection tool”. One of the 21 studies was rated below high on “fit between research question and method of analysis” [(72); 4.76%]. Conversely, 10 studies (47.62%) did not critically discuss their strengths and limitations, and 17 studies (80.95%) failed to provide any detailed recruitment data. No study demonstrated evidence of service user involvement in study design, and only one study had reported consideration of sample size [(22); 4.76%].
As previously mentioned, 12 studies (57.14%) utilised at least one comparison group, while nine studies (42.86%) did not (see Table 2). Studies that did not implement a comparison group presented information on the conceptual systems of specific mental health diagnoses in isolation. Conversely, studies that implemented a comparison group enabled authors to draw comparisons between the conceptual systems of people with and without a mental health condition and/or between different mental health diagnoses. The method of comparison varied across the literature, with most authors performing statistical comparisons between groups [e.g., t-tests (20)]. Alternatively, other authors presented exploratory comparisons to illustrate similarities and differences in construals and construing across groups [e.g (74)]. Therefore, this review was able to synthesise findings relating to conceptual systems and group these according to specific diagnoses and, when possible, summarise the comparisons made across different diagnoses as well as between people with and without mental health conditions.
A central concept was investigated in the 21 included studies related to the self-esteem and construal of self commonly experienced by a person diagnosed with a mental health condition accessing inpatient psychiatric care (see Supplementary Table 2). Across studies, self-esteem was predominantly represented by the actual–ideal discrepancy, with greater discrepancy indicative of lower self-esteem [e.g (30)]. Construal of self was defined in several ways, including by the mean ranked position of the actual self element along all construct poles within the repertory grid, with respect to the preferred pole [e.g., (20)]. For example, if the actual self element had a lower mean ranked position along construct poles, it suggested that this element more closely applied to the preferred ends of the construct poles; therefore, a more positive construal of self was held (20).
For people experiencing a mental health condition, irrespective of diagnoses, reduced self-esteem was associated with increasing duration of mental health condition (29).
Specifically, low self-esteem was observed to be characteristic of depression (20, 30, 70–72). People diagnosed with depression appeared to experience lower self-esteem compared to people with no identified mental health condition and people diagnosed with other mental health conditions including anxiety disorders, personality disorders (PD), and mania, as illustrated in comparison group studies (20, 30, 70). One contrary to this finding was Böker et al. (29), who did not find a significant difference in self-esteem between people diagnosed with depression and people with no identified mental health condition, although dysthymic mood did tend to be associated with lower self-esteem.
Overall, the RGT findings relating to self-esteem and anxiety disorders were inconclusive. Catina and Tschuschke (73) assessed changes to self-esteem following therapeutic intervention for participants diagnosed with an anxiety disorder and found a greater actual–ideal discrepancy was observed in people who continued to present with heightened anxiety relative to those with reduced anxiety symptomology. This finding could have implied that lower self-esteem was associated with experiencing increased anxiety symptomology in anxiety disorders. However, Axford and Jerrom (20) showed that self-esteem was comparable between people with an anxiety disorder and people with no identified mental health condition, thus suggesting that the presence of anxiety symptomology may not necessarily coincide with lower self-esteem.
Interestingly, participants with an anxiety disorder were revealed to experience higher self-esteem in comparison to participants diagnosed with obsessive-compulsive disorder (OCD; (74)). However, Millar (74) did suggest that the difference in self-esteem between participants with OCD and anxiety disorders could possibly relate to the severity of the condition as opposed to the specific condition itself, and hence this finding should be interpreted cautiously. The use of RGT by authors led to the discovery that OCD was characterised by low self-esteem (74, 75) and by perceiving different self-states (i.e., actual and social) as non-ideal (75). Self-esteem was observed to be lower for people diagnosed with OCD, relative to people without a mental health condition, by authors who conducted comparison group studies (74, 75). Therefore, it seems that this review was able to make firmer conclusions concerning lower self-esteem appearing in OCD than it was in the case of anxiety disorders.
The RGT enabled authors to reveal that low self-esteem appeared to be a characteristic of bipolar affective disorder (29) and schizophrenia (30). RGT findings showed self-esteem to improve as psychological stabilisation occurred in bipolar affective disorder, which indicated a relationship between lower self-esteem and episodes of de-stabilisation in this disorder (29). However, one comparison group study did not show a significant difference in a measure of self-esteem between people with schizoaffective disorders and people with no identified mental health condition (29). Furthermore, a different comparison group study highlighted higher self-esteem in people experiencing mania, a central characteristic of bipolar affective disorder (92), compared to people with no identified mental health condition (30). These latter findings hindered the review’s ability to produce robust conclusions about how self-esteem may present in relation to distinct aspects of psychotic disorders and related experiences.
Of the studies that provided findings relating to construal of self, all but one were conducted with people diagnosed with depression. Several studies revealed that depression was characterised by a negative construal of self (20, 69, 71, 72). In fact, de Bonis et al. (69) tentatively speculated that depressive mood was in fact responsible for negative evaluative self-content. However, Rowe (21) challenged this dominant connection between depression and a negative construal of self by suggesting that depression was perceived positively by the person experiencing it and the person diagnosed with depression perceived himself/herself to possess attributes that he/she valued, for example, being “generous”, “soft”, and “affectionate” (p. 298). Nonetheless, it must be acknowledged that the latter study was a single case design study; therefore, it may not be possible to generalise these results to wider experiences of depression (93).
In contrast, an alternative explanation was that, in depression, the actual self is construed both negatively and positively along interrelated dimensions (71, 94) as opposed to being construed consistently negatively (20, 69, 72). Space and Cromwell’s (73) perspective suggested that depression is characterised by an impeded ability to hold a secure, consistent construal of self, which differs from conclusions made by other authors that depression is associated with holding a consistent, albeit negative evaluation of self (20, 69, 72). In one study by Millar (74), OCD was found to be characterised by an extremely negative construal of self.
Several studies explored how people with mental health conditions construed other people and how they construed the self in relation to other people. Studies frequently captured construal of others and construal of the self in relation to others by measuring the conceptual distance between the actual self, ideal self, and non-self elements. Greater conceptual distance between the actual self and non-self elements implied greater perceived dissimilarity between the self and others [e.g (30)].
In general, people with mental health conditions were said to idealise significant others (20), implying that they tended to construe other people positively. However, the same pattern of construing was observed for people with no identified mental health condition (20) and therefore may suggest that construing others positively was not unique to the experience of mental ill health. The RGTs completed by people diagnosed with schizophrenia substantiated the notion that people experiencing mental health conditions construed other people positively. Indeed, prior to achieving psychological stabilisation in schizophrenia, a person was said to construe others positively in comparison to the self (78). Moreover, others, and most strongly the essence of a persecutory delusion, tended to be construed as more malevolent and omnipotent than the actual self (22).
An exception to this pattern was revealed in the instance of depression. Construing others negatively was more evident in people diagnosed with depression, irrespective of the person having a comorbid diagnosis of PD, compared to people with no identified mental health condition, as illustrated in a comparison group study (69). This observation was upheld by a single case study of recurrent depression, which found that the self was construed as more similar to others they valued, and a person without depression as more similar to others they disliked (21). However, as per the findings of Rowe (21) discussed above, generalising this latter finding to other experiences of depression must be done with caution (93). Overall, these findings suggested that depression was linked with construing other people negatively, specifically those without depression.
Some authors challenged the notion that people diagnosed with a mental health condition strictly construed others in a unidimensional manner, i.e., either positively or negatively. Tschuschke and Dies (82) tentatively suggested that construing parental elements either extremely negatively or over-idealised was associated with higher distress symptomology when experiencing a mental health condition. This finding suggested that the extremity of construing, instead of the direction of construing (i.e., positively or negatively), was linked to experiencing a greater severity of mental ill health.
De Bonis et al. (69) discovered a similar result in the experience of borderline PD and comorbid depression by finding that people diagnosed with borderline PD with depression tended to hold a contrasted view of others (i.e., construing them as “good” and “bad”). However, holding a contrasted view of others may be distinctive to borderline PD, as people with a solitary diagnosis of depression and people with no identified mental health condition could not be differentiated from one another by this pattern of construing (69).
Predominantly, people with mental health conditions construed the self as dissimilar to others (20, 30, 70, 71, 74, 79). This notion was observed in presentations of depression (20, 70, 71), schizophrenia (30, 79), and OCD (74, 75), when compared to people with no identified mental health condition.
This pattern of low identification with others in depression, i.e., greater perceived dissimilarity between actual self and non-self elements, was one of the most consistent findings discovered through the RGT (95). Indeed, people diagnosed with depression construed greater dissimilarity between the self and others in comparison to people with no identified mental health condition and people diagnosed with other mental health conditions including anxiety disorders, PD, and mania, as observed in comparison group studies (20, 30, 70, 71). Interestingly, the conceptual distance between actual self and non-self elements was observed to decrease as depression improved (70), implying a movement towards greater social identification as depression alleviated. Collectively, these findings substantiated the notion that people with depression were likely to construe the self as dissimilar to other people.
A contrasting pattern of how the self was construed in relation to others was observed in anxiety disorders and the experience of mania. People diagnosed with these conditions were found to construe greater similarity between the actual self and non-self elements, in comparison to other mental health conditions such as depression (20) and schizophrenia (30). People diagnosed with an anxiety disorder or mania were denoted to construe the self in relation to others in a similar way to people with no identified mental health condition (20, 30).
Finally, the studies could not reach a consensus on the construing of the self in relation to others in people diagnosed with PD. One comparison group study suggested that greater dissimilarity between the actual self and non-self elements was construed by participants with a PD (79), compared to people with no identified mental health condition, while another proposed that such a difference was not evident (20).
Some of the literature explicitly commented on the construing of specific non-self elements. Given the scarcity of studies that reported on specific non-self elements, the following findings are highly exploratory. A greater dissimilarity between the self and parental elements was construed within depression (71) and OCD (74), when compared to people with no identified mental health condition. Again, the reverse pattern seemed to be the case for anxiety disorders. Parental elements, specifically the mother, were construed more similarly to the self by participants who continued to experience heightened anxiety symptomology, relative to their counterparts who presented with reduced anxiety (73). However, it is important to note that the mother was construed negatively in this instance. People experiencing affective and schizoaffective disorders, most specifically schizoaffective psychosis and unipolar mania, appeared to construe their partner as more similar to their actual and ideal selves, compared to people with no identified mental health condition (29).
From the RGT, the authors made conclusions concerning the structure of the conceptual system and construing across mental health conditions. As the reviewers’ ability to assess what appeared to be comparative concepts was threatened by inconsistent definitions across studies, this review compartmentalised structure and process as the cognitive complexity, and the organisation and articulation of a person’s cognitive system. Thus, for the purpose of this review, the definition of cognitive complexity was summarised as the proportion of total variance accounted for by the first principal component and categorised as “simple” or “complex”, with larger proportions indicative of greater simplicity (e.g., (30), p. 250). Typically, an eigenvalue greater than 70% is generally considered to be indicative of “tight” construing (19, 96, 97). To note, the term cognitive complexity has been redefined in recent RGT literature as interpersonal cognitive differentiation (98); however, it will be referred to as cognitive complexity in this review due to this being the terminology used by the included studies. Cognitive organisation was classified as either “loose” or “tight”, with an overly loose organisation occurring when excess construct units are present and an excessively tight organisation when very few construct units exist (e.g., (83), p. 693). Articulation was subcategorised into “non-articulated”, either “monolithic” or “segmented”, and “articulated” structures. A “monolithic” structure comprised a singular primary cluster of constructs, while a “segmented” structure encompassed two or more primary clusters, without linking constructs between the clusters. An “articulated” structure consisted of two or more primary clusters joined by linking constructs [e.g., (74, 75)].
The RGT revealed that cognitive complexity was considered “simple” in depression and anxiety disorders, most specifically OCD (20, 30, 74). Conversely, a tentative interpretation of study findings suggested people experiencing mania and schizophrenia possessed highly “complex” cognitive systems (30); however, the reader is urged to interpret the findings of Ashworth et al. (30) with caution given that this was a non-significant finding. Affirming this, Phillips (84) indicated that greater cognitive complexity was associated with schizophrenia and a higher presence of paranoia and that individuals with greater cognitive complexity were more inclined to present with abstract and disorganised thinking in a sample of people with a range of different mental health conditions. Furthermore, cognitive complexity was depicted as significantly “more complex” in mania and schizophrenia than in depression, as shown in a comparison group study (30). From these findings, it could be inferred that a certain degree of cognitive complexity may be characteristic of specific mental health conditions. As such, cognitive complexity could be used as a dimension in which presentations of depression, anxiety, and OCD could be differentiated from presentations of psychosis and related experiences.
However, cognitive complexity may not serve as an appropriate dimension for distinguishing between people with an identified mental health condition and those without. No significant difference in the degree of cognitive complexity was found between a person with an identified mental health condition and a person with no identified mental health condition (71). Looking explicitly at specific mental health diagnoses, including depression, mania, schizophrenia, anxiety, OCD, and PD (20, 30, 71, 75), findings showed that cognitive complexity did not differ significantly between these mental health diagnoses and people with no identified mental health condition. However, one contradictory observation shown by Millar (74) suggested that cognitive complexity was in fact “more simple” in broad anxiety disorders and people experiencing OCD when compared to people with no identified mental health condition.
Findings regarding the organisation and articulation of the conceptual structure suggested that people with depression, a PD, or an anxiety disorder tended to have a “tightly” organised, “non-articulated”, and predominantly “monolithic” structure (20, 30). Krauthauser et al. (81) substantiated the notion that a “monolithic” conceptual structure tended to be associated with an anxiety or depressive disorder. People experiencing an anxiety or depressive disorder were found to experience greater cognitive contradiction within their construct system, a phenomenon that coincided with a tendency to have a “monolithic” structure and a less differentiated cognitive system (81). Moreover, a “monolithic” conceptual structure, greater cognitive contradiction, and poor differentiation appeared to coincide with greater psychological “disturbance”, higher anxiety and depression, and longer hospitalisation, for participants experiencing an anxiety or depressive disorder (81).
Several studies demonstrated that OCD specifically was said to be characterised by a “non-articulated” conceptual structure, specifically “monolithic” in nature (74–76). However, when collating comparison group studies, a consensus could not be reached on whether people with OCD and people with no identified mental health condition could be differentiated from one another on a measure of articulation (74–76).
In contrast, Ashworth et al. (30) portrayed that the articulation of the cognitive structure of people experiencing mania and schizophrenia was “non-articulated” but primarily “segmented”. One perspective revealed in some RGT studies was that schizophrenia was characterised by a single degree of organisation, “low” organisation, which appeared compatible with a “loose” cognitive system (78, 80). Klion (80) stated that two facets were encompassed within conceptual disorganisation—low construct interrelation (i.e., the degree of relationship between constructs) and low construct integration (i.e., the degree to which superordinate construct structures are utilised to subsume unrelated subordinate constructs)—and were dimensions that people with and without schizophrenia could be differentiated on. Specifically, the negative symptomology of schizophrenia (i.e., irritability, psychoticism, and motor retardation) was said to be associated with characteristics befitting “loose”, or low, organisation (78).
Conversely, an alternative suggestion was that an extremely “tight” or extremely “loose” pattern of cognitive organisation was observed in schizophrenia and schizoaffective disorders (77) and associated with the greatest volume of thinking errors indicative of thought disorder (83). In fact, construing of the self in either form (i.e., “tight” or “loose”) appeared to become “less extreme” as psychological stabilisation occurred in schizophrenia (77). This specific finding implied that it may be the extremity of cognitive organisation and not necessarily the form of organisation that is meaningful. While these findings were summarised to describe the cognitive organisation across the broad experiences of schizophrenia and psychosis, Adelman (1998) reported on distinct differences in organisation in separate conditions in this category of disorders. Adelman (77) showed that “tight” construing was present more frequently in schizoaffective disorder and that “loose” construing was more common in schizophrenia.
The findings suggested that distinct profiles of organisation and articulation were specific to depression, anxiety, OCD, PD, psychosis, and related disorders. The question of whether these conceptual structures were present only when people were actively unwell or whether it was inherent to them was not specifically explored by the included studies. However, some observations in the cases of schizophrenia and related disorders may have assisted with disentangling this. Adelman (77) observed that as psychological stabilisation occurred in schizophrenia, cognitive organisation became “less extreme”, i.e., less “loose” or less “tight”. Kubiak (78) noted that the resolution of a psychotic episode was linked with increased conceptual organisation. Therefore, both findings suggested that the profiles of conceptual systems denoted above may be specific to an active episode of schizophrenia and related disorders.
In depression and anxiety disorders, including OCD, cognitive complexity was described as “simple”, and conceptual structure was predominantly labelled as “non-articulated”, specifically “monolithic”, and construed as “tight” (20, 30, 74–76). A cognitive system comprised of such facets was said to result in a person with a rigid, inflexible, single-dimensional view of the world (95). His/her behaviour was said to be organised along two construct poles on a single dimension, which can produce extreme behavioural consistency. However, whether this conceptual structure was unique to these identified mental health diagnoses remains in dispute (20, 30, 74, 75).
For schizophrenia spectrum and psychotic disorders, two predominant suggestions relating to conceptual structure and organisation emerged. Firstly, some authors described the conceptual system consistent with these groups of disorders as mainly highly “cognitively complex”, “non-articulated”, “segmented”, and extremely “loose” (20, 78, 80, 84). Collectively, this description illustrates a person who likely holds a disorganised, fragmented, unstable, and chaotic view of the self and the world. Construing was portrayed as incoherent, and the person was likely to experience confusion, excessive doubt, and uncertainty. This group of people was said to have an increasingly diverse repertoire of how to perceive the self as well as behaviourally respond (78). Conversely, the alternative was that the conceptual structure associated with schizophrenia spectrum and psychotic disorders was not restricted to a singular dimension of cognitive organisation. Indeed, in the experience of schizophrenia spectrum and psychotic disorders, both patterns denoted above were said to occur depending on whether the person was presenting with an extremely “loose” or exceptionally “tight” conceptual structure (77, 83).
In a first of its kind, this systematic review of 21 studies synthesised findings relating to the content of construal, conceptual structure, and construing, captured through RGT methodology, completed by people whose diagnosed mental health condition necessitated inpatient psychiatric admission. A comprehensive exploration of the review’s aims was possible through the synthesis, leading to the emergence of several meaningful findings across a range of mental health diagnoses. As this review provided insight into the construal and construing processes that a person experiencing a mental health condition may use to make sense of the self, others, and their world, this synthesis may have the potential to significantly enhance therapeutic provision by highlighting potentially meaningful concepts that clinicians could use to better inform psychological assessment, formulation, and treatment.
One main finding that low self-esteem appeared to be present across a range of mental health conditions (20, 29, 30, 69–75, 78) was congruent with other literature that has demonstrated an association between low self-esteem and mental health conditions using alternative approaches to the RGT (99). This finding upheld the notions laid out by self-discrepancy theory that greater actual–ideal discrepancy (i.e., low self-esteem) results in emotional distress across diagnoses (31, 34). Therefore, low self-esteem is likely to be a central facet for exploration for any person accessing mental health services with an identified psychiatric diagnosis. It should be noted that the discrepancy between the actual self and ideal self is not the only way to explore self-esteem because there is also the distress associated with this discrepancy. However, RGT does not examine this distress dimension.
The synthesis of data pertaining to conceptual structure and construing revealed novel findings: mental health conditions possessed distinct profiles of cognitive complexity, organisation, and articulation, and people with an identified mental health condition tended to occupy a position of extremity on each dimension. Cognitive complexity emerged as a dimension potentially capable of distinguishing between presentations of depression, anxiety, PD, and OCD from presentations of psychosis and related disorders (30). Regarding conceptual organisation, Klion’s (80) and Kubiak’s (78) insights relating to construing in schizophrenia spectrum and psychotic disorders implied that these presentations could be distinguished from presentations of depression, anxiety, OCD, and PD based on this dimension. However, considering Adelman’s (74) and Phillips’ (83) notions of construing in schizophrenia spectrum and psychotic disorders, it implied that all aforementioned mental health conditions have the possibility to share the same form of cognitive organisation (i.e., an extremely “tight” conceptual structure). Therefore, the latter findings suggested that using a measure of organisation to differentiate between schizophrenia spectrum and psychotic disorders and presentations of depression, anxiety, OCD, and PD may not be possible.
Another important finding was that people with a mental health condition could not be consistently differentiated from people with no identified mental health condition on dimensions of cognitive complexity, organisation, and articulation (20, 30, 71, 74, 75). This finding, in conjunction with Adelman’s (77) and Kubiak’s (78) findings that psychological stabilisation coincided with the movement towards a more “moderate” conceptual organisation, could infer that to experience healthy, adaptive mental health, a person likely would fall in neither extreme and would exhibit “moderate” degrees of complexity, organisation, and articulation.
The RGT findings that provided insight into the typical conceptual complexity, organisation, and articulation associated with certain mental health conditions could be useful for practicing clinicians to be aware of and provide areas of focus for psychological intervention. Some authors characterised schizophrenia and related disorders by “low” organisation and “loose” construing (78, 80), implying that increasing conceptual organisation could be conducive to psychological stabilisation, and this could be achieved through psychological therapy. However, to the authors’ knowledge, there are no studies that explored the causal role of increasing conceptual organisation through psychological therapy in achieving psychological stabilisation in schizophrenia and related disorders. Alternatively, important insights provided by Adelman (77) and Phillips (83) suggested that, in fact, a movement towards a more “moderate” conceptual organisation is what is necessary to achieve psychological stability. Without the latter insights, clinicians could be at risk of increasing cognitive organisation in an already extremely “tight” and “highly” organised conceptual system, which could have detrimental effects on psychological wellbeing. These specific findings stress the importance of clinicians identifying the direction of construing specifically displayed by their inpatient service users diagnosed with schizophrenia and related disorders. In doing so, clinicians may be more likely to provide meaningful therapeutic interventions that would hopefully support achieving a timely discharge and appropriate transition to community mental health care.
Regarding the construing of others, the “extremity” of construing (e.g., moderate and extreme) was observed to be as important, if not more important, than how others were construed (e.g., negatively or positively), especially for participants diagnosed with PD and comorbid anxiety or depressive symptomology (69, 82). Hence, the extremity to which a service user construes others either positively or negatively, in addition to how they construe others, should be a target for intervention when working therapeutically with inpatient servicer users diagnosed with PD.
Moreover, this review highlighted that certain relationships hold greater significance than others in some mental health conditions, for example, partner figures in affective and schizoaffective disorders (29) and parental figures in depression (71), anxiety (73), and OCD (74). Clinicians should therefore assess how a service user construes and relates to specific significant others (e.g., the conceptual distance between self and non-self elements) as part of psychological therapy with people with a specific mental health diagnosis who are receiving support in inpatient facilities. Following assessment, service users could be supported to develop more adaptive, helpful ways of construing these significant non-self elements, resulting in psychological benefits, which would ultimately support achieving hospital discharge.
Finally, the findings relating to low self-esteem occurring in participants with mental health conditions not only provided substantiating evidence for the link between self-esteem and mental ill health but also demonstrated the usefulness of the RGT as an assessment tool of self-esteem. Thereby, RGT could provide an alternative, idiosyncratic way of exploring self-esteem for clinicians who are working therapeutically with inpatient service users.
Studies included in this systematic review varied in their application of the RGT, from the elements used, to the single or repeated application of the grid, to the method of construct elicitation. A strength of the RGT is its flexibility in application while maintaining the capability to reveal an individual’s conceptual system (15). However, several important limitations of the included literature were observed. Firstly, it became clear during the synthesis process that several definitions relating to the conceptual structure and construing had been used interchangeably across the literature, which meant that drawing conclusions about distinct concepts of cognitive complexity, articulation, and organisation was challenging. Nevertheless, by reflecting on the concepts collectively, many of the terms appeared compatible, and, subsequently, an overall picture of construing and conceptual structure within different mental health conditions appeared to emerge. However, readers are still advised to interpret these findings cautiously. Secondly, studies that requested participants to identify the preferred end of the construct pole often did not clearly define what was specifically meant by “preferred”. This lack of specificity could have meant there were varying interpretations of “preference” across studies, resulting in potential inconsistencies in collected data. A further disadvantage of requesting a participant to identify the preferred end is that a participant may experience ambivalence about which pole is preferred, which may threaten the validity of what is being measured (100).
Concerns arose relating to the studies that had used a “so-called” control group, often for comparative purposes. As mentioned above, as RGT originated from PCT, a classically personal, subjective approach (15), meaning RGT is characteristically idiosyncratic in nature (27, 101), drawing direct comparisons between individual repertory grids would not be viewed as typical, as a control group is normally used to compare one group to another on the same measure. The comparison group studies included in this review did not appear to ask participants directly to construe the self in relation to other people with different mental health conditions or persons without a diagnosis altogether; however, results appeared to be interpreted and presented in this way. While comparison group studies enabled some insights to be revealed, future studies may value including specific elements, such as “person without a mental health condition” or “person with other [specify] mental health condition”, to assess this.
Furthermore, despite this systematic review including information on 760 participants, from four different countries, spanning 45 years of research, the included studies were limited to western populations. This is an important limitation to highlight because a person’s self-construal can be shaped by his/her culture, and differences in self-construal between western and eastern cultures have been noted by some researchers (e.g., 139). Markus and Kitayama (102) emphasised an increased sense of interdependence in self-construal in eastern cultures, suggesting the self is construed as more interconnected with significant others, which differed to western cultures, in which independence and viewing the self as “separate” from others are accentuated. As the review findings could be culturally bound, to increase the generalisability of findings beyond western cultures, inclusion of studies from other geographical regions and cultures may be necessary. This limitation may be in part due to an actual scarcity of this type of research conducted with samples in non-western settings; however, it could also be due to biases introduced by the systematic review process itself. Due to the scope of the review, included studies were limited to publication in the English language; thus, instances of publication, location, and selection biases are possible. Restricting inclusion in this way may have prevented potentially meaningful studies written in different languages from being included (103). Indeed, eight studies were not considered for inclusion because the full text was not available in English. Thus, to expand the review’s breadth, future reviews could incorporate studies of multiple languages.
Eligible studies were limited to those conducted with inpatient participant samples because this approach increased the likelihood that the construals, construing, and conceptual structure were explored when a person’s mental health condition was more prominent or “active”, thereby better isolating the factor under investigation (i.e., mental ill health). Furthermore, limiting eligibility to inpatient participant samples ensured that the findings were specific to this population, which enabled more targeted clinical implications to be drawn. This specificity was essential in potentially enhancing the effectiveness of the psychologically driven assessment and intervention implications recommended by this review for those working with inpatient service users. Restricting the criteria in this way may have prevented meaningful insights from studies undertaken with outpatient samples from being collated as well as the opportunity to highlight meaningful similarities and/or differences between outpatient and inpatient participant samples. Therefore, to substantiate and potentially expand on the findings of this review, a future review encompassing inpatient- and outpatient-based participant samples may be valuable.
The use of an independent reviewer during the quality appraisal of included studies promoted objectivity and transparency regarding the methodological quality of included studies. As all studies were judged to contribute to the review and only three of the 21 studies obtained a moderate quality rating [i.e., (21, 72, 76)], no study was excluded based on methodological rigour. However, the quality appraisal process noted that almost all studies lacked sufficient information on recruitment data, did not critically discuss strengths and limitations, and fell short regarding the representativeness of their sample size. Therefore, because of these quality appraisal ratings, there are possible limitations to the conclusions produced by this review given that the conclusions are based on studies with potentially significant biases. The use of an independent reviewer for the systematic screening of articles enhanced consistency concerning article eligibility and strove to counteract subjectivity and certain biases that could have been introduced. Moreover, in accordance with the inclusion criteria, this review accepted grey literature, and therefore, the risk of publication biases was reduced.
This systematic review was the first to synthesise the findings of RGT studies that explored the content of construal, conceptual structure, and construing shown by people with an identified mental health condition necessitating inpatient admission. Similarities and differences in how a person perceived the self, others, and the self in relation to other people; the degree of cognitive complexity; and the organisation and articulation of conceptual structure were observed across different mental health conditions and between people with and without an identified mental health diagnosis. The review’s findings emphasise that clinicians should curiously assess and integrate the knowledge of conceptual systems into service user formulations to enable more targeted and meaningful psychological treatment. Clinicians should be cautious when service users present with a highly “tight” or extremely “loose” conceptual structure and instead strive to support the movement towards more “moderate” construing.
EW: Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Validation, Writing – original draft, Writing – review & editing. DH: Conceptualization, Formal analysis, Methodology, Supervision, Writing – review & editing. LG: Conceptualization, Formal analysis, Supervision, Writing – review & editing. AW: Conceptualization, Funding acquisition, Investigation, Methodology, Project administration, Resources, Supervision, Writing – review & editing, Writing – original draft.
The author(s) declare that financial support was received for the research and/or publication of this article. External funding was not provided for this systematic review. However, the University of Manchester supported the open-access publication of this manuscript.
The authors would like to thank Isabelle Shone for assisting with the study screening process and quality appraisal.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fpsyt.2025.1431798/full#supplementary-material
1. World Health Organisation.World mental health report: transforming mental health for all excessive summary (2022). Genève, Switzerland: World Health Organisation. Available online at: https://iris.who.int/bitstream/handle/10665/356119/9789240049338-eng.pdf?sequence=1 (Accessed February 01, 2024).
2. World Health Organisation. Depression and other common mental disorders: global health estimates (2017). Genève, Switzerland: World Health Organisation. Available online at: https://iris.who.int/bitstream/handle/10665/254610/WHO-MSD-MER-2017.2-eng.pdf?sequence=1 (Accessed November 13, 2023).
3. Sagar R, Dandona R, Gururaj G, Dhaliwal RS, Singh A, Ferrari A, et al. The burden of mental disorders across the states of India: the Global Burden of Disease Study 1990–2017. Lancet Psychiatry. (2020) 7:148–61. doi: 10.1016/S2215-0366(19)30475-4
4. Australian Bureau of Statistics. National study of mental health and wellbeing (2022). Canberra: Australian Bureau of Statistics. Available online at: https://www.abs.gov.au/statistics/health/mental-health/national-study-mental-health-and-wellbeing/latest-releasecite-window1 (Accessed November 11, 2023).
5. Bebbington PE, McManus S. Revisiting the one in four: the prevalence of psychiatric disorder in the population of England 2000-2014. Br J Psychiatry. (2020) 216:55–7. doi: 10.1192/bjp.2019.196
6. Department of Health and Social Care. Mental health promotion and mental illness prevention: the economic case (2011). London, UK: Department of Health. Available online at: https://www.gov.uk/government/publications/mental-health-promotion-and-mental-illness-prevention-the-economic-case (Accessed February 11, 2024).
7. Ford T, Vizard T, Sadler K, McManus S, Goodman A, Merad S, et al. Data resource profile: Mental health of children and young people (MHCYP) surveys. Int J Epidemiol. (2020) 49:363–364g. doi: 10.1093/ije/dyz259
8. Lipson SK, Lattie EG, Eisenberg D. Increased rates of mental health service utilization by U.S. college students: 10-year population-level trends (2007-2017). Psychiatr Serv. (2019) 70:60–3. doi: 10.1176/appi.ps.201800332
9. McManus S, Bebbington P, Jenkins R, Brugha T. Mental health and wellbeing in England: Adult Psychiatry Morbidity Survey 2014 (2016). Leeds, UK: NHS Digital. Available online at: https://www.researchgate.net/publication/309013865_Mental_health_and_wellbeing_in_England_Adult_Psychiatric_Morbidity_Survey_2014 (Accessed February 11, 2024).
10. National Health Service England. Acute impatient mental health care for adults and older adults (2023). Available online at: https://www.england.nhs.uk/long-read/acute-inpatient-mental-health-care-for-adults-and-older-adults/ (Accessed January 20, 2024).
11. Mental Health Team NHS Digital. Mental health bulletin 2021-22 annual report: official statistics, experimental statistics. England: NHS Digital, part of the Government Statistical Service (2022).
12. British Psychology Society & Association of Clinical Psychologists UK. Psychological services within the acute adult mental health care pathway: guidelines for service providers, policy makers and decision makers (2021). Available online at: https://acpuk.org.uk/wp-content/uploads/2021/10/REP162-Acute-Care-Briefing-WEB.pdf (Accessed March 10, 2024).
13. Weber C, Monero Flores V, Wheele TP, Miedema E, White EV. Patients’ health & well-being in inpatient mental health-care facilities: A systematic review. Front Psychiatry. (2021) 12:758039. doi: 10.3389/fpsyt.2021.758039
14. National Health Service England and National Health Service Improvement. National cost collection 2019/20 report (2021). Available online at: https://www.england.nhs.uk/wp-content/uploads/2021/06/National-Cost-Collection-2019-20-Report-FINAL.pdf (Accessed March 4, 2024).
16. Neimeyer RA, Mahoney MJ. Constructivism in psychotherapy. Washington: American Psychological Association (1995). doi: 10.1037/10170-000
17. Winter DA. Personal Construct Psychology. In: Encyclopedia of Personality and Individual Differences. Springer International Publishing, Cham (2020). doi: 10.1007/978-3-319-24612-3_1147
18. Kelly GA. A theory of personality: the psychology of personal constructs. 2nd ed. New York: Norton (1963).
19. Fransella F, Bell R, Bannister D. A manual for repertory grid technique. 2nd ed. Chichester, England: John Wiley & Sons Ltd (2004).
20. Axford S, Jerrom DW. Self-esteem in depression: a controlled repertory grid investigation. Br J Med Psychol. (1986) 59:61–8. doi: 10.1111/j.2044-8341.1986.tb02666.x
21. Rowe D. Poor prognosis in a case of depression as predicted by the repertory grid. Br J Psychiatry. (1971) 118:297–300. doi: 10.1192/bjp.118.544.297
22. Paget A, Ellett L. Relationships among self, others, and persecutors in individuals with persecutory delusions: a repertory grid analysis. Behav Ther. (2014) 45:273–82. doi: 10.1016/j.beth.2013.12.001
23. Slater P. The measurement of intrapersonal space by grid technique: exploration of intrapersonal space. London, England: John Wiley & Sons Ltd (1977).
24. Feixas G, Geldschläger H, Neimeyer RA. Content analysis of personal constructs. J Constr Psychol. (2002) 15:1–19. doi: 10.1080/107205302753305692
25. Burr V, King N, Heckmann M. The qualitative analysis of repertory grid data: Interpretive Clustering. Qual Res Psychol. (2022) 19:678–702. doi: 10.1080/14780887.2020.1794088
26. Hadley G, Grogan M. Using repertory grids as a tool for mixed methods research: A critical assessment. J Mix Methods Res. (2023) 17:209–27. doi: 10.1177/15586898221077569
28. Goffin K, Lemke F, Koners U. Repertory grid technique. Essential skills Manage Res. (2002) 1:199–225. doi: 10.4135/9781848605305.n11
29. Böker H, Hell D, Budischewski K, Eppel A, Härtling F, Rinnert H, et al. Personality and object relations in patients with affective disorders: idiographic research by means of the repertory grid technique. J Affect Disord. (2000) 60:53–9. doi: 10.1016/S0165-0327(99)00161-5
30. Ashworth CM, Blackburn IM, McPherson FM. The performance of depressed and manic patients on some repertory grid measures: a cross-sectional study. Br J Med Psychol. (1982) 55:247–55. doi: 10.1111/j.2044-8341.1982.tb01505.x
31. Higgins ET. Self-discrepancy: A theory relating self and affect. Psychol Rev. (1987) 94:319–40. doi: 10.1037/0033-295X.94.3.319
32. Yoon S, Dang V, Mertz J, Rottenberg J. Are attitudes towards emotions associated with depression? A Conceptual and meta-analytic review. J Affect Disord. (2018) 232:329–40. doi: 10.1016/j.jad.2018.02.009
33. Young KS, Sandman CF, Craske MG. Positive and negative emotion regulation in adolescence: Links to anxiety and depression. Brain Sci. (2019) 9:76. doi: 10.3390/brainsci9040076
34. Mason TB, Smith KE, Engwall A, Lass A, Mead M, Sorby M, et al. Self-discrepancy theory as a transdiagnostic framework: A meta-analysis of self-discrepancy and psychopathology. Psychol Bull. (2019) 145:372–89. doi: 10.1037/bul0000186
35. Rogers CR. A theory of therapy, personality, and interpersonal relationships as developed in the client-centred framework. New York: McGraw Hill (1959).
36. Baumeister RF. Self-concept, self-esteem, and identity. In: Derlega V, Winstead B, Jones W, editors. Personality: Contemporary theory and research. Nelson- Hall Publishers, San Francisco, CA (1999). p. 339–375.
37. Rosenberg M. Society and the adolescent self-image. Princeton, NJ: Princeton University Press (1965).
38. Henriksen IO, Ranøyen I, Indredavik MS, Stenseng F. The role of self-esteem in the development of psychiatric problems: a three-year prospective study in a clinical sample of adolescents. Child Adolesc Psychiatry Ment Health. (2017) 11:68. doi: 10.1186/s13034-017-0207-y
39. Orth U, Robins RW. Understanding the link between low self-esteem and depression. Curr Dir Psychol Sci. (2013) 22(6), 455–60. doi: 10.1177/0963721413492763
40. Hardin EE, Lakin JL. The Integrated Self-Discrepancy Index: a reliable and valid measure of self-discrepancies. J Pers Assess. (2009) 91:245–53. doi: 10.1080/00223890902794291
41. Gürcan-Yıldırım D, Gençöz T. The association of self-discrepancy with depression and anxiety: Moderator roles of emotion regulation and resilience. Curr Psychol. (2022) 41:1821–34. doi: 10.1007/s12144-020-00701-8
42. Leary MR, Schreindorfer LS, Haupt AL. The role of low self-esteem in emotional and behavioral problems: Why is low self-esteem dysfunctional? J Soc Clin Psychol. (1995) 14:297–314. doi: 10.1521/jscp.1995.14.3.297
43. Orth U, Robins RW, Widaman KF. Life-span development of self-esteem and its effects on important life outcomes. J Pers Soc Psychol. (2012) 102:1271–88. doi: 10.1037/a0025558
44. Rogers CR, Dymond R. Psychotherapy and personality change. Chicago: The University of Chicago Press (1954).
45. Sheehan MJ. A personal construct study of depression. Br J Med Psychol. (1985) 58:119–28. doi: 10.1111/j.2044-8341.1985.tb02624.x
46. Winter D, Sireling L, Riley T, Metcalfe C, Quaite A, Bhandari S. A controlled trial of personal construct psychotherapy for deliberate self-harm. Psychol Psychother. (2007) 80:23–37. doi: 10.1348/147608306X102778
47. Strauman TJ, Kolden GG, Stromquist V, Davis N, Kwapil L, Heerey E, et al. The effects of treatments for depression on perceived failure in self-regulation. Cognit Ther Res. (2001) 25:693–712. doi: 10.1023/A:1012915205800
48. Chuang SP, Wu JYW, Wang CS. Self-perception of mental illness, and subjective and objective cognitive functioning in people with schizophrenia. Neuropsychiatr Dis Treat. (2019) 15:967–76. doi: 10.2147/NDT.S193239
49. Corrigan PW, Watson AC. The paradox of self-stigma and mental illness. Clin Psychol. (2002) 9:35–53. doi: 10.1093/clipsy.9.1.35
50. Corrigan PW, Watson AC, Barr L. The self–stigma of mental illness: Implications for self–esteem and self–efficacy. J Soc Clin Psychol. (2006) 25:875–84. doi: 10.1521/jscp.2006.25.8.875
51. Corrigan PW, Kleinlein P. The impact of mental illness stigma. In: Corrigan PW eds. On the stigma of mental illness: implications for research and social change. Washington, Dc: American Psychology Association Press (2005).
52. Link BG, Phelan JC. Conceptualizing stigma. Annu Rev Sociol. (2001) 27:363–85. doi: 10.1146/annurev.soc.27.1.363
53. Dubreucq J, Plasse J, Franck N. Self-stigma in Serious Mental Illness: A systematic review of frequency, correlates, and consequences. Schizophr Bull. (2021) 47:1261–87. doi: 10.1093/schbul/sbaa181
54. García-Mieres H, Niño-Robles N, Ochoa S, Feixas G. Exploring identity and personal meanings in psychosis using the repertory grid technique: A systematic review. Clin Psychol Psychother. (2019) 26:717–33. doi: 10.1002/cpp.2394
55. Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev. (2021) 10:89. doi: 10.1186/s13643-021-01626-4
56. The well-built clinical question: a key to evidence-based decisions. ACP J Club. (1995) 123:A12. doi: 10.7326/ACPJC-1995-123-3-A12
57. Horsley T, Dingwall O, Sampson M. Checking reference lists to find additional studies for systematic reviews. Cochrane Database Syst Rev. (2011) 2011. doi: 10.1002/14651858.MR000026.pub2
58. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Publishing (2022). doi: 10.1176/appi.books.9780890425787
59. University of York. Searching for information: grey literature (2024). Available online at: https://subjectguides.york.ac.uk/searching/grey-lit (Accessed February 21, 2024).
60. Clarivate Analysis UK Ltd. EndNote Version 20 (2020). Available online at: https://endnote.com/ (Accessed April 6, 2024).
61. Popay J, Roberts H, Sowden A, Petticrew M, Arai L, Rodgers M, et al. Guidance on the conduct of narrative synthesis in systematic reviews: A product from the ESRC Methods Programme. Lancaster, England: Lancaster University (2006). doi: 10.13140/2.1.1018.4643
62. Evans D. Systematic reviews of interpretive research: interpretive data synthesis of processed data. Adelaide Australia: Aust J Advanced Nursing;. (2002) 50:22–6. doi: 10.37464/2003.202.2044
63. Sirriyeh R, Lawton R, Gardner P, Armitage G. Reviewing studies with diverse designs: the development and evaluation of a new tool: Reviewing studies with diverse designs. J Eval Clin Pract. (2012) 18:746–52. doi: 10.1111/j.1365-2753.2011.01662.x
64. Bourne D, Jankowich DA. The repertory grid technique. In: Ciesielska M, Jemielniak D, editors. Qualitative Methodologies in Organisation Studies. Palgrave Macmillam, Cham (2018).
65. Harrison R, Jones B, Gardner P, Lawton R. Quality assessment with diverse studies (QuADS): an appraisal tool for methodological and reporting quality in systematic reviews of mixed- or multi-method studies. BMC Health Serv Res. (2021) 21:144. doi: 10.1186/s12913-021-06122-y
66. Hill K. Personal and professional development: a repertory grid approach. Manchester: The University of Manchester (2014). Available at: https://www.proquest.com/docview/2230897097 (Accessed April 6, 2024).
67. Gillham R, Wittkowski A. Outcomes for women admitted to a mother and baby unit: a systematic review. Int J Womens Health. (2015) 7:459–76. doi: 10.2147/IJWH.S69472
68. Reid HE, Pratt D, Edge D, Wittkowski A. Maternal suicide ideation and behaviour during pregnancy and the first postpartum year: A systematic review of psychological and psychosocial risk factors. Front Psychiatry. (2022) 13:765118. doi: 10.3389/fpsyt.2022.765118
69. de Bonis M, De Boeck P, Lida-Pulik H, Hourtané M, Féline A. Self-concept and mood: a comparative study between depressed patients with and without borderline personality disorder. J Affect Disord. (1998) 48:191–7. doi: 10.1016/S0165-0327(97)00169-9
70. Hewstone M, Hooper D, Miller K. Psychological change in neurotic depression: A repertory grid and personal construct theory approach. BJPsych. (1981) 139:47–51. doi: 10.1192/bjp.139.1.47
71. Space LG, Cromwell RL. Personal constructs among depressed patients. J Nerv Ment Dis. (1980) 168:150–8. doi: 10.1097/00005053-198003000-00005
72. Rowe D. Estimates of change in a depressive patient. BJPsych. (1969) 115:1199–200. doi: 10.1192/bjp.115.527.1199
73. Catina A, Tschuschke V. A summary of empirical data from the investigation of two psychoanalytic groups by means of repertory grid technique. Group Anal. (1993) 26:433–47. doi: 10.1177/0533316493264005
74. Millar DG. A repertory grid study of obsessionality: distinctive cognitive structure or distinctive cognitive content? Br J Med Psychol. (1980) 53:59–66. doi: 10.1111/j.2044-8341.1980.tb02869.x
75. Makhlouf-Norris F, Norris H. The obsessive compulsive syndrome as a neurotic device for the reduction of self-uncertainty. BJPsych. (1973) 122:277–88. doi: 10.1192/bjp.122.3.277
76. Norris FM, Jones HG, Norris H. Articulation of the conceptual structure in obsessional neurosis. Br J Soc Clin Psychol. (1970) 9:264–74. doi: 10.1111/j.2044-8260.1970.tb00672.x
77. Adelman RW. Changes in construct systems of recovering patients. Texas, US: Texas A&M University – Commerce (1998). Available at: https://manchester.idm.oclc.org/login?url=https://www.proquest.com/dissertations-theses/changes-construct-systems-recovering-psychiatric/docview/304485228/se-2 (Accessed April 6, 2024).
78. Kubiak JM. Hierarchical structure of intrapersonal and interpersonal personal construct systems: assessing change in a chronic schizophrenia sample during psychosocial rehabilitation. Nebraska, US: The University of Nebraska – Lincoln (1998). Available at: https://manchester.idm.oclc.org/login?url=https://www.proquest.com/dissertations-theses/hierarchical-structure-intrapersonal/docview/304460621/se-2 (Accessed April 6, 2024).
79. de Bonis M, De Boeck P, Lida-Pulik H, Féline A. Identity disturbances and self-other differentiation in schizophrenics, borderlines, and normal controls. Compr Psychiatry. (1995) 36:362–6. doi: 10.1016/S0010-440X(95)90117-5
80. Klion RE. Construct system organization and schizophrenia: The role of construct integration. J Soc Clin Psychol. (1988) 6:439–47. doi: 10.1521/jscp.1988.6.3-4.439
81. Krauthauser H, Bassler M, Potratz B. A new approach to the identification of cognitive conflicts in the repertory grid: A nomothetic study. J Constr Psychol. (1994) 7:283–99. doi: 10.1080/10720539408405235
82. Tschuschke V, Dies RR. Intensive analysis of therapeutic factors and outcome in long-term inpatient groups. Int J Group Psychother. (1994) 44:185–208. doi: 10.1080/00207284.1994.11490742
83. Phillips WM. The minimax problem of Personal Construct organization and schizophrenic thought disorder. J Clin Psychol. (1981) 37:692–8. doi: 10.1002/1097-4679(198110)37:4<692::AID-JCLP2270370402>3.0.CO;2-M
84. Phillips WM. Role Construct Repertory Technique: some relationships with personality, psychopathology and intelligence for neuropsychiatric inpatients. Psychol Rep. (1976) 38:951–5. doi: 10.2466/pr0.1976.38.3.951
85. Andreasen NC. The scale for the assessment of positive symptoms (SAPS). Iowa city: University of Iowa (1984).
86. Cooper J. The leyton obsessional inventory. Psychol Med. (1970) 1:48–64. doi: 10.1017/s0033291700040010
87. Beck AT. An inventory for measuring depression. Arch Gen Psychiatry. (1961) 4:561. doi: 10.1001/archpsyc.1961.01710120031004
88. World Health Organisation. The ICD-10 classification of mental and behavioural disorders. Genève, Switzerland: World Health Organisation (1993).
89. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 3rd ed. Washington, DC: American Psychiatric Association (1980).
90. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 2nd ed. Washington, DC: American Psychiatric Association (1968).
91. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 3rd ed. Washington, DC: American Psychiatric Association (1987).
92. McIntyre RS, Berk M, Brietzke E, Goldstein BI, López-Jaramillo C, Kessing LV, et al. Bipolar disorders. Lancet. (2020) 396:1841–56. doi: 10.1016/S0140-6736(20)31544-0
93. Lobo MA, Moeyaert M, Baraldi Cunha A, Babik I. Single-case design, analysis, and quality assessment for intervention research. J Neurol Phys Ther. (2017) 41:187–97. doi: 10.1097/NPT.0000000000000187
94. Feixas G, Montesano A, Compañ V, Salla M, Dada G, Pucurull O, et al. Cognitive conflicts in major depression: between desired change and personal coherence. Br J Clin Psychol. (2014) 53:369–85. doi: 10.1111/bjc.12050
95. Feixas G, Moggia D, Niño-Robles N, Aguilera M, Montesano A, Salla M. Measuring cognitive rigidity in construing self and others with the repertory grid technique: further test of the cognitive model for depression. Int J Cogn Ther. (2021) 14:656–70. doi: 10.1007/s41811-021-00122-w
96. Blagden N, Needs A. Personal construct psychology and repertory grids: acknowledging and exploring perspectives. In: Liell GC, Fisher MJ, Jones LF, editors. Challenging bias in forensic psychological assessment and testing theoretical and practical approaches to working with diverse populations. Routledge, London (2022).
97. Winter DA. Personal construct psychology in clinical practice: theory, research, and applications. London: Routledge (1992).
98. Feixas G, Bach L, Laso E. Factors affecting interpersonal construct differentiation when measured using the repertory grid. J Constr Psychol. (2004) 17:297–311. doi: 10.1080/10720530490483202
99. Sowislo JF, Orth U. Does low self-esteem predict depression and anxiety? A meta-analysis of longitudinal studies. Psychol Bull. (2013) 139:213–40. doi: 10.1037/a0028931
100. Winter DA, Bell RC, Watson S. Midpoint ratings on personal constructs: constriction or the middle way? J Constructivist Psychol. (2010) 23:337–56. doi: 10.1080/10720537.2010.502428
101. Winter DA. Repertory grid technique as a psychotherapy research measure. Psychother Res. (2003) 13:25–42. doi: 10.1093/ptr/kpg005
102. Markus HR, Kitayama S. Culture and the self: Implications for cognition, emotion, and motivation. Psychol Rev. (1991) 98:224–53. doi: 10.1037/0033-295X.98.2.224
Keywords: adult mental health, psychiatric disorder, service user, repertory grid, personal construct theory, inpatient admission, construal of self
Citation: Wozniak EE, Hare DJ, Gregg L and Wittkowski A (2025) Construal of self as a mental health inpatient: a systematic review and narrative synthesis of repertory grid studies. Front. Psychiatry 16:1431798. doi: 10.3389/fpsyt.2025.1431798
Received: 12 May 2024; Accepted: 12 February 2025;
Published: 04 April 2025.
Edited by:
Hao Yao, Shanghai Mental Health Center, ChinaReviewed by:
Celine Baeyens, Université Grenoble Alpes, FranceCopyright © 2025 Wozniak, Hare, Gregg and Wittkowski. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Anja Wittkowski, YW5qYS53aXR0a293c2tpQG1hbmNoZXN0ZXIuYWMudWs=
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.