- 1 Research Division, Department of Pain Medicine and Palliative Care, Institute for Non-Invasive Brain Stimulation, Beth Israel Medical Center, New York, NY, USA
- 2 Department of Neurology, Albert Einstein College of Medicine, Bronx, NY, USA
- 3 College of Nursing, New York University, New York, NY, USA
- 4 Department of Psychiatry, Institute for Social and Psychiatric Initiatives, New York University, New York, NY, USA
- 5 Duke University, Durham, NC, USA
- 6 College of Dentistry, New York University, New York, NY, USA
Transcranial direct current stimulation (tDCS) is a novel non-invasive neuromodulatory method that influences neuronal firing rates and excitability of neuronal circuits in the brain. tDCS has been shown to relieve Major Depressive Disorder (MDD) in the general population, suggesting its potential for other vulnerable populations with high MDD prevalence. Aims: This study evaluated the feasibility, safety, acceptability, and clinical outcomes of a 2-week tDCS antidepressant treatment in HIV-MDD co-diagnosed patients, and the feasibility of collecting serum and saliva for analysis of immunity biomarkers. Methods: Ten enrolled patients underwent baseline evaluation and started the tDCS treatment (Monday–Friday for 2 weeks) delivered with Phoresor II 850 PM for 20 min at 2 mA at each visit, using two saline-soaked sponge electrodes placed over the F3 position of EEG 10–20 system and the contralateral supraorbital region. Outcome measures were collected at baseline, after the last tDCS and 2 weeks later. A quantitative microarray (Ray Bio Tech Inc.) for TH1/TH2 cytokines was used for saliva and plasma analysis. Results: Analyzable outcome-data were obtained from eight subjects. Depression scores significantly decreased (p < 0.0005) after the treatment. No serious adverse events occurred. Several transient minor AEs and occasional changes of blood pressure and heart rate were noted. Mini-mental state examination scores remained unchanged or increased after the treatment. All subjects were highly satisfied with the protocol and treatment results and described the desire to find new treatments for HIV-MDD as motivating participation. Conclusion: Findings support feasibility and clinical potential of tDCS for HIV-MDD patients, and justify larger-sample, sham-controlled trials.
Introduction
Transcranial direct current stimulation (tDCS) has been shown to be a powerful technique for non-invasive neuromodulation (Nitsche and Paulus, 2010). The primary mechanism of tDCS is a subthreshold modulation of neuronal resting membrane potential which induces a polarity-dependent modification of N-Methyl-D-aspartate (NMDA) receptor function (Antal et al., 2010; Nitsche and Paulus, 2010) that plays a role in neuroplasticity. Some of tDCS induced changes occurs immediately during the stimulation (so called intra-tDCS changes), while others occur later as short-lasting or long-lasting after-effects (Nitsche and Paulus, 2010). As suggested by pharmacological studies (Liebetanz et al., 2002; Nitsche et al., 2004), the intra-tDCS effects depend on the activity of sodium and calcium channels but not on efficacy changes of NMDA and gamma-aminobutyric acid (GABA) receptors, and thus are probably generated solely by polarity specific shifts of resting membrane potential. However, the after-effects have been shown to be protein synthesis dependent (Gartside, 1968; Hattori et al., 1990; Nitsche and Paulus, 2010) and also involve modulations of NMDA receptors efficacy. (Liebetanz et al., 2002; Nitsche et al., 2005; Nitsche and Paulus, 2010).
In several randomized controlled studies utilizing 2 or 4 week tDCS treatment protocols, tDCS delivered over the dorsolateral prefrontal cortex (DLPFC) was shown to safely relieve Major Depressive Disorder (MDD) in the general population (Fregni et al., 2006; Boggio et al., 2008a; Rigonatti et al., 2008; Murphy et al., 2009; Nitsche et al., 2009; Kalu et al., 2012). Although the mechanisms of tDCS antidepressant effect are not fully understood, it is reasonable to assume that tDCS might have induced a change in the DLPFC activity which is highly relevant to alterations of mood-related neuronal networks (Boggio et al., 2008a).
This suggests the clinical potential of tDCS treatment for other vulnerable populations with high prevalence of MDD, such as persons with HIV infection. Various estimates (McHorney et al., 1994; Lyketsos, 1995; Boland, 1997; Stober et al., 1997; Chander et al., 2006; Hartzell et al., 2008; Rabkin, 2008) suggest that up to 48% of HIV-infected patients have MDD comorbidity. MDD accelerates HIV disease progression, jeopardizes the completion of antiretroviral treatment and is a potent risk factor for transmission of the virus to others (Wilson et al., 2007). Despite the fact that MDD is the most common psychiatric disorder in HIV populations after substance abuse (Rabkin, 2008), conventional antidepressant treatments, such as medication or psychotherapy, leave many patients with undertreated depressive symptoms (Lyketsos, 1995; Chander et al., 2006; Hartzell et al., 2008). For treatment-resistant depressed patients, depression is often lifelong and disabling and represents a significant source of suffering, disruption in role functioning, economic burden to society, and mortality (Gaynes et al., 2008).
Although tDCS treatment may greatly improve the quality of life of HIV patients suffering MDD, to our knowledge, no previous tDCS study has included such patients. Therefore, we carried out a quantitative and qualitative open-label pilot trial to evaluate the safety, tolerability, acceptability, and clinical outcomes of a 2-week tDCS treatment protocol to treat MDD in HIV-infected patients and explore the feasibility of collecting serum and saliva cytokines for future analysis. The purpose of the study was to determine overall feasibility of the study protocol in an HIV patient-sample and to provide initial data for sample size estimates and power for a future, sham-controlled randomized trial (RCT).
Materials and Methods
Subjects
Ten adult subjects diagnosed with HIV and MDD who fully met the following inclusion criteria participated in the study.
Inclusion Criteria comprised of the following: (i) Diagnosed with HIV; (ii) MDD as measured by the Hamilton Depression Rating Scale score at least >17 at the time of enrollment as well as 1 week later at the time of the baseline; (iii) MDD as measured by the Montgomery-Asberg Depression Rating Scale (MADRAS) score at least >11 at the time of enrollment as well as at the baseline.
Subjects were excluded from participation if they met the following exclusion criteria.
Exclusion Criteria: (i) Diagnosed with AIDS; (ii) Active and/or history of schizophrenia, schizoaffective disorder, psychosis, mental retardation, substance dependence, or abuse within the past year (except nicotine), bipolar disorder, psychotic features, amnesic disorder, dementia, delirium, or obsessive-compulsive disorder; (iii) History of opportunistic infection affecting the brain; (iv) Methadone treatment; (v) History of neurological disorder or seizure (except induced by electroconvulsive therapy, ECT), increased intracranial pressure, brain surgery, or head trauma with loss of consciousness for >15 min, implanted electronic device, metal in the head; (vi) History of autoimmune, endocrine, or vascular disorder, unstable cardiac disease, uncontrolled hypertension, or sleep apnea; (vii) Active suicidal intent; (viii) Pregnancy; (ix) Unable to follow instructions or complete assessment tools in English.
Participation in this study did not require any changes in the patient’s medication regimen.
Procedures
Overview
The protocol consisted of 12 study visits. At the initial visit, the informed consent was obtained and patients were screened for eligibility. Baseline values of outcome measures were established at the initial visit and 1 week after the initial visit. The subjects who fully met the inclusion criteria then started a 2-week course of tDCS treatment (10 sessions, visits #2 – #11, Monday–Friday for 2 weeks, each session consisting of 20 min of tDCS). Two weeks after the last tDCS treatment, participants came for visit #12 (Follow-up/Completion). The primary outcome measure was safety; secondary outcomes were treatment benefits/clinical outcomes, tolerability, acceptability, and patients’ satisfaction. The outcome measurement time points were before the first tDCS treatment, immediately after the last tDCS treatment and at the follow-up visit which was conducted 2 weeks after the treatment.
Transcranial direct current stimulation
Transcranial direct current stimulation was delivered by trained study personnel using the battery-operated device Phoresor II Auto (Model No. PM850) with two saline-soaked sponge electrodes of size 6 cm × 6 cm, with a rubber rim of 1 cm and sponge-skin contact area of 5 cm × 5 cm. The anode was placed over the left DLPFC as determined by the international EEG 10–20 classification (point F3), and the cathode was over the contralateral supraorbital region. The current was delivered at the intensity of 2 mA for 20 min. These parameters of stimulation were successfully and safely used in many previous tDCS studies (Fregni et al., 2006; Rigonatti et al., 2008; Knotkova et al., 2009) and were well within safety limits. A detailed review of tDCS safety and parameters of stimulation-protocols in human subjects appear in Sundaram et al. (2009). The tDCS treatment course was considered complete if the subject received at least 8 of 10 treatment sessions, and if the two missed sessions were not on consecutive days.
Assessment methods
(a) The HamD (HamD-24) is the most widely used scale for patient selection and follow-up in research studies of depression treatments. In this clinician-administered instrument, the clinician chooses the best response to each of 24 items by interviewing the patient and by observing the patient’s symptoms. Content includes symptoms of depression designated in the Diagnostic and Statistical Manual of Mental Disorders, fourth edition, text revision; DSM IV-TR) published by the American Psychiatric Association. These include: low mood, insomnia, agitation, anxiety and weight change. The instrument is highly reliable (alpha = 0.87) when the clinician uses the Structure Interview Guide for the Hamilton (SIGH; Williams, 1998) as was done in this study.
(b) The Montgomery-Asberg Depression Rating Scale (MADRAS) is a clinician-administered 10-item rating scale to assess the severity of a patient’s depressive symptoms within the last 7 days. The items were taken from the 65-item Comprehensive Psychopathological Rating Scale (CPRS) and were selected because of their sensitivity to change. The 10 selected items are rated on a scale of 0–6 with anchors at 2-point intervals. The interviewer is encouraged to use his or her observations of the patient’s mental state as an additional source of information. Total scores on the MADRAS range from 0 to 60. It has been shown to have high inter-rater reliability (Spearman r = 0.94) and good concurrent validity (r with HamD between 0.83 and 0.94; Davidson, 1986). We have used this psychometric tool in addition to HamD because MADRAS offers an alternative view of depressive illness, and may be more sensitive than HamD to some depressive symptoms such as hypersomnia, increased appetite, and concentration/indecision.
(c) Mini-Mental State Examination (MMSE; Folstein et al., 1975) is a widely used clinical instrument for quick detection of cognitive impairment and assessing its severity, as well as for monitoring cognitive changes over time. In this study, MMSE was used as a part of the physical and mental evaluation of subjects at the initial and at the completion visit.
(d) Patient’s Satisfaction Rating Scale is a combined 4-point (0–3) scale for participants’ self-rating when answering the question “How satisfied were you with the results of the tDCS treatment?” 0 = not at all; 1 = a little bit; 2 = a lot; 3 = fully satisfied.
(e) Patient’s Daily Records: Throughout the study, participants kept at-home daily records (i.e., Daily Diaries) detailing consumption of medications, and potential changes in health status, including depression, pain, fatigue, and level of physical activity.
(f) Monitoring of the adverse events (AEs) was performed throughout the study using the following: direct contact of study personnel with the participant at study visits, patient’s daily diaries, regular phone calls from the study personnel to the patient in the follow-up period. In addition, subjects were instructed to notify the study personnel immediately if any concerns or if any unexpected/sudden changes of health occurred.
(g) Qualitative Interviews: Giorgi’s phenomenology (Giorgi, 1985) was the method used to describe the experiences of persons undergoing tDCS for treatment of depression. In-person audio-taped interviews were conducted at the completion visit by an experienced qualitative researcher and were immediately transcribed verbatim. Interviews ranged from 30 min to 1 h. Each participant was asked the open-ended question, “Please tell me about your experience undergoing tDCS for the treatment of depression.” Probes included the following questions: “What was the experience like for you? What should we continue to do and what should we change to make the experience better for patients?” Themes were derived using the constant comparative method (Thorne, 2000).
Others
One of the study aims was to determine the feasibility of collecting serum and saliva samples for immunity-biomarkers assessment. At the baseline, after the last tDCS treatment, and at the 2-week follow-up visit, approximately 10 ml of plasma and 10 ml of whole stimulated saliva were collected from subjects. Fluid samples were pipetted in to.0 5 ml aliquots and immediately frozen at −80°C, to be prepared for analysis using RayBiotech TH1/TH2 antibody arrays. Results of the analysis will be reported in a separate manuscript (in preparation).
Statistical analysis
To examine change in scores from pre- to post-tDCS administration to 2-week follow-up, we conducted a repeated measures analysis of variance using Predictive Analytics SoftWare (PASW) Statistics, formerly known as Statistical Package for the Social Sciences (SPSS) before it was acquired by IBM. First, analyses determined whether the sphericity assumption was violated for the analysis of the HamD and MADRAS scores. Helmert contrasts were used when comparing (1) the pre-tDCS with the average of the post-tDCS scores and the 2-week follow-up scores, and (2) the post-tDCS scores and the 2-week follow-up scores.
Enrollment and the study procedures took place at Beth Israel Medical Center, New York, NY. Biochemical analysis took place at New York University, New York, NY. The study was approved by the Institutional Review Boards at both institutions.
Results
Demographic Characteristics and Subjects’ Flow through the Study
The 10 study participants included 5 males and 5 females. Their mean age was 52.5 (s.d. = 6.3) years, ranging from 38 to 59 years. Almost all (9 of 10) were African American and one was non-Hispanic Caucasian. Five were living with partners/spouses and the others were separated, single, or never married, and living alone. Although five of the participants had attended college, only one was working (and on a part-time basis) and three of the remaining nine were disabled. Scores on the MMSE examination at the baseline were 28.0 (s.d. = 3.1), range 20–30, consistent with the possibility of some mild cognitive impairment for a few of the participants. Regarding their health, the 10 participants had been living, on average, with HIV for 19.7 (s.d. = 4.1) years, range10–26 years. All had co-morbid conditions, including three with hepatitis C virus, three with hypertension, and five with a substance abuse history. All had MDD as reflected in their scores of 17 or greater on the HamD scale; 24.8 (5.8), range 17–34, and a score of 14 or greater on the MADRAS scale: 24.6 (7.4), range 14–34. Before the study, none of the participants had ever had ECT, transcranial magnetic stimulation (TMS), or tDCS treatment for their depression or other reasons. All subjects were taking HIV antiretroviral medication. Besides that, several subjects were on stable regimens of other medications, including the following CNS-acting agents: Antidepressants – selective serotonin reuptake inhibitors [Celexa, Zoloft] (subjects #3,6,9), tetracyclic antidepressants [Remeron] (subject #4), and serotonin-norepinephrine reuptake inhibitors [Effexor] (subject #4); Antipsychotics [Zyprexa, Seroquel, Risperidone] (subjects #4,9); Anticonvulsants [Depakote, Gabapentin] (subjects #4,7); Sedative [Ambien] (subject #9); and Histamine H2-receptor antagonists [Famotidine] (subject #3).
The 10 participants were recruited from a pool of 15 subjects referred to the study. Of these, five were interested in participation but could not participate for various reasons (e.g., could not make commitment to 10 consecutive days of tDCS, lived far away). Ten subjects provided informed consent and were screened according to the inclusion/exclusion criteria. All 10 subjects satisfied the criteria and began the study protocol. Analyzable outcome-data were obtained from 8 subjects; 7 of them completed all 10 treatments, and 1 subject completed 8 of 10 treatments (missed the last two treatments due to the death of a family member). Two remaining subjects received only two initial treatment sessions and did not continue due to conflicts with their personal schedules.
Changes in Depression Scales before and after TDCS Administration
Hamilton depression rating scale
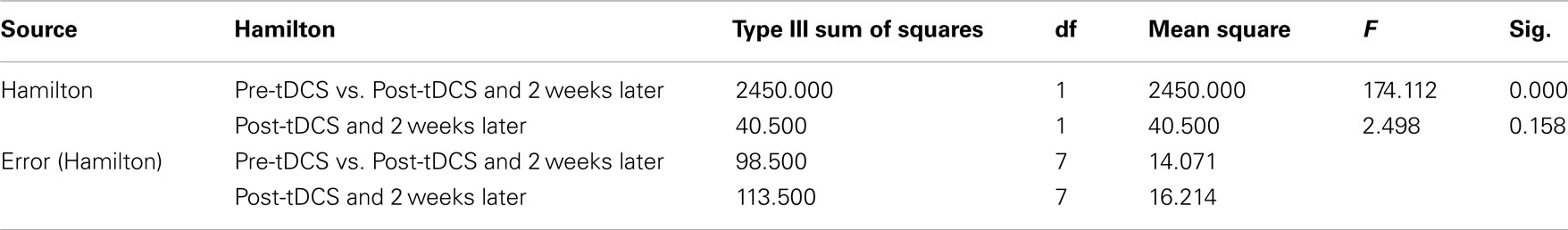
Hamilton Depression Rating Scale scores from the eight subjects at baseline, immediately after the last tDCS treatment and at 2-week follow-up averaged 26.3 (s.d. = 5.5), range 17–34; 9.9 (s.d. = 4.3), range 5–17; and 7.6 (s.d. = 6.7), range 1–19, respectively. The mean HamD scores differed significantly between time points according to the repeated measures ANOVA: F(2, 14) = 94.555; p < 0.0005. The sphericity assumption (see Materials and Methods) was not violated for the HamD scores (p = 0.926). As can be seen in Table 1, the pre-tDCS HamD scores were significantly higher than the average of the post-tDCS HamD scores and the 2-week follow-up HamD scores [F(1, 7) = 174.112; p < 0.0005], indicating a highly significant decrease in depression scores.
Notably, the post-tDCS HamD scores did not differ significantly from the 2-week follow-up HamD scores [F(1, 7) = 2.498; p = 0.158], indicating duration of the decrease of depressive symptoms in the follow-up period.
Madras
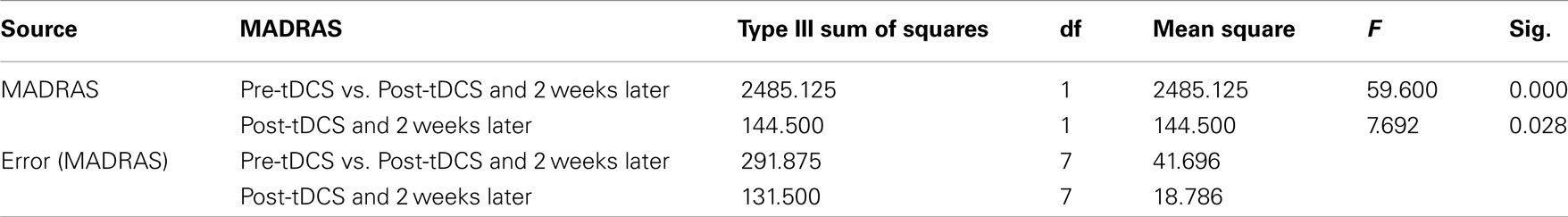
On MADRAS, scores for the eight patients at baseline, immediately after the last tDCS treatment and at 2-week follow-up averaged 26.8 (s.d. = 6.7), range 14–34; 11.3 (s.d. = 6.9), range 6–26; and 7.0 (s.d. = 7.4), range 0–20, respectively. According to the repeated measures ANOVA, the mean MADRAS scores differed significantly between time points: [F(2, 14) = 46.490; p < 0.0005]. The sphericity assumption was not violated for the MADRAS scores (p = 0.421). As can be seen in Table 2, the pre-tDCS MADRAS scores were significantly higher than the average of the post-tDCS HamD scores and the 2-week follow-up MADRAS scores [F(1, 7) = 59.600; p < 0.0005], indicating a highly significant decrease in depression scores.
The post-tDCS MADRAS scores differed significantly from the 2-week follow-up MADRAS scores [F(1, 7) = 7.692; p = 0.028], indicating a further decrease in depression scores in the follow-up period.
Safety
Safety measures included monitoring side effects throughout the study, systolic and diastolic blood pressure and heart rate before and after each tDCS session, and MMSE at baseline and at the completion of the study.
Side effects
No serious adverse events (SAEs) occurred. Several minor non-serious AEs that occurred during the treatment course or in the follow-up period can be seen in Table 3. All these minor events were transient and fully resolved.
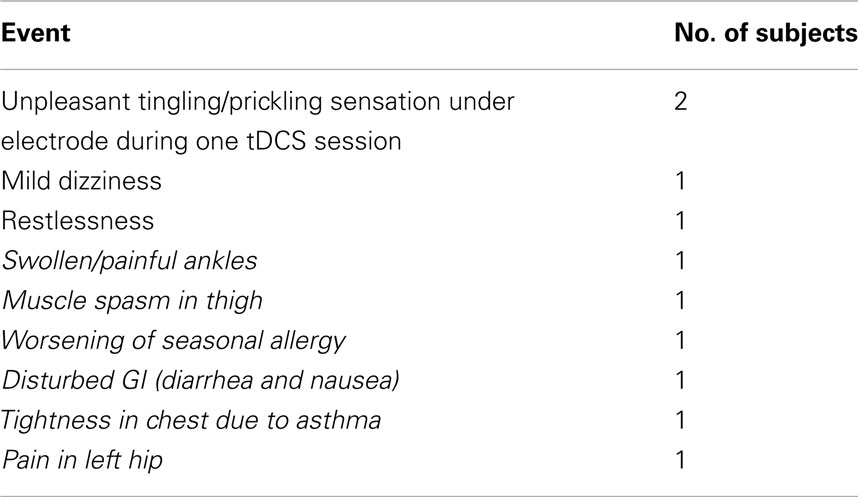
Table 3. Adverse events presented in the table in italics were rated by the study physician as unlikely related or unrelated to the study procedure.
Systolic and diastolic blood pressure and heart rate
For each participant, and for each of the 10-days of the tDCS administration, we examined changes in systolic and diastolic blood pressure and heart rate before and after tDCS administration. For systolic and diastolic blood pressure, we considered a change from pre- to post-tDCS administration to be clinically significant if it varied by 10 mmHg or more. For heart rate, we considered a change from pre- to post-tDCS administration to be clinically significant if the change was 10% or greater.
(a) Clinically significant changes in systolic blood pressure
For the eight participating patients, clinically significant change in systolic blood pressure varied from −27 to 20 mmHg. All patients had such a significant change on at least one of the days of tDCS administration, ranging from 1- to 5-days. As can be seen in Table 4, there were 6 clinically significant increases and 19 clinically significant decreases in systolic blood pressure.
Regarding the days on which the changes occurred, they included a change for one of the patients on each of days 6 and 9; for two patients on days 1, 3, 5, and 8; for three patients on days 2 and 10; for four patients on day 7; and for five patients on day 4.
(b) Clinically significant changes in diastolic blood pressure
For the eight participating patients, clinically significant change in diastolic blood pressure varied from −20 to 15 mmHg. Six of the eight patients had such a significant change on at least one of the days of tDCS administration, ranging from 1- to 5-days. As can be seen in Table 4, there were five clinically significant increases and 10 clinically significant decreases in diastolic blood pressure. Regarding the days on which the changes occurred, they included no changes for any patients on day 2; changes for one patient on days 5, 6, 9, and 10; for two patients on days 1, 3, 7, and 8; and for three patients on day 4.
(c) Clinically significant changes in heart rate
Each of the eight evaluated subjects had at least 1 day on which there was a clinically significant change in heart rate, ranging from 1- to 5-days. There were nine clinically significant increases and 14 clinically significant decreases in heart rate (Table 4). Regarding the days on which the changes occurred, they included change for one patient on days 2, 5, 9, and 10; for two patients on days 3 and 6; for three patients on days 7 and 8; for four patients on day 1; and for five patients on day 4.
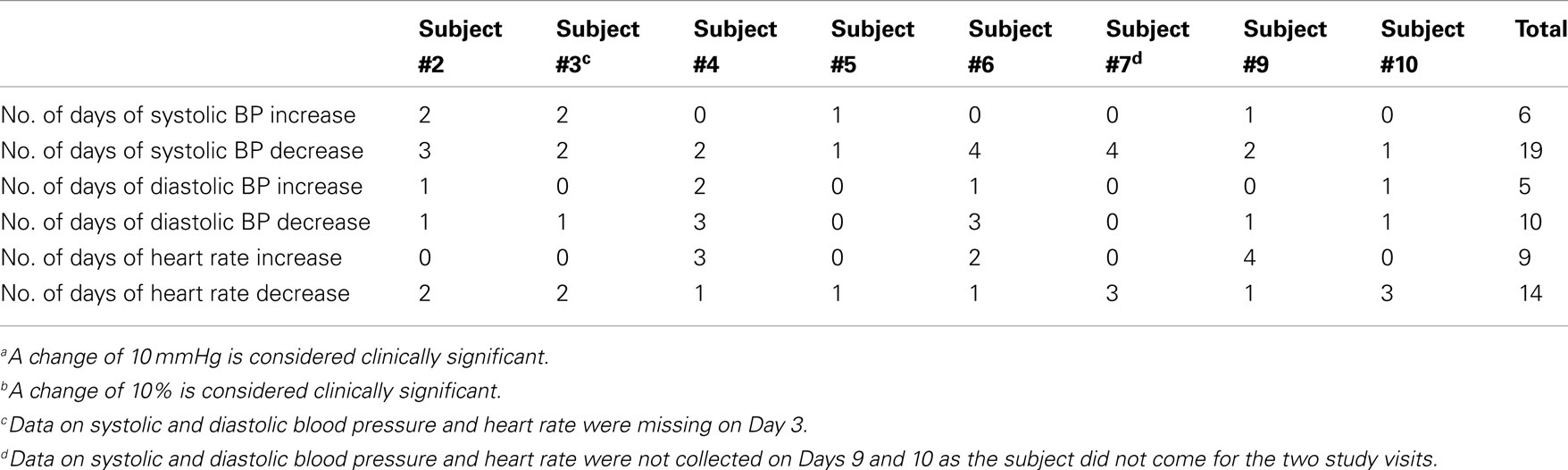
Table 4. Clinically significant change from pre- to post-tDCS administration in systolica and diastolic blood pressurea and heart rateb.
Mini-mental state evaluation before and after treatment
Scores for the eight subjects on the MMSE ranged from 20 to 30 (mean = 28; s.d. = 3.02) before the tDCS treatment and from 25 to 30 (mean = 29.0; s.d. = 1.8) at the follow-up. The individual participant scores remained either unchanged or increased after the treatment. There was no case of the score-decrease between the baseline and the end of the study assessment.
Adherence to the Treatment
Adherence to the treatment was determined as the percentage of participants who finished the 2-week tDCS treatment course, and the percentage who completed the entire study, including participation in the 2-week follow-up. Only two subjects (20%) did not receive the minimum of required eight tDCS treatment sessions. Each of the two subjects completed two treatment sessions at the beginning of the treatment course. Both subjects dropped out due to a personal-schedule conflict and did not come for the follow-up evaluation.
Eight subjects (80% of patients) received the required eight or more treatment sessions. Of these, six subjects did not miss any treatment sessions, one subject missed one treatment, and one subject missed two treatments. As the two missed treatments (last two treatments of the course) for this latter subject were on consecutive days, the subject as per protocol did not finish the treatment course and was not considered a completer. However, all other data and evaluations were collected from this subject and included in the analysis. Qualitative evaluation of this non-completer revealed that the subject missed the two sessions due to the death of family member. The subject’s frequent communication with the study personnel revealed high motivation to participate in the study procedures and exhibited behavior typical for treatment-adherent subjects. If this non-completer is eliminated from the analysis, there were very few substantial changes in study results. In particular, as was the case with the eight participants, the pre-tDCS HamD scores were significantly higher than the average of the post-tDCS HamD scores and the 2-week follow-up HamD scores for the seven completers [F(1, 6) = 137.388; p < 0.0005]. In addition, the pre-tDCS MADRAS scores were significantly higher for the seven completers than the average of the post-tDCS MADRAS scores and the 2-week follow-up MADRAS scores [F(1, 6) = 72.199; p < 0.0005]. For the seven completers, analyses also indicate duration of the decrease in depressive symptoms from immediately post-tDCS to the 2-week follow-up on both the HamD and the MADRAS. However, although there was a statistically significant further decline in depressive symptoms as measured by the MADRAS when the eight participants were included in the analysis [F(1, 7) = 7.692; p = 0.028], the decline on the MADRAS was only of borderline significance when only the seven completers were included [F(1, 6) = 5.250; p = 0.062].
Patients’ Satisfaction
Patient’s scores on the 4-point (0–3) Satisfaction numerical rating scale after the last tDCS session as well as at the follow-up ranged between 2 (satisfied a lot with the results of tDCS treatment) and 3 (fully satisfied). After the last tDCS, six of eight subjects were fully satisfied with the results, and two subjects were satisfied a lot, mean score 2.75, s.d. 0.46. At the 2-week follow-up, seven subjects were fully satisfied and one subject was satisfied a lot, mean score 2.88, s.d. 0.35, indicating that the level of satisfaction with the results of the tDCS treatment did not deteriorate during the post-treatment follow-up period.
Preliminary Findings from Qualitative Interviews
Four themes emerged to describe participants’ experiences with tDCS: (a) a narrative of frustration and helplessness with previous depression and medication treatment, (b) the sensory experience of tDCS, including tingling at site placement and desensitization to tingling or irritation after the first few treatments, (c) altruism, with particular attention to improving depression treatment for other HIV-infected persons, and (d) clearer thinking with reduced perseveration, rigidity of thinking, and drug cravings.
Subjects who did not complete the treatment indicated a high motivation to participate in the entire study but said that unanticipated scheduling conflicts prevented them from doing so. They each suggested that future tDCS treatment protocols be developed to maximize flexibility for participants (i.e., offering options of evening and weekend appointments so that subjects could “make up” a missed session). The subject who received eight sessions of tDCS said she was noting improvement in her mood and clarity in her thinking. The other two non-completers who received two treatment sessions did not perceive any changes in depressive symptoms. The interviews did not reveal any identifiable differences in the demographic or clinical characteristics of subjects who completed the treatment compared with non-completers. All 10 participants reported their willingness to participate in future tDCS clinical trials.
Feasibility of Biomarker-Collection
All study participants agreed to provide samples of blood and saliva for biochemical analysis of immunity biomarkers. At the time of collection, all subjects fully cooperated and followed instruction of study personnel. Data collection of serum and saliva samples for cytokine assays was feasible in this patient population.
Discussion
This was a pilot, open-label study to determine the feasibility of using novel tDCS antidepressant treatment in HIV-infected persons. The study evaluated clinical outcomes, safety, acceptability, and patient’s satisfaction with the treatment, as well as the feasibility of collecting serum and saliva cytokine biomarkers in a 2-week tDCS treatment protocol.
To our knowledge, this is the first study to provide evidence about the feasibility of the tDCS treatment protocol in an HIV population, and the first tDCS study applying a mixed methods approach.
In accordance with the previous tDCS studies in the general population (Fregni et al., 2006; Boggio et al., 2008a; Rigonatti et al., 2008; Kalu et al., 2012), the results of our study showed a decrease of depressive symptoms after tDCS treatment. Although our study was not sham-controlled, the relief of depressive symptoms was well beyond effects attributable solely to placebo response observed in previous studies (Fregni et al., 2006; Boggio et al., 2008a; Rigonatti et al., 2008; Kalu et al., 2012). Further, it is of great clinical interest that the improvement of depressive symptoms after tDCS in our study did not deteriorate in the 2-week follow-up period, which provides a rationale for future studies of durability of tDCS effects.
Further, results of our study contributed to evidence on the safety of tDCS treatment, as none of our subjects experienced any SAE; the few non-SAEs that occurred in our study were minor and transient. Monitoring and evaluation of blood pressure and heart rate before and after each tDCS session showed occasional bi-directional changes in these parameters. The changes were not specific to the study participants with a history and/or present status of hypertension, and a decrease of the parameters was observed more often than an increase. Of note, numerous factors could contribute to the observed changes, including anticipation stress prior the first tDCS stimulation, physical activity immediately prior the study visit, or level of relaxation during the 20-min “quiet time” when receiving tDCS stimulation. The decreasing effect of tDCS on blood pressure has been previously noted and Cogiamanian et al. (2010) discussed the potential use of tDCS in the treatment of hypertension. However, our finding of bi-directional fluctuation suggests caution and monitoring of blood pressure and heart rate during tDCS stimulation, and further studies of tDCS effects.
A gratifying finding in our study was the high adherence of subjects to the study protocol. It could be partially because our study subjects were completers of an NIH-funded study of HIV patients (R01 AI070005, ACT 2, PI M.V. Gwadz; Gwadz et al., 2011) that educated patients on relevant issues concerning research participation to facilitate minorities’ access to participation in suitable research trials. The high adherence in our study not only supports feasibility of the 2-week tDCS treatment protocol and its use in a future RCT, but also contributes to evidence of validity of the ACT 2 educational intervention.
The findings from the qualitative evaluation of the semi-structured interviews at the end of the study revealed high satisfaction with the study and willingness of all subjects to participate in future tDCS studies. The findings were consistent with previously reported (Rosedale et al., 2009) patients’ experiences with the repetitive transcranial magnetic stimulation (rTMS) treatment; participants described intense frustration and helplessness with previous depression and medication treatment, arguing for novel treatment approaches (Rosedale et al., 2009). The theme of electrode placement, tingling, and desensitization to tingling or irritation after the first few treatments has been previously described in the rTMS, but not in the tDCS literature (Anderson et al., 2006). Altruism has not been previously described as a motivating factor for participation in brain stimulation studies and may have been a particular feature of the ACT 2 group participants or a particular motivating factor for persons infected with HIV.
Clearer thinking with reduced perseveration, reduced rigidity of thinking, and reduced drug cravings have been previously described in the tDCS literature and suggest that tDCS may enhance acute attention and working memory in people with depression (Loo, 2012). Notably, attention-enhancement as well as reduced cravings for specific foods and alcohol has also been observed in patients treated with tDCS (Boggio et al., 2008b; Fregni et al., 2008; Kang et al., 2009). This may present enormous clinical opportunity for the HIV patients who present with high comorbidity of substance abuse.
Our results also support feasibility of saliva and blood sample collection for the immunity-biomarker analysis and indicate an applicability of this procedure in future RCT tDCS protocols involving HIV-infected subjects.
The major limitations of the study and its findings are (i) the small sample size that limits generalizability of the results, (ii) the open-label design of the study, (iii) the trained clinical raters were not blinded to the study protocol, (iv) the study have not used parallel versions of MMSE at the post-treatment re-testing, and therefore an order effect might have contributed to the MMSE results. As the study was not sham-controlled, a future RCT is warranted before conclusions on effectiveness of tDCS antidepressant treatment in an HIV population can be drawn.
Conclusion
The study demonstrated feasibility of the 2-week tDCS treatment protocol in HIV-infected patients, as well as the feasibility of study enrollment and satisfactory retention of the subjects which supports future tDCS studies in this patient population.
Conflict of Interest Statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
(1) Department of Pain medicine and Palliative Care, Beth Israel Medical Center, New York, NY, USA. (2) Muriel and Virginia Pless Center for Nursing Research, New York University, New York, NY, USA.
References
Anderson, B., Mishory, A., Nahas, Z., Borckardt, J. J., Yamanaka, K., Rastogi, K., and George, M. S. (2006). Tolerability and safety of high daily doses of repetitive transcranial magnetic stimulation in healthy young men. J. ECT 22, 49–53.
Antal, A., Paulus, W., and Nitsche, M. A. (2010). Principle, and mechanisms of transcranial direct current stimulation (tDCS). J. Pain Manag. 2, 249–259.
Boggio, P. S., Rigonatti, S. P., Ribeiro, R. B., Myczkowski, M. L., Nitsche, M. A., Pascual-Leone, A., and Fregni, F. (2008a). A randomized, double-blind clinical trial on the efficacy of cortical direct current stimulation for the treatment of major depression. Int. J. Neuropsychopharmacol. 11, 249–254.
Boggio, P., Sultani, N., Fecteau, S., Merabet, L., Mecca, T., Pascual-Leone, A., Basaglia, A., and Fregni, F. (2008b). Prefrontal cortex modulation using transcranial DC stimulation reduces alcohol craving: a double-blind, sham-controlled study. Drug Alcohol Depend. 92, 55–60.
Chander, G., Himelhoch, S., and Moore, R. (2006). Substance abuse and psychiatric disorders in HIV-positive patients: epidemiology and impact on antiretroviral therapy. Drugs 66, 769–789.
Cogiamanian, F., Brunoni, A. R., Boggio, P. S., Fregni, F., Ciocca, M., and Priori, A. (2010). Non-invasive brain stimulation for the management of arterial hypertension. Med. Hypotheses 74, 332–336.
Davidson, J. (1986). The Montgomery-Asberg Depression Scale: reliability and validity. Acta Psychiatr. Scand. 73, 544–548.
Folstein, M. F., Folstein, S. E., and McHugh, P. R. (1975). Mini-mental state: a practical method for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 12, 189–198.
Fregni, F., Boggio, P. S., Nitsche, M. A., Marcolin, M. A., Rigonatti, S. P., and Pascual-Leone, A. (2006). Treatment of major depression with transcranial direct current stimulation. Letter to the Editor. Bipolar Disord. 8, 203–205.
Fregni, F., Orsati, F., Pedrosa, W., Fecteau, S., Tome, F. A., Nitsche, M. A., Mecca, T., Macedo, E. C., Pascual-Leone, A., and Boggio, P. S. (2008). Transcranial direct current stimulation of the prefrontal cortex modulates the desire for specific foods. Appetite 51, 34–41.
Gartside, I. B. (1968). Mechanisms of sustained increases of firing rate of neurones in the rat cerebral cortex after polarization: role of protein synthesis. Nature 220, 383–384.
Gaynes, B. N., Rush, A. J., Trivedi, M. H., Wisniewski, S. R., Spencer, D., and Fava, M. (2008). The STAR*D study: treating depression in the real world. Cleve. Clin. J. Med. 75, 57–66.
Giorgi, A. (1985). Phenomenology and Psychological Research. Philadelphia, PA: Duquesne University Press.
Gwadz, M., Leonard, N., Cleland, C., Riedel, M., Banfield, A., and Mildvan, D. (2011). The effect of peer-driven intervention on rates of screening for AIDS clinical trials among African Americans and Hispanics. Am. J. Public Health 101, 1096–1102.
Hartzell, J. D., Janke, I. E., and Weintrob, A. C. (2008). Impact of depression on HIV outcomes in the HAART era. J. Antimicrob. Chemother. 62, 246–255.
Hattori, Y., Moriwaki, A., and Hori, Y. (1990). Biphasic effects of polarizing current on adenosine-sensitive generation of cyclic AMP in rat cerebral cortex. Neurosci. Lett. 116, 320–324.
Kalu, U. G., Sexton, C. E., Loo, C. K., and Ebmeier, K. P. (2012). Transcranial direct current stimulation in the treatment of major depression: a meta-analysis. Psychol. Med. 12, 1–10.
Kang, E., Baek, M., Kim, S., and Paik, N. (2009). Non-invasive cortical stimulation improves post-stroke attention decline. Restor. Neurol. Neurosci. 27, 645–650.
Knotkova, H., Homel, P., and Cruciani, R. A. (2009). Cathodal tDCS over the somatosensory cortex relieved chronic neuropathic pain in a patient with complex regional pain syndrome (CRPS/RSD). Case report. J. Pain Manag. 2, 365–368.
Liebetanz, D., Nitsche, M., Tergau, F., and Paulus, W. (2002). Pharmacological approach to the mechanisms of transcranial DC-stimulation-induced after-effects of human motor cortex excitability. Brain 125, 2238–2247.
Loo, C. K. (2012). Transcranial direct current stimulation for depression: 3-week, randomised, sham-controlled trial. Br. J. Psychiatry 200, 52–59.
Lyketsos, C. G. (1995). Psychiatric issues and emergencies in HIV infection. Emerg. Med. Clin. North Am. 13, 163–177.
McHorney, C. A., Kosinski, M., and Ware, A. E. Jr. (1994). Comparisons of the costs and quality of norms for the SF-36 health survey collected by mail versus telephone interview: results from a national survey. Med. Care 32, 551–567.
Murphy, D. N., Boggio, P. S., and Fregni, F. (2009). Transcranial direct current stimulation as a therapeutic tool for the treatment of major depression: insights from past, and recent clinical studies. Curr. Opin. Psychiatry 22, 306–311.
Nitsche, M. A., Boggio, P. S., Fregni, F., and Pascual-Leone, A. (2009). Treatment of depression with transcranial direct current stimulation (tDCS): a review. Exp. Neurol. 219, 14–19.
Nitsche, M. A., Liebetanz, D., Schlitterlau, A., Henschke, U., Fricke, K., Frommann, K., Lang, N., Henning, S., Paulus, W., and Tergau, F. (2004). GABAergic modulation of DC stimulation-induced motor cortex excitability shifts in humans. Eur. J. Neurosci. 19, 2720–2726.
Nitsche, M. A., and Paulus, W. (2010). Excitability changes induced in the human motor cortex by weak transcranial direct current stimulation. J. Physiol. (Lond.) 527, 633–639.
Nitsche, M. A., Seeber, A., Frommann, K., Klein, C. C., Rochford, C., Nitsche, M. S., Fricke, K., Liebetanz, D., Lang, N., Antal, A., Paulus, W., and Tergau, F. (2005). Modulating parameters of excitability during, and after transcranial direct current stimulation of the human motor cortex. J. Physiol. (Lond.) 568, 291–303.
Rigonatti, S., Boggio, P., Myczkowski, M., Otta, E., Fiquer, J., Ribeiro, R., Nitsche, M., Pascual-Leone, A., and Fregni, F. (2008). Transcranial direct stimulation, and fluoxetine for the treatment of depression. Eur. Psychiatry 23, 74–76.
Rosedale, M., Lisanby, S. H., and Malaspina, D. (2009). The structure of the lived experience for persons having undergone rTMS for depression treatment. J. Am. Psychiatr. Nurses Assoc. 15, 333–337.
Stober, D., Schwartz, J., McDaniel, S., and Robin, F. A. (1997). Depression and HIV disease: prevalence, correlates and treatment. Psychiatr. Ann. 27, 372–377.
Sundaram, A., Stock, V., Cruciani, R. A., and Knotkova, H. (2009). Safety of transcranial direct current stimulation (tDCS) in protocols involving human subjects. J. Pain Manag. 2, 285–293.
Williams, B. (1998). A structured interview guide to the Hamilton depression rating scale. Arch. Gen. Psychiatry 45, 742–747.
Keywords: transcranial direct current stimulation, HIV, major depressive disorder, neuromodulation
Citation: Knotkova H, Rosedale M, Strauss SM, Horne J, Soto E, Cruciani RA, Malaspina D and Malamud D (2012) Using transcranial direct current stimulation to treat depression in HIV-infected persons: the outcomes of a feasibility study. Front. Psychiatry 3:59. doi: 10.3389/fpsyt.2012.00059
Received: 21 March 2012; Accepted: 25 May 2012; Published online: 18 June 2012.
Edited by:
Paulo Sérgio Boggio, Mackenzie Presbyterian University, BrazilCopyright: © 2012 Knotkova, Rosedale, Strauss, Horne, Soto, Cruciani, Malaspina and Malamud. This is an open-access article distributed under the terms of the Creative Commons Attribution Non Commercial License, which permits non-commercial use, distribution, and reproduction in other forums, provided the original authors and source are credited.
*Correspondence: Helena Knotkova, Research Division, Department of Pain Medicine and Palliative Care, Institute for Non-Invasive Brain Stimulation, Beth Israel Medical Center, 120 East 16th Street, 12th floor, New York, NY, USA. e-mail: hknotkov@chpnet.org
†Helena Knotkova and Mary Rosedale have contributed equally to this work.