
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Pediatr. , 01 April 2025
Sec. Pediatric Orthopedics
Volume 13 - 2025 | https://doi.org/10.3389/fped.2025.1563536
Objectives: While both short- and long-leg spica casts present viable options after closed reduction (CR) in developmental dysplasia of the hip (DDH), comprehensive comparative studies are needed to guide clinical practices. This multi-center retrospective study aimed to evaluate their effectiveness in treating DDH and identify predictors of treatment failure.
Methods: This retrospective study analyzed 146 DDH patients (0–18 months) treated with closed reduction and spica casts (70 short-leg vs. 76 long-leg) at two tertiary centers (2005–2024). Incident-free survival (time from casting to failure: re-dislocation, imaging-confirmed reduction loss, or surgical conversion) was analyzed via Kaplan–Meier/Log-rank tests. A multivariable Cox model evaluated eight variables: cast type, age (>6 vs. ≤6 months), sex, laterality (bilateral/unilateral), IHDI grade (IV/III), birth presentation, delivery mode, and family history, allowing quantification of independent predictors associated with treatment failure risks.
Results: The analysis of 146 DDH cases (70 short-leg vs. 76 long-leg casts) revealed significant outcome differences between cast types. Patients receiving long-leg spica casts demonstrated substantially higher 6-month incident-free survival rates (84% vs. 68%, Log-rank p < 0.05), with multivariable Cox regression confirming long-leg casting as an independent protective factor (HR = 0.45, 95% CI 0.32–0.64, p < 0.001). The analysis identified three significant risk predictors: older age (>6 months) increased failure risk by 89% (HR = 1.89, 95% CI 1.02–3.51), bilateral involvement elevated risk by 78% (HR = 1.78, 95% CI 1.25–2.54), and IHDI IV dysplasia doubled failure likelihood (HR = 2.15, 95% CI 1.45–3.18). Notably, cephalic presentation showed a protective trend (HR = 0.67, 95% CI 0.48–0.93), while delivery mode and family history did not reach statistical significance.
Conclusions: Long-leg spica casting shows superior biomechanical stability in DDH management post-CR, particularly for high-risk patients. These findings support its preferential use in patients with bilateral involvement, advanced dysplasia, or older age (>6 months).
Developmental dysplasia of the hip (DDH) is a significant orthopedic condition in pediatrics, characterized by a spectrum from mild dysplasia to complete dislocation of the hip joint (1–3). Early intervention is crucial to prevent long-term disabilities (4, 5). When nonoperative methods such as harnesses fail, closed reduction (CR) is the standard treatment (6, 7). Post-CR immobilization is pivotal for maintaining anatomic hip positioning and fostering normal joint development (8, 9). While long-leg spica casts (extending below the knee) remain traditional for stabilization, their biomechanical advantages are counterbalanced by mobility and hygiene challenges (10, 11). Short-leg spica casts (ending above the knee) have gained traction as a patient-friendly alternative, yet conflicting evidence exists regarding their efficacy compared to long-leg casts (12). Prior studies, limited by small cohorts, report comparable short-term outcomes, but critical knowledge gaps persist regarding long-term stability, failure risks, and predictors such as age (>6 months), bilateral involvement, or severe dysplasia (IHDI grade IV).
This multi-center study evaluates 377 DDH patients (2005–2024) to compare post-CR outcomes between short- and long-leg spica casts, while identifying independent protective factors (e.g., cast type) and risk predictors (e.g., age, laterality, dysplasia severity). By addressing these gaps, we aim to refine evidence-based, patient-centered immobilization strategies for high-risk subgroups. This study hypothesizes that long-leg spica casts provide superior biomechanical stability compared to short-leg casts, resulting in higher incident-free survival and lower complication rates post-CR for DDH.
This multi-center retrospective cohort study analyzed data from Fujian Medical University's Affiliated Children's Hospital and the First Affiliated Hospital of Sun Yat-sen University (January 2005–December 2024), focusing on pediatric patients with DDH treated with CR followed by short-leg (above-knee) or long-leg (below-knee) spica casts. Conducted in compliance with ethical standards and institutional review board approval, this research involved an extensive review of electronic medical records. Inclusion criteria encompassed consecutive patients aged 0–18 months with diagnosis of DDH, treated with CR and spica cast immobilization, having complete medical records.
Radiographic severity was classified using the Tönnis system and International Hip Dysplasia Institute (IHDI) criteria, particularly for cases with an absent ossific nucleus. Patients classified as Tönnis grades I–II or IHDI grades I–II were excluded, as these mild-to-moderate dysplasias typically resolve with bracing alone and do not necessitate CR. Additional exclusions: age >18 months, prior hip surgery/DDH treatment, congenital anomalies affecting the hip, or incomplete medical or follow-up records.
Demographics (age, sex), birth history (presentation, delivery mode), family DDH history, hip laterality (unilateral/bilateral), and cast type (short- vs. long-leg) were extracted. Two blinded pediatric orthopedic surgeons independently evaluated imaging studies, with discrepancies resolved by consensus. Eight clinically relevant variables were analyzed for failure risk: cast type, age (>6 vs. ≤6 months), sex, laterality, Tönnis grade (IV vs. III), birth presentation (breech/cephalic), delivery mode (cesarean/vaginal), and family DDH history.
The primary outcomes focused on incident-free survival and risk predictors. Incident-free survival was defined as the time interval from cast application to the first treatment failure event, including re-dislocation, imaging-confirmed reduction loss, or conversion to open surgery. This outcome was analyzed using Kaplan–Meier survival curves with Log-rank testing for comparative assessment. Risk predictors were evaluated through multivariable Cox proportional hazards regression models to quantify hazard ratios (HRs) for treatment failure while adjusting for covariates.
Secondary outcomes addressed clinical and patient-centered metrics. Acute reduction success was confirmed intraoperatively via arthrography to verify concentric reduction and postoperatively with computed tomography (CT) within 24 h to assess femoral head alignment and acetabular coverage (13, 14). Long-term stability at 12 months post-CR was evaluated using pelvic radiographs, applying thresholds such as an acetabular index ≤25° (normal: ≤20°–25° in children <2 years) (15–17) and Reimer's migration index <20% to confirm stable femoral head coverage (18–20). Complications included residual dysplasia (acetabular index >30°) (21) and avascular necrosis [AVN, classified using the Kalamchi-MacEwen system grades I–IV (22): Grade I (temporary growth disturbance), Grade II (lateral physeal damage), Grade III (central physeal collapse), and Grade IV (total femoral head involvement)]. Reoperations were documented for cases requiring secondary procedures due to treatment failure or complications. Patient-centric outcomes incorporated caregiver-reported Likert-scale assessments of mobility limitations, hygiene challenges, and comfort levels (18, 21, 22).
Descriptive statistics summarized demographic and clinical variables. Group comparisons (short- vs. long-leg casts) employed chi-square tests for categorical variables and t-tests or Mann–Whitney U tests for continuous variables, selected based on normality (assessed via Shapiro–Wilk tests). Kaplan–Meier curves with Log-rank tests compared incident-free survival between cast types. Multivariable Cox regression (forward stepwise selection, α = 0.05) identified independent predictors, with results reported as HRs and 95% confidence intervals (CIs). Proportional hazards assumptions were verified via Schoenfeld residuals. Significance was set at p < 0.05. Analyses were performed using R v.4.4.2 (R Foundation).
The study analyzed 146 pediatric DDH patients treated with CR followed by spica casting, including 70 in the short-leg cast group and 76 in the long-leg cast group (Figure 1). Baseline characteristics were comparable between cohorts (Table 1), with no significant differences in age distribution (≤6 months: 31% short-leg vs. 26% long-leg, p = 0.497), sex (54% short-leg vs. 53% long-leg, p = 0.842), laterality (bilateral: 51% short-leg vs. 46% long-leg, p = 0.518), or IHDI grade IV severity (20% short-leg vs. 24% long-leg, p = 0.592). Birth presentation, delivery mode, and family history showed no significant imbalances (all p > 0.05).
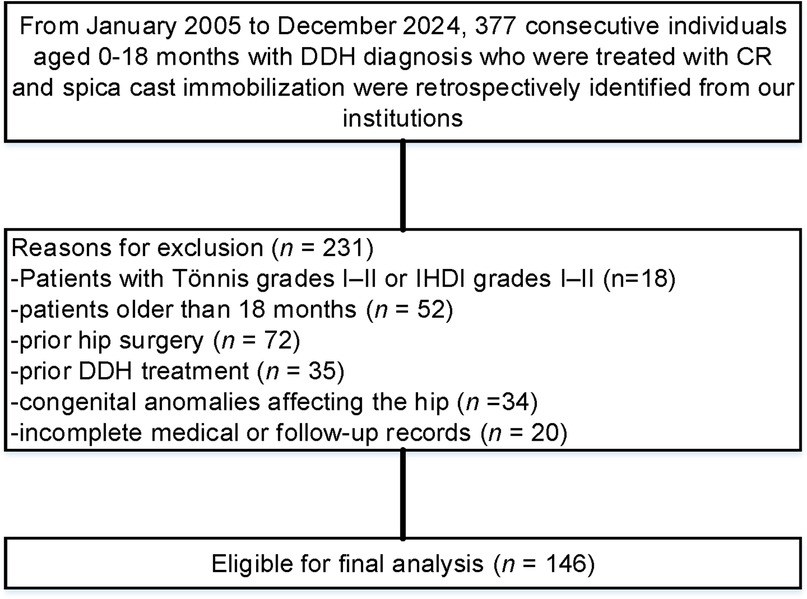

Figure 1. Flow diagram demonstrating the methods used to identify objects to evaluate the effectiveness of short- and long-leg spica casts in treating DDH.
Long-leg spica casts demonstrated superior clinical outcomes. Kaplan–Meier analysis revealed significantly higher 6-month incident-free survival rates in the long-leg group (84% vs. 68%, Log-rank p < 0.05) (Figure 2). Multivariable Cox regression identified long-leg casting as an independent protective factor against treatment failure (HR = 0.45, 95% CI 0.32–0.64, p < 0.001). Conversely, age >6 months (HR = 1.89, 95% CI 1.02–3.51, p = 0.001), bilateral involvement (HR = 1.78, 95% CI 1.25–2.54, p = 0.001), and IHDI grade IV dysplasia (HR = 2.15, 95% CI 1.45–3.18, p < 0.001) were significant risk predictors. Cephalic birth presentation showed a protective trend (HR = 0.67, 95% CI 0.48–0.93, p = 0.018), while delivery mode and family history lacked statistical significance (Table 2).
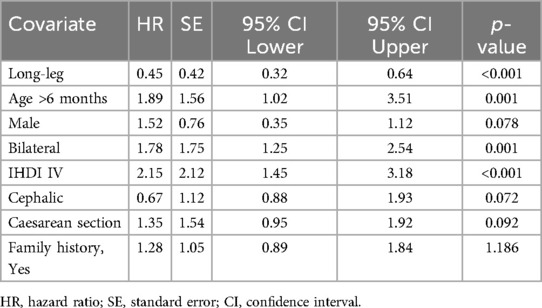
Table 2. Cox regression analysis to assess the correlation between cast type (short vs. long spica) and outcomes.
The long-leg spica group demonstrated superior acute success rates [89% (68/76)] compared to the short-leg spica group [71% (50/70); p = 0.006]. Furthermore, the incidence of residual deformity was significantly lower in the long-leg spica cohort [15% (12/76)] than in the short-leg spica group [34% (24/70); p = 0.01]. Notably, avascular necrosis (AVN) occurred less frequently in the long-leg spica group [9% (7/76)] compared to the short-leg spica cohort [23% (16/70); p = 0.024] (Table 3). These results underscore the clinical advantages of long-leg spica fixation in reducing complications and improving acute treatment success for the studied population.
The findings of this multicenter retrospective analysis provide compelling evidence for the biomechanical superiority of long-leg spica casts in maintaining hip stability following CR for DDH. Our results demonstrate that long-leg spica casting significantly outperforms short-leg casting in both acute success rates and long-term incident-free survival. The Kaplan–Meier analysis revealed a marked disparity in 6-month incident-free survival (84% vs. 68%, Log-rank p < 0.05), corroborated by multivariable Cox regression identifying long-leg casts as an independent protective factor (HR = 0.45, p < 0.001). This aligns with biomechanical principles positing that immobilization extending below the knee enhances femoral head containment by limiting rotational and translational forces across the hip joint, thereby reducing risks of reduction loss (23, 24). Early studies advocating short-leg casts emphasized patient comfort and mobility (25), yet our data challenge the assumption of equivalence in stabilization efficacy. The 19% absolute risk reduction in residual deformity (15% vs. 34%, p = 0.01) and 14% reduction in avascular necrosis (AVN, 9% vs. 23%, p = 0.024) further underscore the clinical relevance of extended immobilization.
Contrary to previous reports (26, 27) suggesting comparable AVN risks between cast types, our cohort revealed significantly lower AVN incidence in the long-leg group. This discrepancy may stem from differences in preoperative protocols, such as traction duration or reduction techniques, which were standardized in our study. Recent studies (12, 28) reported no association between cast length and AVN, their smaller sample size and heterogeneous cohorts may have obscured true differences. Our findings suggest that biomechanical stability conferred by long-leg casts indirectly mitigates ischemic risks by minimizing microtrauma from residual instability, a hypothesis supported by animal models demonstrating vascular compromise during repetitive joint loading (29, 30).
The argument for short-leg casts as a patient-friendly alternative must be weighed against their inferior clinical outcomes. Although researchers reported improved hygiene and mobility with short-leg casts in prior studies (14), these benefits did not translate to superior functional outcomes in our cohort. Instead, the high complication rate and need for surgical conversion in the short-leg group highlight the critical trade-off between convenience and efficacy. Notably, the protective trend associated with cephalic presentation (HR = 0.67, p = 0.072) and the elevated risks linked to bilateral involvement (HR = 1.78) and IHDI grade IV dysplasia (HR = 2.15) further emphasize the need for robust immobilization in high-risk subgroups.
Several limitations merit detailed discussion. First, the retrospective design of most included studies introduces selection bias and confounds causal inference. Second, heterogeneous patient cohorts, variable treatment protocols, and inconsistent outcome measures complicate cross-study comparisons. Finally, the predominance of small sample sizes and limited long-term follow-up restricts the generalizability of findings. Future prospective multicenter studies with standardized endpoints—including patient-reported outcomes and advanced imaging metrics—are essential to refine immobilization protocols and optimize individualized care.
In light of the significantly higher 6-month incident-free survival (84% vs. 68%) and reduced complications observed with long-leg spica casts, we recommend against the use of short-leg casts for DDH patients aged 0–18 months requiring post-CR immobilization. While short-leg casts may offer logistical advantages, their association with higher residual deformity, AVN, and failure rates necessitates prioritizing biomechanical stability over transient comfort. Long-leg spica casting should be the standard of care, particularly for patients with bilateral involvement, severe dysplasia (IHDI IV), or age >6 months, where failure risks are amplified. Future studies should explore hybrid immobilization strategies that balance stability with patient-centered outcomes, ensuring adherence without compromising therapeutic efficacy.
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding authors.
All methods were conducted in accordance with relevant institutional and national guidelines, including the 1964 Helsinki Declaration. The study received approval from the Medical Ethics Committee of Fujian Medical University’s Affiliated Children’s Hospital (No. 2011-342). Informed consent was waived due to the retrospective design and identified data.
ZZ: Data curation, Formal analysis, Methodology, Project administration, Supervision, Validation, Writing – original draft. WY: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. ZC: Writing – original draft, Writing – review & editing. JinrL: Data curation, Formal analysis, Funding acquisition, Writing – original draft. JinlL: Conceptualization, Investigation, Software, Writing – original draft. CH: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing.
The author(s) declare that financial support was received for the research and/or publication of this article. This research received three funding grants (Joint Funds for the Innovation of Science and Technology, Fujian Province, No. 2023Y9064; Natural Science Foundation of Fujian Province, No. 2024J01532; Fujian Medical University Scientific Research and Development Fund Project, No. 2023QH1457).
The authors thank all the doctors and patients who provided data to support this study.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The author(s) declare that no Generative AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fped.2025.1563536/full#supplementary-material
1. Cosgrove AP, Maizen C. Detection and treatment of developmental dysplasia of the hip in infants: updates and recommendations. Curr Opin Pediatr. (2025) 37(1):88–93. doi: 10.1097/MOP.0000000000001420
2. Gahleitner M, Pisecky L, Gotterbarm T, Högler W, Luger M, Klotz MC. Long-term results of developmental hip dysplasia under therapy with pavlik harness. J Pediatr Orthop. (2024) 44(3):135–40. doi: 10.1097/BPO.0000000000002575
3. Cooke SJ, Rees R, Edwards DL, Kiely NT, Evans GA. Ossification of the femoral head at closed reduction for developmental dysplasia of the hip and its influence on the long-term outcome. J Pediatr Orthop Part B. (2010) 19(1):22–6. doi: 10.1097/BPB.0b013e32832fc8ca
4. Saeed A, Bradley CS, Verma Y, Kelley SP. Resolving residual acetabular dysplasia following successful brace treatment for developmental dysplasia of the hip in infants. Bone Jt J. (2024) 106-b(7):744–50. doi: 10.1302/0301-620X.106B7.BJJ-2023-1169.R1
5. Wang JQ, Li TY, Yao YY, Lu CQ, Wang YZ. The role of the cartilaginous to osseous acetabular angle ratio in children with developmental dysplasia of the hip. Front Pediatr. (2024) 12:1347556. doi: 10.3389/fped.2024.1347556
6. Dezateux C, Rosendahl K. Developmental dysplasia of the hip. Lancet. (2007) 369(9572):1541–52. doi: 10.1016/S0140-6736(07)60710-7
7. Huang X, Cheng X, Gao S, Liu Y, Su Y, Feng C. Prediction of the labrum shape in patients with developmental dysplasia of the hip based on pelvic radiography. J Pediatr Orthop. (2024) 44(6):e490–e5. doi: 10.1097/BPO.0000000000002676
8. Caruso G, Gambuti E, Spadoni E, Filipponi S, Saracco A, Artioli F, et al. Incidence of risk factors in developmental dysplasia of the hip: a retrospective study on 18,954 cases. Hip Int. (2024) 34(5):628–32. doi: 10.1177/11207000241248416
9. Chang CH, Hung CL, Lee WC, Kao HK, Wang SM, Kuo KN. Reoperations as an outcome indicator for developmental dysplasia of the hip treated at walking age. J Bone Jt Surg Am. (2025) 107(5):469–75. doi: 10.2106/JBJS.24.00486
10. Yong B, Li Y, Li J, Andreacchio A, Pavone V, Pereria B, et al. Post-operative radiograph assessment of children undergoing closed reduction and spica cast immobilization for developmental dysplasia of the hip: does experience matter? Int Orthop. (2018) 42(11):2725–31. doi: 10.1007/s00264-018-4038-0
11. Chen H, Wang XX, Chen Z, Ge Y. The efficacy of gradual reduction using two-stage traction for developmental dysplasia of the hip in Southern China. Front Pediatr. (2024) 12:1335490. doi: 10.3389/fped.2024.1335490
12. Gangaram-Panday SSG, de Vos-Jakobs S, Reijman M. The effect of traction before closed reduction in patients with developmental dysplasia of the hip. Children-Basel. (2022) 9(9):1325. doi: 10.3390/children9091325
13. Tennant SJ, Eastwood DM, Calder P, Hashemi-Nejad A, Catterall A. A protocol for the use of closed reduction in children with developmental dysplasia of the hip incorporating open psoas and adductor releases and a short-leg cast mid-term outcomes in 113 hips. Bone Jt J. (2016) 98B(11):1548–53. doi: 10.1302/0301-620X.981311.36606
14. Yasin MS, Alisi MS, Hammad YS, Samarah OQ, Abu Hassan FO. Short versus long-leg hip spica after closed reduction in developmental dysplasia of the hip: a retrospective comparative study. Orthop Res Rev. (2022) 14:71–6. doi: 10.2147/ORR.S353279
15. Tönnis D. Normal values of the hip joint for the evaluation of x-rays in children and adults. Clin Orthop Relat Res. (1976) 119:39–47.
16. Li YQ, Guo YM, Li M, Zhou QH, Liu YZ, Chen WD, et al. Acetabular index is the best predictor of late residual acetabular dysplasia after closed reduction in developmental dysplasia of the hip. Int Orthop. (2018) 42(3):631–40. doi: 10.1007/s00264-017-3726-5
17. Li LY, Zhang LJ, Li QW, Zhao Q, Jia JY, Huang T. Development of the osseous and cartilaginous acetabular index in normal children and those with developmental dysplasia of the hip a cross-sectional study using MRI. J Bone Jt Surg Br Vol. (2012) 94B(12):1625–31. doi: 10.1302/0301-620X.94B12.29958
18. Reimers J. The stability of the hip in children. A radiological study of the results of muscle surgery in cerebral palsy. Acta Orthop Scand Suppl. (1980) 184:1–100. doi: 10.3109/ort.1980.51.suppl-184.01
19. Ma SY, Zhou WZ, Li LY, Wang EB, Zhang LJ, Li QW. Retrospective comparison of outcomes between closed and open reduction for developmental dysplasia of the hip in children aged 6–24 months. Indian J Orthop. (2022) 56(9):1640–6. doi: 10.1007/s43465-022-00690-9
20. Ertürk C, Altay MA, Isikan UE. A radiological comparison of Salter and Pemberton osteotomies to improve acetabular deformations in developmental dysplasia of the hip. J Pediatr Orthop Part B. (2013) 22(6):527–32. doi: 10.1097/BPB.0b013e32836337cd
21. Alexiev VA, Harcke HT, Kumar SJ. Residual dysplasia after successful Pavlik harness treatment: early ultrasound predictors. J Pediatr Orthop. (2006) 26(1):16–23. doi: 10.1097/01.bpo.0000187995.02140.c7
22. Kalamchi A, MacEwen GD. Avascular necrosis following treatment of congenital dislocation of the hip. JBJS. (1980) 62(6):876–88. doi: 10.2106/00004623-198062060-00002
23. Sawamura K, Kitoh H, Matsushita M, Mishima K, Kamiya Y, Imagama S. Quality of life in adult patients with developmental dysplasia of the hip who were treated for hip dislocation during childhood. J Pediatr Orthop Part B. (2025) 34(1):38–43. doi: 10.1097/BPB.0000000000001173
24. Okuzu Y, Tsukanaka M, Shimozono F, Soen M, Miwa A, Kuroda Y, et al. Clinical outcomes of gradual reduction of late-detected developmental dysplasia of the hip using ultrasound-guided flexion abduction continuous traction: a midterm follow up study. J Pediatr Orthop Part B. (2025) 34(1):51–6. doi: 10.1097/BPB.0000000000001201
25. Li Y, Guo Y, Shen X, Liu H, Mei H, Xu H, et al. Radiographic outcome of children older than twenty-four months with developmental dysplasia of the hip treated by closed reduction and spica cast immobilization in human position: a review of fifty-one hips. Int Orthop. (2019) 43(6):1405–11. doi: 10.1007/s00264-019-04315-z
26. Park K-B, Narendravaidya V, Shin H, Kwak YH. Prereduction traction for the prevention of avascular necrosis before closed reduction for developmental dysplasia of the hip: a meta-analysis. Ther Clin Risk Manag. (2018) 14:1253–60. doi: 10.2147/TCRM.S166531
27. Cai Z, Li L, Zhang L, Ji S, Zhao Q. Dynamic long leg casting fixation for treating 12- to 18-month-old infants with developmental dysplasia of the hip. J Int Med Res. (2017) 45(1):272–81. doi: 10.1177/0300060516675110
28. Tennant SJ, Eastwood DM, Calder P, Hashemi-Nejad A, Catterall A. A protocol for the use of closed reduction in children with developmental dysplasia of the hip incorporating open psoas and adductor releases and a short-leg cast: mid-term outcomes in 113 hips. Bone Jt J. (2016) 98-b(11):1548–53. doi: 10.1302/0301-620X.98B11.36606
29. Greenhill BJ, Hainau B. Ellis RD, El-sayed RM. Acetabular changes in an experimental model of developmental dysplasia of the hip (DDH). J Pediatr Orthop. (1995) 15(6):789–93. doi: 10.1097/01241398-199511000-00012
Keywords: cast, dysplasia, spica, survival, developmental dysplasia of the hip
Citation: Zheng Z, Yu W, Chen Z, Lin J, Lin J and Chen H (2025) Long-leg spica casts demonstrate superior outcomes in developmental dysplasia of the hip: a multi-center retrospective analysis of failure risks and protective factors. Front. Pediatr. 13:1563536. doi: 10.3389/fped.2025.1563536
Received: 20 January 2025; Accepted: 17 March 2025;
Published: 1 April 2025.
Edited by:
Danilo Leonetti, University of Messina, ItalyReviewed by:
Ali Saleh Mahdi Aljanabi, University of Al-Qadisiyah, IraqCopyright: © 2025 Zheng, Yu, Chen, Lin, Lin and Chen. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Weiguang Yu, eXV3ZzNAbWFpbC5zeXN1LmVkdS5jbg==; Hui Chen, ZnpjaDAzMjFAMTYzLmNvbQ==
†These authors have contributed equally to this work
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.