
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
CASE REPORT article
Front. Oncol. , 26 March 2025
Sec. Genitourinary Oncology
Volume 15 - 2025 | https://doi.org/10.3389/fonc.2025.1476988
 Frank Obeng1,2*
Frank Obeng1,2* Aishah Fadila Adamu2
Aishah Fadila Adamu2 Samuel Edudzi Gavor2
Samuel Edudzi Gavor2 Blessings Yao Setsoafia2
Blessings Yao Setsoafia2 Ebenezer Kwame Antwi2
Ebenezer Kwame Antwi2 Nelson Affram1,2
Nelson Affram1,2 Ayamba Mamudu Ali1,2
Ayamba Mamudu Ali1,2Prostate cancer is typically asymptomatic and usually diagnosed through concerted screening programs. However, in settings where there are no existing national prostate cancer screening programs, it may be picked up at the clinics in patients presenting with urinary symptoms, erectile dysfunction, and hematospermia/hematuria. Rare atypical presentations may also occur, delaying diagnosis and management. This case report discusses a 61-year-old male of Black-African descent, whose first presentation to the hospital for a condition ultimately diagnosed as metastatic prostate cancer, was due to lower gastrointestinal bleeding, rectal pain, and psoriasiform dermatitis. The patient’s clinical findings included a moderate-sized (grade 2) nodular prostate on digital rectal examination (DRE), a total serum prostate-specific antigen (PSA) level of >200 ng/mL, low back bone pain, and osteoblastic lesions on lumbosacral spine X-ray. Prostate core biopsy histopathologically confirmed adenocarcinoma with a Gleason score of 4 + 4 = 8. Histopathological examination of the synchronous skin lesions revealed psoriasiform dermatitis. The patient was managed with surgical androgen deprivation therapy (ADT), followed by oral bicalutamide, dermatologist consultation, and blood transfusions. He was also scheduled for further radiotherapy and chemotherapy (to complete the multimodality prostate cancer treatment). This case highlights the importance of considering prostate cancer with atypical presentations and underscores the need for a multidisciplinary approach in managing advanced cases.
Prostate cancer is the second most common cancer among men worldwide (1). Early prostate cancer is typically asymptomatic and screen-detected but may present with urinary symptoms such as frequency, urgency, hesitancy, erectile dysfunction, and hematospermia/hematuria (2, 3). However, atypical presentations can occur, delaying its diagnosis and management (4–6). This situation may be starker in settings such as Ghana, where there is no concerted national prostate cancer screening program. This case report discusses a 61-year-old male of Black-African descent who presented with lower gastrointestinal (GI) bleeding and an associated psoriasiform dermatitis, ultimately diagnosed with metastatic prostate cancer (Figure 1). This case highlights the importance of considering prostate cancer in the differential diagnosis of atypical rectal bleeding.
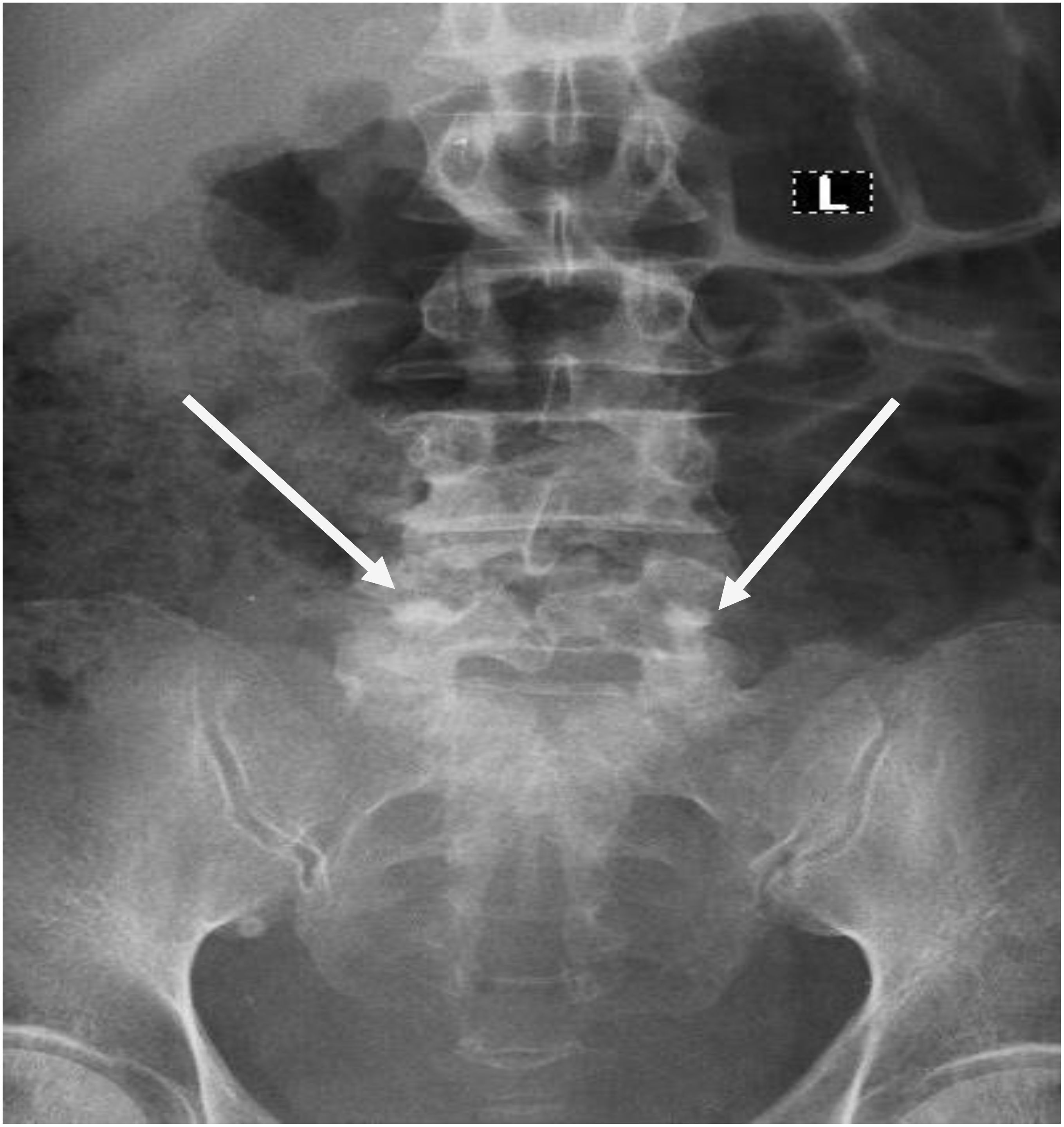
Figure 1. Lumbosacral Spine X-rays; AP-view. Shows suspiscious osteoblastic lesions on L5 (white arrows).
The patient was a 61-year-old Black-African male who presented with a one-month history of recurrent bloody stools and a one-week history of dizziness and easy fatigability. He had been experiencing lower urinary tract symptoms (LUTS), including dysuria, frequency, nocturia, and straining, since March 2019, with a worst International Prostate Symptom Score (IPSS) of 14 and a Quality of Life (QOL) score of 5/6.
In February 2022, he sought treatment at an herbal clinic, where he was managed for benign prostatic hyperplasia (BPH) and was started on tamsulosin and finasteride. Despite this, his symptoms progressed, and in June 2023, he developed acute urinary retention requiring the placement of a urethral catheter, which remained in situ at the time of his first presentation to the teaching hospital (Table 1).
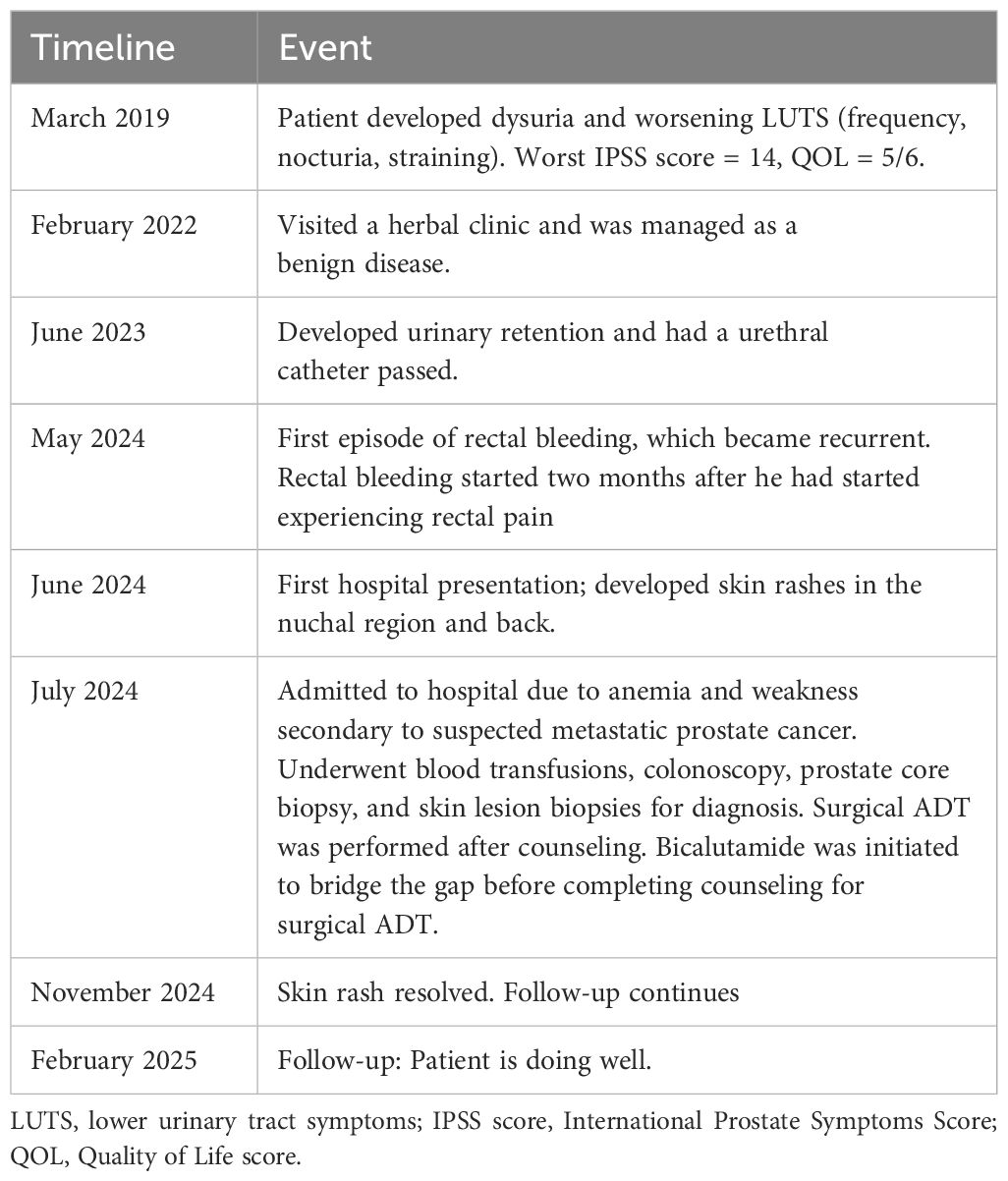
Table 1. Timeline of clinical events in the index patient with atypical presentation of metastatic prostate cancer.
His symptoms worsened in May 2024 when he experienced his first episode of rectal bleeding with associated rectal pain, both of which recurred. By June 2024, he had developed skin rashes in the nuchal region and back (Figures 2, 3). He presented to the teaching hospital in the same month, where he was found to be anemic and weak, leading to his admission in July 2024 (Table 1).

Figure 2. The skin lesions; clinical pictograph. Found to be psoriasiform dermatitis on histopathology of excision biopsies of sampled ones. carcinoma en-cuirasse ruled out.
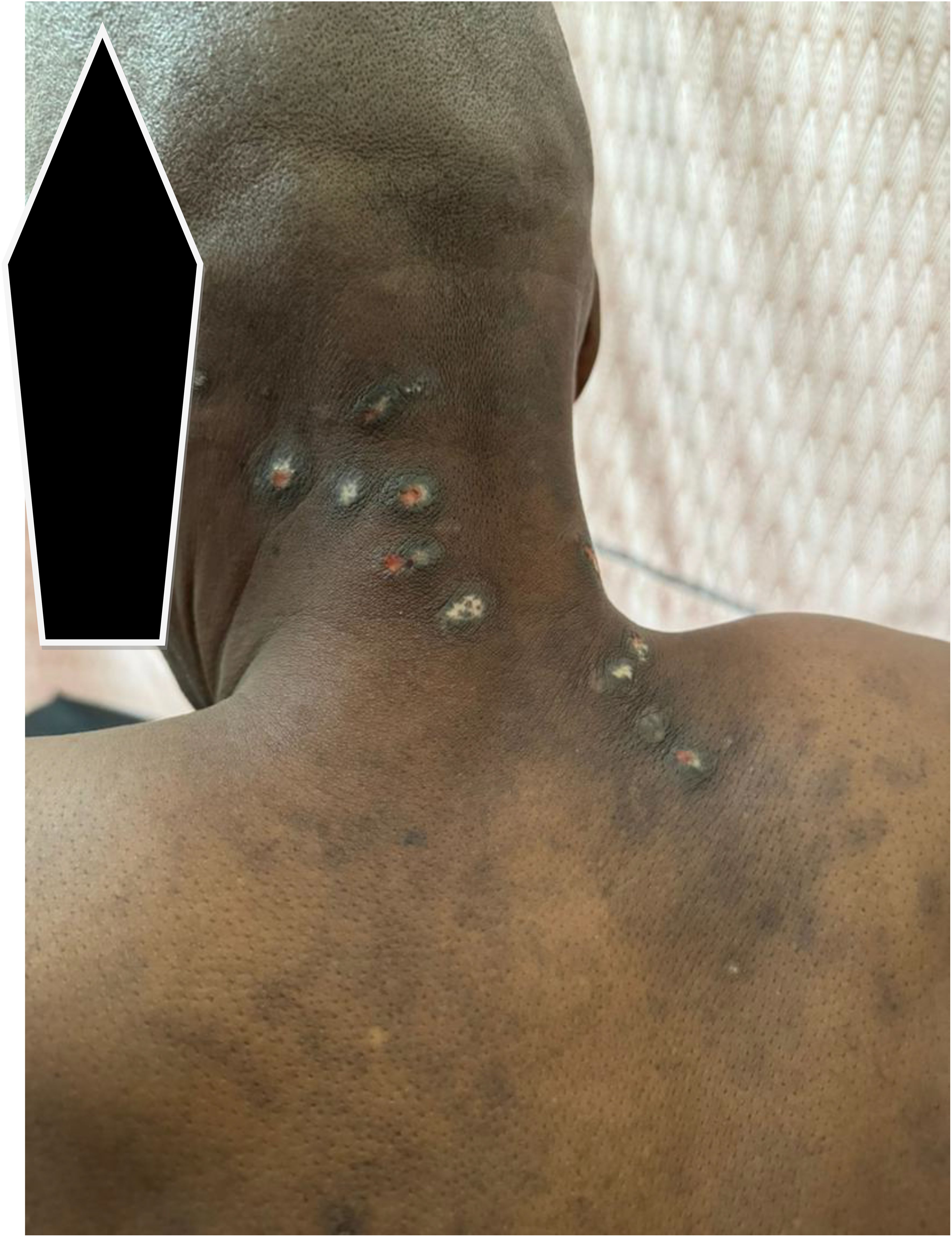
Figure 3. The skin lesions; clinical pictograph of the upper back and nuchal regions. Found to be psoriasiform dermatitis on histopathology of excision biopsies of sampled ones. carcinoma en-cuirasse ruled out.
His medical history included hypertension for which he was taking amlodipine 10 mg once daily. His father had a significant family history of prostate cancer, suggesting a genetic predisposition.
Upon admission, the patient appeared acutely ill, but not in distress. He had a urethral catheter in situ draining amber urine, and his abdomen was flat, with multiple hyperpigmented skin lesions (Figures 2, 3). Digital rectal examination (DRE) revealed a moderately enlarged (grade 2—size), nodular, asymmetrical prostate. His vital signs were stable and he showed no signs of respiratory distress or edema.
Initial laboratory investigations revealed anemia (Hb 8.1 g/dL), leukocytosis (WBC 12.27 × 109/L), elevated creatinine (140.18 µmol/L), and a PSA level >200 ng/mL. Imaging studies included a lumbosacral spine X-ray (Figure 1) showing osteoblastic lesions at L5, an abdominopelvic ultrasound indicating hepatomegaly (but no nodules), right hydroureteronephrosis, and an enlarged prostate with irregular margins. Chest X-rays revealed no cannonball lesions in the lungs. No other tumor markers, apart from PSA, were assayed.
Proctosigmoidoscopy revealed a nodular prostate with eroded mucosa (over approximately 40% of the prostatic-rectal mucosa coverage area). Under the same proctosigmoidoscopy, a conservative six-core prostate biopsy was performed from the areas of the prostate with apparently healthy/intact rectal mucosal coverage. Histopathology confirmed adenocarcinoma of the prostate, Gleason score 4 + 4 = 8 (acinar, not otherwise specified) with 100% core involvement. Additional biopsy of the skin lesions revealed benign psoriasiform dermatitis.
For further metastatic assessment, the patient was prepared for advanced imaging studies, including a technetium bone scan, the gold standard for bone metastasis evaluation (7). However, this was delayed owing to limited availability.
The patient was managed with surgical androgen deprivation therapy (ADT) following a confirmed diagnosis of metastatic prostate cancer. Prior to bilateral orchidectomy, bicalutamide was initiated to provide a temporary androgen blockade. His medications included amlodipine 10 mg once daily (OD) for hypertension, vitamin K 10 mg intramuscularly (IM) daily for five days for coagulopathy correction, and levofloxacin 500 mg OD for infection prophylaxis.
Owing to significant anemia, he received multiple blood transfusions, which led to clinical stabilization.
Given his persistent skin lesions, he was scheduled for dermatological review, and as part of his multimodal treatment plan, he was scheduled to receive external beam radiotherapy and docetaxel-based chemotherapy for advanced metastatic prostate cancer (8).
Following treatment, the patient’s rectal bleeding abated and he demonstrated clinical improvement. His serum total PSA remained >200 ng/mL, while his serum testosterone dropped to 0.2 nmol/L within one-month post-orchidectomy. Hydroureteronephrosis resolved after androgen deprivation therapy (ADT), and his renal function tests were normalized. The catheter was also removed, and he successfully voided per urethra.
He was scheduled for dermatology review due to persistent skin lesions and was scheduled for external beam radiotherapy and docetaxel-based chemotherapy as part of his multimodal treatment for advanced metastatic prostate cancer (8). However, his skin lesions completely disappeared within four months of ADT and dermatological consultation.
Regarding treatment adherence and tolerability, the patient remained compliant with ADT and tolerated bicalutamide and subsequent interventions well with no reported significant adverse effects. No unanticipated complications were noted during the follow-up.
By November 2024, his skin rashes had fully resolved, and at his February 2025 follow-up, he remained clinically stable with no new symptoms.
The patient expressed satisfaction with the treatment received, particularly relief from rectal bleeding, improvement in urinary symptoms, and resolution of skin lesions. He acknowledged the challenges faced during his diagnostic journey, including the delayed presentation and diagnosis, but was grateful for the multidisciplinary approach that ultimately led to his diagnosis and management.
He reported feeling physically stronger and more hopeful about his condition after surgical androgen deprivation therapy and supportive care. He also expressed a strong commitment to adhering to follow-up appointments and ongoing treatment plans, recognizing the importance of regular monitoring and early intervention to optimize health outcomes.
Prostate cancer typically presents with lower urinary tract symptoms (2, 9); however, atypical presentations (6), such as lower GI bleeding, can occur, as seen in the index case. This can be attributed to the invasion of the rectal mucosa by locally advanced tumors, a rare but documented phenomenon (5, 10). The presence of psoriasiform dermatitis in this case adds another layer of complexity, as skin metastasis from prostate cancer, although rare, has been reported previously (11).
The diagnosis of metastatic prostate cancer in the index case was supported by high PSA levels, histopathological findings (which confirmed the cancer), and imaging studies indicating osteoblastic lesions. Management includes hormonal therapy, surgical intervention, and planning for radiotherapy and chemotherapy, reflecting a comprehensive approach for advanced prostate cancer (12).
The presentation of prostate carcinoma with lower gastrointestinal (GI) bleeding is atypical. Prostate cancer is generally associated with urinary symptoms, bone pain, and sometimes systemic manifestations (3) but rarely with rectal bleeding. In this case, SD, a 61-year-old male, presented with rectal bleeding, dizziness, and easy fatigability, which led to the discovery of locally advanced likely metastatic prostate cancer. This discussion explores the unusual presentation, diagnostic challenges, and therapeutic strategies involved in the management of this case.
Prostate cancer typically manifests with urinary symptoms, such as frequency, urgency, nocturia (2), and hematuria. Metastasis often involves the bones, leading to bone pain and fractures (13). However, rectal bleeding as a presenting symptom is rare and can lead to misdiagnoses. The patient’s symptoms were initially suggestive of primary colorectal pathology. Rectal bleeding in the patient is likely due to direct invasion of the rectal mucosa by the prostate tumor, which underscores the aggressive nature of the disease (14). Prostate cancer invading the rectum is rare, but has been documented in advanced cases, suggesting a poor prognosis and a higher likelihood of metastatic spread (10).
Initial clinical evaluation and imaging studies, including colonoscopy, are crucial in excluding primary colorectal malignancies. A nodular, irregular prostate with a PSA level exceeding 200 ng/ml was strongly indicative of advanced prostate cancer. The diagnosis was further supported by histopathological examination of the prostate biopsy specimen, which revealed a Gleason score of 8 (4 + 4) adenocarcinoma with extensive involvement.
The presence of osteoblastic lesions in the lumbosacral spine on X-ray and high PSA levels were consistent with metastatic prostate cancer. Osteoblastic lesions are hallmarks of prostate cancer metastasis to the bone and are characterized by the formation of new bone material (15). The patient’s anemia was likely multifactorial, resulting from chronic disease and possibly from ongoing blood loss (14).
Another atypical aspect of the patient’s presentation was the presence of psoriasiform dermatitis, a condition that is not commonly associated with prostate cancer. Skin manifestations in prostate cancer are rare and typically associated with paraneoplastic syndromes or direct metastatic involvement (16). The histopathology of the skin lesions revealed (a benign condition) psoriasiform dermatitis rather than metastatic disease, adding another layer of complexity to his clinical picture. Psoriasiform dermatitis in the context of cancer may be related to immune dysregulation, although its exact association with prostate cancer remains unclear (16, 17).
Prostate cancer, especially in the advanced stages, can lead to immunological dysregulation. This dysregulation can result from cancer itself and the body’s response to cancer. Importantly, even in the absence of treatment, cancer can cause significant changes in immune function (18).
1. Cancer and Immune System Interaction: Advanced prostate cancer can affect the immune system in several ways. Tumor cells can evade the immune system through various mechanisms, including alteration of the tumor microenvironment and suppression of the immune response. Chronic inflammation associated with cancer can also lead to immune system changes (18).
2. Treatment-Induced Dysregulation: Treatments for advanced prostate cancer, such as chemotherapy, androgen deprivation therapy (ADT), and newer immunotherapies, can also affect the immune system. These treatments may weaken the immune response or, conversely, trigger immune-related adverse events (18, 19).
1. Paraneoplastic Syndromes: Advanced cancers, including prostate cancer, occasionally lead to paraneoplastic syndromes. These conditions are caused by the immune system’s response to the tumor and can affect various organs, including the skin (16).
2. Generalized Psoriasiform Dermatitis: Although less common, advanced prostate cancer is associated with paraneoplastic skin conditions. Psoriasiform dermatitis, which is characterized by skin lesions resembling psoriasis, can occur in patients with paraneoplastic syndromes. This type of dermatitis is marked by red scaly patches that can spread across the body (16, 20).
Mechanisms: The exact mechanisms by which prostate cancer might lead to generalized psoriasiform dermatitis are not fully understood but could involve the following:
● Cytokine release and inflammatory mediators from tumor and immune cells (18).
● Cross-reactivity of immune cells, targeting both tumor and skin antigens (16).
● Immune system dysregulation induced by cancer (18).
In this case, the patient developed generalized psoriasiform dermatitis before initiating treatment for prostate cancer. This suggests that immunological dysregulation and the resulting skin lesions were related to the cancer itself, rather than a side effect of cancer treatment. This aligns with the understanding that advanced prostate cancer can cause significant immune system changes independent of external therapeutic interventions (18).
In conclusion, advanced prostate cancer can cause immunological dysregulation, leading to various systemic manifestations, including skin conditions, such as generalized psoriasiform dermatitis. If a patient with advanced prostate cancer presents with unusual or widespread skin lesions, it is essential to consider the potential paraneoplastic nature of these symptoms and to manage them appropriately in conjunction with oncological treatment.
Patient management required a multidisciplinary approach involving urology, proctology, oncology, and dermatology. The initial therapeutic strategy focused on controlling bleeding and addressing metastatic disease. Androgen deprivation therapy (ADT) with Casodex (bicalutamide) a priori, followed by surgical castration, is a common first-line treatment for advanced prostate cancer (21–23). ADT aims to reduce the levels of androgens that fuel prostate cancer growth (22). In addition to hormonal therapy, the anemia was managed with blood transfusions.
Given the index case’s high-risk and advanced metastatic prostate cancer, his treatment plan included potential external beam radiotherapy and chemotherapy with docetaxel, which are standard treatments for advanced prostate cancer with bone metastases. Studies have shown that combining ADT with radiotherapy and chemotherapy can improve survival outcomes in patients with metastatic hormone-sensitive prostate cancer (12).
Furthermore, this case highlights the importance of considering atypical presentations in patients with known risk factors for prostate cancer. The patient’s positive family history of prostate cancer and prior diagnosis of BPH should have heightened clinical suspicion earlier in his presentation. This underscores the need for comprehensive evaluation and a high index of suspicion in similar cases (24, 25).
This case illustrates the diagnostic challenges of atypical prostate cancer presentations such as rectal bleeding, rectal pain, and psoriasiform dermatitis. The modest success of therapy in this advanced stage of diagnosis, further emphasizes the need for early recognition and multidisciplinary approaches for prostate cancer management.
Further research is essential to understand these atypical manifestations and improve early detection and management strategies.
The original contributions presented in the study are included in the article/supplementary material. Further inquiries can be directed to the corresponding author.
Ethical approval was not required for the studies involving humans because not applicable to this research, since it is a case study. The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study. Written informed consent was obtained from the individual(s) for the publication of any potentially identifiable images or data included in this article.
FO: Conceptualization, Data curation, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Writing – original draft, Writing – review & editing. AFA: Conceptualization, Data curation, Methodology, Writing – original draft, Writing – review & editing. SG: Investigation, Methodology, Writing – original draft, Writing – review & editing. BYS: Investigation, Writing – original draft, Writing – review & editing. EA: Investigation, Writing – original draft, Writing – review & editing. NA: Investigation, Methodology, Writing – original draft, Writing – review & editing. AMA: Supervision, Writing – original draft, Writing – review & editing.
The author(s) declare that no financial support was received for the research and/or publication of this article.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
1. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. (2018) 68:394–424. doi: 10.3322/caac.21492
2. Kyei MY, Mensah JE, Djagbletey R, Akpali E, Ahiaku F, Ayamba A, et al. Trifecta outcomes of screening detected and patients with lower urinary tract symptoms after open radical prostatectomy for localized prostate cancer. Open J Urol. (2023) 13:282–92. doi: 10.4236/oju.2023.138032
3. Schröder FH, Hugosson J, Roobol MJ, Tammela TLJ, Ciatto S, Nelen V, et al. Screening and prostate-cancer mortality in a randomized european study. N Engl J Med. (2009) 360:1320–8. doi: 10.1056/NEJMoa0810084
4. Ahmad A, Tan W. Atypical presentation of prostate cancer and the workup of an adenocarcinoma of unknown primary. World J Oncol. (2012) 3:187–90. doi: 10.4021/wjon482w
5. Salako A, Badmus T, Komolafe A, David R, Igbokwe M, Laoye A, et al. Unusual presentation of advanced prostate cancer in a black population of South-Western Nigeria. Pan Afr Med J. (2019) 32. doi: 10.11604/pamj.2019.32.15.14417
6. Oyortey MA, Adanu KK, Ali MA. The effect of unusual presentation on delayed diagnosis of prostate cancer : a case series. J Med Case Rep. (2024) 18:1–6. doi: 10.1186/s13256-024-04543-x
7. Özgür BC, Gültekin S, Ekici M, Yılmazer D, Alper M. A narrowing range of bone scan in newly diagnosed prostate cancer patients: A retrospective comparative study. Urol Ann. (2015) 7:193–8. Available online at: http://www.ncbi.nlm.nih.gov/pubmed/25835063.
8. Joensuu T, Joensuu G, Kairemo K, Kiljunen T, Riener M, Aaltonen A, et al. Multimodal primary treatment of metastatic prostate cancer with androgen deprivation and radiation. Anticancer Res. (2016) 36:6439–47. doi: 10.21873/anticanres.11242
9. Hugosson J, Roobol MJ, Tammela TLJ, Nelen V, Kwiatkowski M, Lujan M, et al. (2020) 76:43–51. HHS Public Access.
10. Haq MS, Thomas PM, Almonte M, Mohan V. Prostate cancer presenting with an unusual presentation of rectal pain and bleeding. Cureus. (2021) 13:1–5. doi: 10.7759/cureus.18766
11. Tengue K, Kpatcha T, Sewa E, Sikpa K, Botcho G, Leloua E, et al. Prostate cancer revealed by skin metastasis: A case report in black African man. Afr J Urol [Internet]. (2017) 23:204–7. Available online at: https://linkinghub.elsevier.com/retrieve/pii/S1110570416301333 (Accessed March 15, 2025).
12. Kishan AU, Karnes RJ, Romero T, Wong JK, Motterle G, Tosoian JJ, et al. Comparison of multimodal therapies and outcomes among patients with high-risk prostate cancer with adverse clinicopathologic features. JAMA Netw Open. (2021) 4:1–13. doi: 10.1001/jamanetworkopen.2021.15312
13. European Association of Urology. The European Association of Urology Guidelines. Arnhem, The Netherlands: EAU Guidelines Office (2017). Available online at: http://uroweb.org/guidelines/compilations-of-all-guidelines/ (Accessed March 15, 2025).
14. Ekwere PD, Egbe SN. The changing pattern of prostate cancer in Nigerians: current status in the southeastern states. J Natl Med Assoc. (2002) 94:619–27. Available online at: http://www.ncbi.nlm.nih.gov/pubmed/12126288.
15. Ayyathurai R, Mahapatra R, Rajasundaram R, Srinivasan V, Archard NP, Toussi H. A study on staging bone scans in newly diagnosed prostate cancer. Urol Int. (2006) 76:209–12. Available online at: http://www.ncbi.nlm.nih.gov/pubmed/16601380.
16. Da Silva JA, Mesquita KDC, Igreja ACDSM, Lucas ICRN, Freitas AF, de Oliveira SM, et al. Paraneoplastic cutaneous manifestations: concepts and updates*. Bras Dermatol. (2013) 88:09–22. doi: 10.1590/S0365-05962013000100001
17. de Castro e Souza B, Miyashiro D, Pincelli MS, Sanches JA. Cutaneous metastases from solid neoplasms – Literature review. Anais Brasileiros de Dermatologia. (2023) 98(5):571–9. doi: 10.1016/j.abd.2022.10.009
18. Bou-Dargham MJ, Sha L, Sang QXA, Zhang J. Immune landscape of human prostate cancer: Immune evasion mechanisms and biomarkers for personalized immunotherapy. BMC Cancer. (2020) 20:1–10. doi: 10.1186/s12885-020-07058-y
19. Wang I, Song L, Wang BY, Rezazadeh Kalebasty A, Uchio E, Zi X. Prostate cancer immunotherapy: a review of recent advancements with novel treatment methods and efficacy. Am J Clin Exp Urol. (2022) 10:210–33. Available online at: http://www.ncbi.nlm.nih.gov/pubmed/36051616%0A.
20. Johansson JE, Andrén O, Andersson SO, Dickman PW, Holmberg L, Magnuson A, et al. Natural history of early, localized prostate cancer. JAMA. (2004) 291:2713–9. Available online at: http://www.ncbi.nlm.nih.gov/pubmed/15187052.
21. Yeboah ED, Hsing AW, Mante S, Mensah JE, Kyei MY, Yarney J, et al. Management of prostate cancer in Accra, Ghana. J West Afr Coll Surg. (2016) 6:31–65. Available online at: http://www.ncbi.nlm.nih.gov/pubmed/29181364.
22. Lorent M, Maalmi H, Tessier P, Supiot S, Dantan E, Foucher Y. Meta-analysis of predictive models to assess the clinical validity and utility for patient-centered medical decision making: Application to the CAncer of the Prostate Risk Assessment (CAPRA). BMC Med Inform Decis Mak. (2019) 19:1–12. doi: 10.1186/s12911-018-0727-2
23. Tyrrell CJ, Kaisary AV, Iversen P, Anderson JB, Baert L, Tammela TL, et al. A randomized comparison of 'Casodex' (bicalutamide) 150 mg monotherapy versus castration in the treatment of metastatic and locally advanced prostate cancer. European Urology. (1998) 33(5):447–56.
Keywords: atypical presentation of prostate cancer, lower gastrointestinal bleeding, psoriasiform dermatitis, metastasis, androgen deprivation therapy, gleason score, multidisciplinary approach, case report
Citation: Obeng F, Adamu AF, Gavor SE, Setsoafia BY, Antwi EK, Affram N and Ali AM (2025) Case Report: Atypical prostate cancer presentation: rectal bleeding, pain, and psoriasiform dermatitis. Front. Oncol. 15:1476988. doi: 10.3389/fonc.2025.1476988
Received: 07 August 2024; Accepted: 03 March 2025;
Published: 26 March 2025.
Edited by:
Salvatore Siracusano, University of L’Aquila, ItalyCopyright © 2025 Obeng, Adamu, Gavor, Setsoafia, Antwi, Affram and Ali. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Frank Obeng, Zm9iZW5nQHVhaGFzLmVkdS5naA==
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.