
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Neurol. , 04 April 2025
Sec. Neurotrauma
Volume 16 - 2025 | https://doi.org/10.3389/fneur.2025.1536421
This article is part of the Research Topic Mechanisms of Traumatic Brain Injury and its Pharmacotherapy View all 4 articles
 Tee-Tau Eric Nyam1†
Tee-Tau Eric Nyam1† Kuan-Chi Tu1†
Kuan-Chi Tu1† Yun-Hsuan Kuo2
Yun-Hsuan Kuo2 Che-Chuan Wang1
Che-Chuan Wang1 Chung-Feng Liu3
Chung-Feng Liu3 Jen-Chieh Liao1*
Jen-Chieh Liao1* Ching-Lung Kuo1,2,4*
Ching-Lung Kuo1,2,4*This study investigates the relationship between mortality and specific clinical factors in patients with severe traumatic brain injury (TBI) who present with a Glasgow Coma Scale (GCS) score of 3. Data from 161 adult patients were collected from the Chi-Mei Medical Center in Taiwan, spanning 2010 to 2019. The findings revealed an overall mortality rate of 44.10%, with significant predictors of mortality identified as age and pupil size. The Spearman correlation analysis showed that both age and pupil sizes were positively correlated with mortality rates. Multiple logistic regression confirmed age and left pupil size as strong predictors of mortality. Patients with GCS 3 and both unreactive pupils measuring 4 mm or more experienced the highest mortality rate of 68.39%, while those with pupils less than 4 mm had a lower mortality rate of 32.26%. The study determined optimal cut-off values for age and pupil size using ROC and AUC analysis, highlighting the significance of age in mortality predictions. These findings underscore the critical role of age and pupil size in the prognosis of TBI patients and provide valuable guidance for clinicians managing such cases.
Traumatic brain injury (TBI) rates have risen steadily in the US, from 521 cases per 100,000 in 2001 to 824 in 2010 (1). After TBI, mortality rates are about 11.2 per 100,000 in Europe (57,000 deaths) and 17.7 per 100,000 in the US (53,000 deaths) (2, 3). In Taiwan, TBI mortality rates range from 26.15 to 36.36% between 1997 and 2007 (4, 5). TBI remains a significant public health concern, straining resources and impacting patients’ well-being (6).
The Glasgow Coma Scale (GCS), introduced by Teasdale and Jennett (7) and revised in 1976, assesses eye, verbal, and motor responses, with scores ranging from 3 to 15. A score of 8 or lower indicates critical condition requiring intubation (7, 8). A GCS score of 3 at initial assessment is strongly linked to poor prognosis (9–13), with mortality rates between 49.2% (12) and 89% (9). Physicians facing TBI patients with a GCS score of 3 grapple with questions regarding survival, aggressive treatments, and potential recovery.
Several studies have identified key predictive factors for TBI outcomes, including age and surgery (14), sex (15), obesity (16), GCS, pupil reactivity (17), midline shift in computed tomography (CT) findings (18), coagulopathy (19) and associated extracranial injuries (20). Age, GCS, pupil reactivity, brain CT findings, and intracranial pressure are particularly important for patients with severe initial assessments. However, most predictors require post-admission evaluation through blood sampling, imaging studies, or surgery. Early mortality risk prediction and detailed pupil size assessment in ER triage remain areas requiring further clarification.
Recently, our team has developed a computer-assisted system that eliminates the need for brain CT scans and blood sampling to predict early mortality risk in TBI patients during the emergency room triage process (21). This predictive model incorporates essential twelve variables (22, 23). These variables are recognized as significant prognostic indicators for trauma patients. This study aimed to predict mortality risk for TBI patients with a GCS score of 3 at ER arrival using twelve variables. We analyzed the hospital’s TBI database retrospectively to identify key factors associated with early outcomes, aiming to inform healthcare decisions and educate patient families.
All head injury patients who presented at the emergency room triage of Chi-Mei Medical Center between 2010 and 2019 were retrospectively included in this study. The inclusion criteria were as follows: patients with head trauma who were admitted to the ER and had the following diagnostic codes—ICD-9: 800*-804*, 850*-854*, 959.0, 959.01, 959.8–959.9, ICD-10: S00*-T07*. Patients with missing or ambiguous values were excluded. Other patients and the public were not involved in any way in this research. Figure 1 displays the study flow diagram.
The twelve feature variables including patients’ age, gender, body mass index (BMI), Taiwan Triage and Acuity Scale (TTAS), heart rate, body temperature, respiratory rate, GCS, left and right pupil size, and light reflex were enrolled due to their wide availability in the triage setting. Dilated pupils were defined as ≥4 mm in diameter (11). The presence of unresponsive pupil is defined as unresponsive (<1 mm) to a light stimulus (19, 24). The pupillary light reflex was divided into three categories including both unreactive, one unreactive and both reactive. All patients in our hospital received the standard management protocol for TBI patients. Specifically, following surgery, patients underwent cerebral perfusion-guided management with the goal of maintaining a cerebral perfusion pressure of 60 mmHg or higher and ensuring intracranial pressure remained at 20 mmHg or lower. The recorded outcome was categorized as either mortality or survival.
Significant testing was conducted using the t-test for numerical variables and the Chi-square test for categorical variables. Additionally, data were analyzed using Spearman’s correlation method to demonstrate the strength of the correlation between each feature and mortality. Multiple logistic regression models were used for correlation between two variables and defined the independent risk factors for poor outcome. Using the Receiver Operating Characteristic (ROC) and the area under curve (AUC), variables cutoff value and its reliability in prognosis could be estimated (25). Commercial statistical software (SPSS for Windows, Version 15, SPSS Inc., Chicago, IL, United States) was utilized for this analysis. p-values less than 0.05 were considered statistically significant.
This study obtained ethics approval (IRB no. 10911-006) from the Institutional Review Board of Chi Mei Medical Center in Tainan, Taiwan. The authors conducted all methods in compliance with applicable guidelines and regulations. The Ethics Committee waived the need for informed consent due to the retrospective nature of the study.
A total of 161 patients were retrospectively included from the electronic medical records system of Chi-Mei Hospital. There were 118 males and 43 females. The average age was 55.64 ± 17.41 years (mean ± SD). Seventy-one patients died, and the total mortality rate was 44.10% (71/161). The survival time from ER arrival to discharge is 6.18 ± 5.68 days. Among these 11 features, age (p < 0.001**), left and right pupil size (p < 0.001**), and pupil light reflex (p = 0.001**) showed a significant difference in relation to mortality. Table 1 provides detailed information about the demographics and clinical pictures of patients with TBI.
Table 2 displays the correlations between various features and mortality, measured using the Spearman correlation coefficient (r). Among these features, age (r = 0.342, p < 0.001**) and the size of the left (r = 0.357, p < 0.001**) and right pupils (r = 0.357, p < 0.001**), as well as both unreactive pupil light reflex (r = 0.282, p < 0.001**), exhibit significant positive correlations with mortality. This underscores their substantial impact on prediction.
In the multiple logistic regression models, the adjusted odds ratio (OR) for predicting mortality was significant for age (OR 1.044, 95% CI 1.021–1.068; p < 0.001**) and left pupil size (OR 1.712, 95% CI 1.312–2.232; p < 0.001**) (Table 3).
The overall mortality rate for patients with a Glasgow Coma Scale (GCS) score of 3 was 44.10%. Among these patients, those with a GCS score of 3 and both unreactive pupils with both pupils measuring ≥4 mm exhibited the highest mortality rate, which was 69.39% (34 out of 49 cases). In contrast, patients with a GCS score of 3 and both unreactive pupils with both pupils measuring <4 mm had the lowest mortality rate, at 32.26% (10 out of 31 cases). For a more comprehensive understanding of the association between pupil reactivity and size with mortality in patients with a GCS score of 3, the detailed information was provided in Table 4.
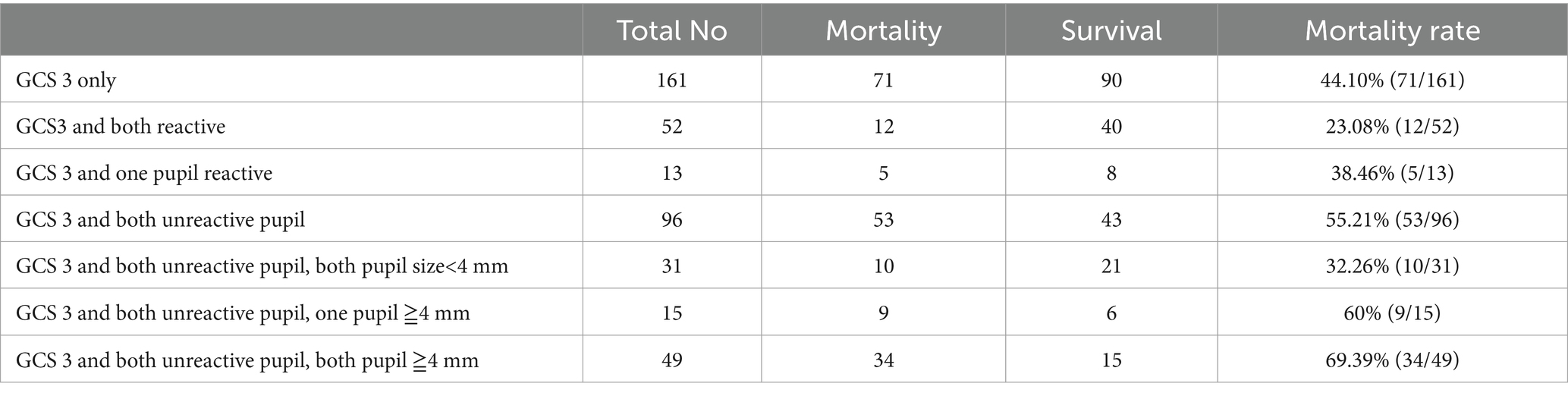
Table 4. The mortality rate in patients with combination of pupil reactivity and size for Glasgow coma scale scores 3.
In Tables 5–7, we observed varying results regarding the statistical significance of different variables concerning mortality and survival groups under distinct pupil conditions. Specifically, in Table 5, only the variable ‘age’ exhibited a statistically significant difference between the mortality and survival groups when considering individuals with both unreactive pupils and pupils with a size less than 4 mm. On the other hand, in Table 6, it revealed that ‘age’ was significantly different between these groups when one pupil had a size of 4 mm or greater. Lastly, Table 7 indicated that the variable ‘age’ showed significant differences between the mortality and survival groups when both pupils had a size of 4 mm or greater. However, the other variables did not display statistically significant differences in either case.
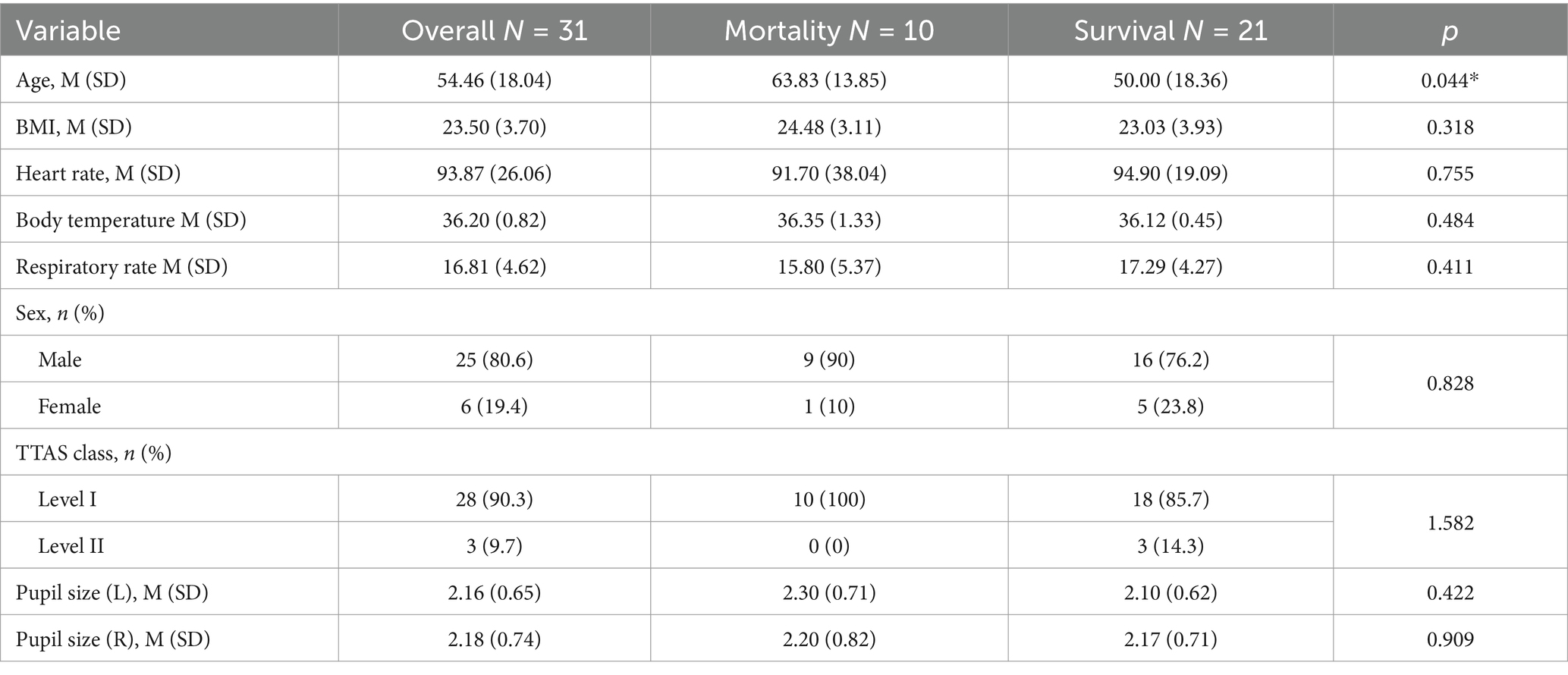
Table 5. Comparison of mortality and survival groups with both unreactive pupil and both pupil size <4 mm.
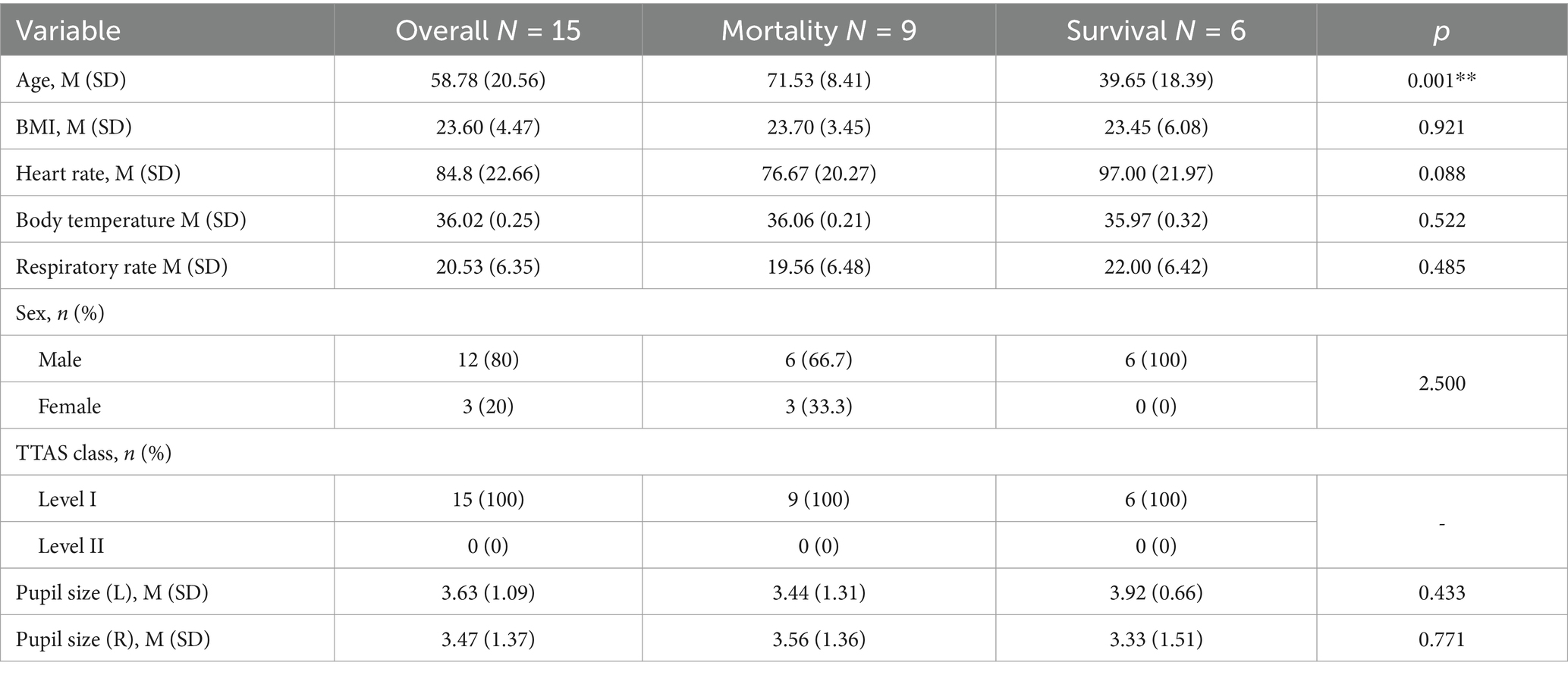
Table 6. Comparison of mortality and survival groups with both unreactive pupil and one pupil ≧4 mm.
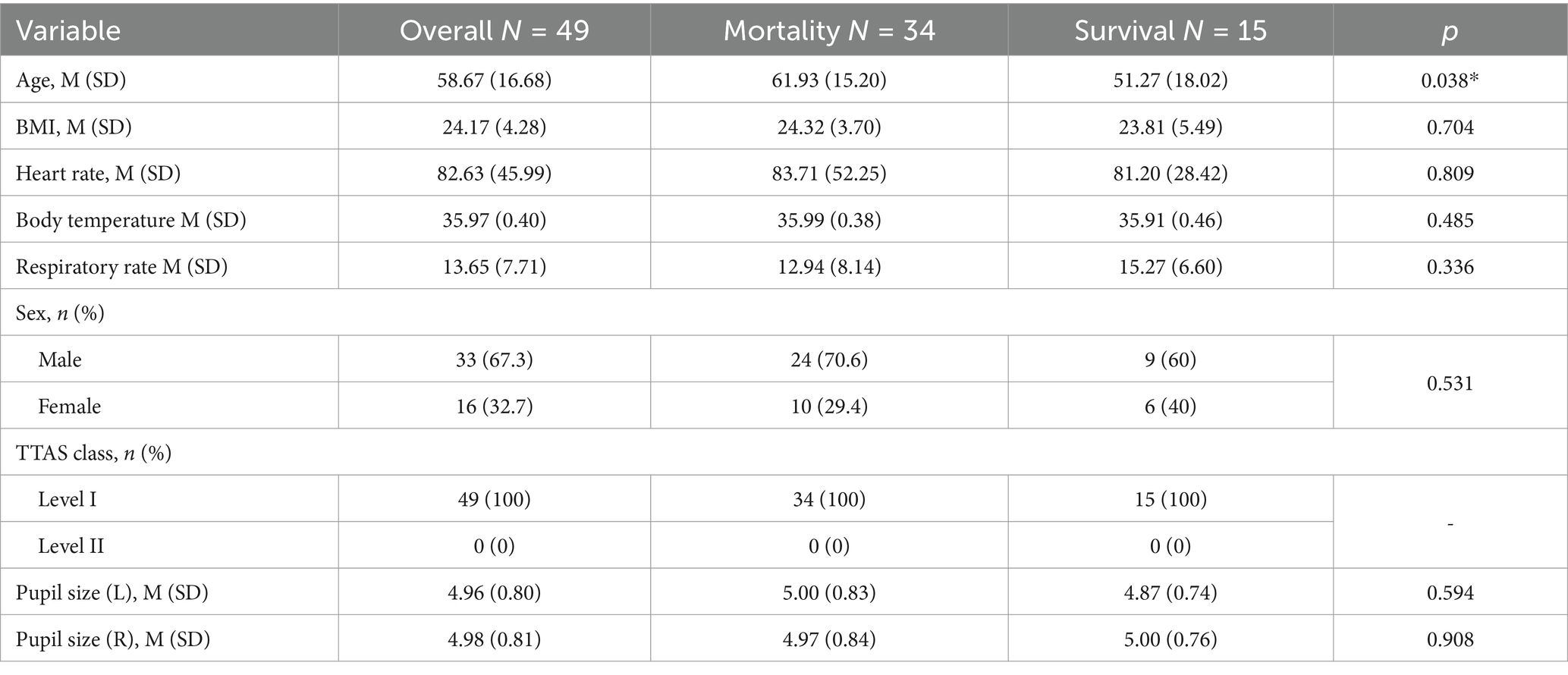
Table 7. Comparison of mortality and survival groups with both unreactive pupil and both pupil size≧4 mm.
Through ROC analysis and AUC calculations, we have identified key cutoff points in our study. For GCS 3 patients, we discovered an age cutoff point of 41.11 years, which strikes a balance between sensitivity (0.944) and specificity (0.367). The AUC for age was 0.689 with a 95% CI of 0.608–0.770 (Figure 2). Additionally, we established a reliable left pupil size cutoff point at approximately 3.25 mm, with an AUC of 0.703 (Figure 3). Furthermore, the cutoff point for right pupil size was 3.25 mm, and the AUC was 0.609 (Figure 4).
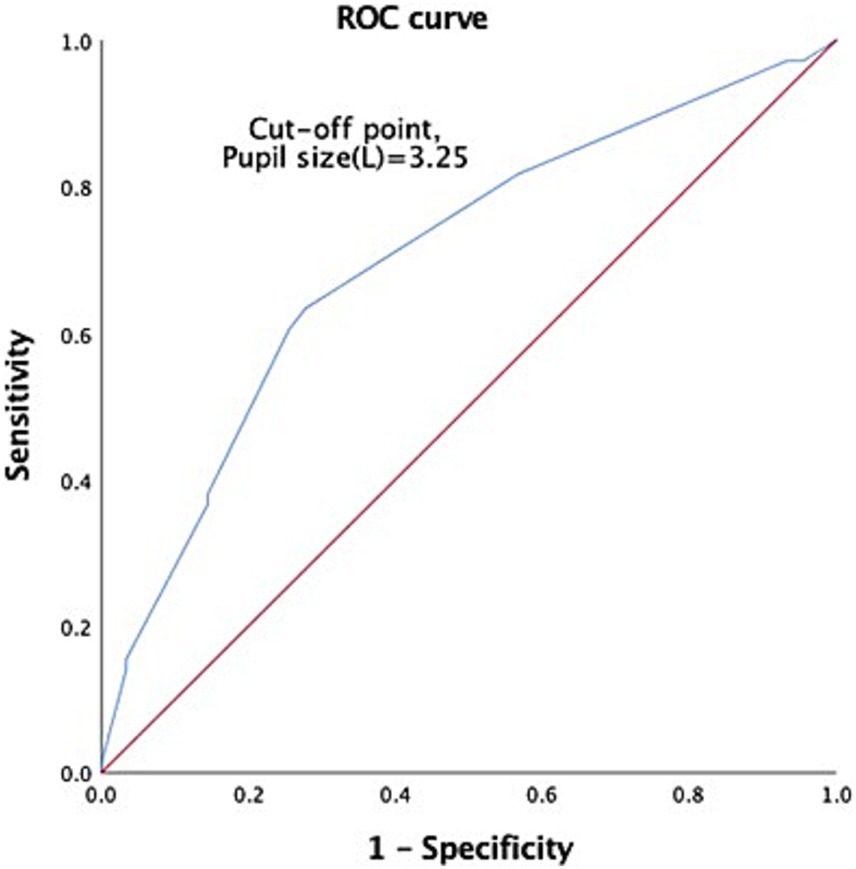
Figure 2. Receiver operating characteristics curve (ROC) to predict the probable mortality of TBI patients by measurement of age. A value of 41.11 y/o was considered the cutoff point, with AUC 0.689, 95% CI 0.608–0.770.
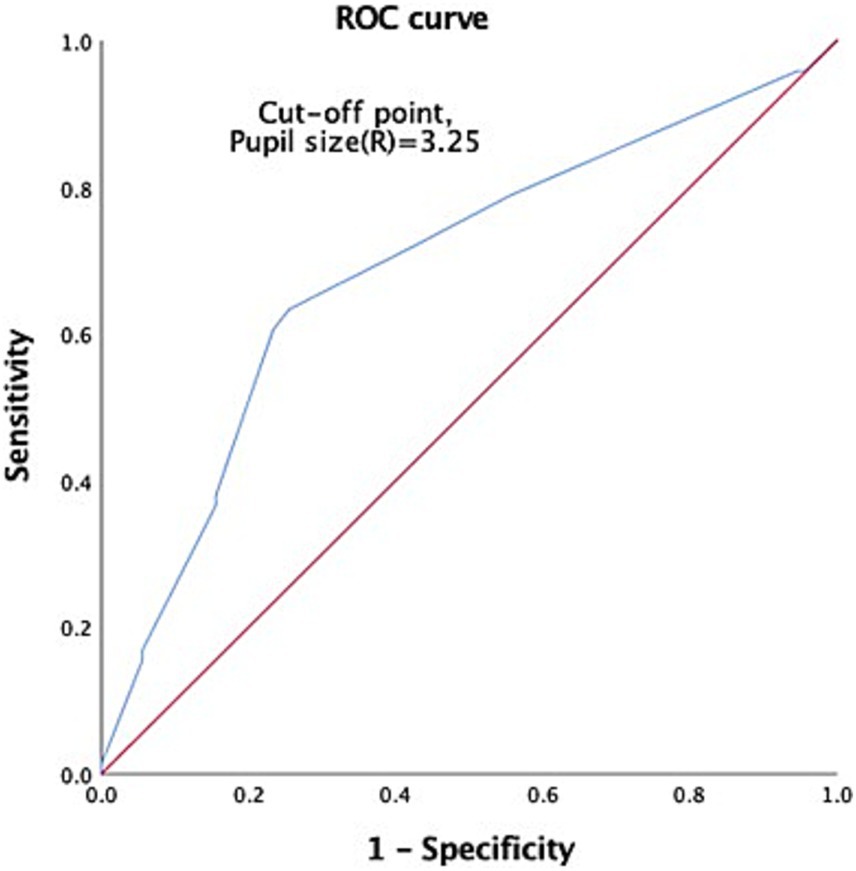
Figure 3. ROC to predict the probable mortality of TBI patients by measurement of left pupil size. A value of 3.25 mm was considered the cutoff point, with AUC 0.703, 95% CI 0.621–0.785.
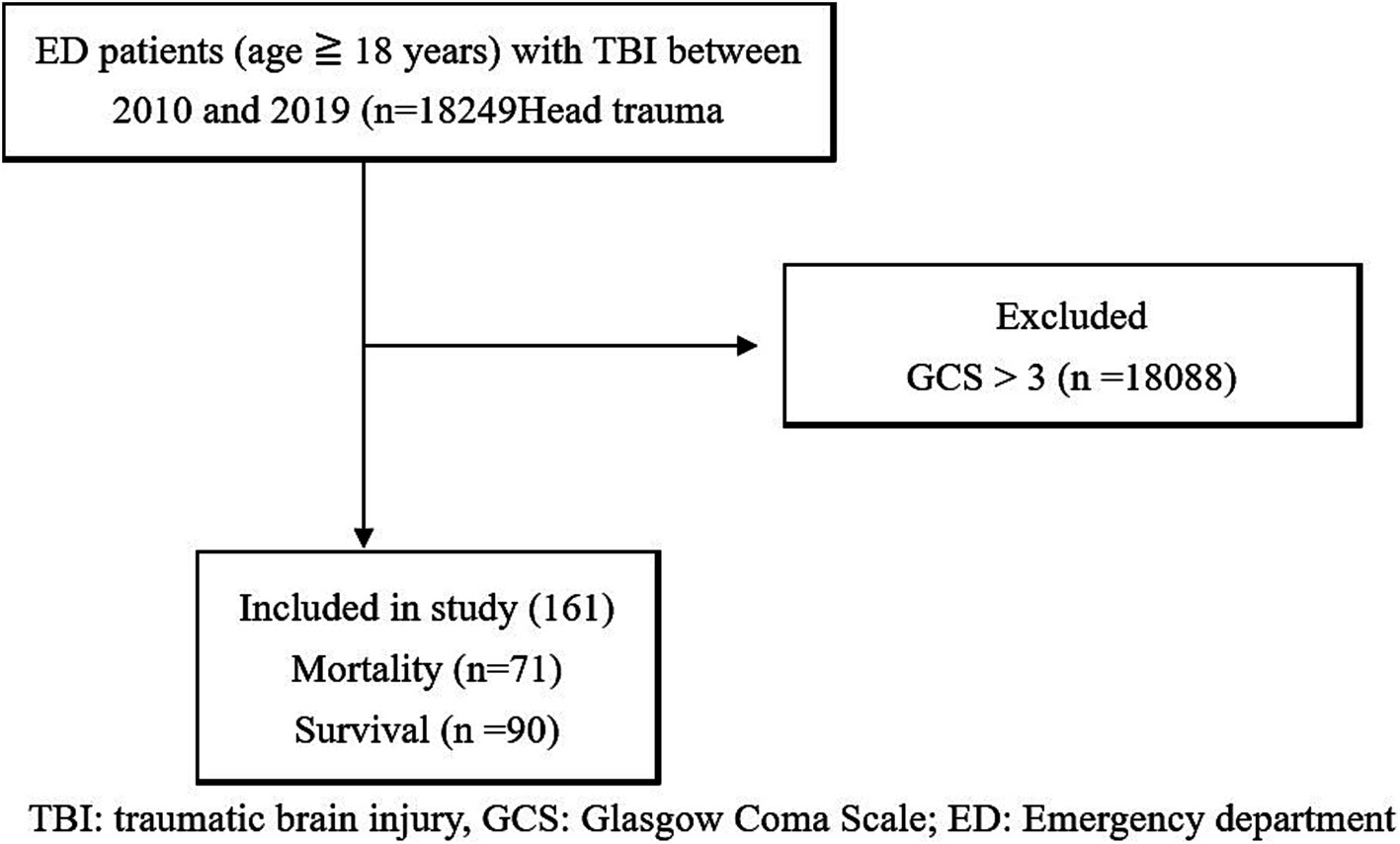
Figure 4. ROC to predict the probable mortality of TBI patients by measurement of right pupil size. A value of 3.25 mm was considered the cutoff point, with AUC 0.690, 95% CI 0.606–0.775.
We also evaluated GCS 3 patients with unreactive pupils and those with GCS 3 plus unreactive pupils and both pupils ≥4 mm, taking into account age, left pupil size, and right pupil size AUC cutoff points, among other factors. This showed the cut off points for age and pupil size are 58.55 years and 3.75 mm (left), 3.25 mm (right), respectively in GCS 3 with unresponsive pupil light reflex. Detailed results are provided in Table 8.
Table 9 showed a comparison with related studies in TBI patients. Long study period (2010–2019) providing a comprehensive view. Our research includes a broader age distribution, encompassing older patients (21.2% are over 70 years old). Our study meticulously records both pupil size and reactivity. In contrast, some other studies either lack this data or do not provide corresponding information.
This study conducted a review of relevant literature and introduced an innovative approach to early mortality risk prediction in the emergency triage setting, without the need for brain CT scans or blood sampling. We offer a more precise method for assessing a patient’s risk by considering various variables, including the size and reactivity of the left and right pupils, which are combined to provide a comprehensive assessment. We have also established specific thresholds for age (58.55 years), left pupil size 3.75 mm and right pupil size 3.25 mm that are associated with predicting the risk of death in TBI patients with GCS 3 and unresponsive pupil light reflex. These distinctions can aid physicians in accurately evaluating the risk of TBI patients and in developing more effective treatment plans. Nonetheless, it is advisable for physicians to consider the results of multiple studies when making clinical decisions.
A GCS score of 3 at the initial assessment has been associated with high mortality rates: 49.2% (12), 64% (10), 80.6% (13), and 89% (9). In our current study, the mortality rate was 44.10%, similar to Chamoun RBs’ reported 49.2% and better than the others (Table 8). This discrepancy may be related to changes in healthcare practices (e.g., ICP-guided management), patient characteristics (such as age distribution), and the timing of the observation endpoint (whether in-hospital or 6 months later).
Our results (Table 4) suggest that when patients have a GCS score of 3 and both pupils are reactive, the mortality rate is 23.08% (12/52), similar to Chamoun RBs’ reported 23.5% (12). Additionally, we observed that patients with a GCS score of 3 and both unreactive and dilated pupils (≥4 mm) have a significantly higher mortality rate of 69.39%, which is lower than the 79.7% reported by Chamoun et al. (12). In contrast, patients with a GCS score of 3 and both unreactive pupils with both pupils measuring <4 mm have a lower mortality rate (32.26%) compared to the GCS of 3-only group (44.10%). These statistics indicate that the combination of a low GCS score and pupil reactivity has varying impacts on the likelihood of patient survival, and this information is crucial for understanding patient outcomes in cases of severe neurological impairment. Therefore, we want to emphasize the importance of measuring pupil size in predicting mortality.”
Numerous studies consistently underscore the pivotal role of age in predicting prognosis. For instance, in patients with a Glasgow Coma Scale (GCS) score of 3 suffering from traumatic brain injury (TBI), earlier research found that all survivors were under 50 years old (9), while individuals above 55 faced a notably higher mortality risk (10). In our current study, non-survivors had a mean age of 62.32 years, whereas survivors averaged 50.37 years (Table 1). This discrepancy may be attributed to the relatively advanced age of our patient cohort compared to that in previous studies (Table 8). It is plausible that older patients may have pre-existing chronic health issues that negatively impact their recovery ability (26), whereas younger individuals may possess more resilient brains better able to withstand damage (27). Additionally, treatment complications and effectiveness may vary between younger and older individuals, potentially influencing treatment outcomes (28).
We also reaffirm that age is an independent predictive factor for mortality (as shown in Tables 3, 5–7). Furthermore, we identified specific age thresholds of 41.11, 58.55, and 43.87 years in three categories with varying feature combinations (as presented in Table 8). In all three categories, age emerges as the most clinically significant feature, exhibiting the highest AUC and statistical significance. Notably, pupil size, especially right pupil size, holds less significance in Category III. These findings suggest that age outperforms pupil size as a predictor of patient condition in these categories. Importantly, age is a non-invasive and easily obtainable parameter, making it a practical clinical tool. The age threshold can be clinically applied to assist in decisions regarding TBI conditions.
Lieberman et al. reported 100% mortality in cases with fixed, dilated pupils (29). In the current study, both the size of the left (r = 0.357, p < 0.001**) and right (r = 0.357, p < 0.001**) pupils showed a significant correlation with mortality. This suggests that both left and right pupil size measurements appear to have potential clinical significance, and that patients with larger pupils have a higher risk of mortality (Table 2). Additionally, we observed that left pupil size had an odds ratio of 1.712 (p < 0.001**) for independently predicting mortality (Table 3). Furthermore, left pupil size, with a slightly higher area under the curve (AUC) value than the right pupil, was found to be a significant predictor of prognosis in different feature combinations (Tables 5–7).
The probable reasons for the left pupil size being a more meaningful determinant of prognosis compared to the right pupil size may relate to (1) left-sided dominance brain injuries could affect functions that are more closely linked to the left eye, which might be reflected in left pupil size, (2) specific injuries or conditions on the left side of the brain that we were not considered in this study.
In the current study, the setting was the triage of the ER, and no imaging studies had been conducted yet. Therefore, left hemisphere compression by hematomas, or cases with greater midline shift, were not considered as predictors. However, it’s possible that left pupil size was associated with more cases of left hemisphere compression by hematomas, or those with greater midline shift. In the future, it will be necessary to include the aforementioned parameters as predictors of mortality. Pupil size measurements can be valuable in assessing and stratifying the risk of TBI patients. Further research and clinical validation may be necessary to determine the most effective clinical applications.”
Recently, several studies have shown that both age and pupil conditions are among the top predictors of in-hospital mortality after TBI (30–32). These studies also indicate that brain CT findings serve as important predictors. Our results are consistent with these findings. However, even without CT examination, we identified age and pupil size as key predictors of mortality in TBI patients with GCS 3 in the triage setting.
Our study underscores the significance of early mortality assessment in patients with a GCS score of 3, a group already recognized for its challenging prognosis. The recognition that age and pupil size serve as robust mortality predictors equips healthcare providers with valuable tools for making well-informed decisions in TBI patient management. This knowledge facilitates a more precise and individualized approach to care. For instance, patients exhibiting identified risk factors, such as advanced age or specific pupil size, can be closely monitored, and timely interventions can be initiated to enhance their chances of survival and minimize unfavorable outcomes while simultaneously improving their overall quality of life.
Furthermore, our study illuminates the necessity for additional research. While age and pupil size have emerged as prominent predictors, other variables have shown varying degrees of significance. This highlights the potential for further investigations into additional factors that might contribute to TBI patient outcomes, thus leading to a more comprehensive understanding of prognosis and the development of more effective treatment strategies.
Our study possesses several strengths. Firstly, the data in the current study is the most recent, covering the period from 2010 to 2019, thus reflecting the latest advancements in modern medical practices and technologies. Secondly, unlike other studies, our research includes a broader age distribution, encompassing older patients (22% over 70 years), which enhances our ability to gain a more comprehensive understanding of prognosis across various age groups. Thirdly, our study meticulously records both pupil size and reactivity, both of which are critical prognostic factors. In contrast, some other studies either lack this data or do not provide corresponding information.
However, it’s important to acknowledge several limitations in our study. Firstly, as a retrospective observational study, there is the possibility of miscoded feature variables. Researchers have limited control over the data collection process, which may introduce biases or confounding factors. Secondly, in comparison to some other studies, the current study has a relatively smaller sample size (161 cases), potentially constraining its statistical power and limiting the generalizability of findings to larger and more diverse patient populations. Thirdly, the accuracy of GCS scores and the consistency in measuring pupil size and reactivity may vary among different healthcare providers, potentially leading to measurement errors. Fourthly, the study, conducted at the ER triage, did not account for the existence of uncontrolled or unmeasured confounding factors that could influence the results. For instance, other medical conditions, various treatments, surgical procedures, and complications that could impact the outcome after TBI were not considered in the analysis. Finally, variations in study endpoints, with some studies focusing on in-hospital outcomes while others use a 60-day endpoint, may affect the comparability of study results.
Consequently, there is a need for larger prospective studies with more comprehensive data collection and the inclusion of additional variables to be considered in future research.
In conclusion, our research highlights the practical significance of age and pupil size as key predictors of mortality in TBI patients with a GCS score of 3. These findings offer valuable insights for healthcare providers and researchers, enabling them to make more informed decisions in the assessment and management of TBI patients. By taking these factors into account, we can improve patient prognosis and increase their chances of survival.
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
The studies involving humans were approved by the Institutional Review Board of Chi Mei Medical Center, Tainan, Taiwan. The studies were conducted in accordance with the local legislation and institutional requirements. The ethics committee/institutional review board waived the requirement of written informed consent for participation from the participants or the participants' legal guardians/next of kin due to the retrospective nature of the study.
T-TE: Conceptualization, Writing – original draft, Writing – review & editing. K-CT: Writing – original draft. Y-HK: Formal analysis, Methodology, Writing – original draft. C-CW: Conceptualization, Methodology, Supervision, Writing – review & editing. C-FL: Data curation, Formal analysis, Investigation, Methodology, Resources, Writing – review & editing. J-CL: Formal analysis, Writing – original draft. C-LK: Conceptualization, Project administration, Resources, Visualization, Writing – review & editing.
The author(s) declare that no financial support was received for the research and/or publication of this article.
The authors would like to thank all of the researchers, especially Yu-Shan Ma and Yu-Ting Shen, who extended her unwavering support in this study.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The author(s) declare that no Gen AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
1. Centers for Disease Control and Prevention. Traumatic Brain Injory& Concussion. Available online at: www.cdc.gov/traumaticbraininjury/data/
2. Majdan, M, Plancikova, D, Brazinova, A, Rusnak, M, Nieboer, D, Feigin, V, et al. Epidemiology of traumatic brain injuries in Europe: a cross-sectional analysis. Lancet Public Health. (2016) 1:e76–83. doi: 10.1016/S2468-2667(16)30017-2
3. Traumatic Brain Injury-Related Emergency Department Visits. Hospitalizations, and deaths—United States, 2007 and 2013. MMWR Surveill Summ. (2017) 66:1–16. doi: 10.15585/mmwr.ss6609a1
4. Cheng, CY, Ho, CH, Wang, CC, Liang, FW, Wang, JJ, Chio, CC, et al. One-year mortality after traumatic brain injury in liver cirrhosis patients--a ten-year population-based study. Medicine (Baltimore). (2015) 94:e1468. doi: 10.1097/MD.0000000000001468
5. Liao, JC, Ho, CH, Liang, FW, Wang, JJ, Lin, KC, Chio, CC, et al. One-year mortality associations in hemodialysis patients after traumatic brain injury--an eight-year population-based study. PLoS One. (2014) 9:e93956. doi: 10.1371/journal.pone.0093956
6. GBD 2016 Traumatic Brain Injury and Spinal Cord Injury Collaborators. Global, regional, and national burden of traumatic brain injury and spinal cord injury, 1990-2016: a systematic analysis for the global burden of disease study 2016 [published correction appears in Lancet Neurol. 2021, 20(12), e7]. Lancet Neurol. (2019) 18:56–87. doi: 10.1016/S1474-4422(18)30415-0
7. Teasdale, GM, and Jennett, B. Assessment of coma and impaired consciousness. Pract Scale Lancet. (1974) 2:81–4. doi: 10.1016/s0140-6736(74)91639-0
8. Teasdale, GM, and Jennett, B. Assessment and prognosis of coma after head injury. Acta Neurochir. (1976) 34:45–55. doi: 10.1007/BF01405862
9. Kotwica, Z, and Jakubowski, JK. Head-injured adult patients with GCS of 3 on admission—who have a chance to survive? Acta Neurochir. (1995) 133:56–9. doi: 10.1007/BF01404948
10. Demetriades, D, Kuncir, E, Velmahos, GC, Rhee, P, Alo, K, and Chan, LS. Outcome and prognostic factors in head injuries with an admission Glasgow coma scale score of 3. Arch Surg. (2004) 139:1066–8. doi: 10.1001/archsurg.139.10.1066
11. Tien, HC, Cunha, JR, Wu, SN, Chughtai, T, Tremblay, LN, Brenneman, FD, et al. Do trauma patients with a Glasgow coma scale score of 3 and bilateral fixed and dilated pupils have any chance of survival? J Trauma. (2006) 60:274–8. doi: 10.1097/01.ta.0000197177.13379.f4
12. Chamoun, RB, Robertson, CS, and Gopinath, SP. Outcome in patients with blunt head trauma and a Glasgow coma scale score of 3 at presentation. J Neurosurg. (2009) 111:683–7. doi: 10.3171/2009.2.JNS08817
13. Sadaka, F, Jadhav, A, Miller, M, Saifo, A, O’Brien, J, Trottier, S, et al. Is it possible to recover from traumatic brain injury and a Glasgow coma scale score of 3 at emergency department presentation? Am J Emerg Med. (2018) 36:1624–6. doi: 10.1016/j.ajem.2018.01.051
14. Kuo, JR, Lo, CJ, Lu, CL, Chio, CC, Wang, CC, and Lin, KC. Prognostic predictors of outcome in an operative series in traumatic brain injury patients. J Formos Med Assoc. (2011) 110:258–64. doi: 10.1016/S0929-6646(11)60038-7
15. Berry, C, Ley, EJ, Tillou, A, Cryer, G, Margulies, DR, and Salim, A. The effect of gender on patients with moderate to severe head injuries. J Trauma. (2009) 67:950–3. doi: 10.1097/TA.0b013e3181ba3354
16. Cone, JT, Benjamin, ER, Alfson, DB, and Demetriades, D. Isolated severe blunt traumatic brain injury: effect of obesity on outcomes. J Neurosurg. (2020) 134:1667–74. doi: 10.3171/2020.3.JNS193458
17. Brennan, PM, Murray, GD, and Teasdale, GM. Simplifying the use of prognostic information in traumatic brain injury. Part 1: the GCS-pupils score: an extended index of clinical severity. J Neurosurg. (2018) 128:1612–20. doi: 10.3171/2017.12.JNS172780
18. Eisenberg, HM, Gary, HE, Aldrich, E, Saydjari, C, Turner, B, Foulkes, MA, et al. Initial CT findings in 753 patients with severe head injury. A report from the NIH traumatic coma data Bank. J Neurosurg. (1990) 73:688–98. doi: 10.3171/jns.1990.73.5.0688
19. Kuo, JR, Chou, TC, and Chio, CC. Coagulopathy as a parameter to predict the outcome in head injury patients–analysis of 61 cases. J Clin Neurosci. (2004) 11:710–4. doi: 10.1016/j.jocn.2003.10.011
20. Liu, C, Xie, J, Xiao, X, Li, T, Li, H, Bai, X, et al. Clinical predictors of prognosis in patients with traumatic brain injury combined with extracranial trauma. Int J Med Sci. (2021) 18:1639–47. doi: 10.7150/ijms.54913
21. Tu, KC, Eric Nyam, TT, Wang, CC, Chen, NC, Chen, KT, Chen, CJ, et al. A computer-assisted system for early mortality risk prediction in patients with traumatic brain injury using artificial intelligence algorithms in emergency room triage. Brain Sci. (2022) 12:612. doi: 10.3390/brainsci12050612
22. Bullard, MJ, Musgrave, E, Warren, D, Unger, B, Skeldon, T, Grierson, R, et al. Revisions to the Canadian emergency department triage and acuity scale (CTAS) guidelines 2016. CJEM. (2017) 19:S18–27. doi: 10.1017/cem.2017.365
23. Ng, CJ, Yen, ZS, Tsai, JC, Chen, LC, Lin, SJ, Sang, YY, et al. TTAS national working group. Validation of the Taiwan triage and acuity scale: a new computerised five-level triage system. Emerg Med J. (2011) 28:1026–231. doi: 10.1136/emj.2010.094185
24. Brain Trauma Foundation. American Association of Neurological Surgery. Joint section in Neurotrauma and critical care: pupillary diameter and light reflex. J Neurotrauma. (2000) 17:583–90. doi: 10.1089/neu.2000.17.583
25. Zweig, MH, and Campbell, G. Receiver-operating characteristic (ROC) plots: a fundamental evaluation tool in clinical practice. Clin Chem. (1993) 39:561–77. doi: 10.1093/clinchem/39.4.561
26. Dell, KC, Grossner, EC, Staph, J, Schatz, P, and Hillary, FG. A population-based study of pre-existing health conditions in traumatic brain injury. Neurotrauma Rep. (2021) 2:255–69. doi: 10.1089/neur.2020.0065
27. Eaton, S, Cornwell, H, Hamilton-Giachritsis, C, and Fairchild, G. Resilience and young people’s brain structure, function and connectivity: a systematic review. Neurosci Biobehav Rev. (2022) 132:936–56. doi: 10.1016/j.neubiorev.2021.11.001
28. Hukkelhoven, CW, Steyerberg, EW, Rampen, AJ, Farace, E, Habbema, JDF, Marshall, LF, et al. Patient age and outcome following severe traumatic brain injury: an analysis of 5600 patients. J Neurosurg. (2003) 99:666–73. doi: 10.3171/jns.2003.99.4.0666
29. Lieberman, JD, Pasquale, MD, Garcia, R, Cipolle, MD, Mark Li, P, and Wasser, TE. Use of admission Glasgow coma score, pupil size, and pupil reactivity to determine outcome for trauma patients. J Trauma. (2003) 55:437–43. doi: 10.1097/01.TA.0000081882.79587.17
30. Andishgar, A, Rismani, M, Bazmi, S, Mohammadi, Z, Hooshmandi, S, Kian, B, et al. Developing practical machine learning survival models to identify high-risk patients for in-hospital mortality following traumatic brain injury. Sci Rep. (2025) 15:5913. doi: 10.1038/s41598-025-89574-0
31. Li, J, Jin, M, and Yang, J. Enhanced prognostic accuracy in severe TBI: a comprehensive nomogram analysis. Neurochirurgie. (2025) 71:101597. doi: 10.1016/j.neuchi.2024.101597
Keywords: traumatic brain injury, mortality, emergency room triage, GCS 3, pupillary reaction, pupil size
Citation: Eric Nyam T-T, Tu K-C, Kuo Y-H, Wang C-C, Liu C-F, Liao J-C and Kuo C-L (2025) Age and pupil size: key predictors of mortality in traumatic brain injury patients with GCS 3. Front. Neurol. 16:1536421. doi: 10.3389/fneur.2025.1536421
Received: 28 November 2024; Accepted: 26 March 2025;
Published: 04 April 2025.
Edited by:
Jin Lu, Shanghai Jiao Tong University, ChinaReviewed by:
Leonardo de Macedo Filho, Penn State Milton S. Hershey Medical Center, United StatesCopyright © 2025 Eric Nyam, Tu, Kuo, Wang, Liu, Liao and Kuo. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Ching-Lung Kuo, a3VvamlubnJ1bmdAZ21haWwuY29t; Jen-Chieh Liao, Z2F3YXR3aW5mYWNlQGdtYWlsLmNvbQ==
†These authors have contributed equally to this work
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.