
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Med. , 25 February 2025
Sec. Healthcare Professions Education
Volume 12 - 2025 | https://doi.org/10.3389/fmed.2025.1511405
This article is part of the Research Topic Widening Participation and Access to Medicine as a Career View all articles
 Celeste Coler1*
Celeste Coler1* Kareena Patel1
Kareena Patel1 A. J. Balatico2
A. J. Balatico2 Kumhee Ro3
Kumhee Ro3 Joshua Villarreal4
Joshua Villarreal4 Nora Coronado1
Nora Coronado1 Estell Williams5
Estell Williams5Introduction: Health profession enrichment programs for underrepresented minority students are crucial to supporting students’ interest in healthcare careers and improving preparedness for important academic and professional milestones. Doctor for a Day, an enrichment program at the University of Washington School of Medicine, hosts monthly events where underrepresented kindergarten-12th grade students are exposed to careers in medicine by healthcare professionals from diverse backgrounds.
Methods: This study investigates to what extent participation in Doctor for a Day programming improves self-efficacy using a survey study of 958 students who attended at least one Doctor for a Day event between 2017 and 2023.
Results: Using an evaluation tool composed of six questions, our results demonstrate that participation in Doctor for a Day programming increases self-efficacy and interest in medicine as a career. Analysis of these results found significant differences in responses based on grade level, with students in high school demonstrating the largest improvement in self-efficacy.
Discussion: These findings underscore the value of such enrichment programs and offer insights for the development of similar initiatives.
A diverse healthcare workforce is critical to improving the quality of care offered to diverse populations (1, 2). This is supported by a growing body of evidence that highlights the connection between increased diversity among healthcare professionals and the enhanced delivery of culturally appropriate care to diverse patient populations (1, 3–8). While the racial and socioeconomic diversity in many healthcare professions has improved in recent years, students who are the first in their family to attend college and those from racially and ethnically minoritized groups, rural regions, and low socioeconomic backgrounds remain grossly underrepresented across the healthcare workforce (9, 10). For example, in the last decade, Black and Latinx individuals have comprised only 5 and 5.8% of the physician workforce despite representing 12.8 and 18.4% of the general United States population, respectively, (10). In 2022, the National Nursing Workforce Survey reported that 6.2% of registered nurses identify as Black or African American and 6.9% identify as Latinx (11). The United States Bureau of Labor Statistics reported similar disparities in 2022 among dentists, physical therapists, and occupational therapists (12). In terms of socioeconomic representation, 25% of medical students report parental income in the top 5% of United States households while students of families in the lowest quintile make up only 6% of medical students (13).
The explanation for these disparities is multifactorial and includes challenges due to systemic and institutional racism, inadequate or biased career advising, high costs of education, and difficulty accessing required courses (14–17). The disproportionately low number of physicians from backgrounds underrepresented in medicine also contributes to fewer opportunities for race-concordant mentorship among underrepresented youth, trainees, and faculty (18, 19). This is particularly concerning, as research has consistently shown that race-concordant mentorship is important for learning and professional development, and can even inform the medical specialty students ultimately pursue (20–22). Furthermore, race-concordant mentorship has been shown to minimize perceived challenges and address feelings of isolation (23). Enrichment programs for students traditionally underrepresented in medicine help overcome these barriers to medicine by providing science education, clinical exposure, and race-concordant mentorship. They also represent an evidence-based approach to promoting health equity and matriculating diverse student populations into healthcare professional training programs (24).
There is tremendous variation between pre-health enrichment programs nationwide. Parsons et al.’s review of physician pipeline and pathway programs highlights the diversity of current enrichment initiatives, which target various age groups, help with the development of different skill sets, and vary in time commitment. Some programs are short-term workshops (e.g., mock interviews, application workshops, financial literacy seminars, sample lectures), while others require longitudinal engagement (e.g., standardized test preparation, residential summer programs). These programs also employ a range of instructional methods, including problem-based learning, role-playing, and hands-on didactics (25).
There are various ways to evaluate enrichment programming, each offering unique insights into program effectiveness and impact. One common method of evaluation is assessing changes in self-efficacy, which is defined as one’s belief in their ability to achieve a goal and overcome challenges. In recent years, the construct of self-efficacy has become increasingly used to evaluate health profession enrichment programs (22, 26), as it has been shown that increased self-efficacy is associated with greater resilience in the face of academic challenges, increased likelihood to take on challenging tasks, and increased preparedness for a healthcare career (26–28). Social theories such as Bandura’s social cognitive theory also propose that student beliefs about personal capabilities may play a role in future choices such as career decisions (29, 30). Additional evaluation methods involve assessing changes in academic performance, skill development, or participant engagement. Research indicates that many enrichment programs linked to improvements in grade point average, retention rates, academic and research knowledge, as well as personal and professional growth (25, 31–36).
University of Washington’s Doctor for A Day (DFAD) is an enrichment program for kindergarten-12th grade (k-12) students traditionally underrepresented in health careers that aims to address disparities within the healthcare workforce and introduce youth to healthcare careers. The objective of this study is to determine whether participation in Doctor for a Day increases participants’ self-efficacy toward a career in medicine.
DFAD was designed to address barriers that underrepresented students face when exploring careers in healthcare. DFAD provides mentorship, opportunities to develop professional and interpersonal skills, knowledge on applying to graduate biomedical programs, and exposure to scientific topics relevant to medical careers. In DFAD’s monthly event, students from backgrounds traditionally underrepresented in health careers spend an afternoon engaging in hands-on activities such as suturing, physical exam skills, and ultrasound, led by medical students, residents, and faculty from various health specialties. Students also learn about disparities in healthcare and innovative solutions to the current challenges in medicine. Each event focuses on a specific organ system or disease process, providing variety for students who choose to attend multiple events.
The DFAD model is novel in its approach, in that it utilizes service learning to provide mentorship at multiple levels. Our curriculum allows students to interact and learn from individuals from diverse backgrounds who are at various points in their training and medical careers. Additionally, medical students learn from faculty, fellows, and residents as they work together to develop informative and interactive workshops. Attendings, residents, and fellows also benefit by giving back to local communities, further strengthening their community connections. Not only is learning facilitated at all levels, but inter-professionalism is emphasized through the representation of diverse healthcare careers and specialties. This creates a cycle of giving, learning, trust, and community building that has a far-reaching impact.
All Washington State k-12 students are eligible to participate in DFAD programming. K-12 students include students between the ages of 5–18. All participants participate in the same workshops regardless of age, and students are not separated based on age or grade level. Many of the participants are affiliated with one of DFAD’s community partners, including Gear Up, College Success Foundation, Spin Girls, Rainier Scholars, Africatown Center for Excellence and Innovation, Boys and Girls Club, Young Men’s Christian Association, and multiple schools and school districts across Washington State. Community partnerships are critical to DFAD because they help facilitate information sharing about specific community needs to best support individual and group learning and help with the recruitment and transportation of students.
Many healthcare careers are represented among the volunteers including medical students, residents, attendings, and allied health professionals (i.e., physical and occupational therapists, respiratory therapists, etc.). Volunteers are responsible for leading small cohorts of students through hands-on activities and answering students’ questions during panel discussions at each event. These interactive activities are meant to provide insight into a healthcare field, medical specialty, or disease process and introduce students to the interdisciplinary nature of healthcare.
Immediately following participation in a DFAD event, participants complete an anonymous post-participation survey developed by researchers from Seattle University and the University of Washington that assesses changes in self-efficacy and attitudes towards healthcare careers, participant demographics, and program and curricular feedback (Supplementary material S1).
The instrument used here was developed to measure the construct of self-efficacy within the domains of “understanding” and “ability.” Understanding was measured using the statements “I better understand what it takes to go to a medical or other health care professional school,” “I better understand what a doctor does,” and “I better understand what other health care professionals (e.g., nurses, dentists, PT and OT, etc.) do.” Ability was measured using the statements “I am more likely to go to college,” “I am more likely to pursue a career in the health care professions (e.g., doctor, nurse, dentist, etc.),” “I feel that having a career as a healthcare professional 116 is an achievable goal for me”. Each question response used a 5-point Likert scale.
In the survey, students also reported their race, gender identity, and grade level. Students between grades k-5 (elementary school) were between the ages of 5–9, students between grades 6–8 (middle school) were between the ages of 10–14, and students between grades 9–12 (high school) were between the ages of 15–18.
This study was deemed exempt by the University of Washington’s Institutional Review Board because participants incurred minimal risk. Informed consent from parents and legal guardians and assent from all students was obtained during registration for the workshop and in the post-participation survey.
Statistical analysis of demographic data including frequencies and means were performed on survey responses from 2017 to 2023 using SPSS v.24. Statistical analysis of self-efficacy Likert-score was conducted using two-sample t-tests and ANOVA tests. Effect sizes were expressed as Hedges’s g. Significance was denoted by p < 0.05.
Between 2017 and 2023, 958 students attended at least one of 29 DFAD events and completed a post-participation survey (Table 1). Of the 958 students, 26.8% were Asian, 34% were Black or African American, 16.4% were Latinx/Hispanic, 3.4% were Middle Eastern, 4.4% were mixed-race, 1% were American Indian or Alaska Native, 5.7% were white, and 8.8% did not disclose. Among all participants, 0.3% were in college, 73.4% were in high school, 22.8% were in middle school, 4.2% were in elementary school, and 0.4% did not disclose. Additionally, 76.6% identified as female and 21.2% identified as male. Additional participant demographics were recorded, including the level of parent education and the use of free or reduced lunch programs (Supplementary material S2).
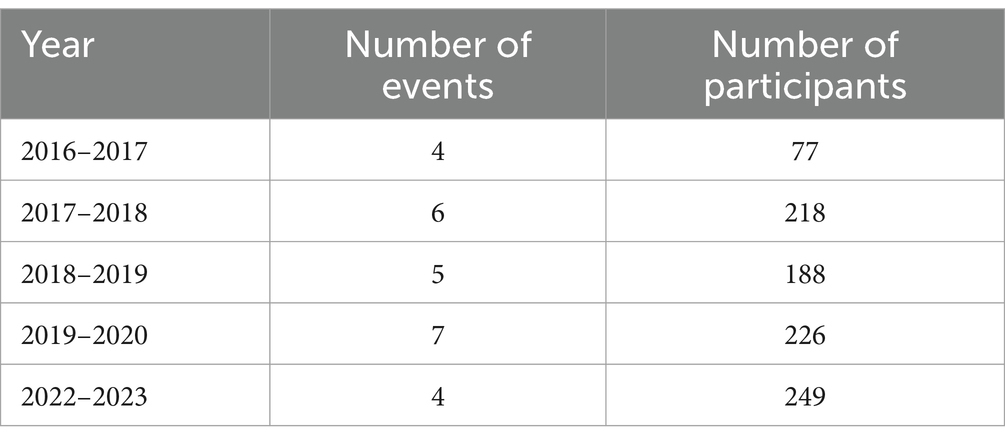
Table 1. Workshops hosted from the 2016–2017 school year to 2022–2023 school year not including virtual events hosted during the COVID-19 pandemic.
Likert scales were used to record the responses to six questions assessing students’ perceived ability, understanding, and interest in healthcare professions following participation in DFAD programming (Figure 1). 89% agreed or strongly agreed with the statement “I am more likely to go to college,” 76% agreed or strongly agreed with the statement “I am more likely to pursue a career in the health care professions (e.g., doctor, nurse, dentist, etc.),” 82% agreed or strongly agreed with the statement “I feel that having a career as a health care professional is an achievable goal for me,” 89% agreed or strongly agreed with the statement “I better understand what it takes to go to a medical or other health care professional school,” 89% agreed or strongly agreed with the statement “I better understand what a doctor does,” and 84% agreed or strongly agreed with the statement “I better understand what other health care professionals (e.g., nurses, dentists, physical therapists and occupational therapists, etc.) do.”
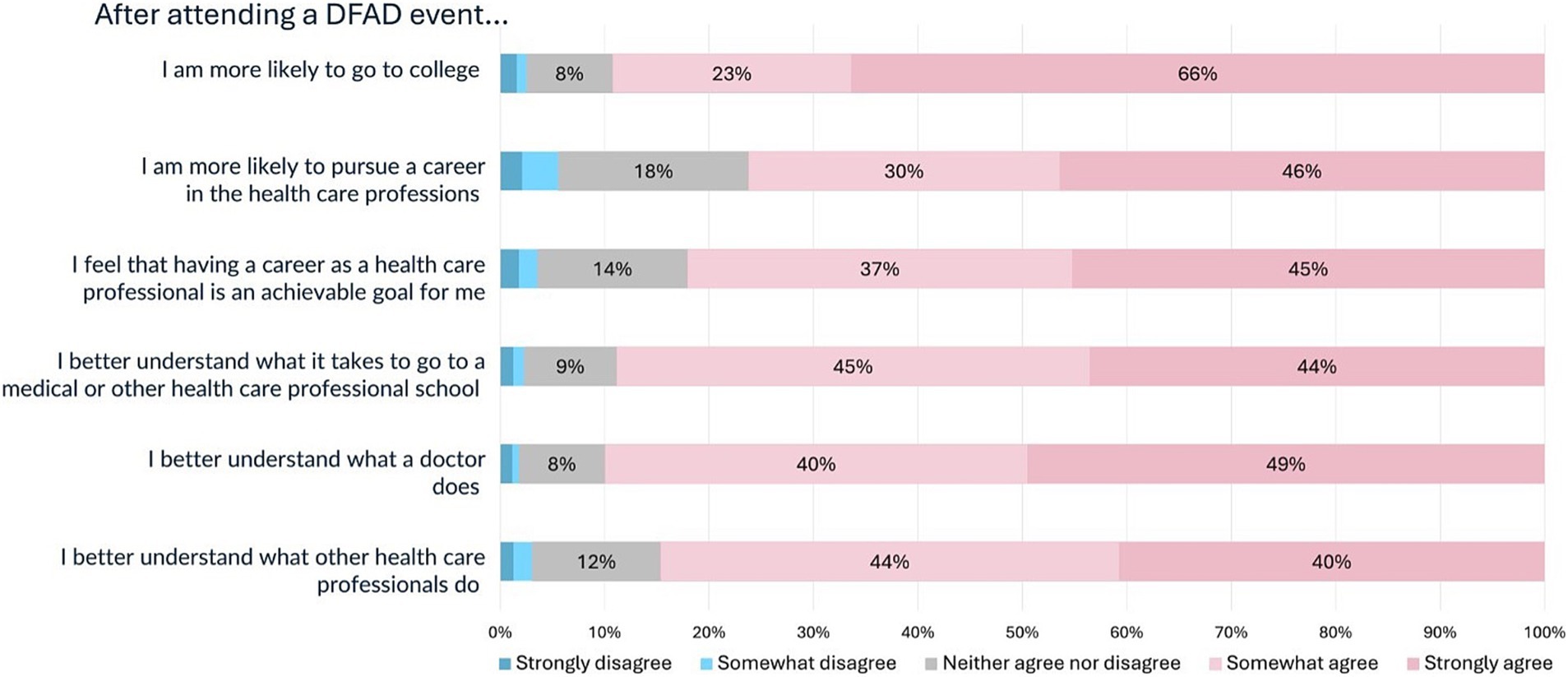
Figure 1. Likert-scale responses to questions evaluating self-efficacy after attending a DFAD event.
ANOVA tests showed that there were significant differences in responses by age for the following questions: “I am more likely to pursue a career in the health professions” with a small effect size between the elementary and high school groups (Hedge’s g = 0.44), “I better understand what it takes to go to a medical or other health care professional school” with a small effect size between the elementary vs. high school groups (Hedge’s g = 0.40), and “I better understand what other healthcare professionals (e.g., nurses, dentists, physical therapists, occupational therapists) do” (p < 0.001) with a small effect size between the middle vs. high school groups (Hedge’s g = 0.30) (Table 2).
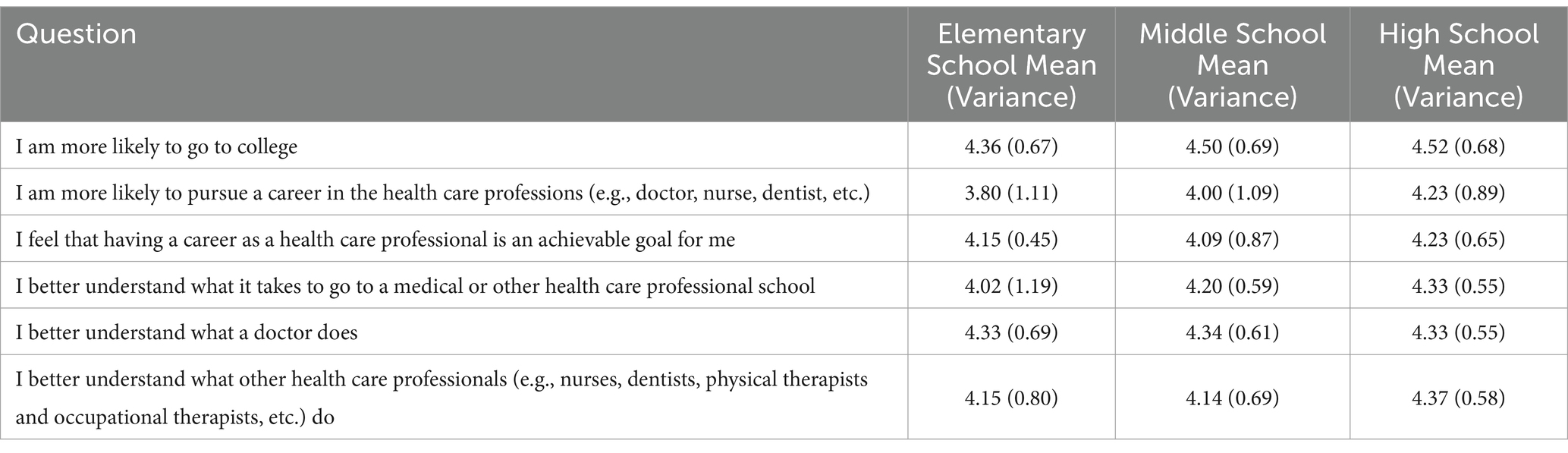
Table 2. Self-efficacy questionnaire by grade level (elementary school: ages 5–9, middle school: ages 10–14, high school: ages 15–18).
Race was not associated with a significant difference in the response to “I am more likely to go to college” (F = 1.51, p = 0.17), “I am more likely to pursue a career in the health care professions (e.g., doctor, nurse, dentist, etc.)” (F = 1.17, p = 0.32), “I feel that having a career as a health care professional is an achievable goal for me” (F = 0.96, p = 0.45), “I better understand what it takes to go to a medical or other health care professional school” (F = 0.81, p = 0.56), “I better understand what a doctor does” (F = 1.02, p = 0.41), and “I better understand what other health care professionals (e.g., nurses, dentists, physical therapists, and occupational therapists, etc.) do” (F = 1.94, p = 0.072). Therefore, race did not significantly affect changes in self-efficacy (Table 3).
Survey responses demonstrated that DFAD programming is utilized by underrepresented minority students with multiple social and economic barriers to healthcare careers. Over half of the DFAD participants received free and reduced lunch, a proxy for low socioeconomic status (37, 38). Moreover, a third of students had parents with a high school diploma as their most advanced degree, and half of the students did not know someone with a job in healthcare. These findings indicate that many students attending DFAD events may lack the necessary support networks and guidance to navigate graduate education and careers in healthcare.
Additionally, responses to the six self-efficacy questions suggest that participation in DFAD programming increases students’ self-efficacy, interest in medicine as a career, and understanding of different healthcare careers. These findings are consistent with similar enrichment programs including the Access Summer Scholars Program at the University of Pennsylvania which showed an improved understanding of the physician identity and increased preparedness for medical school following program participation (39). The Vanderbilt Summer Science Academy similarly found that program participation was associated with an improved understanding of post-graduate programs and a greater sense of belonging in the science and medical community (40).
To date, few studies assess how student age or grade may influence program effectiveness. In this study, grade level appeared to play an important role in influencing perceived self-efficacy after DFAD attendance despite all students receiving the same curriculum regardless of age. Our findings suggest that DFAD participation resulted in the greatest increase in self-efficacy for high school students compared to middle and elementary school students. Although self-efficacy was greatest among high school students, research has also shown that without early intervention with enrichment programming in elementary school, underrepresented students may lose interest and confidence in science and math by their teenage years, underscoring the importance of enrichment programs that include elementary-aged students (41). When designing curriculums for DFAD events, volunteers must balance the needs of younger students, who benefit most from programs that foster interest and self-confidence in the sciences, with those of older students, who benefit from programs that prepare them academically for challenging science courses (41).
Very few studies have assessed whether the effect of an enrichment program differs by student race. An evaluation of the Center for Disease Control and Prevention Public Health Scholars Program found a difference in program influence by racial and ethnic background, however, this study does not include whether these differences were statistically significant (42). By demonstrating that there were no statistically significant differences in survey responses by self-reported race, this study addresses a critical knowledge gap.
Our assessment of DFAD programming would benefit from pre-participation surveys assessing baseline interest in healthcare careers and self-efficacy, as well as long-term follow-up. Although the anonymity of DFAD’s surveys makes long-term follow-up challenging, long-term follow-up is a valuable way of evaluating DFADs’ influence on high school, undergraduate, and graduate school matriculation and ultimate career choice.
In the future, conducting interviews and focus groups with current and past participants may allow for a more nuanced exploration of the factors influencing participants’ experiences, motivations, challenges, and perceptions. Qualitative research may also benefit our assessment of DFAD by contextualizing and validating quantitative findings. Additionally, future surveys should collect information on the number of DFAD events students have participated in to determine whether consistent participation has a greater impact on the behaviors and beliefs being studied. We have adapted our surveys for the 2024–2025 academic year to collect this information. In addition, the adapted study is being reviewed using exploratory factor analysis to test for the reliability of the adapted survey questions.
Finally, studies have shown that volunteering can decrease burnout and stress and improve the quality of life among healthcare professionals and trainees (43–45). Still, data on the effect of enrichment programs on volunteers’ burnout is limited. Since DFAD programming supports mentorship between volunteers at various points in their healthcare professional training, assessing the impact of DFAD on volunteers’ job satisfaction, burnout, and quality of life may address a large gap in the literature.
One limitation of this study is the use of an evaluation tool that has not yet been validated, which may affect the reliability of the findings. Without formal validation, it is unclear whether the evaluation tool consistently measures the intended constructs. Future program evaluation should prioritize the use of a validated tool to enhance the generalizability of the results.
This cohort study is also limited due to the lack of information about the participants’ baseline characteristics prior to participating in DFAD programming. The distribution of pre-participation surveys that assess baseline interest in healthcare professions and self-efficacy would provide useful information regarding the impact of DFAD on self-efficacy and attitudes toward healthcare careers.
This study adds to the growing literature on the impact of enrichment programming on self-efficacy among underrepresented students interested in medicine. The findings of this study demonstrate that participation in DFAD increases participants’ self-efficacy toward a career in medicine, with high school students showing the greatest improvement in their self-efficacy. These findings highlight the program’s potential to support the career aspirations of underrepresented students interested in medicine and improve access to medicine as a career.
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding author.
The studies involving humans were approved by University of Washington Institutional Review Board. The studies were conducted in accordance with the local legislation and institutional requirements. Written informed consent for participation in this study was provided by the participants’ legal guardians/next of kin.
CC: Writing – original draft, Writing – review & editing. KP: Formal analysis, Writing – original draft, Writing – review & editing. AB: Writing – original draft, Writing – review & editing. KR: Writing – original draft, Writing – review & editing. JV: Writing – original draft, Writing – review & editing. NC: Writing – original draft, Writing – review & editing. EW: Funding acquisition, Writing – original draft, Writing – review & editing.
The author(s) declare that financial support was received for the research, authorship, and/or publication of this article. This work was supported by funding from anonymous donations to the DFAD program through UW Medicine Advancement and the Cambia Health Foundation Grant awarded through the Foundation’s Healthy People, Healthy Communities funding track.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The author(s) declare that no Gen AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fmed.2025.1511405/full#supplementary-material
1. Snyder, JE, Upton, RD, Hassett, TC, Lee, H, Nouri, Z, and Dill, M. Black representation in the primary care physician workforce and its association with population life expectancy and mortality rates in the US. JAMA Netw Open. (2023) 6:e236687. doi: 10.1001/jamanetworkopen.2023.6687
2. Wilbur, K, Snyder, C, Essary, AC, Reddy, S, Will, KK, and Saxon, M. Developing workforce diversity in the health professions: a social justice perspective. Health Prof Educ. (2020) 6:222–9. doi: 10.1016/j.hpe.2020.01.002
3. Hoever, IJ, van Knippenberg, D, van Ginkel, WP, and Barkema, HG. Fostering team creativity: perspective taking as key to unlocking diversity’s potential. J Appl Psychol. (2012) 97:982–96. doi: 10.1037/a0029159
4. Gomez, LE, and Bernet, P. Diversity improves performance and outcomes. J Natl Med Assoc. (2019) 111:383–92. doi: 10.1016/j.jnma.2019.01.006
5. Gonzalvo, JD, and Sharaya, NH. Language concordance as a determinant of patient outcomes in a pharmacist-managed cardiovascular risk reduction clinic. J Pharm Pract. (2016) 29:103–5. doi: 10.1177/0897190014544790
6. Greenwood, BN, Hardeman, RR, Huang, L, and Sojourner, A. Physician-patient racial concordance and disparities in birthing mortality for newborns. Proc Natl Acad Sci USA. (2020) 117:21194–200. doi: 10.1073/pnas.1913405117
7. Shen, MJ, Peterson, EB, Costas-Muñiz, R, Hernandez, MH, Jewell, ST, Matsoukas, K, et al. The effects of race and racial concordance on patient-physician communication: a systematic review of the literature. J Racial Ethn Health Disparities. (2018) 5:117–40. doi: 10.1007/s40615-017-0350-4
8. Ma, A, Sanchez, A, and Ma, M. The impact of patient-provider race/ethnicity concordance on provider visits: updated evidence from the medical expenditure panel survey. J Racial Ethn Health Disparities. (2019) 6:1011–20. doi: 10.1007/s40615-019-00602-y
9. Majerczyk, D, Behnen, EM, Weldon, DJ, Kanbar, R, Hardy, YM, Matsuda, SK, et al. Racial, ethnic, and sex diversity trends in health professions programs from applicants to graduates. JAMA Netw Open. (2023) 6:e2347817. doi: 10.1001/jamanetworkopen.2023.47817
10. Association of American Medical Colleges (2019). Diversity in medicine: facts and figures 2019. Available at: https://www.aamc.org/data-reports/workforce/report/diversity-medicine-facts-and-figures-2019 (Accessed September 17, 2024).
11. Smiley, RA, Allgeyer, RL, Shobo, Y, Lyons, KC, Letourneau, R, Zhong, E, et al. The 2022 National Nursing Workforce Survey. J Nurs Regul. (2023) 14:S1–S90. doi: 10.1016/S2155-8256(23)00047-9
12. U.S. Bureau of Labor Statistics (2024). Employed persons by detailed occupation, sex, race, and Hispanic or Latino ethnicity. Available at: https://www.bls.gov/cps/cpsaat11.htm (Accessed November 12, 2024).
13. Association of American Medical Colleges (2018). An updated look at the economic diversity of U.S. Medical students [internet]. (Analysis in Brief). Available st: https://www.aamc.org/media/9596/download?attachment (Accessed September 17, 2024).
14. Sandino, AH, and Rowe, DJ. Students from underrepresented racial and ethnic groups entering the dental hygiene profession. J Dent Educ. (2014) 78:465–72. doi: 10.1002/j.0022-0337.2014.78.3.tb05696.x
15. Joseph, J, Dao, D, Hwang, SM, Dotzler, SM, Chesak, SS, Weiskittel, TM, et al. Perceptions of barriers and facilitators to becoming a medical professional among underrepresented undergraduate and Postbaccalaureate learners. Mayo Clin Proc Innov Qual Outcomes. (2021) 5:347–58. doi: 10.1016/j.mayocpiqo.2021.01.003
16. Rao, V, and Flores, G. Why aren’t there more African-American physicians? A qualitative study and exploratory inquiry of African-American students’ perspectives on careers in medicine. J Natl Med Assoc. (2007) 99:986–93.
17. Barr, DA, Gonzalez, ME, and Wanat, SF. The leaky pipeline: factors associated with early decline in interest in premedical studies among underrepresented minority undergraduate students. Acad Med J Assoc Am Med Coll. (2008) 83:503–11. doi: 10.1097/ACM.0b013e31816bda16
18. Yehia, BR, Cronholm, PF, Wilson, N, Palmer, SC, Sisson, SD, Guilliames, CE, et al. Mentorship and pursuit of academic medicine careers: a mixed methods study of residents from diverse backgrounds. BMC Med Educ. (2014) 14:26. doi: 10.1186/1472-6920-14-26
19. Ramanan, RA, Taylor, WC, Davis, RB, and Phillips, RS. Mentoring matters. Mentoring and career preparation in internal medicine residency training. J Gen Intern Med. (2006 Apr) 21:340–5. doi: 10.1111/j.1525-1497.2006.00346.x
20. Pershad, AR, Kidwai, MS, Lugo, CA, Lee, E, Tummala, N, and Thakkar, P. Factors influencing underrepresented medical students’ career choice in surgical subspecialties. Laryngoscope. (2024) 134:1498–506. doi: 10.1002/lary.31094
21. Penaloza, NG, Kassandra, EZA, Does, S, Washington, SL, Tandel, MD, Braddock, CH, et al. Someone like me: an examination of the importance of race-concordant mentorship in urology. Urology. (2023) 171:41–8. doi: 10.1016/j.urology.2022.08.059
22. Cheng, JL, Park, LS, Dibble, EH, Baird, GL, George, PF, and Ahn, SH. Diversity in interventional radiology: survey of medical student interest with focus on women and members of underrepresented in medicine racial and ethnic groups. Clin Imaging. (2023) 103:109964. doi: 10.1016/j.clinimag.2023.06.026
23. Butts, GC, Hurd, Y, Palermo, AGS, Delbrune, D, Saran, S, Zony, C, et al. Role of institutional climate in fostering diversity in biomedical research workforce: a case study. Mt Sinai J Med N Y. (2012) 79:498–511. doi: 10.1002/msj.21323
24. Grbic, D, Poll-Hunter, N, Felida, N, and Andriole, DA. Association of Summer College Academic Enrichment Program Participation with Medical Student Diversity and Intent to practice in underserved areas. JAMA Netw Open. (2021) 4:e2034773. doi: 10.1001/jamanetworkopen.2020.34773
25. Parsons, M, Caldwell, MT, Alvarez, A, Davenport, D, Gallegos, M, Landry, A, et al. Physician pipeline and pathway programs: an evidence-based guide to best practices for diversity, equity, and inclusion from the Council of Residency Directors in emergency medicine. West J Emerg Med. (2022) 23:514–24. doi: 10.5811/westjem.2022.2.54875
26. Cassidy, S. Resilience building in students: the role of academic self-efficacy. Front Psychol. (2015) 6:1781. doi: 10.3389/fpsyg.2015.01781
27. Jebram, L, and Harendza, S. Relationships between self-efficacy beliefs and personal factors in final-year medical students. BMC Med Educ. (2024) 24:1104. doi: 10.1186/s12909-024-06087-6
28. Yelorda, K, Bidwell, S, Fu, S, Miller, MO, Merrell, SB, Koshy, S, et al. Self-efficacy toward a healthcare career among minority high school students in a surgical pipeline program: a mixed methods study. J Surg Educ. (2021) 78:1896–904. doi: 10.1016/j.jsurg.2021.04.010
29. Bandura, A. Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev. (1977) 84:191–215. doi: 10.1037/0033-295X.84.2.191
30. Bandura, A. (2002). Social foundations of thought and action. In: The Health Psychology reader [internet]. 1 Oliver’s Yard, 55 City Road, London EC1Y 1SP United Kingdom: SAGE Publications Ltd. p. 94–106. Available at: https://sk.sagepub.com/books/the-health-psychology-reader/n6.xml (Accessed November 19, 2024).
31. Stephenson-Hunter, C, Strelnick, AH, Rodriguez, N, Stumpf, LA, Spano, H, and Gonzalez, CM. Dreams realized: a long-term program evaluation of three summer diversity pipeline programs. Health Equity. (2021) 5:512–20. doi: 10.1089/heq.2020.0126
32. Bradford, BC, Beier, ME, and Oswald, FL. A Meta-analysis of university STEM summer bridge program effectiveness. CBE life. Sci Educ. (2021) 20:ar21. doi: 10.1187/cbe.20-03-0046
33. Kohut, OB, Wang, Z, Sanchez, RR, Rausch, JC, Nieto, A, and Minguez, MM. Assessing the impact of a 6-year health sciences enrichment program for underrepresented minority youth on healthcare workforce diversity, career path, and public health. Front Public Health. (2023) 11:1244593. doi: 10.3389/fpubh.2023.1244593
34. Hill, K, Raney, C, Jackson, K, Murdock, HM, Dawson, E, Hamilton, R, et al. A new way of evaluating effectiveness of URM summer pipeline programs. Adv Med Educ Pract. (2021) 12:863–9. doi: 10.2147/AMEP.S293744
35. Fritz, CDL, Press, VG, Nabers, D, Levinson, D, Humphrey, H, and Vela, MB. SEALS: an innovative pipeline program targeting obstacles to diversity in the physician workforce. J Racial Ethn Health Disparities. (2016) 3:225–32. doi: 10.1007/s40615-015-0131-x
36. Patel, SI, Rodríguez, P, and Gonzales, RJ. The implementation of an innovative high school mentoring program designed to enhance diversity and provide a pathway for future careers in healthcare related Fields. J Racial Ethn Health Disparities. (2015) 2:395–402. doi: 10.1007/s40615-015-0086-y
37. Taylor, C. The reliability of free school meal eligibility as a measure of socio-economic disadvantage: evidence from the millennium cohort study in Wales. Br J Educ Stud. (2018) 66:29–51. doi: 10.1080/00071005.2017.1330464
38. Nicholson, LM, Slater, SJ, Chriqui, JF, and Chaloupka, F. Validating adolescent socioeconomic status: comparing school free or reduced Price lunch with community measures. Spat Demogr. (2014) 2:55–65. doi: 10.1007/BF03354904
39. Zhou, C, Okafor, C, Hagood, J, and DeLisser, HM. Penn access summer scholars program: a mixed method analysis of a virtual offering of a premedical diversity summer enrichment program. Med Educ Online. (2021) 26:1905918. doi: 10.1080/10872981.2021.1905918
40. Oliver, KH, Keeton, C, Chalkley, R, and Bowman, E. Virtual Vanderbilt summer science academy highlighted the opportunity to impact early STEMM students career knowledge through narrative. PLoS One. (2021) 16:e0258660. doi: 10.1371/journal.pone.0258660
41. Valla, JM, and Williams, WM. Increasing achievement and higher-education representation of under-represented groups in science, technology, engineering, and mathematics fields: a review of current k-12 intervention programs. J Women Minorities Sci Eng. (2012) 18:21–53. doi: 10.1615/JWomenMinorScienEng.2012002908
42. Young, KH, Liburd, L, and Penman-Aguilar, A. An evaluation of a pipeline program to support diversity in the public health workforce: CDC undergraduate public health scholars (CUPS) program. Pedagogy Health Promot. (2021) 7:23S–35S. doi: 10.1177/23733799211047522
43. Metzger, T, Nguyen, N, Le, H, Havo, D, Ngo, K, Lee, S, et al. Does volunteering decrease burnout? Healthcare professional and student perspectives on burnout and volunteering. Front Public Health. (2024) 12:1387494. doi: 10.3389/fpubh.2024.1387494
44. Duncan, SA, Sperling, GL, Moy, MI, Hansen, R, Soudah, CK, Rodriguez, P, et al. Investigating the impact of community volunteerism on the mental health of medical students. J Med Educat Curri Develop. (2023) 10:23821205231191903. doi: 10.1177/23821205231191903
Keywords: diversity, self-efficacy, mentorship, healthcare, medicine, underrepresented, outreach
Citation: Coler C, Patel K, Balatico AJ, Ro K, Villarreal J, Coronado N and Williams E (2025) Doctor for a day: the impact of a health professions enrichment program on self-efficacy. Front. Med. 12:1511405. doi: 10.3389/fmed.2025.1511405
Received: 14 October 2024; Accepted: 13 February 2025;
Published: 25 February 2025.
Edited by:
Diantha Soemantri, University of Indonesia, IndonesiaReviewed by:
Ruth Strudwick, University of Suffolk, United KingdomCopyright © 2025 Coler, Patel, Balatico, Ro, Villarreal, Coronado and Williams. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Celeste Coler, Y2NvbGVyMjNAdXcuZWR1
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.