- 1Department of Infectious Diseases, The First Hospital of Lanzhou University, Lanzhou, Gansu, China
- 2The First School of Clinical Medicine, Lanzhou University, Lanzhou, Gansu, China
Streptococcus constellatus, recognized as a commensal bacterium, has the potential to induce severe infections in patients with immunodeficiency. Here, we reported a rare case of Streptococcus constellatus infection that manifested as gelatinous pleural effusion in a patient with HIV. Although the effusion was gelatinous and partially encapsulated, it was completely resolved with timely administration of antibiotics, thereby eliminating the necessity for thoracic drainage, urokinase injection, or surgical intervention.
Introduction
Streptococcus constellatus is found in various areas of the human body, such as the skin, nasopharynx, stomach, and intestines. When the immune system is compromised by various factors, Streptococcus constellatus can become pathogen. Patients infected with human immunodeficiency virus (HIV) are especially vulnerable to opportunistic infections due to chronic inflammation and T-cell dysfunction. Several cases have reported that HIV-positive patients present with brain abscesses (1), muscle abscesses (1), liver abscesses (2), and pleural effusions (3) attributed to Streptococcus constellatus.
Pleural fluid resulting from Streptococcus constellatus is predominantly purulent in nature and can be easily encapsulated (3). To the best of our knowledge, only one case reported that Streptococcus constellatus leaded to pleural fluid in patient with HIV, while the characteristics of fluid was milky white (3).
It is well known that jelly-like effusions primarily occur in the patients with malignant tumors, and these cases are challenging to treat and often resulting in a poor prognosis (4). There have been no documented cases of jelly-like effusions linked to Streptococcus constellatus. The case highlights the importance of identifying atypical clinical presentations, such as gelatinous pleural effusion, which may indicated an underlying bacterial infection.
Case description
A 58-year-old male patient was diagnosed with HIV approximately one year ago. He has been receiving antiretroviral therapy consisting of lamivudine, tenofovir disoproxil fumarate, and efavirenz. His medical history includes type 2 diabetes and a tooth extraction.
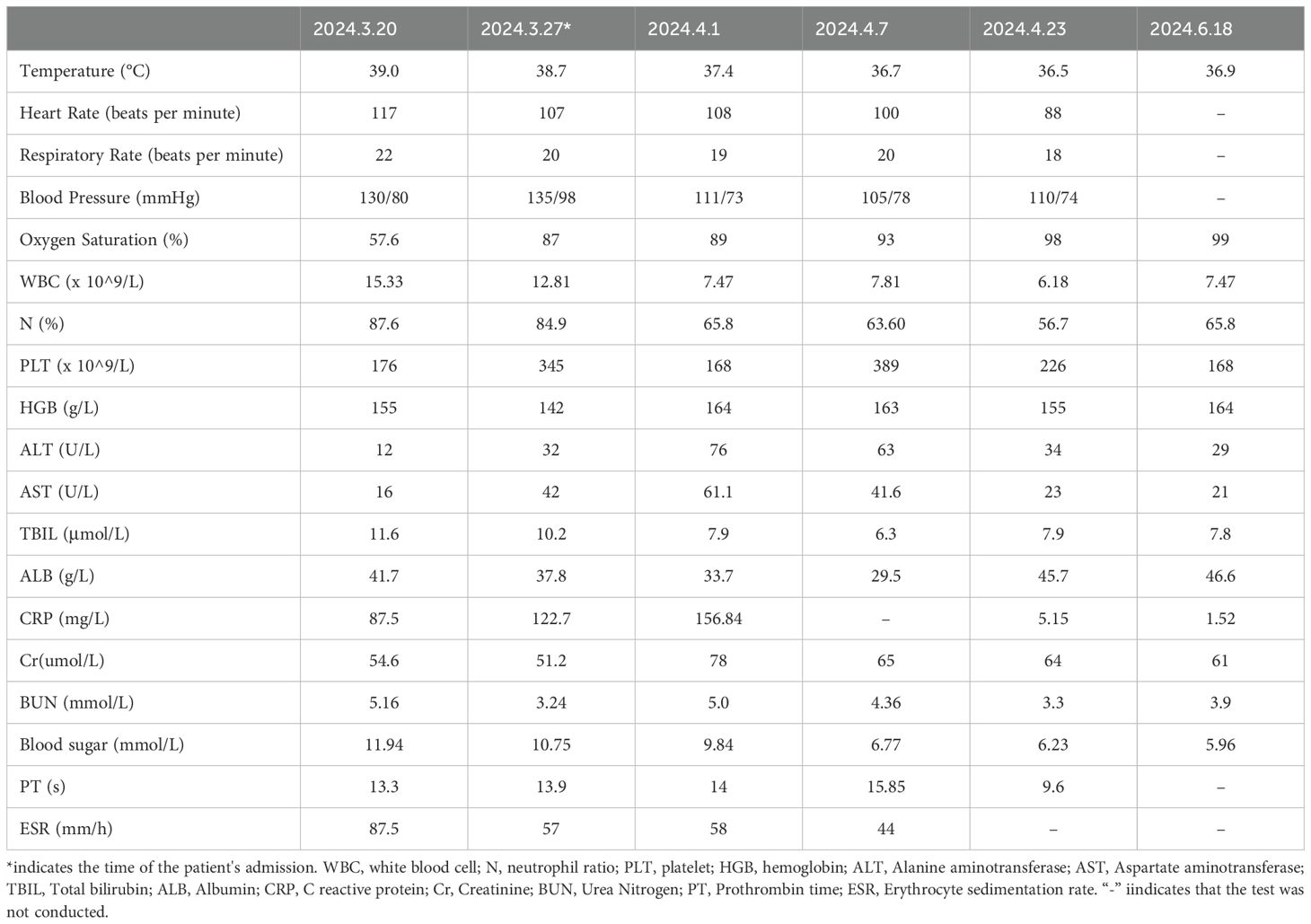
The patient was admitted to our hospital with hyperpyrexia, shortness of breath, chest pain, and chest tightness, symptoms that had persisted for seven days. The highest recorded body temperature was 39°C, without chills, cough, or expectoration. Upon admission, his vital signs were as follows: temperature 38.7°C, heart rate 107 beats per minute, respiratory rate 20 breaths per minute, blood pressure 135/98 mmHg, and oxygen saturation 87% on room air. Percussion of the left lung revealed dullness, and auscultation indicated absent breath sounds. The laboratory results were as follows: white blood cell (WBC) count was 12.81 x 10^9/L, neutrophil ratio was 84.9%, and lymphocyte ratio was 29.6%. C-reactive protein was 122.7 mg/L, and procalcitonin was 0.060 ng/mL. The erythrocyte sedimentation rate was 57 mm/h. Tumor markers, γ-interferon release test, and blood culture were negative. Ferritin level was 609.00 ng/mL. The CD4+ T cell count was 437 cells/µL, with a CD4/CD8 ratio of 0.56. Chest CT revealed pneumonia, left-sided pleural effusion, and partial encapsulation (Figures 1A, B). Approximately 50 mL of yellow, jelly-like pleural effusion was extracted from the left pleural cavity (Figure 1F). Effusion was sticky and difficult to remove. The results of the effusion analysis showed an erythrocyte count of 31,900 x 10^6/L, a WBC count of 46 x 10^6/L, a negative mucin test, a glucose level of 7.77 mmol/L, an LDH level of 1,266 U/L, and an adenosine deaminase level of 23.50 U/L. The pleural effusion culture, acid-fast staining, and tuberculosis bacteria GeneXpert tests were all negative. The metagenomic next-generation sequencing (mNGS) of the pleural effusion identified Streptococcus constellatus.
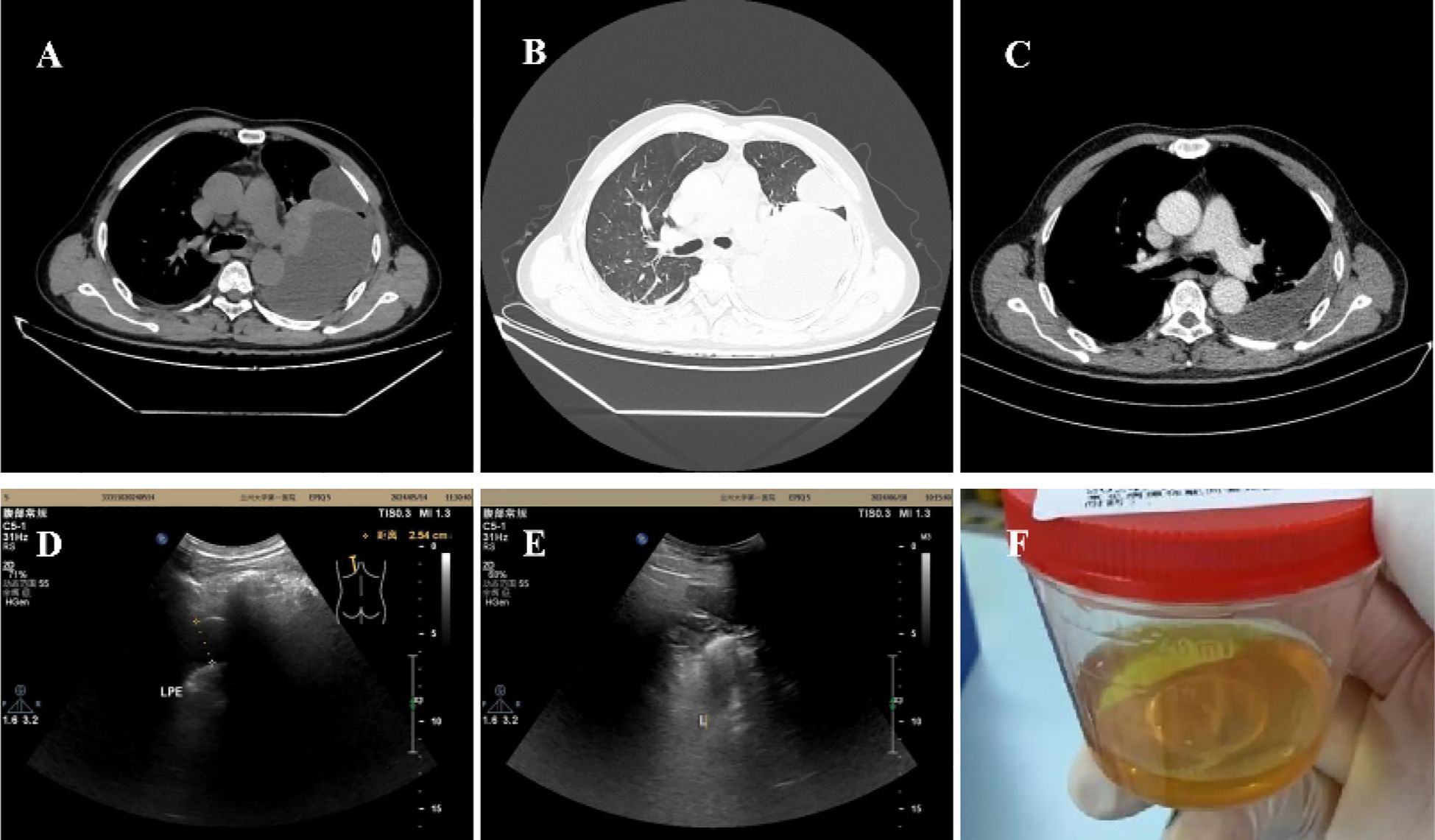
Figure 1. (A, B) On admission, CT showed a left-sided pleural effusion, partially encapsulated. (C) CT showed pleural effusion was signaficatlly decreased 15 days after treatment. (D) 30 days after discharge, ultrasound showed the left thoracic cavity (posterior axillary line, scapula level) had 10 mm and 25 mm pleural effusion, respectively. (E) Pleural effusion was completely absorbed 66days after discharge. (F) Jelly-like pleural fluid was withdrawn on admission.
The diagnoses were: 1. Pleural effusion, 2. Pneumonia, 3. AIDS, 4. Type 2 diabetes. Anti-infective treatment was piperacillin sodium and tazobactam sodium 4.5 g, administered intravenously every 12 hours. The symptoms were significantly relieved and CT showed that the pleural effusion had decreased significantly after therapy (Figure 1C). The patient was discharged from the hospital and continued medication treatment after 16 days. The antibiotics were adjusted to nemonoxacin malate tablets 0.5 g, taken once daily by mouth. The pleural fluid was gradually absorbed (Figure 1D). After 66 days post-discharge, a follow-up ultrasound showed that the pleural effusion had disappeared (Figure 1E). The changes in vital signs and laboratory indicators during the patient’s course of illness are presented in Table 1.
Discussion and conclusions
Streptococcus constellatus is considered as a pathogenic bacterium capable of causing abscesses, deep-seated inflammation, and vascular lesions, including brain abscesses (5), liver abscesses (6), pneumonia (7), lung abscesses (8), empyema (3), descending necrotizing mediastinitis (9), pelvic inflammatory disease (10), suppurative thrombophlebitis (11), venous sinus thrombosis (12), and secondary bone destruction (13). Infections caused by Streptococcus constellatus are diverse in nature and are strongly associated with compromised host immunity. The current case presented as pleural effusion attributed to Streptococcus constellatus, with the underlying medical condition being HIV.
It is essential to identify the nature of effusion to improve therapeutic outcomes. Typically, the appearance of effusion caused by Streptococcus constellatus is purulent, turbid, or milky white (3)and is prone to forming loculated effusions. However, the appearance of the pleural effusion in our case was jelly-like, which is not consistent with other patients. The jelly-like effusion primarily originates from malignant tumors, such as mesothelioma (4) and melanoma (14), and is occasionally found in infections caused by tuberculous bacilli (15, 16). The gelatinization of pleural fluid indicates a higher viscosity, primarily linked to the content of mucoproteins and hyaluronic acid in the effusion (15–19). Malignant cells may produce large amounts of mucin. Additionally, hyaluronic acid has been found in pleural effusions caused by malignant tumors and inflammatory pleural diseases (15–17, 19). Patients with pleural metastatic melanoma may develop pleural effusion (20). Here, we reported the first case of jelly-like effusion caused by a Streptococcus constellatus infection.
The pathogenicity of Streptococcus constellatus is also associated with the disruption of the barrier at the colonization site. Streptococcus constellatus may originate from the oral cavity, esophagus, stomach, hepatobiliary system, or urinary tract. The onset of this case may be linked to a history of tooth extraction.
The duration of antibiotic treatment is often prolonged due to the tendency of Streptococcus constellatus to cause deep infections. If pleural effusion is not treated promptly, it can worsen, leading to complications such as effusion encapsulation and even pleural adhesion. Thoracotomy or thoracoscopic surgery can significantly increase both the psychological and financial burden on patients. Early diagnosis and timely administration of sensitive antibiotics can simplify the treatment, reduce the duration of the illness and hospitalization, and enhance the cure rate. In our case, the pathogen was promptly identified using metagenomic next-generation sequencing (mNGS), and the patient received a prolonged course of the appropriate antibiotic. As a result, the patient’s pyothorax was successfully treated, avoiding more complex interventions such as thoracic drainage, urokinase injection, and surgery.
In summary, Streptococcus constellatus is a pathogenic bacterium that can cause pleural effusion in patients with HIV/AIDS, and this pleural effusion may present with gelatinous characteristics. Early diagnosis and a timely, complete course of antimicrobial therapy can effectively treat gelatinous pleural effusion and may help the need for surgery.
Data availability statement
The original contributions presented in the study are included in the article/supplementary material. Further inquiries can be directed to the corresponding author/s.
Ethics statement
Written informed consent was obtained from the individual(s) for the publication of any potentially identifiable images or data included in this article. Written informed consent was obtained from the participant/patient(s) for the publication of this case report.
Author contributions
ZY: Writing – original draft, Writing – review & editing, Formal Analysis, Funding acquisition. WX: Data curation, Formal Analysis, Writing – original draft. ZQ: Data curation, Methodology, Writing – original draft. XM: Formal Analysis, Writing – review & editing.
Funding
The author(s) declare that no financial support was received for the research and/or publication of this article.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Generative AI statement
The author(s) declare that no Generative AI was used in the creation of this manuscript.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Coll Crespo B, Pérez Bernalte RM, Alonso Villaverde Lozano C, Fernández Juliá R, Ballester Bastardie F, Masana Marín L. Disseminated infection due to Streptococcus constellatus in an HIV patient with negative viral load. Anales Med Intern (Madrid Spain: 1984). (2001) 18:660–1. doi: 10.4321/s0212-71992001001200016
2. Hsu SL, Wu CT, Chang YC, Fan CK, Lee YJ. Case report of an unusual hepatic abscess caused by Actinomyces odontolyticus in a patient with human immunodeficiency virus infection. BMC Infect Dis. (2021) 21:998. doi: 10.1186/s12879-021-06703-6
3. Yang HH, Li M, Yu Q, Liu Q, Liu M. Empyema caused by Streptococcus constellatus in a patient infected with HIV: a case report and literature review. AIDS Res Ther. (2024) 21:2. doi: 10.1186/s12981-023-00587-z
4. Ibnian AM, Khan OU, Chan R, Bangalore Lakshminarayana U, Kiran F, Abed S, et al. Gelatinous pleural effusion: A diagnostic challenge for pleural mesothelioma in an 80-year-old man. Am J Case Rep. (2023) 24:e941263. doi: 10.12659/AJCR.941263
5. Xiao K, Zhao D, Luo Y, Si Y. Streptococcus constellatus causing brain abscess identified by metagenomics next-generation sequencing. Surg Infections. (2022) 23:207–8. doi: 10.1089/sur.2021.338
6. Datta P, Mohi GK, Chander J, Attri AK. Streptococcus constellatus causing multiple liver abscesses: an elusive pathogen. Trop Doctor. (2018) 48:154–6. doi: 10.1177/0049475517721817
7. Navarro-Esteva J, Barbera-Colina DB, Gil-Lorenzo RM. Streptococcus constellatus pneumonia invading the chest wall: A rare presentation. Open Respir Archives. (2023) 5:100272. doi: 10.1016/j.opresp.2023.100272
8. Lin J, Zhang Y, Bao C, Lu H, Zhong Y, Huang C, et al. The clinical features and management of empyema caused by streptococcus constellatus. Infection Drug Resistance. (2022) 15:6267–77. doi: 10.2147/IDR.S382484
9. Guo J, Lin L, Zhou H, Yang W, Shi S, et al. Descending necrotizing mediastinitis caused by Streptococcus constellatus: A case report and review of the literature. Medicine. (2023) 102:e33458. doi: 10.1097/MD.0000000000033458
10. Mora-Palma JC, Guillot-Suay V, Sánchez Gila MM, Gutiérrez-Fernández J. Pelvic inflammatory disease by Streptococcus constellatus. Clinical experience and a review. Rev Espanola Quimioterapia: Publicacion Oficial La Sociedad Espanola Quimioterapia. (2020) 33:285–8. doi: 10.37201/req
11. Takada K, Nakamura M, Samura M, Inoue J, Hirose N, Kurata T, et al. Suppurative thrombophlebitis of the posterior neck caused by streptococcus constellatus: A case report and literature review. Yakugaku Zasshi: J Pharm Soc Japan. (2022) 142:189–93. doi: 10.1248/yakushi.21-00179
12. Paul SP, Mubashar T, James JA, Mubashar Y, Turner PC. Streptococcus constellatus-associated Lemierre’s syndrome presenting with extensive venous sinus thrombosis in a child. Br J Hosp Med (London England: 2005). (2021) 82:1–4. doi: 10.12968/hmed.2020.0541
13. Al Asaadi Z, Srinivasan B, Melchers LJ, Brennan PA. Streptococcus constellatus causing bony destruction secondary to odontogenic infection: three rare cases. Br J Oral Maxillofac Surgery. (2019) 57:594–6. doi: 10.1016/j.bjoms.2019.05.004
14. Barroso D, Rego R. A gelatinous pleural effusion as a diagnostic clue. Cureus. (2023) 15:e35942. doi: 10.7759/cureus.35942
15. Yoshino Y, Wakabayashi Y, Seo K, Koga I, Kitazawa T, Ota Y. Hyaluronic Acid concentration in pleural fluid: diagnostic aid for tuberculous pleurisy. J Clin Med Res. (2015) 7:41–4. doi: 10.14740/jocmr1980w
16. Liu JS, Tu CY, Shen TC. Jelly-like pleural effusion. QJM: Monthly J Assoc Physicians. (2014) 107:481. doi: 10.1093/qjmed/hct214
17. Foo CT, Paterson A, Duckworth A, Herre J. Intrapleural hyaluronidase in viscous Malignant mesothelioma pleural effusion. Chest. (2021) 160:e609–e11. doi: 10.1016/j.chest.2021.07.031
18. Zahedi S, Carvalho AS, Ejtehadifar M, Beck HC, Rei N, Luis A, et al. Assessment of a large-scale unbiased Malignant pleural effusion proteomics study of a real-life cohort. Cancers (Basel). (2022) 14:4366. doi: 10.3390/cancers14184366
19. Chang LC, Hua CC, Liu YC, Chu CM, Chen HJ, Lee N. Pleural fluid viscosity may help identifying Malignant pleural effusions. Respirol (Carlton Vic). (2008) 13:341–5. doi: 10.1111/j.1440-1843.2008.01276.x
Keywords: Streptococcus constellatus, gelatinous, pleural effusion, HIV, infection
Citation: Yang Z, Xiong W, Qian Z and Mao X (2025) Case Report: Infection with Streptococcus constellatus manifesting as gelatinous pleural effusion in an HIV-positive patient. Front. Immunol. 16:1545165. doi: 10.3389/fimmu.2025.1545165
Received: 14 December 2024; Accepted: 26 February 2025;
Published: 18 March 2025.
Edited by:
Tarani Kanta Barman, University of Texas Medical Branch at Galveston, United StatesReviewed by:
Sudeep Kumar, Albany Medical College, United StatesAvijit Dutta, Amity University, India
Copyright © 2025 Yang, Xiong, Qian and Mao. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Xiaorong Mao, bWFveHJAbHp1LmVkdS5jbg==
†ORCID: Zhongxia Yang, orcid.org/0000-0002-1257-234
 Zhongxia Yang
Zhongxia Yang Wanyuan Xiong1,2
Wanyuan Xiong1,2 Zibing Qian
Zibing Qian