
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Glob. Womens Health , 20 March 2025
Sec. Maternal Health
Volume 6 - 2025 | https://doi.org/10.3389/fgwh.2025.1501001
 Mohammed Aliyi1
Mohammed Aliyi1 Yimar Hotessa2
Yimar Hotessa2 Abdisa Haro2
Abdisa Haro2 Belda Negesa Beyene2
Belda Negesa Beyene2 Misgana Desalegn2
Misgana Desalegn2 Derese Eshetu Debela3*†
Derese Eshetu Debela3*†
Background: Breast cancer is the most common cancer among women. It is the leading or second cause of female cancer-related deaths in both developed and developing countries, including Ethiopia. Breast self-examination is an effective and efficient screening method used by women for the early detection of breast cancer. There is limited data about breast self-examination practice among pastoralist women in the study area. Therefore, the aim of this study was to assess the magnitude of breast self-examination practice and associated factors among women of childbearing age in the West Guji Zone, South Ethiopia.
Methods: A community-based cross-sectional study was conducted from 1 March to 30 April 2023 on 424 randomly selected women of childbearing age in the West Guji Zone. A systematic sampling technique was employed to select the study participants. Data was collected using pre-tested and structured questionnaires through face-to-face interviews, entered into EpiData version 4.6 and then exported to SPSS version 25 for cleaning and analysis. Bivariable and multivariable analyses were conducted using binary logistic regression to identify factors associated with breast self-examination practice. Statistical significance was declared at a P-value <0.05.
Result: In this study, 62 (14.6%) of the women had a good practice of breast self-examination. Maternal age (25–34 years) [adjusted odds ratio (AOR) = 1.98, 95% confidence interval (CI): 1.07–3.70], monthly income (AOR = 3.92, 95% CI: 1.34–11.49), residence (AOR = 2.28, 95% CI: 1.09–4.78), and knowledge about breast self-examination (AOR = 2.15, 95% CI: 1.14–4.05) were factors significantly associated with breast self-examination practice.
Conclusion: The study's findings indicated a significantly low level of breast self-examination practice among pastoralist women. Women's education should be promoted, income generated, and the practice of breast self-examination should be advocated.
Breast cancer is a malignant tumor originating from the breast cells that can range in severity from non-invasive to metastatic carcinoma (1). Breast cancer is a major public health problem, the most common form of cancer in women, and the second leading cause of cancer-related morbidity and deaths next to lung cancer (2). Among women of reproductive age, twice as many breast cancer cases are being diagnosed in low and middle-income countries than in industrialized countries (3). Globally, 1.15 million women are diagnosed with breast cancer, and more than half a million die from this disease every year (4).
There were an estimated 2.1 million newly diagnosed female breast cancer (FBC) cases worldwide in 2018, accounting for one in four cancer cases in women (5). The incidence rates vary greatly worldwide, from 19.3 per 100,000 in Eastern Africa to 89.7 per 100,000 in Western Europe (6). In sub-Saharan Africa, the incidence of breast cancer among women aged 15 and above was 23.5 per 100,000 women (7). In Ethiopia, 24.4% of women have had breast cancer (8). Any delay in the screening of breast cancer and treatment can lead to the diagnosis of the disease at a more advanced stage, leading to an increase in the death rate and a reduction in the chance of survival (9). The low survival rate in developing countries is due to the lack of appropriate early screening programs (10).
The early detection of breast cancer is crucial and involves mammography, a clinical breast examination (CBE), and a breast self-examination (BSE) (11). Of these strategies, BSE is a cost-effective method to detect breast cancer in resource-constrained countries (12). Breast self-examination is a simple, non-invasive, convenient, private, and non-harmful screening method used for the early detection of breast cancer. More than 90% of cases of breast cancer can be detected by women themselves; for this reason, it is important that women should understand the importance of BSE as the key breast cancer detection mechanism (13).
It is recommended that every woman starts BSEs at the age of 20, and it should be carried out once a month for 20 min between the 7th and 10th day of the menstrual cycle to detect breast cancer at the early stages (14).The method involves the woman herself looking at and feeling each breast for a possible mass, discharge, swelling of the breast, skin irritation or dimpling, and any change in size and shape of the breast (15). Regular breast self-examination practice is crucial for the early detection of breast cancer, potentially saving lives and a woman's regular and accurate BSE practice increases her motivation to seek medical attention (4).
Studies have revealed that breast self-examination practice remains low in many African countries. In Nigeria, the prevalence is 12.8% (12), 16.9% in Uganda (16), 16% in Cameroon (17), 8% in Sudan (18), and 6.9% in Ethiopia (19). Knowledge of BSE and breast cancer, income, level of education, ever heard about BSE, fear of detecting cancer, feeling that it violates privacy, and feeling of embarrassment are factors contributing to the low level of breast self-examination practice (7).
The Ethiopian government devotes a great deal of attention and resources to addressing non-communicable, infectious, and communicable diseases. Focus was placed on these illnesses by the government, non-governmental organizations, and international partners. Of these, breast cancer is at the bottom of the priority list (20). Studies have shown that the primary reason women do not undertake breast self-examinations is because they are unaware of the proper technique, timing, and position and because of their attitude toward the practice (19).
Breast cancer prevention is crucial, but early detection methods such as mammography and clinical breast examinations are inaccessible in low- and middle-income countries such as Ethiopia. Furthermore, mammography and clinical breast examinations are expensive as they need trained professionals and regular health facility visits, which are difficult for women living in rural, remote areas of the country (21). BSE is the only feasible approach for wide population coverage as it is a cheap and easy method (10).
Our research considers women of childbearing age because breast cancer is most commonly found in this age group. At this time, the breast cancers are more aggressive and grow faster, and it is the crucial period to detect and prevent breast cancer through breast self-examination screening in this age group. A previous study conducted in the country primarily focused on the health facility level. However, studies done at the community level, particularly in the pastoralist area of the country, are limited, and many women missed early detection and treatment opportunities. Moreover, no previous study has been conducted in the study area. Therefore, the purpose of this study was to assess the level of breast self-examination practice and associated factors among women of childbearing age in the West Guji Zone, Oromia, Ethiopia.
The study was conducted in the West Guji Zone, Oromia Region, Ethiopia, from 1 March 1 to 30 April 2023. The area is located 462 km from Addis Ababa, the capital city of Ethiopia, and 300 km from the Ethiopia–Kenya border. The zone has nine woredas and one town administration and a projected population of 1,422,767, of whom 697,156 are male and 725,611 are female. According to the 2007 National Census, there were 265,061 reproductive-age women and 49,370 pregnant women. The zone has 166 health posts, 42 health centers, 2 primary hospitals, and 1 general hospital. A community-based cross-sectional study design was employed.
All women of childbearing age who lived in the West Guji Zone at least 6 months prior to the study period were considered the source population, while all women of childbearing age who lived in seven randomly selected kebeles in the West Guji Zone during the study period were considered the study population.
Women of childbearing age who lived in the West Guji Zone for the 6 months prior to the study were included in the study, while women who could not provide responses, such as critically ill mothers and women with mental health problems, and female health workers who had knowledge of breast cancer were excluded.
The sample size needed for this study was determined using a single population proportion formula by considering a confidence level of 95%, a margin of error of 5%, a design effect of 1.5%, and a level of breast self-examination practice of 21.3% from the previous study (22), and adding a non-response rate of 10%. The final sample size was 424. The study participants were selected using multistage sampling. First, three woredas were selected from a total of 10 woredas found in the West Guji Zone using simple random sampling by lottery method. In the next stage, kebeles from each selected woreda were randomly selected.
A proportional allocation was then employed to decide the number of households that would be selected from each kebele. To prepare a sampling frame, a list of households in each kebele was used. Finally, households were selected using a systematic random sampling technique. The starting household was selected by the lottery method, and then every Kth household was obtained from their respective sampling frame, and an adequate number of eligible women was obtained based on the sample size proportionally allocated to each kebele.
The interviewer-based structured questionnaire was adapted and modified from different peer-reviewed studies in the literature and scientific facts (4, 10, 20, 22). The English version of the questionnaire was translated to Afan Oromo and then back to English to ensure relevance and accuracy. The questionnaires comprise sociodemographic characteristics, history of breast cancer, knowledge of BSE, perception toward BSE, and BSE practice. Seven health extension workers and three supervisors were recruited for data collection. One day of training was given to the data collectors and supervisors. The pre-test was conducted and the data was collected through a face-to-face interview at the participants’ homes.
Breast self-examination practice.
Sociodemographic characteristics including age, occupation, educational status, employment status, income, marital status, religion, residence, marital status, religion, family history of breast cancer, personal history of breast cancer, knowledge of BSE and early danger signs of breast cancer, and risk perception about breast cancer.
Good breast self-examination practice was defined as those who performed a breast self-examination a week after each menses using their palm and three middle fingers, otherwise defined as poor practice. Regular BSE practice was defined as performing BSE correctly at least once in a month after menses consistently.
Good knowledge was defined as a mean score or above for the provided 14 closed-ended questions about BSE. Poor knowledge was defined as a score below the mean for the provided 14 closed-ended questions about BSE (22).
A favorable attitude was defined as a score equal to and greater than the mean for the attitude questions. An unfavorable attitude was defined as a score less than the mean for the attitude questions (22). Regarding perceived benefits, scores to the answers to the four questions on the benefit of performing a BSE for the early detection of breast cancer below two were defined as low perceived benefits and above 2 was defined as good perceived benefits (22).
The questionnaires were prepared in English, translated to Afan Oromo, and translated back to English to ensure their originality. A pre-test was conducted on 5% of the sample population at Gerba Kebele, and based on the result, some modifications were made to the questionnaire after the pre-test. Data collectors and supervisors were trained for 1 day to make them familiar with the objective of the study. Data were collected under the supervision of the principal investigator and supervisor. Questionnaires were checked for completeness on a daily basis by supervisors.
The data was entered into EpiData version 4.6 and exported to SPSS version 25 for coding and analysis. Descriptive statistics, including frequencies, percentages, means, and standard deviations, were calculated to describe the characteristics of the study respondents. Bivariate and multivariable analyses were conducted in a binary logistic regression model to identify factors associated with BSE. The assumption of binary logistic regression was checked. The Hosmer and Lemeshow test was conducted to check the final model's fitness. Multicollinearity among independent variables was checked by the variance inflation factor (VIF <10). Adjusted odds ratios (AORs) with a 95% confidence interval (CI) were computed to determine the level of significance. Statistical significance was declared at P-value <0.05. The results are presented using tables and figures.
A total of 424 reproductive-age women were involved in the study. The mean age (±SD) of study respondents was 28 (±6) years. Of the study participants, 210 (49.5%) were between the ages of 25–34 years; 372 (87.7%) were married; 137 (32.3%) had no formal education, and 224 (52.8%) study respondents were housewives (Table 1). Of the study participants, 357 (84.2%) reported that they did not have a family history of breast cancer, and 67 (15.8%) had a family history of breast cancer. Furthermore, 30 (7.1%) respondents had a personal history of breast cancer and 49 (11.6%) knew someone or patients suffering from breast cancer (Table 2).
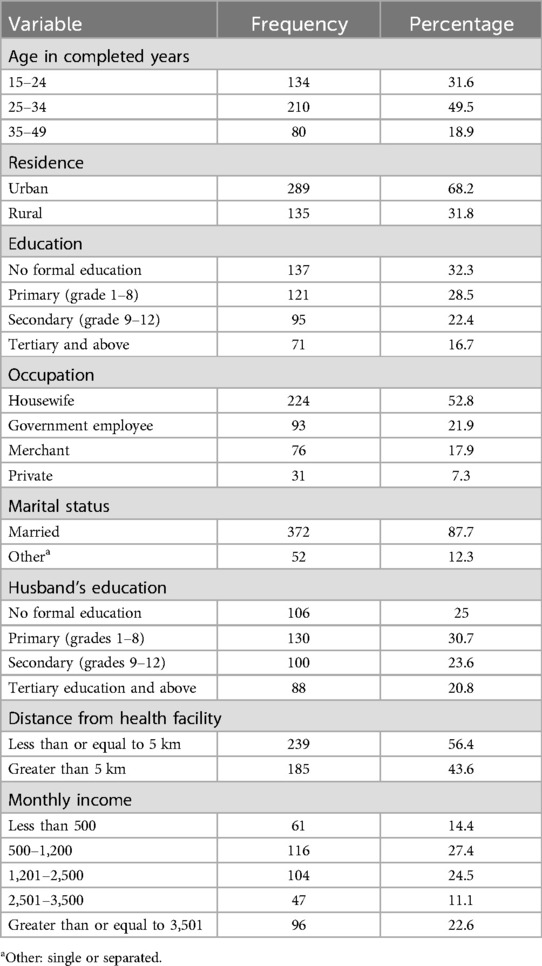
Table 1. Sociodemographic characteristics of the study participants in the West Guji Zone, Oromia, Ethiopia.
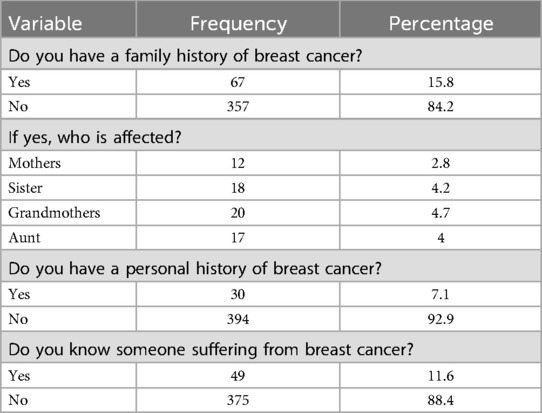
Table 2. Family and personal history of breast cancer among women of childbearing age who participated in the study in the West Guji Zone, Oromia region, Southern Ethiopia.
Of the study respondents, 142 (33.9%) participants had good knowledge of breast self-examination practice. Furthermore, 209 (49.5%) of the total respondents had ever heard about BSE and 324 (76.4%) participants had begun BSE after 20 years of age (Table 3).
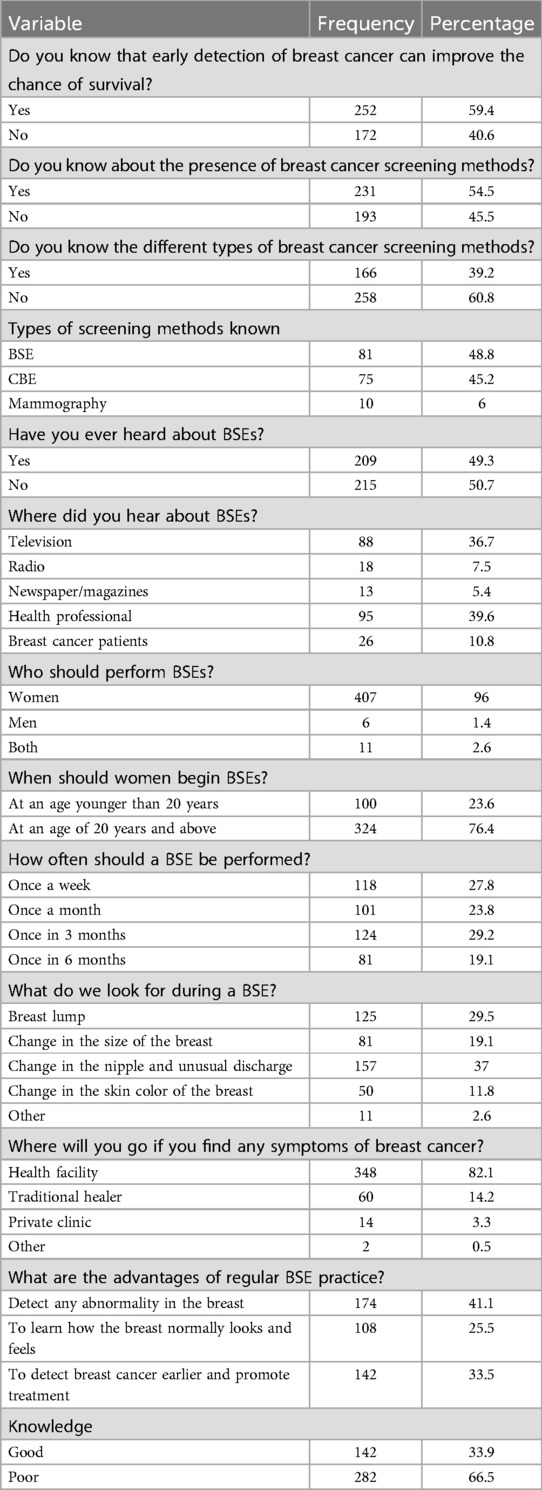
Table 3. Knowledge of breast self-examination practice of women of childbearing age who participated in the study in the West Guji zone, Southern Ethiopia, in 2023 and associated factors.
Of the study respondents, 285 (67.2%) of the study participants had a favorable attitude toward breast self-examination practice and 139 (32.8%) had an unfavorable attitude (Table 4).
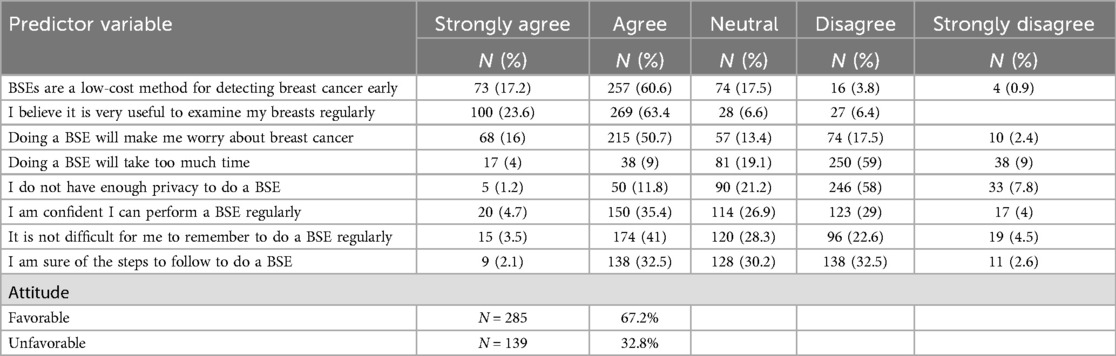
Table 4. The attitude toward breast self-examination practice of women of childbearing age who participated in the study in the West Guji Zone, Southern Ethiopia, in 2023 and associated factors.
Of the study participants, 62 (14.6%) women had good breast self-examination practice. Furthermore, 39 (9.2%) study participants were doing a breast self-examination regularly, and 92 (21.7%) knew the appropriate time to perform a breast self-examination (Table 5).
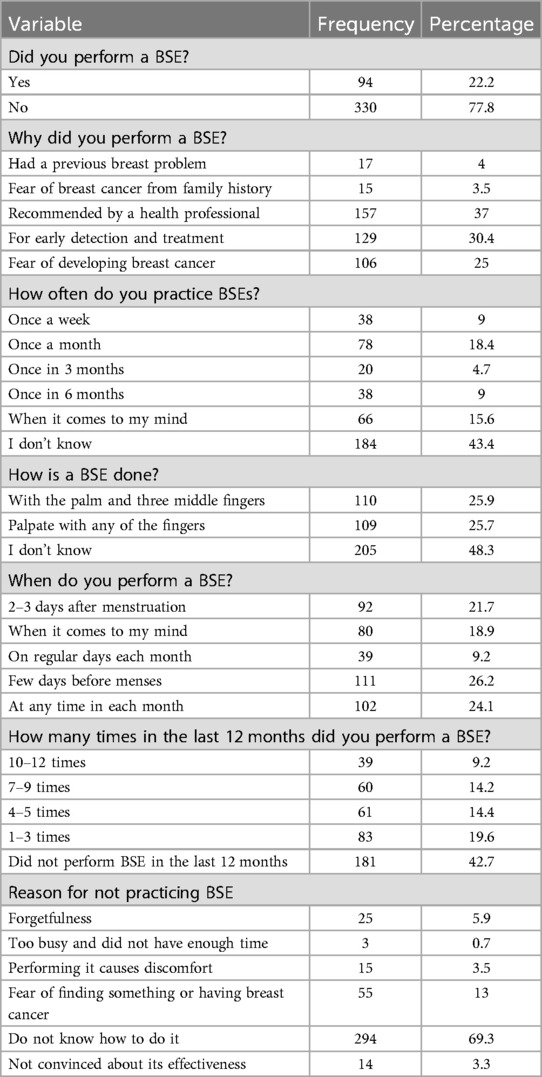
Table 5. Assessment of BSE practice among women of childbearing age in the West Guji Zone, Southern Ethiopia, in 2023.
In this study, the magnitude of breast self-examination practice among reproductive-age women was 14.6% (95% CI: 11.4%–18.4%). In the multivariable logistic regression analysis, after controlling for possible confounding variables, the age, residence, income, and knowledge variables were significantly associated with breast self-examination practice at a P-value <0.05. According to the findings of this study, breast self-examination was 1.98 times more likely to be practiced among reproductive women aged 25–34 years (AOR = 1.98; 95% CI: 1.06–3.70) than those aged 15–24 years.
In this study, women who had earned an average monthly income of between 2,501 and 3,500 Ethiopian birr (AOR = 3.92; 95% CI: 1.34–11.48) were 3.92 times more likely to practice BSE compared to women who had a monthly income less than 500 Ethiopian birr. Women who were urban residents (AOR = 2.28; 95% CI: 1.09–4.78) were 2.28 times more likely to practice breast self-examinations compared to women who were rural residents. The odds of practicing breast self-examination were 2.15 times higher among women who had good knowledge (AOR = 2.15; 95% CI: 1.14–4.05) of BSE compared to women who had poor knowledge of BSE (Table 6).
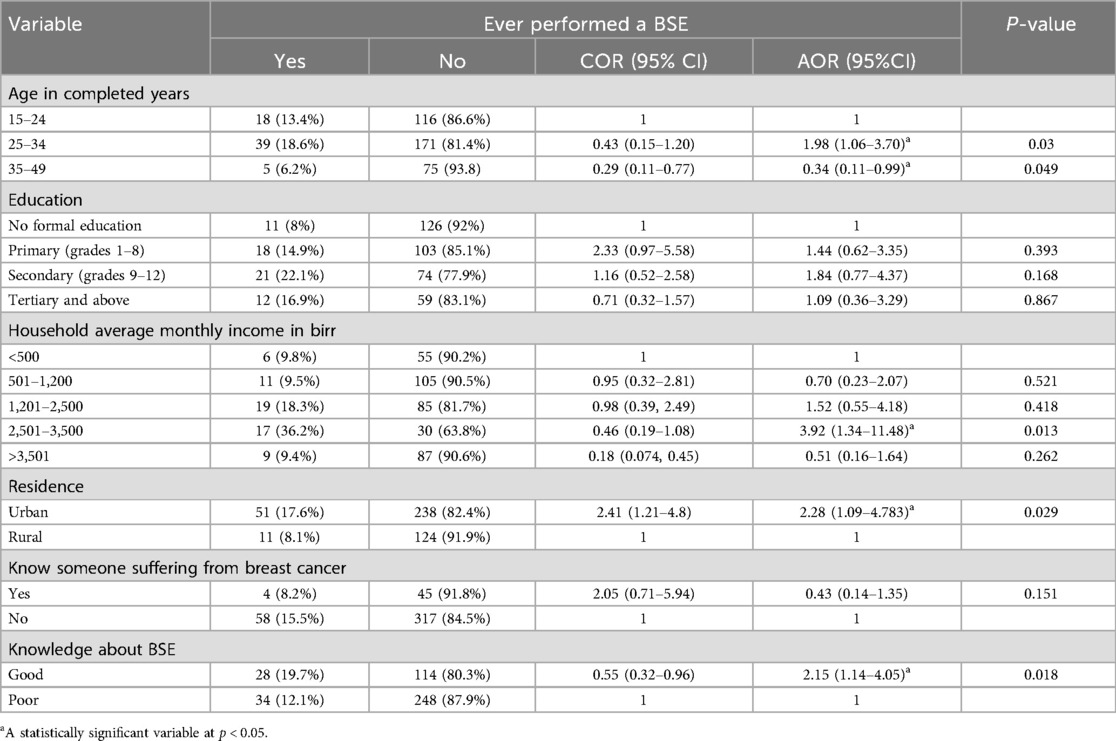
Table 6. Bivariate and multivariate logistic regression analysis of BSE practice among the study participants in the West Guji Zone, Southern Ethiopia.
Breast cancer is the most prevalent cancer among women, particularly in developing countries. A breast self-examination is one of the screening methods in which a woman examines her breasts for any abnormal changes. There was limited data on BSE in the study area. Therefore, the aim of this study was to assess the practice of breast self-examination and its associated factors among women of childbearing age in the West Guji Zone, Oromia, Southern Ethiopia, in 2023.
This study revealed that the magnitude of breast self-examination practice among reproductive-age women was 14.6% (62; 95% CI: 11.4–18.4), which was consistent with the study done in Jimma with 15% (10) and the Bale Zone with 13.2% (21). This could be due to the similar socioeconomic characteristics of the study populations. However, the prevalence was lower than in studies conducted in Ghana (37.6%) (23) and Ethiopia (32.6%) (24). However, it was higher than studies conducted in Eritrea (11.7%) (25) and northern Ethiopia (6.5%) (20). This discrepancy could be a result of differences in sample size, study period, populations, economic status, and geography.
In this study, 67.2% of the study respondents had a favorable attitude toward breast self-examination practice. This finding was supported by 4.7% of women who were confident that they could perform a breast self-examination regularly every month. Furthermore, 15.8% of the study participants had a family history of breast cancer. In this study, 4.7% of the participants’ grandmothers had been affected by breast cancer and 7.1% of the cases were related to the personal history of breast cancer of the study participants.
In this study, maternal age was statistically significant with breast self-examination practice. This finding was supported by studies conducted in Bangladesh (26), Cameroon (17), and Ethiopia (10, 21, 27). This implies that as age increases, the prevalence of breast self-examinations also increases. This may be due to the fact that at this age, women are paying attention to their reproductive activity, and, as a result of increased contact with health facilities and health professionals than at any other time in their lives, their attention to and care of their breast health increases.
According to these study findings, average monthly income was statistically associated with breast self-examination practice. This finding was in line with studies conducted in Palestine (28) and Jimma (10). This could be due to the fact that women who have a higher income level can visit health facilities and they might have access to information about the early practice of BSE.
In this study, the residence of the study participants affected the prevalence of breast self-examinations among reproductive-aged women. This finding was consistent with studies conducted in Uganda (16) and Jimma, Ethiopia (10). This may be due to mothers who lived in urban areas having access to information about BSE practice and the accessibility of health facilities and health professionals, and, thus, they are aware more about BSE practice. Breast self-examination practice was significantly affected by the knowledge of the study respondents. This finding was supported by studies conducted in Uganda (16) and Ethiopia (7, 29). This might be due to the awareness levels of the study respondents.
For breast self-examination practice, each variable was managed independently to control the effect of confounders and prevent bias from being introduced at the analysis stage. Furthermore, the results can be generalized for the total population of the study area. The responses of the study participants were based on self-reported information, which is subject to bias since the study raised personal issues; thus, there is the possibility of underestimation or overestimation. In addition, the study only included women of reproductive age, defined as those between the ages of 15 and 49; women over the age of 49 were not considered. The use of a cross-sectional design has limited the degree of cause-and-effect associations that can be made among the variables of interest.
The practice of breast self-examination among women of childbearing age in the West Guji Zone was low. Factors such as maternal age, income, residence, and knowledge were the factors associated with breast self-examination practice. Health professionals should raise awareness of and provide health education on BSE to reproductive-age mothers. The government should promote income-generating mechanisms for women and ensure the accessibility of information through different media outlets.
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
The studies involving humans were approved by Bole Hora University, School of Graduate Studies. The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
MA: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. YH: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. AH: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. BB: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. MD: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. DD: Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing.
The author(s) declare financial support was received for the research and/or publication of this article. Bule Hora University provided funds for the data collection and stationary materials of this research work (http://www.bhu.edu.et). The funders had no role in study design, data collection, and analysis, decision to publish, or preparation of the manuscript.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The author(s) declare that no Generative AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
1. Abeje S, Seme A, Tibelt A. Factors associated with breast cancer screening awareness and practices of women in Addis Ababa, Ethiopia. BMC Women’s Health. (2019) 19:4. doi: 10.1186/s12905-018-0695-9
2. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. (2018) 68:394–424. doi: 10.3322/caac.21492
3. Barba D, León-Sosa A, Lugo P, Suquillo D, Torres F, Surre F, et al. Breast cancer, screening and diagnostic tools: all you need to know. Crit Rev Oncol Hematol. (2021) 157:103174. doi: 10.1016/j.critrevonc.2020.103174
4. Jemebere W. Practice of breast self-examination and associated factors among female nurses of Hawassa university comprehensive specialized hospital, South Ethiopia, 2018. J Health Med Nurs. (2019) 12:1457–66. doi: 10.5281/zenodo.3543722
5. Shrivastava SR, Sowbha C, Shrivastava PS. A cross-sectional descriptive study to assess the awareness of breast cancer and practice of breast self-examination among rural women in Kancheepuram district. Indian J Community Fam Med. (2020) 6:61–5. doi: 10.4103/IJCFM.IJCFM_69_19
6. Gemta EA, Bekele A, Mekonen W, Seifu D, Bekurtsion Y, Kantelhardt EJ. Patterns of breast cancer among Ethiopian patients: presentations and histopathological features. J Cancer Sci Ther. (2019) 11:1–5. doi: 10.4172/1948-5956.1000581
7. Mekuria M, Nigusse A, Tadele A. Breast self-examination practice and associated factors among secondary school female teachers in Gammo Gofa zone, Southern, Ethiopia. Breast Cancer (Dove Med Press). (2020) 12:1–10. doi: 10.2147/BCTT.S232021
8. Tesfaw A, Demis S, Munye T, Ashuro Z. Patient delay and contributing factors among breast cancer patients at two cancer referral centres in Ethiopia: a cross-sectional study. J Multidiscip Healthc. (2020) 13:1391–401. doi: 10.2147/JMDH.S275157
9. Alshahrani SM, Almutiran A, Ahmed NJ. Awareness and attitudes regarding breast self-examination and breast cancer among females in Alkharj. J Pharm Res Int. (2020) 32:71–7. doi: 10.9734/jpri/2020/v32i2630840
10. Biratu Terfa Y, Bayana Kebede E, Olani Akuma A. Breast self-examination practice among women in Jimma, Southwest Ethiopia: a community-based cross-sectional study. Breast Cancer (Dove Med Press). (2020) 12:181–8. doi: 10.2147/BCTT.S279148
11. Shiferaw WS, Aynalem YA, Akalu TY, Demelew TM. Incidence and predictors of recurrence among breast cancer patients in black lion specialized hospital adult oncology unit, Addis Ababa, Ethiopia: retrospective follow-up study with survival analysis. J Cancer Prev. (2020) 25:111–8. doi: 10.15430/JCP.2020.25.2.111
12. Hanson VF, El-Kader RGA, Ilesanmi RE. Practice and barriers of breast self-examination among women in a rural community in south western, Nigeria. Int J Stud Nurs. (2019) 4:46–53. doi: 10.20849/ijsn.v4i3.588
13. Kumarasamy H, Veerakumar AM, Subhathra S, Suga Y, Murugaraj R. Determinants of awareness and practice of breast self examination among rural women in Trichy, Tamil Nadu. J Midlife Health. (2017) 8:84–8. doi: 10.4103/jmh.JMH_79_16
14. Usman IN, Olanrewaju SO, Usman SO. Breast self-examination practice among female secondary school students in Osogbo, Western Nigeria. Eur J Med Health Sci. (2020) 2:1–7. doi: 10.24018/ejmed.2020.2.2.173
15. Udoh RH, Tahiru M, Ansu-Mensah M, Bawontuo V, Danquah FI, Kuupiel D. Women’s knowledge, attitude, and practice of breast self- examination in sub-Saharan Africa: a scoping review. Arch Public Health. (2020) 78:84. doi: 10.1186/s13690-020-00452-9
16. Joyce C, Ssenyonga LVN, Iramiot JS. Breast self-examination among female clients in a tertiary hospital in eastern Uganda. Int J Africa Nurs Sci. (2020) 12:100186. doi: 10.1016/j.ijans.2019.100186
17. Azemfac K, Christie SA, Carvalho MM, Nana T, Fonje AN, Halle-Ekane G, et al. A community-based assessment of knowledge and practice of breast self-examination and prevalence of breast disease in southwest Cameroon. J Cancer Epidemiol. (2019) 2019:2928901. doi: 10.1155/2019/2928901
18. Al-Biatty S, Salih E, Alamin S, Altoom N, Babeker R, Gnawi O. Knowledge, attitude and practice of breast self-examination in Khartoum state, Sudan. Clin Med (Lond). (2020) 20:s2–3. doi: 10.7861/clinmed.20-2-s2
19. Birhane K, Alemayehu M, Anawte B, Gebremariyam G, Daniel R, Addis S, et al. Practices of breast self-examination and associated factors among female Debre Berhan university students. Int J Breast Cancer. (2017) 2017:1–6. doi: 10.1155/2017/8026297
20. Abay M, Tuke G, Zewdie E, Abraha TH, Grum T, Brhane E. Breast self-examination practice and associated factors among women aged 20–70 years attending public health institutions of Adwa town, North Ethiopia. BMC Res Notes. (2018) 11:622. doi: 10.1186/s13104-018-3731-9
21. Hussen A, Kumbi M, Bedewi J, Lette A, Nuriye S. Breast self-examination practice and associated factors among women of reproductive age in southeast Ethiopia. Front Oncol. (2023) 13:1176022. doi: 10.3389/fonc.2023.1176022
22. Mereta B, Shimbre M, Mekonnen B, Desalegn N, Getie A, Abdilwohab MG. Assessment of breast self- examination and associated factors among women age 20–64 years at Arba Minch Zuria district, Gamo zone SNNPR Ethiopia. Res Sq. (2020):1–18. doi: 10.21203/rs.2.21847/v1
23. Dadzi R, Adam A. Assessment of knowledge and practice of breast self-examination among reproductive age women in Akatsi south district of Volta region of Ghana. PLoS One. (2019) 14:e0226925. doi: 10.1371/journal.pone.0226925
24. Shallo SA, Boru JD. Breast self-examination practice and associated factors among female healthcare workers in West Shoa Zone, Western Ethiopia 2019: a cross-sectional study. BMC Res Notes. (2019) 12:637. doi: 10.1186/s13104-019-4676-3
25. Kifle MM, Kidane EA, Gebregzabher NK, Teweldeberhan AM, Sielu FN, Kidane KH, et al. Knowledge and practice of breast self examination among female college students in Eritrea. Am J Health Res. (2016) 4:104. doi: 10.11648/j.ajhr.20160404.16
26. Tithi NS, Asaduzzaman M, Nasrin N, Hossan MS, Rahman N, Nizum NA. A cross-sectional survey on knowledge regarding breast cancer and breast self-examination among Bangladeshi women. IOSR J Pharm Biol Sci. (2018) 13:38–44. doi: 10.9790/3008-1301013844
27. Dinegde NG, Demie TG, Diriba AB. Knowledge and practice of breast self-examination among young women in tertiary education in Addis Ababa, Ethiopia. Breast Cancer (Dove Med Press). (2020) 12:201–10. doi: 10.2147/BCTT.S279557
28. Baloushah S, Salisu WJ, Elsous A, Muhammad Ibrahim M, Jouda F, Elmodallal H, et al. Practice and barriers toward breast self-examination among Palestinian women in Gaza city, Palestine. ScientificWorldJournal. (2020) 2020:7484631. doi: 10.1155/2020/7484631
Keywords: breast cancer, breast self-examination, practice, pastoralist women, Guji Zone, Ethiopia
Citation: Aliyi M, Hotessa Y, Haro A, Beyene BN, Desalegn M and Debela DE (2025) Breast self-examination practice and associated factors among pastoralist women in the West Guji Zone, Oromia, Ethiopia: a community-based cross-sectional study. Front. Glob. Women's Health 6:1501001. doi: 10.3389/fgwh.2025.1501001
Received: 24 September 2024; Accepted: 24 February 2025;
Published: 20 March 2025.
Edited by:
Giorgio De Nunzio, University of Salento, ItalyReviewed by:
Meesha Chaturvedi, National Centre for Disease Informatics and Research (NCDIR), IndiaCopyright: © 2025 Aliyi, Hotessa, Haro, Beyene, Desalegn and Debela. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Derese Eshetu Debela, ZGVyZXNlZXNoZXR1MTJAZ21haWwuY29t
†ORCID:
Derese Eshetu Debela
orcid.org/0000-0003-1753-8272
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.