
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Glob. Womens Health , 18 March 2025
Sec. Maternal Health
Volume 6 - 2025 | https://doi.org/10.3389/fgwh.2025.1444184
Background: Quality of intrapartum and newborn care is increasingly recognized internationally as a critical aspect of the unfinished maternal and newborn health agenda. Although the world has made significant progress in reducing maternal and newborn mortality, there are still far too many preventable and treatable maternal and newborn deaths globally. Poor-quality intrapartum and newborn care along with inadequate access to basic maternal and newborn healthcare services has contributed to high maternal and child mortality in low- and middle-income countries. However, there is not enough evidence describing the status quality of intrapartum and newborn care in Ethiopia, specifically in the study area. Thus, this study aims to assess the quality of intrapartum and newborn care in public health facilities of Wolkite town, Central Ethiopia.
Methods: A facility-based cross-sectional study design was conducted from March to April 2023 among five public health facilities, and observation of health service provision was employed among 185 mothers. A consecutive random sampling method was applied. Data were collected through document review, interview, health service provision observation, and health facility audit against the standard checklist. Quality of intrapartum and newborn care was measured using standard intrapartum and newborn care criteria. Thus, good-quality care was considered if the mother and newborn scored 75% or more of the intrapartum criteria during childbirth. Data were entered, coded, and cleaned using EpiData version 4 and exported to SPSS version 25 for analysis. Descriptive summary statistics including proportions, mean, and median were computed to describe study variables. Multivariable logistic regression analysis was performed to identify factors significantly associated with the outcome variable. Finally, adjusted odds ratios with 95% confidence intervals and p-values <0.05 were considered to declare the statistical significance level of a variable.
Result: The study revealed that the level of good quality of intrapartum and newborn care was 35.1% and 69.7%, respectively. Input quality (AOR = 4.52; 95% CI 1.31, 14.98), health workers with 5 or more years of experience (AOR = 7.23; 95% CI 1.49, 35.84), received on job training (AOR = 5.82; 95% CI 1.91, 13.61), and friendly maternal and newborn care (AOR = 6.89; 95% CI 1.34, 35.62) were significantly associated with quality of intrapartum care.
Conclusion: The quality of intrapartum care is found poor in the study area. Clients are not getting intrapartum care with state-of-the-art knowledge and current clinical best practices. Input quality, the experience of healthcare providers, friendly care, and continuous training were factors associated with the quality of intrapartum care. Improving the availability of essential inputs, enhancing the performance of healthcare providers through training, and continuous objective monitoring of the standard clinical practices are crucial to ensuring the quality of intrapartum care.
Intrapartum and newborn care represents the entire range of services offered to mothers and babies from the onset of labor to the period immediately after birth, which includes monitoring, managing complications, providing interventions, and ensuring a safe transition for the baby into neonatal life (1, 2). Quality of intrapartum and newborn care is increasingly recognized internationally as a critical aspect of the unfinished maternal and newborn health agenda (3). The World Health Organization recommends that every pregnant woman and newborn receives high-quality care throughout the intrapartum period, as the time around childbirth is the most critical for saving the maximum number of maternal and newborn lives (4).
Although maternal mortality has declined from 339 to 223 per 100,000 live births between 2000 and 2020 globally, there are still far too many preventable and treatable maternal and newborn deaths due to poor-quality intrapartum and newborn care in health facilities (5, 6). This number is far behind the Sustainable Development Goal (SDG) that aims to reduce maternal mortality ratio (MMR) to less than 70 per 100,000 live births and neonatal mortality to at least as low as 12 per 1,000 live births (7). Each year, more than 295,000 women die from complications of pregnancy and delivery, and an estimated 2.4 million children die within their first month of life (8), 94% of these deaths occur in low- and middle-income countries (LMIC) and sub-Saharan Africa (5, 8).
There is strong evidence showing that the highest magnitude of maternal death has happened around childbirth and the immediate postpartum period (9). Improvement in quality of care throughout the intrapartum period can have a significant impact on maternal and newborn survival and well-being (10). Enhancing the quality of intrapartum and newborn care can be achieved through ensuring access to skilled birth attendants with evidence-based practice and respectful care, creating a supportive environment, using effective clinical and non-clinical best practices, building healthcare infrastructure, and ensuring healthcare providers have optimum skills, knowledge, and positive attitude (11, 12).
The lives of over 3 million mothers and babies can be saved every year with high coverage of high-quality intrapartum and newborn care (13). According to the results of an evidence-based intervention study conducted in 2020 among 81 countries, the provision of good-quality healthcare could reduce maternal and infant mortality by 28% and stillbirths by 22% when compared to scenarios without any improvement in quality of care (10).
In sub-Saharan Africa, the quality of intrapartum care in public health facilities remains a challenge, and these problems are made worse by the health system’s struggles to meet both the demand for routine quality healthcare and the frequent need to respond to drought, conflict, and disease outbreak including COVID-19 (14). According to estimates, in low- and middle-income countries (LMIC), about six out of ten neonatal problems and 50% of maternal deaths are due to inadequate quality of intrapartum and newborn care (15). Hence, achieving high-quality, effective, safe, people-centered, timely, equitable, integrated, and efficient care is crucial to advancing women's and neonatal health outcomes (16, 17).
Despite remarkable progress in reducing the rate of maternal and newborn mortality over the last decades, Ethiopia still experiences one of the highest maternal and newborn mortality rates in the world which stood at 401 per 100,000 live births and 33 per 1,000 live births, respectively (18). According to the FMoH report, in Ethiopia in 2017, 49% of reported maternal deaths occurred after women were found at health facilities, 14% of that maternal mortality was due to a shortage of supplies and instruments, 11% due to patient management delay at the facility, 6% due to care providers error and mismanagement, and 28% due to referral delays from different facilities (19). Therefore, increasing access to and utilization of maternal care alone is insufficient to enhance maternal health outcomes (15).
A study conducted in 2021 assessed the standard of maternal and newborn care in Ethiopia, revealing that most health facilities did not comply with the national standards for maternal and newborn health (MNH) quality of care requirements (15). Only 15.6%, 9.3%, and 10.7% of health facilities met the standard care for MNH and fulfilled the expected input, process, and output maternal and neonatal healthcare quality criteria, respectively (11). In 2016, Ethiopia adopted the World Health Organization’s standard for raising the quality of maternity and newborn healthcare in health institutions and developed a health sector quality transformation that aids in national quality strategy (NQS) implementation (16, 20). There are numerous methods for consistently measuring the process of various maternal and newborn health (MNH) care (21).
According to the Donabedian model, quality is measured in terms of three major aspects, namely, the structure (materials, infrastructure, and human resources), process (adherence to standard care throughout intrapartum and postpartum periods), and outcome (maternal satisfaction with the service's accessibility and use of emergency obstetric and newborn care) (22). Ethiopia's healthcare strategy has given due attention to the quality of health services recently (23). Therefore, generating rigorous evidence on the level of intrapartum quality of care will support the implementation of the national healthcare quality strategy.
One of the major obstacles to improving the quality of intrapartum and newborn care in low- and middle-income countries (LMIC) is the absence of relevant and reliable evidence (24). Although the quality of intrapartum care is essential for further improvement of maternal and neonatal health outcomes, there is not enough evidence about the status of the quality of intrapartum and newborn care in Ethiopia specifically in the study area.
The majority of the available studies mostly focused on survey-based client satisfaction (25–27), and few studies tried to assess the quality of intrapartum care through structure, process, and outcome of quality measurement (28). However, the relationship between the quality of the input and process of the intrapartum care was not evaluated in the previous studies. Therefore, the purpose of this study is to fill the knowledge gap by objectively assessing the quality of intrapartum and newborn care through survey and service provision observation methods. Furthermore, the association between the input and process quality of intrapartum care is examined in the current study.
A facility-based cross-sectional study design was conducted from March to April 2023 in the public health facilities of Wolkite town. Wolkite town is the administrative center of the Gurage Zone in Central Ethiopia and is located 155 km west of the capital city of the country, Addis Ababa. The town has three sub-cities and six kebeles (small administrative units). According to Wolkite town’s administration health office, the total population is expected to be 61,309. Out of the total population, 31,268 (51%) are females, and the rest 30,041 are males. The number of women who are in the child-bearing age group (15–49) is 13,568; from this, 2,128 are pregnant and expecting deliveries. There are three government health centers, one specialized hospital, one primary hospital, and 11 private clinics in the town. In Ethiopia including the study setting there is a medical cost exemption for maternal health services consisting of antenatal care (ANC) and intrapartum care provision. However, clients may experience the cost of transportation and other associated expenses.
All mothers who gave birth at public health facilities of Wolkite town were considered the source population. All mothers who gave birth at public health facilities of Wolkite town during the period of data collection were included in the study, while mothers who came for elective cesarean section delivery during the period of data collection period were excluded. Moreover, all public health facilities providing maternity services were included in the study. A total of 185 laboring mothers and skilled birth attendants from five health facilities were included in the study.
Sample size calculation for laboring mothers was determined by a single proportion of a finite population with a 95% confidence interval and marginal error (d) of 5% and by taking a 12.6% proportion (P) of respectful maternal care (29). Adding 10% to the non-response rate, a total of 185 mothers attending obstetric care were selected for the observation and document review. By considering the assumption of delivery attendance, a consecutive random sampling method was applied in the selected health facilities. The study participants were allocated proportionally to each health facility based on the number of delivery services provided in each health facility for 3 months prior to the study period.
Quality of intrapartum care is a composite variable measured using 92 items taken from the WHO guidelines, national guidelines (3, 30), and other studies that are consistent with the national guidelines. The included assessment of activities during the examination of mothers at admission, care during the various stages of labor (first, second, third), and the immediate postpartum period and infection prevention practice. The response of each item was rated 1 for “yes” and 0 for “no” by giving equal weight to all items. Then, the quality of intrapartum care was measured as good process quality if they scored ≥75% from process quality domain items (31).
Maternal-related (age of mothers, level of education, economic status, marital status, residence, ANC follow-up, parity and mode of delivery), physical- and human-related (availability of skilled care provider, type of institution, infrastructures, functional diagnostic service, availability of transportation, and distance from health facilities), interpersonal process-related (privacy, respectful, information provision politely, support and involvement of family members), health professional-related (profession, sex, and experience), and technical process-related (adherence to established standard care).
Input quality was measured using 40 items adopted from the WHO standards and other studies that are consistent with the national guidelines (3). These include the availability of basic equipment, infrastructure, and essential drugs. The response of each item was rated 1 for “yes” and 0 for “no” by giving equal weight to all items. Thus, input quality was measured as good quality if they scored ≥75% of the input quality score (31).
Quality of newborn care was measured using 11 items adopted from the WHO standards similar to the national guidelines (3, 30). This is part of the intrapartum quality care. The response of each item was rated 1 for “yes” and 0 for “no” by giving equal weight to all items. If they scored ≥75% of the items, they are considered as receiving good quality care (31).
Friendly mother and newborn care was measured using nine items. The response of each item was rated 1 for “yes” and 0 for “no” by giving equal weight to all items. Good friendly care was measured if they scored ≥75% of friendly care criteria (3). This is part of the intrapartum quality care (31).
Comprehensive emergency obstetric and newborn care (CEMONC) is a set of key obstetrics services or signal functions for pregnant women and newborns that may experience fatal complications, such as severe bleeding, infection, prolonged or obstructed labor, eclampsia, and asphyxia in the newborn (32).
Completeness of the partograph was measured using 14 items. The response of each item was rated 1 for “yes” and 0 for “no” by giving equal weight to all items. Completeness was assessed if ≥80% of the 14 items were filled correctly in the partograph to be categorized as a complete partograph (31).
Knowledge of a skilled birth attendant (SBA) was measured using 17 items. Firstly, the responses for each item were coded as “1” if the response was correct, otherwise coded as “0.” Secondly, individual responses to each item was summed up. Finally, individuals who correctly responded ≥70% of the knowledge items were categorized as having “good knowledge”, otherwise coded as having “poor knowledge” (31).
To assess the quality of intrapartum and newborn care, the data were collected by using observation, document review, structured interview guide, and facility audit. Data collection tools that were in line with national guidelines were adapted from different literature, and WHO standard was used to collect all the necessary data (3, 11, 31, 33). A facility inventory checklist was used to assess the input component to interview the head of the facility and experienced maternity about the availability of equipment, drugs, and supplies at the time of the data collection period to assess input quality care. An observation checklist was used to observe service provision during childbirth care starting from admission in the labor ward till the immediate postpartum period to assess the quality of intrapartum care, newborn care, and women- and newborn-friendly care. A structured interview guide was used to conduct interviews with SBAs to describe their experiences and knowledge level. A document review form was used to gather data from the mothers’ charts to assess the completeness of the partograph.
There were two BSc public health professionals as supervisors and seven BSc midwives as data collectors who were working in health facilities other than the study area. The data collectors were properly dressed and had an adequate number of unfilled questionnaires. Written informed consent and permission letters from the maternity ward were obtained prior to the survey. The data collectors explained the purpose of the study for both the mother and healthcare professional, and written informed consent was obtained from both before starting data collection. First, the data collector identified of availability of basic resources for the provision of intrapartum and newborn care using observation and interviewing the head of the institution, a focal person of labor and delivery at the facilities. Second, the data collector stayed in the delivery room without interfering with the care being provided to mothers and newborns and observed the entire labor, including history taking, physical examination, diagnosis, and women-friendly care (interpersonal and technical aspects). The observation covered the active phase of the first stage of labor, followed by continuous observation of the second and third stages of labor, newborn care, and the immediate postpartum period. Additionally, the document about partograph usage was reviewed. To minimize observer bias between data collectors and the Hawthorne effect, the first three observations were excluded from the data analysis.
To assess the quality of intrapartum and its predictors, both descriptive and inferential statistics were used. Data were checked for completeness; then cleaned, edited, coded, and entered into EpiData version 4; and exported to Stata version 14 and SPSS version 25 for analysis. Before the data analysis, the data were screened for missing and data entry errors using the frequency distribution of the variables and observation of the entered data. Suspected errors were validated against the raw data, and necessary corrections were made. Descriptive and summary statistics were computed. Binary logistic regression was performed to identify determinants of maternal satisfaction with the quality of intrapartum care. Variables with p-values of ≤0.25 in the bivariate analysis outcome were selected and included in the multivariable regression analysis. Finally, adjusted odds ratios with 95% confidence intervals and p-values <0.05 were considered significant independent factors of maternal satisfaction with the quality of intrapartum and newborn care. Model fitness was checked using the Hosmer–Lemeshow test (p = 0.772) by randomly inserting some of the variables whether the measured items correctly explained the dependent variable (quality of intrapartum care).
To enhance the quality of the data, the data collectors and supervisors were trained for 2 days on the objective and methodology of the research and data collection approach. The questionnaires were translated into the local language Amharic to increase the response rate. Then a questionnaire developed in Amharic was back translated into English to ensure the validity of the question. Regular supervision and meeting were made daily, and any problems raised during data collection were solved immediately. Pre-testing of the questionnaire was performed on 5% of the sample in Agena primary hospital which was not included in the actual study, and the questionnaire was modified based on the result of the pretest study. To check the internal consistency of the questionnaires, Cronbach's α test was performed (α coefficients = 0.904). All the questionnaires and data were checked for completeness and accuracy before, during, and after data collection, and double data entry was used to avoid data entry errors.
The ethical issues were considered throughout the study by considering the basic ethical research principles. Ethical clearance was obtained from the institutional review board (IRB) of Addis Ababa University, College of Health Science, School of Public Health, and a permission letter to carry out the study was obtained from Gurage zone health bureau. All study participants were given detailed information about the aims and methods of the study prior to the interview and observation, and written informed consent was obtained to participate in the current study. Confidentiality of information and privacy of participants was assured, and a close and harmonious relationship was established.
In this study, service provision sessions were observed for 185 mothers and healthcare professionals in charge of providing the services for these mothers. More than half of the mothers were within the age range of 25–34 years. The majority (83.9%) of respondents were Gurage by their ethnicity, and almost all 175 (94.5%) were married. Of the total mothers, 90 (48.6%) attended primary school. Regarding health professionals, more than half of the skilled birth attendants who gave the service were female 106 (57.3%), their work experience is within the range of 2–5 years 81 (43.7%), and 84 (45.4%) of deliveries were conducted by degree-level midwives (Table 1).
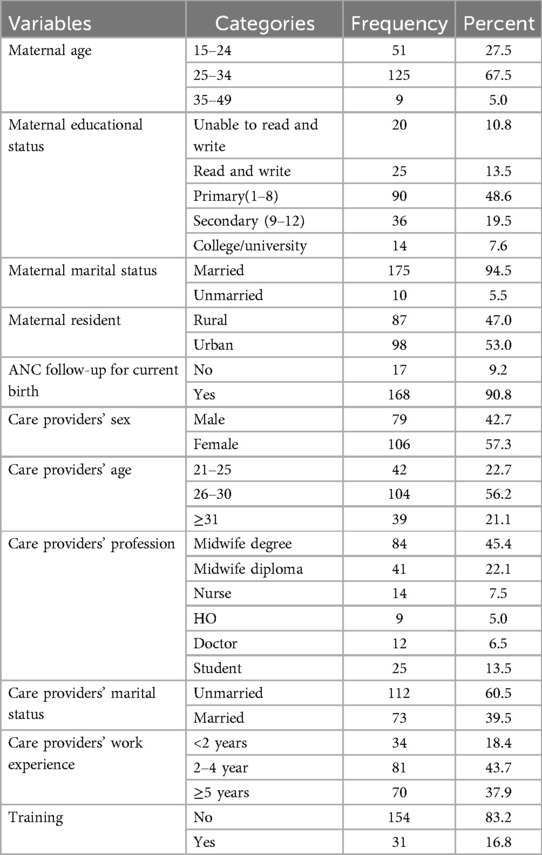
Table 1. Sociodemographic characteristics of mothers and healthcare professionals study on quality of intrapartum and newborn care in public health facility Wolkite town, Central Ethiopia, 2023 (N = 185).
In the five health facilities, 20 focal health professionals were interviewed, and verification by observation was conducted to assess input quality. Accordingly, out of the five health facilities, only three scored ≥75% of input quality items and were considered as having a good input quality. All facilities have electric power whereas only two had a standby backup automatic generator which starts within 5 min. However, only 40% of the health facilities have an adequate water supply. Functional basic laboratory tests (blood group, HCT, WBC count, and Rh test) were available only in one health facility.
Regarding human resources, all skilled healthcare professionals working in the delivery room and included in this study did not receive refresher training on managing obstetric complications, and only one facility has at least one skilled birth attendant trained to provide neonatal resuscitation. In addition, most of the health facilities lack towels to dry and wrap babies after delivery. Only one health facility has a functional toilet with shower service. Among the studied health facilities, only one health center and two hospitals gave all BEmONC and CEmONC signal functions, respectively (Table 2).
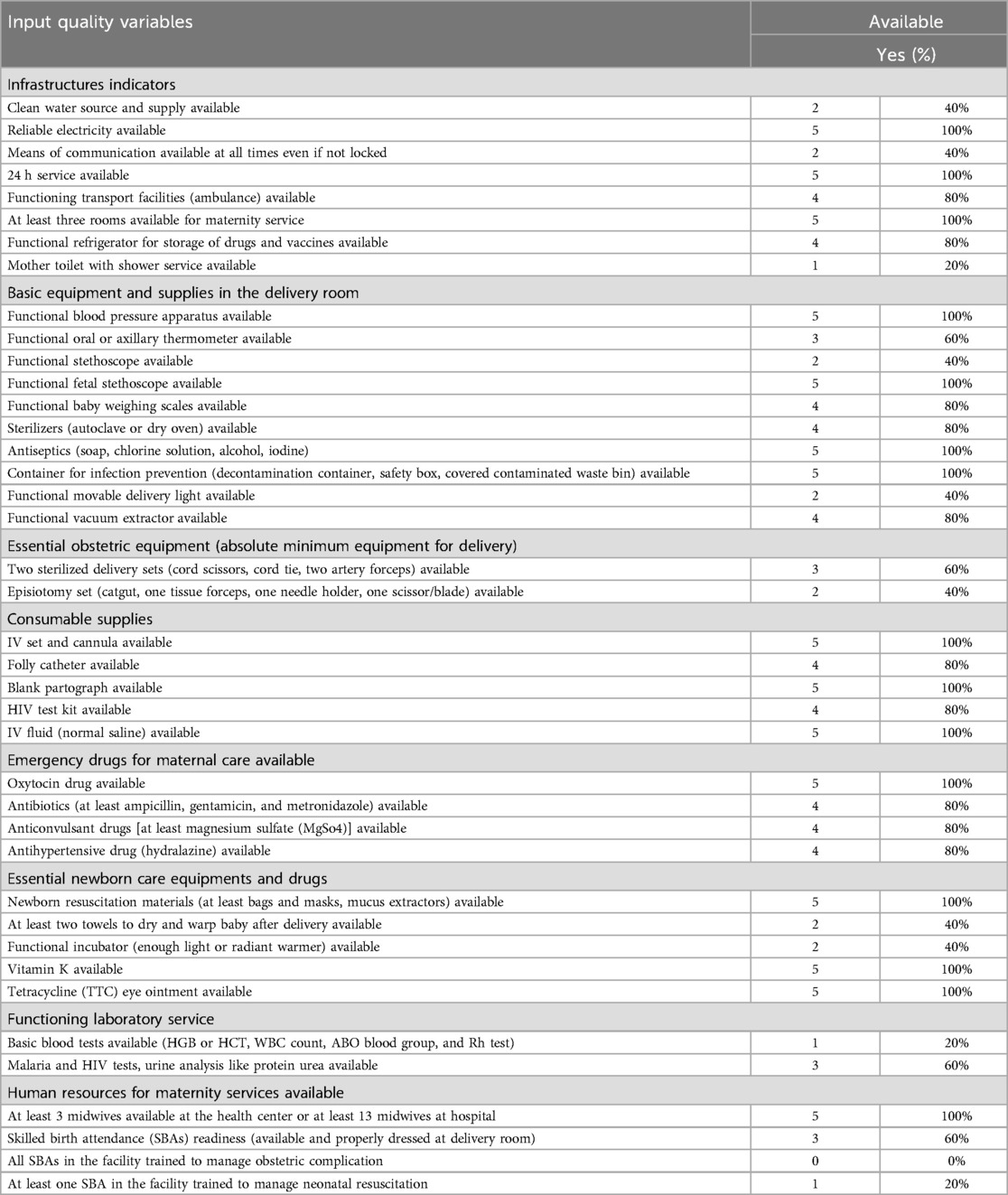
Table 2. Availability of infrastructure, human resources, drugs, and supplies for quality of input dimension in public health facilities of Wolkite town, Central Ethiopia 2023 (N = 5).
In this study, 185 deliveries were observed, and only 35.1% (95% CI: 28.3%, 41.9%) of mothers received good-quality intrapartum care. During labor admission, first stage, second stage, and third stage of labor and during the immediate postpartum period, 51 (27.3%), 64 (34.6%), 141 (76.2%), 153 (82.7%), and 91 (49.2%) of mothers received good-quality care, respectively (Figure 1). In the current study, 107 (57.8%; 95% CI: 50.4%, 65%) of mothers and newborns received maternal- and newborn-friendly care during the intrapartum period. Additionally, the finding of this study revealed that only 73 (39.5%; 95% CI: 32.4%, 46.9%) laboring mothers' partographs were completely and properly recorded during the progress of labor (Table 3).
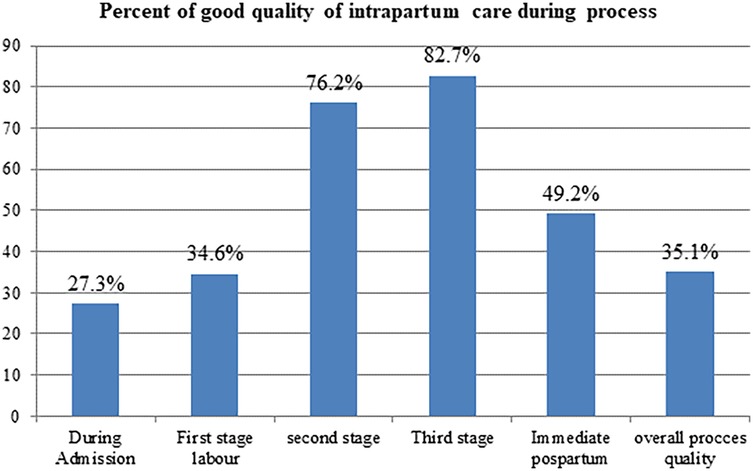
Figure 1. Proportion of good quality of intrapartum care in public health facilities of Wolkite town, Central Ethiopia, 2023.
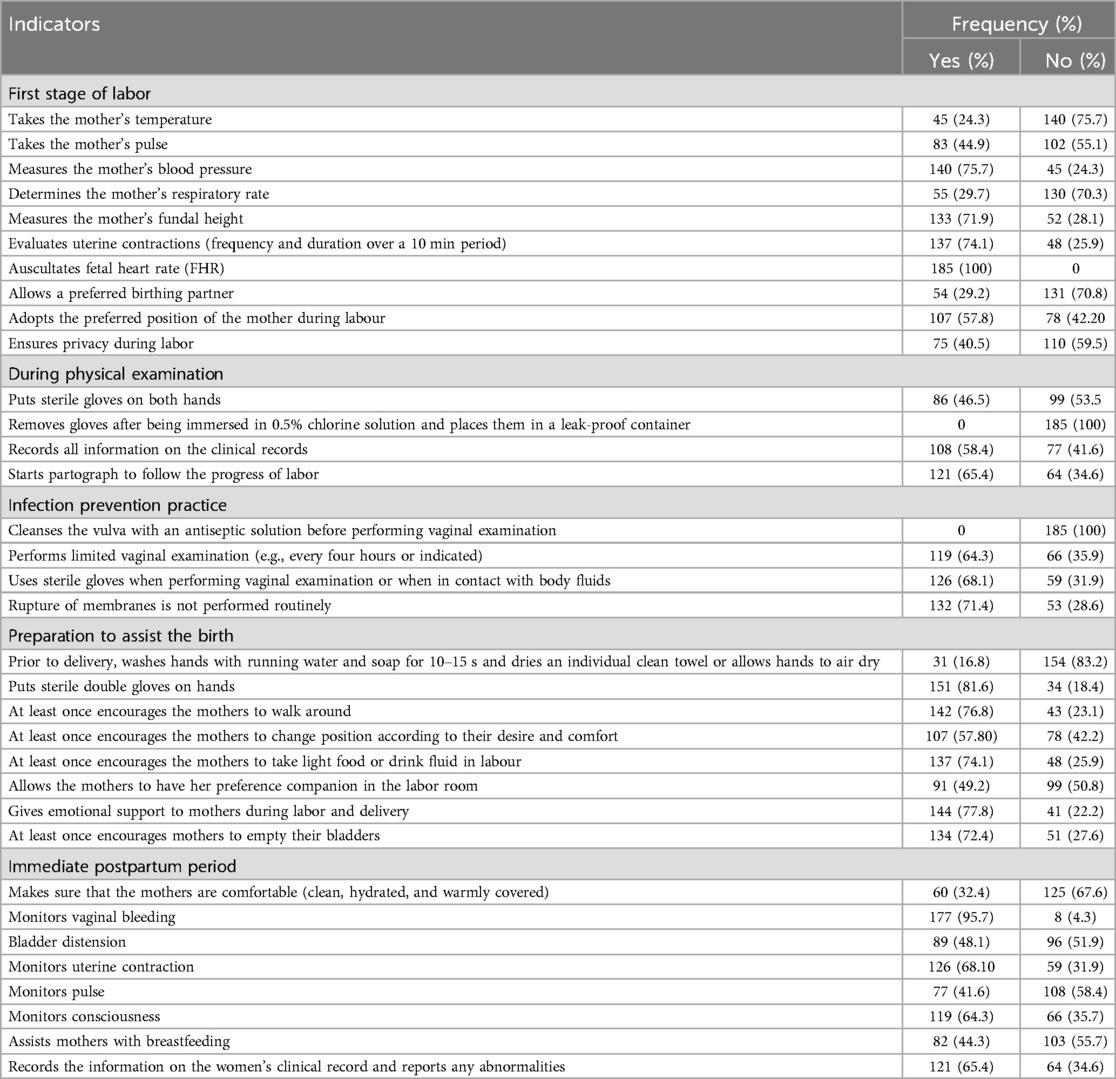
Table 3. Quality of intrapartum care aspect in public health facilities of Wolkite town, Central Ethiopia, 2023 (N = 185).
According to the 2016 WHO quality standards, the experience of newborn care was assessed. The findings of this study show that the overall quality of newborn care was 69.7% with 95% CI (62.6%, 76.3%) (Figure 2). In this study, almost all 172 (93%) of newborns started breastfeed within one 1 h. Vitamin K and TTC were administered to 164 (88.6%) and 174 (94.1%) of newborns, respectively. Additionally, only 71 (38.4%) of the newborns were passed to the mothers for skin-to-skin contact.
Figure 2. Quality of newborn care in public health facilities of Wolkite town, Central Ethiopia, 2023.
By using both bivariate and multivariable logistic regression analysis, this study identified that input quality, experience of healthcare providers, training, and maternal- and newborn-friendly care were significantly associated with the quality of intrapartum care.
The odds of mothers who gave birth in health facilities with good quality in input component were 4.5 times more likely to get good-quality intrapartum care than those who gave birth in health facilities with poor input component (AOR = 4. 52 95% CI: 1.31, 14.98). Mothers who get care from health professionals with ≥5 years of experience were seven times more likely to get good overall quality intrapartum care than their counterparts (AOR = 7.23, 95% CI: 1.49, 35.84). Mothers who get friendly healthcare were seven times more likely to receive good overall quality intrapartum care than their counterparts (AOR = 6.89, 95% CI: 1.34, 35.62). In addition, mothers who received care from trained skilled birth attendants were six times more likely to get good overall quality intrapartum care than mothers who received care from professionals who did not get refresher training on intrapartum care (AOR = 5.82, 95% CI: 1.91, 13.61) (Table 4).
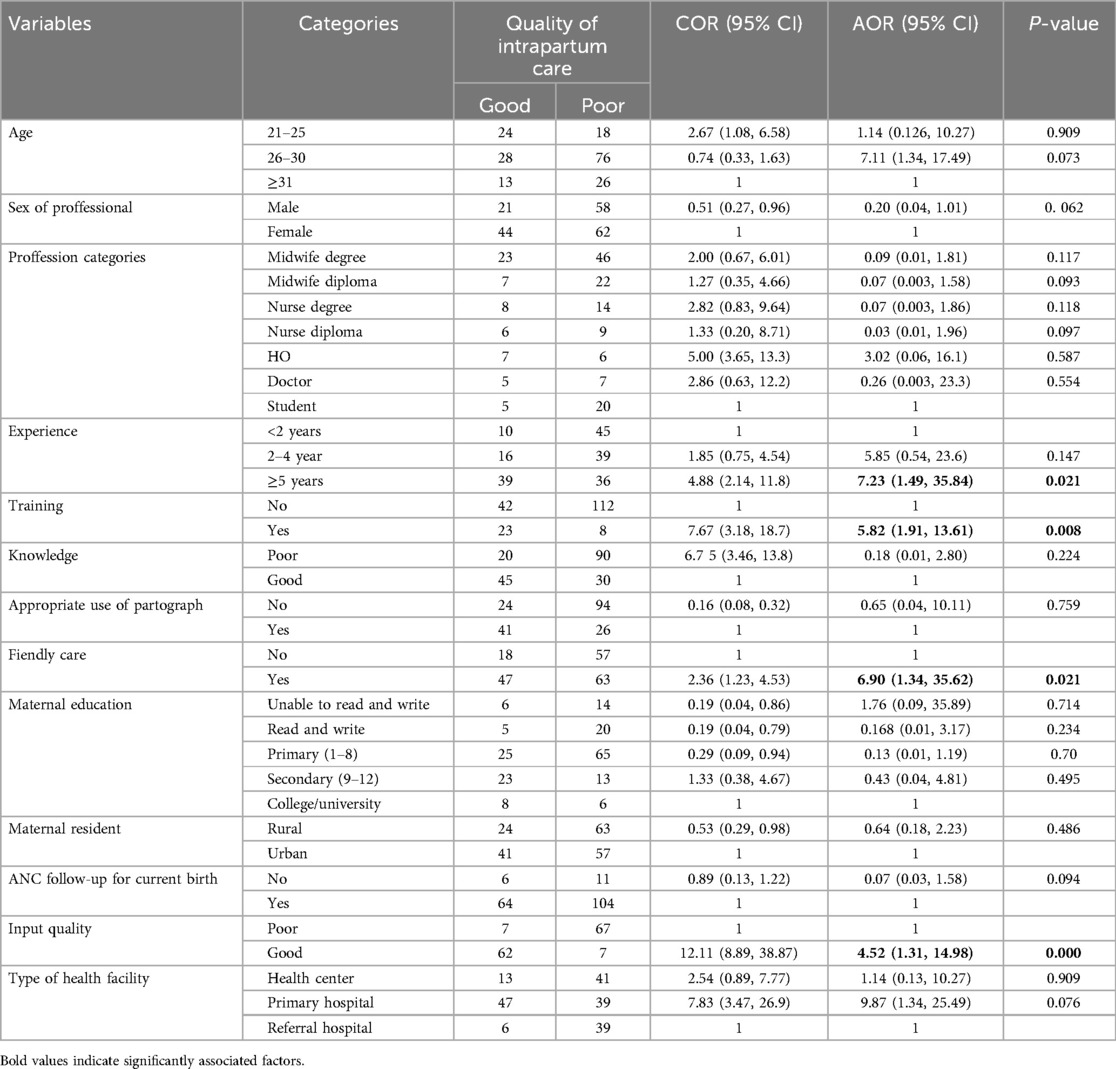
Table 4. Binary and multilevel logistic regression model of factors associated with good-quality intrapartum care in public health facilities Wolkite town, Central Ethiopia, 2023 (N = 185).
The finding of this study indicates that some institutions met the requirements to give high-quality care based on the standards of care in one dimension but not in others. This study shows that none of the skilled healthcare professionals have received the capacity building to manage obstetric complication training in all health institutions and that only one (20%) facility skilled birth attendant was trained to manage neonatal resuscitation to provide quality care, which is consistent with the findings of a study conducted in Addis Ababa, where none of the skilled birth attendants had completed all components of Comprehensive Emergency Obstetric and Newborn Care (CEMONC) training (34). The similarity in the governing health system could be a contributing factor.
In this study, three (60%) of the health facilities met the necessary input quality aspect, which was comparable with a study conducted in Bangladesh where only 57.1% and 52.7% of district hospitals and maternity and child welfare centers met all items of infrastructure, respectively (35). The finding of this study is also consistent with that of another study conducted in Zanzibar, where out of five hospitals, only 60% fulfilled the minimum standards of a skilled healthcare provider (36). The argument is based on the fact that all of the above nations are African nations with comparable economic prospects to the region under investigation. This shows that infrastructure is influenced by the economy of the countries. In contrast, a study in Jabi Tehinan district, Ethiopia, indicated that 49% of mothers had access to good-quality human and material resources (37).
In this study, only 40% of the facilities had water accessibility in delivery wards, similar to a study in Nigeria where only 38% of facilities had running water near the delivery ward (38). However, a study in Tanzania and Kenya showed that only 7% and 18% of facilities had water accessibility, respectively (39). In this study, only 40% and 80% of facilities had functional incubators and bags/masks for newborn resuscitation, respectively, similar to a study in Kenya, where only 50% and 80% of the hospitals had incubators and bags/masks for newborn resuscitation (40). Such variation could occur as a result of the system’s strength and the focus on healthcare service. In this study, only two (40%) health facilities provided towels for drying and covering the babies immediately after birth. This finding was in line with another study conducted in southern Ethiopia where 45.6% of mothers dried their babies with prepared towels (41). A study conducted in six sub-Saharan African countries revealed that the largest gap in newborn care was the lack of towels for drying the newborns (42), which is a basic action for preventing hypothermia.
Developing detailed and written standards of care is crucial for good-quality care at the time of childbirth, and the process aspect is actual intrapartum care between provider and client interaction (28). In this study, only 35.1% (95% CI: 28.3%, 41.9%) of mothers received good-quality intrapartum care, which was consistent with a study conducted in the northern part of Ethiopia in which only 31.25% of health facilities met process quality care (28). The similarity in the governing health system, the low levels of health professional's skills, and the comparably poor health infrastructure could be contributing factors. On the other hand, the finding is higher than that in a study in Ghana in which only 18% of health facilities met process quality care (43) and lower than that in a study in Ethiopia in the Wolayta zone in which only 40.8% of mothers received the standard care (44). The incompetence of the healthcare experts, an insufficient quantity of healthcare professionals, and the lack of quality monitoring could be causes of poor-quality intrapartum care (45).
The lack of adherence to recommended infection prevention procedures puts healthcare professionals, clients, and the general public at a greater risk of contracting infection and illness and leads to low-quality care. In this study, infection prevention practices, such as hand washing before physical examination, were performed only for 8.1% of mothers and only for 31 (16.8%) of mothers before delivery. This was similar to a study in Côte d'Ivoire where only 6.71% of caregivers practiced washing their hands before the examination (46). This study showed that proper gloving on both hands before vaginal examination was practiced only for 46.5% of mothers, which is higher than that in a study in Burkina Faso where 7.96% of care providers used sterile gloves for vaginal examinations (46). This could be caused by the different types of facilities including study settings and the lack of skilled care providers.
In this study, proper partograph utilization was 39.5% (95% CI: 32.4%, 46.9%), which was higher than that in various studies conducted in different regions of Ethiopia where 10.1%, 25%, and 23.8% of the facilities used partograph properly (28, 47, 48). This variation could be due to the availability of well-planned and executed programs, effectiveness of mentoring, supportive supervision, and commitment towards using partographs routinely for each laboring mother.
The result of this study showed that only 57.8% (95% CI: 50.4%, 65%) of mothers and newborns experienced friendly care throughout delivery and the immediate postpartum period. This finding is higher than that in a study carried out in Tigray, which revealed that only 47.2% of mothers and newborns experienced friendly care throughout delivery (31). This could have an impact on future prenatal, delivery, and postpartum maternal health service consumption and reduce maternal and infant mortality. The result of this study showed that only 29.2% of mothers were allowed companionship during delivery, which was higher than that in a study in Arbaminch town (13.8%), Ethiopia, and this finding was similar to the findings of a study in Kenya and Bangladesh where only 29% and 39% of mothers were allowed companionship during childbirth, respectively (49–51). The closeness between these findings could be due to the actual quality of care that was delivered during childbirth.
In this study, the overall immediate postnatal care for the women and their newborns before discharge from the health facilities was only 49.2% (95% CI: 42.2%, 56.2%), which was higher than that in a study done in theWolaita zone (34.9%) in Southern Ethiopia (52). The reported discrepancy is related to the scope of the studies, study sites, and the components of quality measurement indices. Since, postpartum hemorrhage is a danger that all newly delivered mothers face, the WHO postnatal guidelines recommend that all postpartum women have a routine screening for vaginal bleeding, uterine contraction, temperature, and pulse rate during the first 24 h (13). In this study, only 68.1% of mothers were checked for uterine contraction. This suggests that care providers are missing procedures, underperforming, or neglecting to provide care for mothers within the immediate postpartum period. However, the finding was higher than that in another study conducted in Tigray region primary hospitals at 45.5% (53). This variation could be due to different study setting and study time. This indicates the need to have regular updating and auditing in the clinical areas to ensure the best standard care practices.
The overall newborn quality of care in this study was 69.7% (95% CI; 62.6%, 76.3%). The finding is almost similar to that of a study in Tigray in that 67.6% of newborns received good-quality newborn care (31). It is higher than that of a study conducted in West Guji which showed that the good-quality essential newborn care was only 17.9% (54). This discrepancy in the outcome could be caused by differences in the measuring criteria used to determine the quality of newborn care, the type of health institutions, the study sample employed, and the study setting.
This study found that 38.4% of newborns were ensured skin-to-skin contact with their mothers, similar to a study in other regions of Ethiopia which showed that only 35% of newborns had skin-to-skin contact with their mothers (11). In contrast, this finding is lower than that in a study conducted in Kenya in which 57% of newborns received skin-to-skin contact with their mothers after childbirth (55). Although they received capacity-building training and are aware of the benefits of skin-to-skin contact, most healthcare professionals have not implemented behavioral changes to comply with the criteria, which could be the cause of this mismatch.
This study found that input quality, training, health professional experience, and maternal- and newborn-friendly care were significant predictors of good-quality intrapartum and newborn care. The findings of this study show that health facilities with good input quality care provided better intrapartum and newborn care. Facilities with good infrastructure and other resources were more likely to provide better quality care than their counterparts (56). Healthcare providers who received training in partographs, basic emergency obstetric and infant care training, and proper training in evidence-based intrapartum care provided better intrapartum and newborn care than their counterparts. This finding is supported by a study conducted in another region of Ethiopia (57).
Additionally, this research showed that care provider's experience were independent predictors of observed intrapartum and newborn care quality. This finding was supported by a study conducted in Wolayta zone, Southern Ethiopia (44). The study indicated that maternal- and newborn-friendly care was also a significant predictor of observed service quality. This finding was in line with a study conducted in Tigray which revealed that mother- and infant-friendly care services was one of the independent predictors of quality intrapartum and newborn care (31, 33).
This study aimed to evaluate various aspects of quality, including the availability of basic infrastructure, essential medications and instruments, the competence of providers (process), and predictors of good-quality intrapartum care. Different approaches (interview, service provision observation, and document review) were used for specific purposes. The study included all of the public health facilities in Wolkite town to make them representative of the findings. The use of the two aspects of quality (input and process) and their association was the most advantageous aspect of this study.
A limitation of this study is the possibility of observer bias among data collectors and the Hawthorne effect. However, to reduce this impact, the first three observations from each skilled attendant were excluded. The observation aspect of this study did not include caesarian section deliveries. The majority of laboring women arrived at the facility after the first stage of labor had been completed at home, which necessitated extending the data collection period to recruit enough participants to meet the sample size. Additionally, it is difficult to observe the second stage of lobar when some laboring mothers elect to have a cesarean section. The application of multilevel analysis would have helped identify individual- and group-level factors associated with the quality of intrapartum care.
The quality of intrapartum and newborn care in this study area was suboptimal. Clients are not receiving intrapartum care with state-of-the-art knowledge and current clinical best practices. Input quality, training, health professional experience, and maternal- and newborn-friendly care were significant predictors of good-quality intrapartum and newborn care. The local and national health systems should focus on improving the infrastructure of public health institutions including the sustainable provision of medicines, basic supplies, diagnostic services, and water and sanitary facilities required for maternal and newborn care. Additionally, regular monitoring of health facilities is crucial to improve the quality of intrapartum and newborn care provided. Care providers' adherence to the standard procedures and guidelines should be improved through training, supervision, and regular monitoring and evaluation. It is also important to implement respectful maternity care to improve intrapartum care by supporting mothers during delivery, ensuring consented care, and preventing abandonment of care. Further studies should be conducted to identify additional factors affecting the utilization of quality intrapartum and newborn care.
The original contributions presented in the study are included in the article/Supplementary Material; further inquiries can be directed to the corresponding author.
Ethical clearance was obtained from the institutional review board (IRB) of Addis Ababa University, College of Health Science, School of Public Health. This study was conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
BM: Conceptualization, Data curation, Formal Analysis, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. AZ: Data curation, Formal Analysis, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. AK: Data curation, Formal Analysis, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. MG: Data curation, Formal Analysis, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. AN: Data curation, Formal Analysis, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing. TM: Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing, Data curation, Formal Analysis.
The author(s) declare that no financial support was received for the research and/or publication of this article.
We would like to acknowledge the study participants for their kind and respected responses.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fgwh.2025.1444184/full#supplementary-material
Supplementary File S1 | SPSS data set for the study of quality of intrapartum and newborn care in public healthcare facilities of Wolkite town, Gurage Zone, Central Ethiopia.
Supplementary File S2 | File All items used for the study of quality of intrapartum and newborn care in public healthcare facilities of Wolkite town, Gurage Zone, Central Ethiopia.
ANC, antenatal care; BEMONC, basic emergency obstetric and newborn care; CEMONC, comprehensive emergency obstetric and newborn care; FMoH, Federal Ministry of Health; HO, health officer; IRB, institutional review board; LMIC, low- and middle-income countries; MNH, maternal and newborn health; NQS, national quality strategy; SBA, skilled birth attendant; SDG, sustainable development goal; WHO, World Health Organization.
1. World Health Organization. Continuity and Coordination of Care: A Practice Brief to Support Implementation of the WHO Framework on Integrated People-Centred Health Services. Geneva: World Health Organizaton (2018). CC BY-NC-SA 3.0 IGO.
2. World Health Organization. WHO Recommendations on Intrapartum Care for a Positive Childbirth Experience. Geneva: World Health Organization (2018).
3. World Health Organization. Standards for Improving Quality of Maternal and Newborn Care in Health Facilities. Geneva: World Health Organization Lancet (2016).
4. Tuncalp Ö, Were WM, MacLennan C, Oladapo OT, Gulmezoglu AM, Bahl R, et al. Quality of care for pregnant women and newborns—the WHO vision. Br J Obstet Gynaecol. (2015) 122:1045–9. doi: 10.1111/1471-0528.13451
5. Wilson A, Spotswood N, Hayman G, Vogel J, Narasia J, Elijah A, et al. Improving the quality of maternal and newborn care in the Pacific region: a scoping review. Lancet Reg Health West Pac. (2020) 3:100028. doi: 10.1016/j.lanwpc.2020.100028
6. World Health Organization. Improving Maternal and Newborn Health and Survival and Reducing Stillbirth: Progress Report 2023. Geneva: World Health Organization (2023).
7. World Health Organization. Strategies Towards Ending Preventable Maternal Mortality (EPMM). Geneva: World Health Organization (2015).
8. World Health Organization. Trends in Maternal Mortality 2000–2017: Estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division. Switzerland: Executive Summary (2019). Available at: https://coilink.org/20.500.12592/f4sp5q
9. Blencowe H, Cousens S, Jassir FB, Say L, Chou D, Mathers C, et al. National, regional, and worldwide estimates of stillbirth rates in 2015, with trends from 2000: a systematic analysis. Lancet Glob Health. (2016) 4(2):e98–108. doi: 10.1016/S2214-109X(15)00275-2
10. Chou VB, Walker N, Kanyangarara M. Estimating the global impact of poor quality of care on maternal and neonatal outcomes in 81 low-and middle-income countries: a modeling study. PLoS Med. (2019) 16(12):e1002990. doi: 10.1371/journal.pmed.1002990
11. Biadgo A, Legesse A, Estifanos AS, Singh K, Mulissa Z, Kiflie A, et al. Quality of maternal and newborn health care in Ethiopia: a cross-sectional study. BMC Health Serv Res. (2021) 21(1):1–10. doi: 10.1186/s12913-021-06680-1
12. Austin A, Langer A, Salam RA, Lassi ZS, Das JK, Bhutta ZA. Approaches to improve the quality of maternal and newborn health care: an overview of the evidence. Reprod Health. (2014) 11:1–9. doi: 10.1186/1742-4755-11-S2-S1
13. World Health Organization. Department of Maternal, Newborn, Child and Adolescent Health (MCA): Progress Report 2014–15. Geneva: World Health Organization (2016).
15. Negero MG, Sibbritt D, Dawson A. Access to Quality Maternal Healthcare Services in Ethiopia: A Multilevel Analysis (2022). doi: 10.21203/rs.3.rs-1627642/v1
16. Lindtjørn B, Mitiku D, Zidda Z, Yaya Y. Reducing maternal deaths in Ethiopia: results of an intervention programme in southwest Ethiopia. PLoS One. (2017) 12(1):e0169304. doi: 10.1371/journal.pone.0169304
17. Brenner S, De Allegri M, Gabrysch S, Chinkhumba J, Sarker M, Muula AS. The quality of clinical maternal and neonatal healthcare–a strategy for identifying “routine care signal functions”. PLoS One. (2015) 10(4):e0123968. doi: 10.1371/journal.pone.0123968
18. FMOH. 7. National Antenatal Care Guidelines for Ensuring Positive Pregnancy Experience. (2022). Vol. 80.
19. (PHEM): EPHI-PHEMC. Ethiopian National Maternal Death Surveillance and Response System Annual Report 2010 Ethiopian Fiscal Year. (2019). Available at: https://wwwafrowhoint/publications/ethiopia-national-maternal-death-surveillance-andresponse-system-annual-report-2010 (Accessed December 2, 2024).
20. MoH Ethiopia. Health Sector Transformation in Quality: A Guide to Transform the Quality of Healthcare in Ethiopia. Addis Ababa (2016).
21. National Academies of Sciences, Engineering, and Medicine. Improving Quality of Care in Low- and Middle-Income Countries: Workshop Summary. Washington, DC: The National Academies Press (2015). doi: 10.17226/21736
22. Donabedian A. Evaluating the quality of medical care. 1966. Milbank Q. (2005) 83(4):691–729. doi: 10.1111/j.1468-0009.2005.00397.x
23. Tilahun B, Zeleke A, Kifle M, Fritz F. The Ethiopian national eHealth strategy and its alignment with the health informatics curriculum. J Health Inform Afr. (2014) 2(2):1–6. doi: 10.12856/JHIA-2014-v2-i2-100
24. Alyahya MS, Khader YS, Batieha A, Asad M. The quality of maternal-fetal and newborn care services in Jordan: a qualitative focus group study. BMC Health Serv Res. (2019) 19(1):425. doi: 10.1186/s12913-019-4232-9
25. Bitew K, Ayichiluhm M, Yimam K. Maternal satisfaction on delivery service and its associated factors among mothers who gave birth in public health facilities of Debre Markos town, northwest Ethiopia. Biomed Res Int. (2015) 2015:460767. doi: 10.1155/2015/460767
26. Asres GD. Satisfaction and associated factors among mothers delivered at Asrade Zewude Memorial Primary Hospital, Bure, West Gojjam, Amhara, Ethiopia: a cross sectional study. Asres. Prim Health Care. (2018) 8:2. doi: 10.4172/2167-1079.1000293
27. Silesh M, Lemma T. Maternal satisfaction with intrapartum care and associated factors among postpartum women at public hospitals of north Shoa zone Ethiopia. PLoS One. (2021) 16(12):e0260710. doi: 10.1371/journal.pone.0260710
28. Fisseha G, Berhane Y, Worku A, Terefe W. Quality of the delivery services in health facilities in northern Ethiopia. BMC Health Serv Res. (2017) 17(1):187. doi: 10.1186/s12913-017-2125-3
29. Amsalu B, Aragaw A, Sintayehu Y, Sema A, Belay Y, Tadese G, et al. Respectful maternity care among laboring women in public hospitals of Benishangul Gumuz region, Ethiopia: a mixed cross-sectional study with direct observations. SAGE Open Med. (2022) 10:20503121221076995. doi: 10.1177/20503121221076995
30. UNICEF. WHO Guidelines Approved by the Guidelines Review Committee. Pregnancy, Childbirth, Postpartum and Newborn Care: A Guide for Essential Practice. Geneva: World Health Organization (2015).
31. Fisseha G, Berhane Y, Worku A. Quality of intrapartum and newborn care in Tigray, northern Ethiopia. BMC Pregnancy Childbirth. (2019) 19(1):37. doi: 10.1186/s12884-019-2184-z
32. Germossa GN, Wondie T, Gerbaba M, Mohammed E, Alemayehu WA, Tekeste A, et al. Availability of comprehensive emergency obstetric and neonatal care in developing regions in Ethiopia: lessons learned from the USAID transform health activity. BMC Health Serv Res. (2022) 22(1):1307. doi: 10.1186/s12913-022-08712-w
33. Asmare Y, Tilahun T, Debela Y, Eshetie Y, Minuye B, Yalew ZM, et al. Quality of intrapartum care at public health institutions of North Achefer district, north west Ethiopia: a mixed method study. BMC Pregnancy Childbirth. (2022) 22(1):626. doi: 10.1186/s12884-022-04907-5
34. Austin A, Gulema H, Belizan M, Colaci DS, Kendall T, Tebeka M, et al. Barriers to providing quality emergency obstetric care in Addis Ababa, Ethiopia: healthcare providers’ perspectives on training, referrals and supervision, a mixed methods study. BMC Pregnancy Childbirth. (2015) 15(1):1–10. doi: 10.1186/s12884-015-0493-4
35. Farzana Islam AR, Halim A, Eriksson C, Rahman F, Dalal K. Assessment of quality of infrastructure and clinical care performance of HCPs during MNH services at district and sub-district level government hospitals, Bangladesh. HealthMED. (2015) 9:12.
36. Housseine N, Punt MC, Mohamed AG, Said SM, Maaløe N, Zuithoff NPA, et al. Quality of intrapartum care: direct observations in a low-resource tertiary hospital. Reprod Health. (2020) 17(1):36. doi: 10.1186/s12978-020-0849-8
37. Asrese K. Quality of intrapartum care at health centers in Jabi Tehinan district, north west Ethiopia: clients’ perspective. BMC Health Serv Res. (2020) 20(1):439. doi: 10.1186/s12913-020-05321-3
38. Ifeadike CO, Ezeama NN, Nnaji GA, Emelumadu OF, Ugwoke U, Ofoegbu C. An assessment of reproductive health services in selected health facilities, Anambra state, Nigeria. Res J Womens Health. (2016) 3(2):1–8. doi: 10.7243/2054-9865-3-2
39. Gon G, Restrepo-Méndez MC, Campbell OM, Barros AJ, Woodd S, Benova L, et al. Who delivers without water? A multi country analysis of water and sanitation in the childbirth environment. PLoS One. (2016) 11(8):e0160572. doi: 10.1371/journal.pone.0160572
40. Gao X, Kelley DW. Understanding how distance to facility and quality of care affect maternal health service utilization in Kenya and Haiti: a comparative geographic information system study. Geospat Health. (2019) 14(1). doi: 10.4081/gh.2019.690
41. Chichiabellu TY, Mekonnen B, Astawesegn FH, Demissie BW, Anjulo AA. Essential newborn care practices and associated factors among home delivered mothers in Damot Pulasa Woreda, southern Ethiopia. Reprod Health. (2018) 15(1):1–11. doi: 10.1186/s12978-018-0609-1
42. de Graft-Johnson J, Vesel L, Rosen HE, Rawlins B, Abwao S, Mazia G, et al. Cross-sectional observational assessment of quality of newborn care immediately after birth in health facilities across six sub-Saharan African countries. BMJ Open. (2017) 7(3):e014680. doi: 10.1136/bmjopen-2016-014680
43. Nesbitt RC, Lohela TJ, Manu A, Vesel L, Okyere E, Edmond K, et al. Correction: quality along the continuum: a health facility assessment of intrapartum and postnatal care in Ghana. PLoS One. (2015) 10(10):e0141517. doi: 10.1371/journal.pone.0141517
44. Alemayehu M, Yakob B, Khuzwayo N. Quality of emergency obstetric and newborn care services in Wolaita zone, southern Ethiopia. BMC Pregnancy Childbirth. (2022) 22(1):686. doi: 10.1186/s12884-022-05019-w
45. Brizuela V, Leslie HH, Sharma J, Langer A, Tunçalp Ö. Measuring quality of care for all women and newborns: how do we know if we are doing it right? A review of facility assessment tools. Lancet Glob Health. (2019) 7(5):e624–32. doi: 10.1016/S2214-109X(19)30033-6
46. Millogo T, Agbre-Yace ML, Kourouma RK, Yameogo WME, Tano-Kamelan A, Sissoko FB, et al. Quality of maternal and newborn care in limited-resource settings: a facility-based cross-sectional study in Burkina Faso and Cote d'Ivoire. BMJ Open. (2020) 10(6):e036121. doi: 10.1136/bmjopen-2019-036121
47. Yigzaw T, Abebe F, Belay L, Assaye Y, Misganaw E, Kidane A, et al. Quality of midwife-provided intrapartum care in Amhara regional state, Ethiopia. BMC Pregnancy Childbirth. (2017) 17(1):261. doi: 10.1186/s12884-017-1441-2
48. Zelellw DA, Tegegne TK. Level of partograph utilization and its associated factors among obstetric caregivers at public health facilities in East Gojam zone, northwest Ethiopia. PLoS One. (2018) 13(7):e0200479. doi: 10.1371/journal.pone.0200479
49. Afulani P, Kusi C, Kirumbi L, Walker D. Companionship during facility-based childbirth: results from a mixed-methods study with recently delivered women and providers in Kenya. BMC Pregnancy Childbirth. (2018) 18(1):150. doi: 10.1186/s12884-018-1806-1
50. Beyene Getahun K, Ukke GG, Alemu BW. Utilization of companionship during delivery and associated factors among women who gave birth at Arba Minch town public health facilities, southern Ethiopia. PLoS One. (2020) 15(10):e0240239. doi: 10.1371/journal.pone.0240239
51. Perkins J, Rahman AE, Mhajabin S, Siddique AB, Mazumder T, Haider MR, et al. Humanised childbirth: the status of emotional support of women in rural Bangladesh. Sex Reprod Health Matters. (2019) 27(1):1610277. doi: 10.1080/26410397.2019.1610277
52. Dewana Z, Gebremariam A, Abdulahi M, Fikadu T, Facha W. Quality of delivery service at public health facilities in Arba Minch district, Gamo Gofa zone, southern Ethiopia. J Gynecol Obstetr. (2017) 5(2):31–6. doi: 10.11648/j.jgo.20170502.12
53. Berhe A, Araya T, Tesfay K, Bayray A, Etsay N, Gidey G, et al. Assessment of quality of postnatal care services offered to mothers in hospitals, of Tigray Ethiopia 2016. Res Rev. (2017) 6(1):11–9. doi: 10.37591/rrjomst.v6i1.1225
54. Rajan DR, Jaldo D, Gemechu T, Kasimayan P, Kanapathy A, Kasirajan T. Quality of essential newborn care and its associated factors in public health facilities of west Gujji, Oromia, Ethiopia: a cross sectional study. Ann Roman Soc Cell Biol. (2021) 25(4):7616–29.
55. Shikuku DN, Milimo B, Ayebare E, Gisore P, Nalwadda G. Quality of care during neonatal resuscitation in Kakamega county general hospital, Kenya: a direct observation study. Biomed Res Int. (2017) 2017:2152487. doi: 10.1155/2017/2152487
56. Kassaw A, Debie A, Geberu DM. Quality of prenatal care and associated factors among pregnant women at public health facilities of Wogera district, northwest Ethiopia. J Pregnancy. (2020) 2020:9592124. doi: 10.1155/2020/9592124
Keywords: quality, intrapartum, newborn, care, Ethiopia
Citation: Mulat BS, Zewdie A, Kasahun AW, Gashu M, Nega A and Melis T (2025) Quality of intrapartum and newborn care in public healthcare facilities of Wolkite town, Central Ethiopia: facility-based cross-sectional study. Front. Glob. Women's Health 6:1444184. doi: 10.3389/fgwh.2025.1444184
Received: 2 July 2024; Accepted: 28 February 2025;
Published: 18 March 2025.
Edited by:
Sk Masum Billah, International Centre for Diarrhoeal Disease Research (ICDDR), BangladeshReviewed by:
Stephen Okumu Ombere, Maseno University, KenyaCopyright: © 2025 Mulat, Zewdie, Kasahun, Gashu, Nega and Melis. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Berhanu Semra Mulat, YnJpc2hzZW1AZ21haWwuY29t
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.