- Department of Midwifery, Asrat Weldeyes Health Science Campus, Debre Berhan University, Debre Birhan, Ethiopia
Background: Menstrual irregularity can occur at any age, but it is most common among women under the age of 23 years. Menstrual irregularity is a foremost gynecological problem and a cause of anxiety to students and those close to them. These students experience monthly absenteeism, premenstrual symptoms, and a lack of concentration due to menstrual problems, all of which interfere with their education. Therefore, this study aimed to assess the magnitude of menstrual irregularity and associated factors among college students in Debre Berhan Town, North Shewa, Amhara Regional State, Ethiopia, in 2021.
Methods: An institution-based cross-sectional study was conducted from June to July 2021 in Debre Berhan town. Data was collected using self-administered questionnaires in 420 eligible female college students by systematic random sampling technique. Weight and height were measured and Body Mass Index (BMI) was calculated after data collection. Each questionnaire was checked for completeness, cleaned, coded, entered into EPI-DATA, and then transported to SPSS software. Bi-variable and multivariable logistic regression analyses were employed to determine the association of each independent variable with the dependent variable. P ≤ 0.05 were used to declare association and select predictors.
Results: In the current study, 395 students participated with a response rate of 93.6%. Of all the total respondents, the magnitude of menstrual cycle irregularity was 33.4% (95% CI 28.6–38.2). Age < 20 years old [AOR = 3.88, 95% CI (1.25–12.18)], age of menarche ≤ 12 years [AOR = 4, 95% CI (1.18–13.9), sleeping hours ≤ 5 h [AOR= 2.26, 95% CI (1.04–4.93)], perceived stress [AOR = 2, 95% CI (1.53–3.23)] and being overweight [AOR = 2, 95% CI (1.13–3.23) were the variables significantly associated with the magnitude of menstrual irregularity.
Conclusion and recommendation: This study shows that more than one-third of the college students in Debre Berhan town have experienced menstrual irregularity. Being less than 20 years old, having a history of early menarche, being overweight, and perceived stress were a variable significantly associated with menstrual irregularity. To control menstrual irregularity, girls should control their weight and lead a healthy lifestyle, including getting adequate sleep which could be aided by training on time management.
Introduction
The menstrual cycle is the monthly set of changes that a woman's body undergoes in preparation for pregnancy. Hormones cause the lining of the uterus to become thicker with extra blood and tissue. The uterine lining sheds through the vaginal opening if ovulation occurs and the egg is not fertilized. The release of blood and tissue from the lining of the uterus is a menstrual period (1, 2).
Normal menstruation can last from 2 to 7 days and can happen every 21–35 days (1). However, 14–25 percent of women have irregular menstrual cycles, which means their periods are heavier or lighter than usual, longer than 35 days or shorter than 21 days, or they have other issues, such as abdominal cramps (3). In addition, bleeding or spotting in between periods, bleeding or spotting after sex, menstrual cycle length varying by more than 7–9 days, and/or not having a period for 3–6 months are menstrual irregularities (1, 3, 4).
At any age, menstrual irregularity can occur. However, it is usual for a woman's periods to be irregular at particular times in her life. When a girl initially starts having periods, they may not come on a regular basis (5). The anovulatory cycle, which is linked to the immaturity of the hypothalamic-pituitary-ovarian axis, is the most common cause of abnormal uterine bleeding (AUB) in adolescents during the first 19 months of menstruation. The common cause of AUB is a miscarriage, ectopic pregnancy, infection, hormonal contraception, stress, bleeding disorders, and endocrine disorders (6). Menstrual problems and AUB are two of the most common gynaecologic issues among teenagers (7).
Women under the age of 23 were the most likely to have menstrual irregularity (5). Menstrual irregularity was reported to be widespread in 35.7 and 64.2 percent of women in India and Nepal, respectively, according to several studies (8, 9). In addition, the prevalence of menstrual irregularity in Sudan was 55 percent (10). Furthermore, menstrual irregularity was reported to be prevalent in Ethiopia at 26.5–32.6 percent. Lack of adequate sleep, alcohol intake, stress, Anemia, hereditary factors, and being underweight are major contributing factors to menstrual irregularity (11–13).
Female students face many problems that challenge their quality of life and academic performance. Of the problems that affect the quality of life of female students, menstrual cycle irregularity is a foremost gynecological problem and a cause of anxiety to students and those close to them (14). It affects the different day-to-day events of students (15, 16). Different studies revealed that menstrual irregularities can also affect issues later on in life, such as osteoporosis, infertility, future diabetes mellitus, and cardiovascular disease (14, 17, 18).
College students have reported menstrual discomfort, feelings of guilt and sadness, and difficulty containing menses as bad menstrual experiences. These factors adversely affect their education through absenteeism, reduced engagement, and poor academic performance. Menstruation, on the other hand, can be a pleasant experience for some students, and their capacity to adjust to dysmenorrhea's problems indicates their perseverance and ingenuity. Monthly absenteeism, premenstrual symptoms, and lack of concentration cause issues in studies (19). As a result, this study aimed to assess the magnitude of menstrual irregularity using the International Federation of Gynecology and Obstetrics menstrual guidelines parameters for normal and abnormal uterine bleeding 2018's standard of menstrual irregularity definition (20).
Methods and materials
Study design, settings, and participants
An institutional-based cross-sectional study design was conducted at colleges in the Debre Berhan town from June to July 2021. Debre Berhan Town is the capital of the North Shewa Zone in the Amhara regional state, which is 130 km away from the capital of Ethiopia, Addis Ababa. There were three public colleges in the town and, during the physical year, the total population of the study area was 2,755.
Population
All regular college students in Debre Berhan town during the study period were a study population. Students who were pregnant, had delivered, and were breastfeeding during the study year, had a history of menstrual irregularity therapy, or were using hormonal contraceptives throughout the data-collecting period were excluded from the study.
Sample size and sampling procedures
The sample size was calculated using a formula for estimating a single population proportion with a 95 percent confidence interval, a 5% margin of error, and the prevalence of menstrual irregularity as 50% and a 10% no-response rate. The total number of people in the sample was determined to be 422. All colleges in Debre Berhan Town were included in the study. The sampling allocation was also made based on the number of students in each college. For this study, a systematic random sampling method was used. Of all colleges, there were 2,755 (N) female students. The sample size was 420 (n); therefore, the skip interval was calculated as K = N/n where K, which is skipped interval, was seven. The starting point was chosen at random, and then everyone that corresponded to the skip interval was chosen starting from that point (Figure 1).
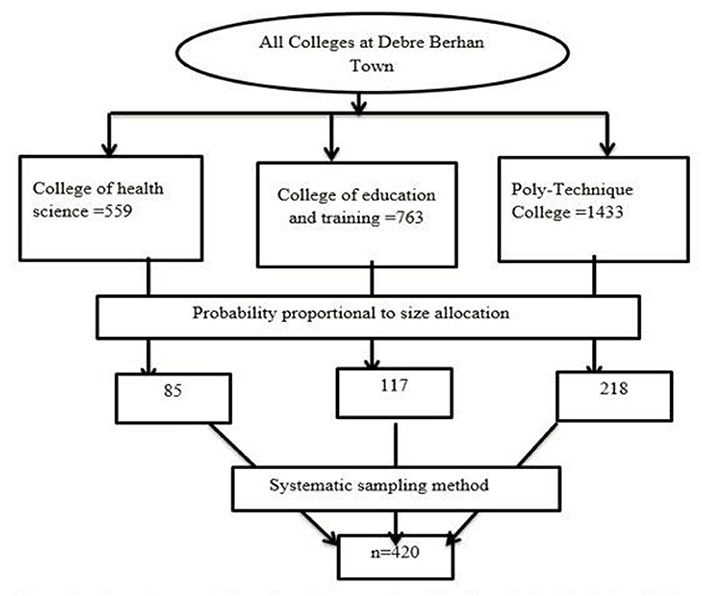
Figure 1. Schematic presentation of sampling procedure of college students in Debre Berhan town, 2021.
Data collection procedures
The data was collected using a pre-tested self-administered questionnaire. Anthropometric measurements were performed to calculate the body mass index (BMI) of the participants. The height of participants was measured in meters and weight was recorded close to 100 g (least count of electronic weighing scale = 100 g). After analyzing several works of literature, the questionnaire was first written in English, then translated into Amharic to ensure that it was appropriate for female students, and then back to English to ensure consistency by a third party. To meet the study's aims, the questionnaire was built based on the variables. Sociodemographic information, menstrual-related questions, lifestyle and behavioral questions, medical history inquiries, and anthropometric measurements are all included in the questionnaire (height and weight).
Data quality control and analysis
Every questionnaire was checked for completeness and consistency. As data collectors and supervisors, three diploma-trained midwives and one BSc-trained midwife were hired. The principal investigator provided data collectors and supervisors with training to address the study's relevance, objectives, and confidentiality concerns. Epi-Data was used to enter, edit, and clean data before being exported to SPSS version 21 for analysis. Frequencies were also subjected to descriptive statistics. Then, one by one, bivariate logistic regression was run between the dependent and independent variables. Variables with P < 0.25 in the bi-variable analysis were entered into a multivariable logistic regression to control the possible effect of confounders. Crude and adjusted odds ratios with h 95% confidence interval were computed. Finally, variables at p < 0.05 were considered statistically significant.
Outcome measurement
The International Federation of Gynecology and Obstetrics (FIGO) 2018 criteria for menstrual irregularity definition have been used to establish if the menstrual cycle is regular or irregular. As a result, in the current investigation, a regular menstrual cycle was defined as having a frequency of 24–38 days, a duration of bleeding of less than or equal to 8 days, a cycle-to-cycle variance of fewer than 10 days during the previous year, and a normal individual assessment of the quantity (20). Menstrual irregularity, on the other hand, refers to anything that occurs outside of the normal menstrual cycle.
Operational definition
Body mass index (BMI)
Body mass index (BMI) is defined is a measure for indicating nutritional status in adults. It is defined as a person's weight in kilograms divided by the square of the person's height in meters (kg/m2). Based on the calculated BMI, the study participants were classified as underweight (BMI < 18.5), normal weight (BMI 18.5–24.9), overweight (BMI 25–29.9), and obese (BMI ≥ 30) (21).
Perceived stress scale (PSS) assessed perceived stress
The PSS is a well-known stress assessment tool; it is a 10-item multiple-choice self-report psychological questionnaire used to assess stress perception. Each response was given a score ranging from 0 to 4. PSS is calculated by adding all scale items together. The total score ranges 0.0–21.0 [mean = 13.7 (± 6.6)]. The stress limit cut-off values were set at 15 (22).
Substance abuse
Substance abuse refers to the harmful or hazardous use of psychoactive substances, including alcohol and illicit drugs. One of the key impacts of illicit drug use on society is the negative health consequences experienced by its members. Drug use also puts a heavy financial burden on individuals, families, and society (23). Alcohol drinking was measured based on the frequency of alcohol drinking. Cigarette smoker was defined as someone who smokes cigarette either daily or occasionally.
Sleeping hour
Sleep duration was measured for just one sleep period or over the course of a 24-h day (24). We assessed the students' sleeping hours by asking, “How many hours do you sleep on average per day?”
Result
Socio-demographic characteristics
Three hundred ninety-five female students participated with a respondent rate of 93.6%. Most of the respondents (227 or 57.5%) were below 21 years old. The mean age of the study participants was 20.94 ± 2.10 years. The religion of most respondents 341 (90.9%) was orthodox. Regarding the respondents' ethnicity, 341 (86.3%), 39 (9.9%), and 15 (3.8%) were Amhara, Oromo, and Tigre, respectively. Of all participants, 86.3% were married. Concerning respondents' mothers' educational status, most of them 63.8% had no formal education, followed by primary education 26.8%. Regarding residence before college admission, 53.2% of them came from a rural area (Table 1).
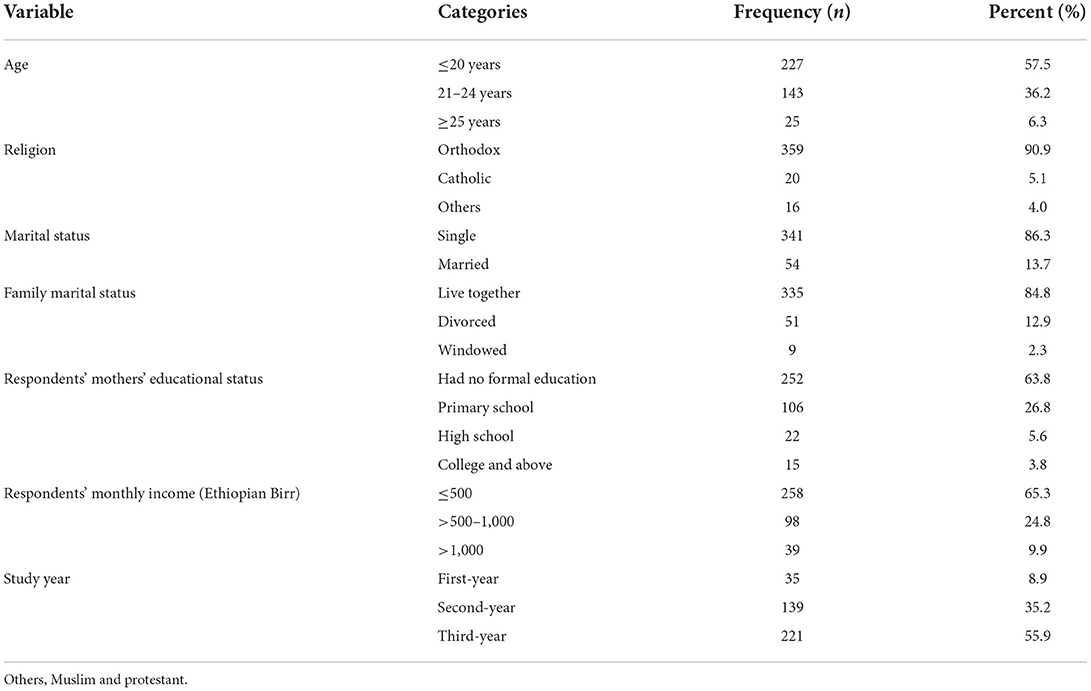
Table 1. Socio-demographic characteristics of female college students, Debre Berhan, Ethiopia 2021 (n = 395).
Body mass index
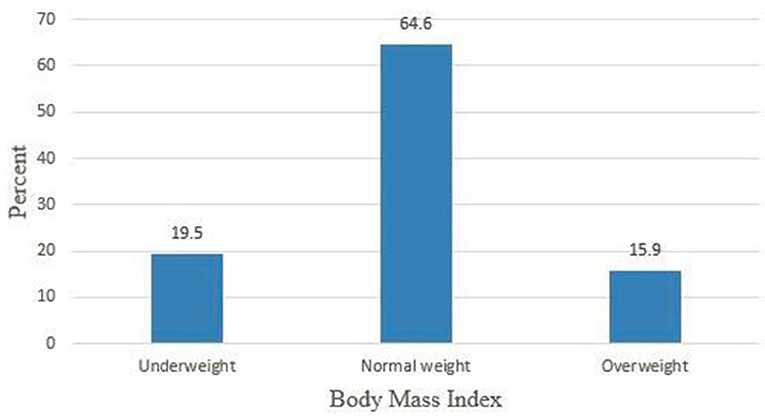
For all study respondents, body mass index was calculated and 77 (19.5%) respondents were underweight (Figure 2).
Perceived stress
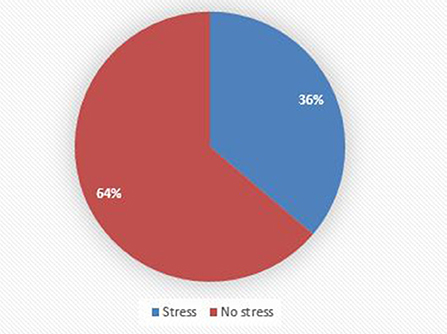
Out of the total respondents, 143 (36%) of college students had perceived stress (Figure 3).
Substance use
Around 16 percent of the total respondents had consumed alcohol in the past. Almost all (98.4%) individuals who had a history of drinking alcohol had consumed alcohol in the previous 30 days. The types of alcohol they drank were beer 30 (49.2%), wine 12 (19.7%), or traditional drinks like local beer. Concerning the frequency of drinking alcohol, 10 (16.4%), 30 (49.2%), and 21 (34.4%) of the respondents drunk daily, weekly, and monthly respectively. In this study, none of the respondents had chewed chat or smoked cigarettes.
Sleeping hours
Concerning the sleeping hours of the study respondents; 59 (14.9%), 212 (53.7%), and 124 (31.4%) of the respondents slept <5, 6–8, and 9 h and more per day, respectively.
Medical and gynecological history
Of all study respondents, 385 (97.5%) had no history of gynecological problems. Of those who had a history of gynecological problems, 10 (2.5%) of the respondents had a history of sexually transmitted disease. Ninety-two of the study respondents (23.3%) started sexual activity and around 8% of them used emergency contraceptives. Regarding the medical history of the respondents, 2 (0.5%), 10 (2.5%), and 11 (2.8%) had a history of Diabetic Mellitus, goiter, and head injury, respectively.
Patterns of the menstrual cycle
In this study, 132 (33.4%) [(95% CI 28.6–38.2)] of the respondents had an irregular menstrual cycle. Among those who had menstrual irregularity, 77 (58%) of the respondents had irregular onset and 16 (12.12%) of the respondents had heavy bleeding during menstruation. The mean age of menarche was 14.88 ± 1.419 years (Table 2).
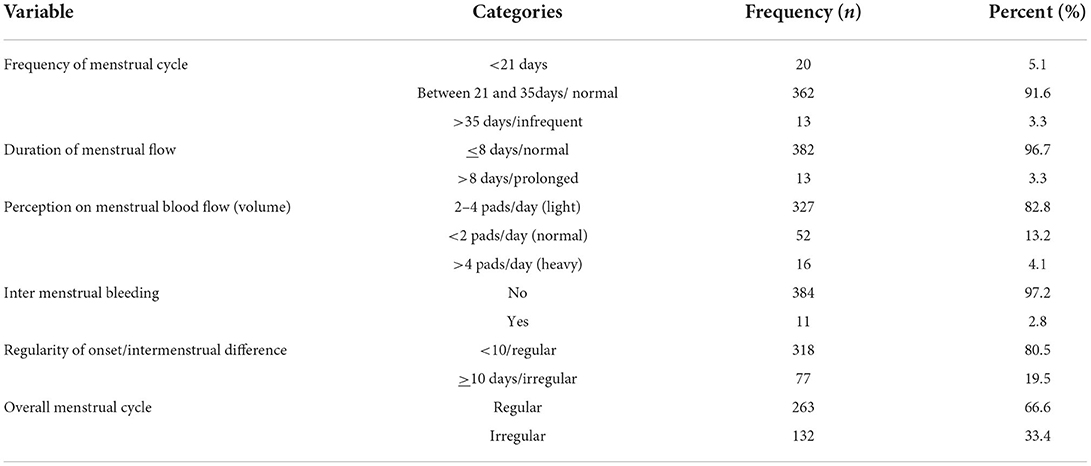
Table 2. Patterns of the menstrual cycle among female college students, Debre Berhan, Ethiopia, 2021 (n = 395).
Factors associated with menstrual irregularity
Bivariate analysis for each independent variable has been used to assess factors associated with menstrual irregularity, and then the age of respondent, body mass index, sleeping hour, age of menarche, psychological stress, residence, and head injury were statistically associated with menstrual cycle irregularity. Statistical significance was accepted at p < 0.25 (Table 3).
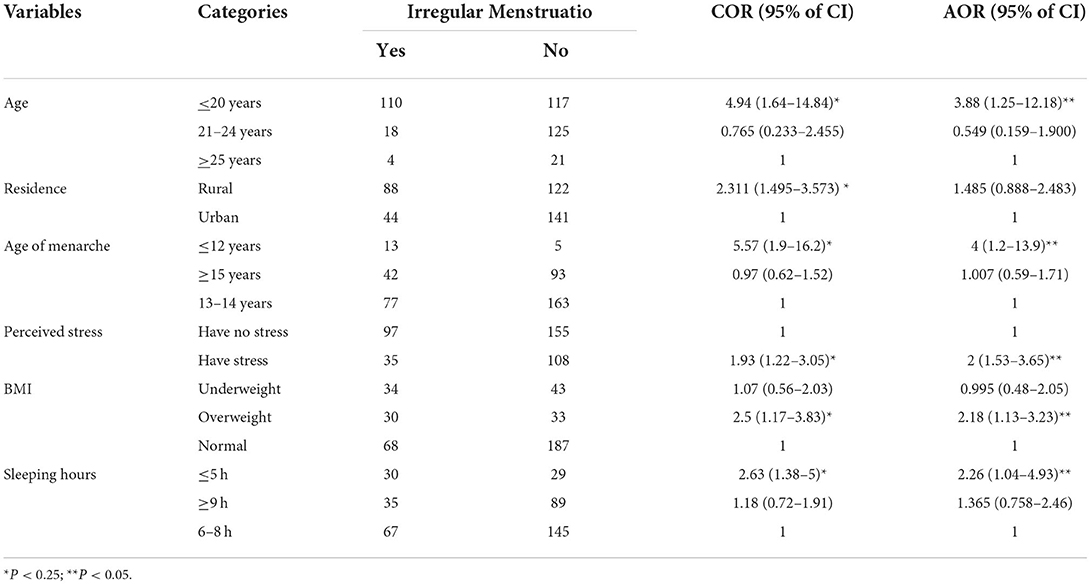
Table 3. Factors associated with menstrual irregularity of female college students, Debre Berhan, Ethiopia, 2021 (n = 395).
The above variables which showed a p < 0.25 during bivariate analysis were used in multivariate logistic regression to control confounders. Age of respondent, body mass index, sleeping hour, age of menarche, and psychological stress were the variables that showed significant association on multivariate logistic regression. The significant association was also declared at p < 0.05 (Table 3).
Students whose age was less than 20 years old were 3.88 times [AOR = 3.88, 95% CI (1.25–12.18)] more likely to experience irregular menstrual cycles than those aged 25 years and above. Those with menarche ≤12 years had 4 times greater [AOR = 4, 95% CI (1.18–13.9)] risk for menstrual irregularity than those who were seen with menses at 13–14 years old. Similarly, those respondents who were overweight were 2 times more likely [AOR =2.18, 95% CI (1.13–3.23)] to have more menstrual cycle irregularity as compared to those who were normal weight. On the other hand, participants who slept ≤ 5 h/days were 2.26 times [AOR = 2.26, 95 CI (1.04–4.93)] more likely to experience irregular menstrual cycles than those who were sleeping 6–8 h. per day. Finally, participants who had perceived stress were 2 times [AOR = 2, 95% CI (1.53–3.23)] more likely to have an irregular menstrual cycle than those who did not (Table 3).
Discussion
This institution-based cross-sectional study was done on menstrual cycle irregularity and associated factors among college students in Debre Berhan town. The magnitude of menstrual cycle irregularity in the current study is 33.4% (132). This finding is consistent with previous studies conducted in Ethiopia, Japan, and Saudi Arabia (11, 25, 26). However, the finding of the current study is lower than studies conducted in Ethiopia Bahir Dar University, Sudan, Malaysia, and Lebanon (10, 27–29). On the other hand, the current study is higher than the study conducted in Adama, and India studies (30, 31). These differences could be attributable to the respondents' age ranges, stress levels, where they live, or undiscovered medical and gynecological issues.
Students whose age was less than 20 years old were shown to be 3.88 times more likely than the age group of ≥25 years to have irregular menstrual cycles in this study. This is in line with a study conducted in India (32). Menstrual irregularity is common in the first 2 years of menarche and is related to hypothalamus-pituitary-ovarian axis maturation. For the first few years after menstruation begins, long, irregular cycles are common. The irregularity during this time is due to anovulatory cycles. In youngsters, this often happens because their bodies have not yet settled into a pattern of regular menstrual cycles.
This study revealed that early menarche increases the risk of having irregular menstruation four-fold compared to those who started menses at 13–14 years old. This finding is consistent with previous findings in Ethiopia Adama, Lebanon, and Taiwanese college students (29, 30, 33). This might be because the girls at an early age might be exposed to stress, and the part of the brain that regulates periods is influenced by stress. Furthermore, at a young age, the hypothalamic-pituitary-ovarian axis is not mature enough to regulate the release of steroid hormones that are critical for controlling the menstrual cycle.
Our studies show overweight students were at two-fold greater risk for menstrual irregularity compared to those who were of normal weight. This result is consistent with other studies conducted in Ethiopia Adama, Lebanon, Taiwan, and India (11, 29, 30, 33, 34). This could be due to hormonal abnormalities caused by obesity and being overweight (body fat). Being overweight or obese have been linked to increased testosterone, disrupted estrogen, and decreased sex hormone-binding globulin (SHBG). Higher levels of testosterone have been associated with polycystic ovary syndrome, which is related to ovulatory dysfunction and menstrual irregularity. Clinical studies have also shown elevated total and free androgen levels and depressed SHBG in overweight/obese women with amenorrhea or oligomenorrhea (35–37). D-chiro-inositol downregulates the expression of aromatase, reducing the conversion of androgens into estrogens. Myo-insitol is currently used to treat menstrual irregularity in polycystic ovary syndrome (PCOS) (38).
Perceived stress made menstrual irregularities 2 times more likely. This finding is in line with studies conducted in Adama, Saudi Arabia, and India (26, 30, 31). This could be due to the psychological stress that might affect the coordination of HPO-Axis. The hypothalamus, which controls the pituitary gland, the body's master gland, which, in turn, controls the thyroid, adrenal glands, and the ovaries, which all work together to maintain hormones, is clearly affected by stress. This incoordination leads to irregular menstruation.
Our findings show those respondents who sleep < 5 h were two times more at risk of having menstrual irregularity than those who sleep 6–8 h per day. This result is consistent with studies done in Ethiopia (Adama and Debre Berhan University), China, and Korea (11, 13, 30, 39). This could be related to sleep disruption, which can cause hormone imbalances, which can disrupt the menstrual cycle, and cause discomfort and stress. The hypothalamic-pituitary-adrenal axis is crucial for maintaining alertness and sleep regulation. Dysfunction of this axis at any level can disrupt sleep. The hypothalamic-pituitary- axis activities regulate the menstrual cycle.
Limitation of the study
Our study was carried out during the global pandemic of COVID-19, which might have increased the students' level of stress, which is one of the strong risk factors for menstrual irregularities. This study was also conducted in a single study area.
Conclusion
In this study, more than one-third of the college girls in Debre Berhan town were shown to have experienced menstrual irregularity. Being less than 20 years old, having a history of early menarche, being overweight, and perceived stress were variables significantly associated with menstrual irregularity.
Recommendations
There is a need to plan strategies for girls to help them control menstrual irregularity; girls should control their weight and lead a healthy lifestyle, including getting adequate sleep. In addition, it is better to give training for students in life skills like study and time management skills to avoid or minimize their stress and to help them achieve adequate rest or sleep. Girls who follow healthy living choices may be able to control menstrual irregularity and lessen its impact on everyday activities as well as academic performance.
Data availability statement
The original contributions presented in the study are included in the article/supplementary material, further inquiries can be directed to the corresponding author/s.
Ethics statement
The Ethical Review Board of Debre Berhan University's College of Health Sciences provided ethical approval. Formal letters acquired from the Amhara Regional Health and Teaching Bureau were used to contact with the Dean and Heads of Department. Each study respondent gave written consent after being informed of the study's purpose and/or objectives.
Author contributions
YM considered the study, analyzed the data, and wrote the manuscript. HM, GWo, MT, and GWa were involved in the interpretation of the data and contributed to manuscript preparation. All authors read and approved the final manuscript.
Acknowledgments
The authors would like to express their gratitude to Debre Berhan University for participating in the study. The authors also want to express their gratitude to the department heads and Deans of each institution, as well as the girls/students who participated in the study. The authors also thank the data collectors and supervisors of the data collectors.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Abbreviations
AUB, Abnormal Uterine Bleeding; AOR, Adjusted odds ratio; BMI, Body Mass Index; CI, Confidence Interval; COR, Crude Odds Ration; HPO, Hypothalamic Pituitary Ovary; PSS, Perceived Stress Scale; SHBG, Sex Hormone-Binding Globulin.
References
1. MayoClinic. Menstrual Cycle: What's Normal, What's Not, Healthy Life Style, Women Health (2021). Available online at: https://www.mayoclinic.org/healthy-lifestyle/womens-health/in-depth/menstrual-cycle/art-20047186
2. ACOG. What Is Menstrual Period (2019). Available online at: https://www.acog.org/womens-health/faqs/your-first-period
3. ACOG. Abnormal Uterine Bleeding (2021). Available online at:https://www.acog.org/womens-health/faqs/abnormal-uterine-bleeding
4. Whitaker L, Critchley HO. Abnormal uterine bleeding. Best Pract Res Clin Obstetr Gynaecol. (2016) 34:54–65. doi: 10.1016/j.bpobgyn.2015.11.012
5. Aram Aber PDF. Prevalence of menstrual disturbances among female students of fourth and fifth classes of curative medicine faculty (KUMS). IJRDO J Health Sci Nurs. (2018) 3:1–14. doi: 10.53555/hsn.v3i4.1989
6. Smith R, Bradley L, Ke R, Strickland JL. APGO Educational Series on Women's Health Issues. Clinical Management of Abnormal Uterine Bleeding Boston'Jespersen and Associates (2006).
7. Deligeoroglou E, Tsimaris P, Deliveliotou A, Christopoulos P, Creatsas G. Menstrual disorders during adolescence. Pediatr Endocrinol Rev. (2006) 3:150–9. Available online at: https://europepmc.org/article/med/16641850
8. Kumar A, Seshadri J, Murthy NS. Correlation of anthropometry and nutritional assessment with menstrual cycle patterns. J SAFOG. (2018) 10:263–9. doi: 10.5005/jp-journals-10006-1603
9. Sharma S, Deuja S, Saha C. Menstrual pattern among adolescent girls of Pokhara Valley: a cross sectional study. BMC Womens Health. (2016) 16:74. doi: 10.1186/s12905-016-0354-y
10. Ali A, Khalafala H, Fadlalmola H. Menstrual disorders among nursing students at Al Neelain University, Khartoum state. Sudan J Med Sci. (2020) 15:199–214. doi: 10.18502/sjms.v15i2.7067
11. Zeru AB, Gebeyaw ED, Ayele ET. Magnitude and associated factors of menstrual irregularity among undergraduate students of Debre Berhan University, Ethiopia. Reproduct Health. (2021) 18:1–8. doi: 10.1186/s12978-021-01156-1
12. Ansong E, Arhin SK, Cai Y, Xu X, Wu X. Menstrual characteristics, disorders and associated risk factors among female international students in Zhejiang Province, China: a cross-sectional survey. BMC Womens Health. (2019) 19:35. doi: 10.1186/s12905-019-0730-5
13. Xing X, Xue P, Li SX, Zhou J, Tang X. Sleep disturbance is associated with an increased risk of menstrual problems in female Chinese university students. Sleep Breath. (2020) 24:1719–27. doi: 10.1007/s11325-020-02105-1
14. West S, Lashen H, Bloigu A, Franks S, Puukka K, Ruokonen A, et al. Irregular menstruation and hyperandrogenaemia in adolescence are associated with polycystic ovary syndrome and infertility in later life: Northern Finland Birth Cohort 1986 study. Hum Reproduct. (2014) 29:2339–51. doi: 10.1093/humrep/deu200
15. Kadir R, Edlund M, Von Mackensen S. The impact of menstrual disorders on quality of life in women with inherited bleeding disorders. Haemophilia. (2010) 16:832–9. doi: 10.1111/j.1365-2516.2010.02269.x
16. Gujarathi J, Jani D, Murthi A. Prevalance of menstrual disorders in hostellers and its effect on education-a cross sectional study. World J Pharm Res. (2014) 3:4060–5. Available online at: https://www.researchgate.net/profile/Jasmine-Gujarathi/publication/262186721_PREVALENCE_OF_MENSTRUAL_DISORDERS_IN_HOSTELLERS_AND_ITS_EFFECT_ON_EDUCATION__A_CROSS_SECTIONAL_STUDY/links/00b7d536f87669c44a000000/PREVALENCE-OF-MENSTRUAL-DISORDERS-IN-HOSTELLERS-AND-ITS-EFFECT-ON-EDUCATION-A-CROSS-SECTIONAL-STUDY.pdf
17. Rostami Dovom M, Ramezani Tehrani F, Djalalinia S, Cheraghi L, Behboudi Gandavani S, Azizi F. Menstrual cycle irregularity and metabolic disorders: a population-based prospective study. PLoS ONE. (2016) 11:e0168402. doi: 10.1371/journal.pone.0168402
18. Solomon CG, Hu FB, Dunaif A, Rich-Edwards JE, Stampfer MJ, Willett WC, et al. Menstrual cycle irregularity and risk for future cardiovascular disease. J Clin Endocrinol Metab. (2002) 87:2013–7. doi: 10.1210/jcem.87.5.8471
19. Munro AK, Hunter EC, Hossain SZ, Keep M. A systematic review of the menstrual experiences of university students and the impacts on their education: a global perspective. PLoS ONE. (2021) 16:e0257333. doi: 10.1371/journal.pone.0257333
20. Munro MG, Critchley HO, Fraser IS, FIGO Menstrual Disorders Committee, Haththotuwa R, Kriplani A, et al. The two FIGO systems for normal and abnormal uterine bleeding symptoms and classification of causes of abnormal uterine bleeding in the reproductive years: 2018 revisions. Int J Gynecol Obstetr. (2018) 143:393–408. doi: 10.1002/ijgo.12666 Available online at: https://www.sleepfoundation.org/how-sleep-works/sleep-dictionary
21. Cashin K, Oot L. Guide to anthropometry a practical tool for program planners. Manag Implement. (2018) 360:93–115. Available online at: https://www.fantaproject.org/sites/default/files/resources/FANTA-Anthropometry-Guide-May2018.pdf
22. Cohen S. Perceived stress in a probability sample of the United States. In: Spacapan S, Oskamp S, editors. The Social Psychology of Health. Sage Publications, Inc. (1988). p. 31–67.
23. WHO. Substance Abuse (2013). Available online at: https://www.afro.who.int/health-topics/substance-abuse.
24. Sleeping Hour (2022). Available online at: https://www.google.com/search?q=sleeping+hours+meaning&rlz
25. Sherly Deborah G, Siva Priya D, Rama Swamy C. Prevalence of menstrual irregularities in correlation with body fat among students of selected colleges in a district of Tamil Nadu, India. Natl J Physiol Pharm Pharmacol. (2017) 7:740–3. doi: 10.5455/njppp.2017.7.0307422032017
26. Rafique N, Al-Sheikh MH. Prevalence of menstrual problems and their association with psychological stress in young female students studying health sciences. Saudi Med J. (2018) 39:67. doi: 10.15537/smj.2018.1.21438
27. Shiferaw MT, Mamo Wubshet DT. Menstrual problems and associated factors among students of Bahir Dar University, Amhara National Regional State, Ethiopia: a cross-sectional survey. Pan Afr Med J. (2014) 17:2–9. doi: 10.11604/pamj.2014.17.246.2230
28. Lee LK, Chen P, Lee K, Kaur J. Menstruation among adolescent girls in Malaysia: a cross-sectional school survey. Singapore Med J. (2006) 47:869. Available online at: www.smj.org.sg/sites/default/files/4710/4710a6.pdf
29. Karout N, Hawai S, Altuwaijri S. Prevalence and pattern of menstrual disorders among Lebanese nursing students. Eastern Mediterranean Health J. (2012) 18:346–52. doi: 10.26719/2012.18.4.346
30. Negesso K. Prevalence of Menstrual Irregularity and Associated Factors Among Preparatory School Girls in Adama Town, Oromia Region, Ethiopia (2021). Available online at: http://etd.aau.edu.et/handle/123456789/28617
31. Varghese L, Prakash P, Viswanath L. A study to identify the menstrual problems and related practices among adolescent girls in selected higher secondary school in Thiruvananthapuram, Kerala, India. J SAFOG. (2019) 11:13–6. doi: 10.5005/jp-journals-10006-1642
32. Omidvar S, Amiri FN, Bakhtiari A, Begum K. A study on menstruation of Indian adolescent girls in an urban area of South India. J Fam Med Primary Care. (2018) 7:698. doi: 10.4103/jfmpc.jfmpc_258_17
33. Chang PJ, Chen PC, Hsieh CJ, Chiu LT. Risk factors on the menstrual cycle of healthy Taiwanese college nursing students. Austral N Z J Obstetr Gynaecol. (2009). 49:689–94. doi: 10.1111/j.1479-828X.2009.01097.x
34. Deborah SG, Priya SD, Swamy RC. Prevalence of menstrual irregularities in correlation with body fat among students of selected colleges in a district of Tamil Nadu, India. Natl J Physiol Pharm Pharmacol. (2017) 7:740.
35. Von Schoultz B, Carlström K. On the regulation of sex-hormone-binding globulin-a challenge of an old dogma and outlines of an alternative mechanism. J Steroid Biochem. (1989) 32:327–34. doi: 10.1016/0022-4731(89)90272-0
36. ZHANG Y-W, STERN B, REBAR RW. Endocrine comparison of obese menstruating and amenorrheic women. J Clin Endocrinol Metab. (1984) 58:1077–83. doi: 10.1210/jcem-58-6-1077
37. Hosseinian AH, Kim MH, Rosenfield RL. Obesity and oligomenorrhea are associated with hyperandrogenism independent of hirsutism. J Clin Endocrinol Metab. (1976) 42:765–9. doi: 10.1210/jcem-42-4-765
38. Laganà AS, Forte G, Bizzarri M, Kamenov Z, Bianco B, Kaya C, et al. Inositols in the ovaries: activities and potential therapeutic applications. Expert Opin Drug Metab Toxicol. (2022) 18:123–33. doi: 10.1080/17425255.2022.2071259
39. Kaur R, Singh S, Kaushal K. Prevalence of sleep disturbances in menstrual cycle irregularities: a pilot study. Int J Sci Healthcare Res. (2020) 5:117–120. Available online at: https://ijshr.com/IJSHR_Vol.5_Issue.3_July2020/IJSHR0019.pdf
Keywords: age of menarche, body mass index, college students, menstrual irregularity, perceived stress
Citation: Mittiku YM, Mekonen H, Wogie G, Tizazu MA and Wake GE (2022) Menstrual irregularity and its associated factors among college students in Ethiopia, 2021. Front. Glob. Womens Health 3:917643. doi: 10.3389/fgwh.2022.917643
Received: 11 April 2022; Accepted: 20 June 2022;
Published: 23 August 2022.
Edited by:
Valentina Lucia La Rosa, University of Catania, ItalyReviewed by:
Antonio Simone Laganà, University of Palermo, ItalyBayew Kelkay Rade, University of Gondar, Ethiopia
Copyright © 2022 Mittiku, Mekonen, Wogie, Tizazu and Wake. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Yohannes Moges Mittiku, eW9oYW5uZXNtb2dlczE4QHlhaG9vLmNvbQ==
 Yohannes Moges Mittiku
Yohannes Moges Mittiku Haile Mekonen
Haile Mekonen Girma Wogie
Girma Wogie Michael Amera Tizazu
Michael Amera Tizazu