
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
PERSPECTIVE article
Front. Cardiovasc. Med. , 28 March 2025
Sec. Heart Failure and Transplantation
Volume 12 - 2025 | https://doi.org/10.3389/fcvm.2025.1548595
This article is part of the Research Topic A Patient-Centered Approach to the Management of Heart Failure and Comorbidities View all 3 articles
 Piotr Z. Sobanski1,2*
Piotr Z. Sobanski1,2* Maria Luisa De Perna3
Maria Luisa De Perna3 Sandra Eckstein4
Sandra Eckstein4 Tanja Fusi-Schmidhauser5,6,7
Tanja Fusi-Schmidhauser5,6,7 Jan Gaertner8,9
Jan Gaertner8,9 Valentina Gonzalez-Jaramillo10
Valentina Gonzalez-Jaramillo10 Lisa Hentsch11
Lisa Hentsch11 Caroline Hertler12
Caroline Hertler12 Roger Hullin13
Roger Hullin13 Lukas Hunziker14
Lukas Hunziker14 Philip Larkin15
Philip Larkin15 Jean-Baptiste Mercoli16
Jean-Baptiste Mercoli16 Philippe Meyer17
Philippe Meyer17 Giorgio Moschovitis18
Giorgio Moschovitis18 Matthias Paul19
Matthias Paul19 Otmar Pfister20
Otmar Pfister20
Introduction: Heart failure (HF) causes high symptom burden and shortens life expectancy. Implementation of Palliative Care (PC) concurrently with cardiologic guidelines-directed medical therapy (GDMT) improves quality-of-life (QoL) more than disease-oriented management alone but is underused. To facilitate provision of PC for people living with HF, the Swiss Society of Cardiology (SSC) and the Swiss Society for Palliative Care (palliative.ch) have created joint working-group.
Methods: Dyads representing cardiology and PC from Swiss HF centres have been identified. Through online voting, workshops and Delphi process priority topics for incorporation of PC into standard care for people with HF have been identified.
Results: 18 experts, from 8 Swiss HF-centres identified main topics relevant for implementation of PC in usual HF care: timely recognition of unaddressed health-related needs of affected people and their relatives (using validated assessment tools ID-PALL or NAT-PD:CH at least as the triggers evolve), identifying key palliative interventions for care of people living with HF, identifying strategies to facilitate cooperation between specialist PC and cardiology, defining research agenda to investigate efficacy of PC interventions, quality of care criteria, and outcomes of PC provision in Switzerland.
Discussion: Improvement of QoL of people with HF and their relatives could be greater if PC would be integrated in usual care timely. Frequent needs assessment, using validated tools helps to recognize people having unaddressed needs, and helps to replace the outdated, based on risk of dying, involvement of PC. Dialogue between both disciplines is crucial to provide care prolonging life of best quality during the whole journey living with disease.
Palliative care (PC) is a concept of care that focuses on improving the quality of life (QoL) of people living with serious, chronic, potentially life-limiting diseases and their relatives by implementing symptomatic interventions. It is usually applied in addition to the disease-specific, guidelines-directed medical therapy (GDMT) provided by other medical specialties. Both palliative and disease-specific approaches aim to improve QoL, but in different ways. A palliative approach is oriented toward the relief of suffering by means of the alleviation of symptoms and problems (e.g., decreasing the sensation of breathlessness and the suffering it causes), while disease-oriented management improves disease-related pathophysiology (by decreasing the stimuli evoking breathlessness, such as congestion or low cardiac output in the case of heart failure, HF). Applying PC and disease-specific interventions concurrently should be understood as setting a meta-goal for comprehensive care, ensuring a life of the best possible length and quality, from the beginning to the very end of living with a serious disease, using all available approaches.
The Swiss Societies of Cardiology (SSC) and Palliative Care (palliative.ch) have created a joint working group to facilitate interdisciplinary exchange, aimed at facilitating the provision of PC for those living with HF, in a uniform way across all regions of the country. The working group stressed the significance of distinguishing between two types of PC when design care: specialist PC (for those with complex and/or persistent problems, provided by or with the engagement of PC specialists/teams) and primary (general) PC (sufficient for the majority, provided by the usual care team which has basic PC training and specialist PC back-up). Once unaddressed needs have been recognized (which can emerge at any time, and do not correspond with either planned management, prognosis or disease progression), they should be evaluated in accordance with existing local structures and standards of care by the team deemed responsible. In most cases, the usual care team (cardiology, internal medicine, geriatrics, general practice) remains in charge of providing comprehensive care, including the elements of generalist PC. PC specialists/teams should be involved as needed, in the form of consultation, engagement with the usual care team, taking the lead in care only occasionally, in complex situations. Regardless of who is providing the PC, needs should be reassessed regularly to ensure they have been addressed appropriately, and in the case of insufficient efficacy, the intensity of collaboration between teams may need to be increased. Adequate multidisciplinary support (which may include medical management, psychosocial service, chaplaincy, and support by allied therapies such as physio- or ergo-therapy) can be more effective than generalist PC in alleviating the burden experienced by patients and their relatives/caregivers. A multidisciplinary PC team provides additional support to the usual care team by facilitating in-depth communication, preparedness for shared decision making, or assisting in advance care planning (ACP). Such collaborative support increases the quality of care, reduces the workload for the general practitioner (GP)/usual care team, and potentially prevents care fragmentation. Moreover, it increases satisfaction with care, and the concordance between care desired and received, especially during the end-of-life (EoL). Patient-reported outcomes and financial issues related to providing PC require further investigation to verify the clinical efficacy and cost-effectiveness of the proposed approach (1–3).
In the course of a kick-off meeting held during the National SSC Congress in Basel in June 2023, the working group identified the following four most relevant topics for establishing the provision of palliative elements in the standard care for people living with HF:
I. The timely recognition of the unaddressed health-related needs of people living with HF and their relatives (identification of needs assessment tools and triggers to apply them),
II. Identifying key palliative interventions for the care of people living with HF,
III. Identifying strategies to facilitate cooperation between specialist PC and cardiology,
IV. Defining research agenda to investigate the efficacy of PC interventions, quality of care criteria, and outcomes of PC provision in Switzerland.
Early integration of PC into disease management strategies alleviates disease-related suffering and improves QoL. For this reason, the World Health Organization (WHO) recommends the timely inclusion of PC in the standard care pathways for people living with any potentially life-limiting disease, including cardiovascular diseases, with HF as a key example (1, 4–6). Despite this, to date PC integration into care for those living with non-oncological disease has been scarce. The major barriers prohibiting early integration are misconceptions of PC as being appropriate for those who are imminently dying and/or are suffering from oncological diseases only (7). However, almost every person living with HF cannot be cured, despite receiving optimal GDMT, and can be confronted with limitations to the length and quality of life. Thus, they should be considered as candidates for receiving PC. Providing optimal, comprehensive care for all people living with HF without delay requires the timely and reliable recognition of unmet needs and the initiation of appropriate interventions. The working group has confirmed such a strategy as appropriate and applicable for people living with HF in Switzerland and has identified the crucial meaning of the timely recognition of unaddressed needs using validated tools. To choose the most suitable needs assessment tools for people living with HF, an additional workshop, held during the National Palliative Care Congress in Biel in November 2023, and two rounds of using the Delphi process were needed. 21 health care professionals in the first Delphi round and 17 in the second (both nurses and physicians), working in different settings of cardiology and PC in all regions of Switzerland made their recommendations. From the set of needs assessment tools (8–17) (Supplementary Figure S1), the experts proposed two as being the most appropriate for gauging whether those living with HF could have unmet needs and potentially require PC interventions: the IDentification of patients in need of PALLiative care (ID-PALL) and the Needs Assessment Tool: Progressive Disease—Heart Failure (NAT:PD-HF). Both tools are simple, based on clinical evaluations (neither requires special tests), and can be easily applied by health care professionals (mostly nurses or physicians) without special training in PC. ID-PALL (Supplementary Figure S2) has been designed to identify those living with non-malignant or malignant (i.e., oncological) disease who might require PC support in a different acute medical care setting (except in intensive care units and emergency departments) and is available in English, French, and Italian (18–20). NAT:PD-HF (Supplementary Figure S3) has been specifically designed to target needs in HF in any settings of care. It is available in English and has been validated in German (17, 21). The working group has undertaken efforts to make both tools available in all of the national languages of Switzerland. ID-PALL guides evaluation regarding which form of PC should be provided—general or specialized, whereas NAT:PD-HF includes a question on who is needed to address the recognized needs.
ID-PALL uses the surprise question (SQ) as one of the main criteria—a question which healthcare professionals should ask themselves: “would you be surprised if the patient died in the next ….” between 3 and 12 moths has been proposed, with one year being most commonly used (22, 23). NAT:PD-HF contains four sections (patient wellbeing, caregiver wellbeing, their ability to provide care, and issues suggesting a high probability of a need for PC referral) with prompts aiding the evaluation of unmet needs. The tool does not contain any questions on disease progression, prognosis, or risk of death, as studies during the validation process of this tool indicated that needs do not correlate with disease progression.
The SQ, sometimes proposed as a single indicator for the probability of the need for PC, should be seen as more difficult to apply than it seems, as it is neither reliably sensitive (11.6%–95.6%) nor specific (13.8%–98.2%). It carries very high inter-observer differences, making it unreliable and rather difficult to use, especially for health care professionals not trained in providing EoL care and to assess people living with a non-oncological disease, having unpredictable trajectory (22, 24). Additionally, the SQ recognizes the risk of dying and not the need for care, and the risk of death-based initiation of PC is considered outdated and no longer recommended by PC societies, the WHO, and the latest American Heart Association Guidelines on Heart Failure (1, 2). Some experts propose using the SQ as the absolute minimum when more sensitive and validated tools have not been applied, as an indicator who might be in need. Choosing SQ strengthen the stigmatization of PC as care for those at risk of dying. The authors of this statement promote the incorporation of PC at an early stage of living with HF and to perceive the SQ as a way that could help identify those who might require PC urgently due to short life expectancy.
After identifying the needs assessment tools, the second most important step in setting up PC provision for people living with HF is to define when to apply them. The working group proposes that needs should be assessed (using the suggested, validated tools: ID-PALL or NAT:PD-HF) every time there is a significant change in:
- The patient's disease trajectory: e.g., repeated, unscheduled HF-related hospitalizations, emergency room or outpatient visits, considering candidacy for high-risk interventions—mechanical circulatory support, MCS, implantation or heart transplantation, considering management influencing trajectory of living—implantation or exchanging of implantable cardioverter defibrillator (ICD), diagnosing HF for the first time, or its end-stage;
- General health condition: e.g., diagnosis of new, potentially serious concomitant diseases);
- Situation of the next family or the caregiver: e.g., serious disease or death of a spouse.
Additionally, needs assessment should eventually become a routine element of yearly HF follow-up, and more often in the case of those with an unstable condition (Table 1).
The person who performs the given assessment should be determined individually in each centre, according to the local functioning standards and capacities. Basic screening can be initiated by e.g., a (HF) nurse, in both in- or out-patient settings. Studies have shown that after obtaining the required competence in using the proposed tools, performing needs assessment does not prolong the time of a consultation or an outpatient visit and provides additional insights into patient's needs (25–27).
The pattern of assessing needs in people living with HF and assignment of responsibility for PC provision, is depicted in Supplementary Figure S4.
The palliative interventions provided, usually concurrently with optimal cardiac management and care, can be divided into those dedicated to: (1) people living with HF, (2) their relatives and informal caregivers, and/or (3) health care professionals (Table 2). The most relevant interventions dedicated to patients include the following:
• In-depth communication,
• Provision of support in decision-making,
• Provision of symptom management,
• Provision of nonmedical support.
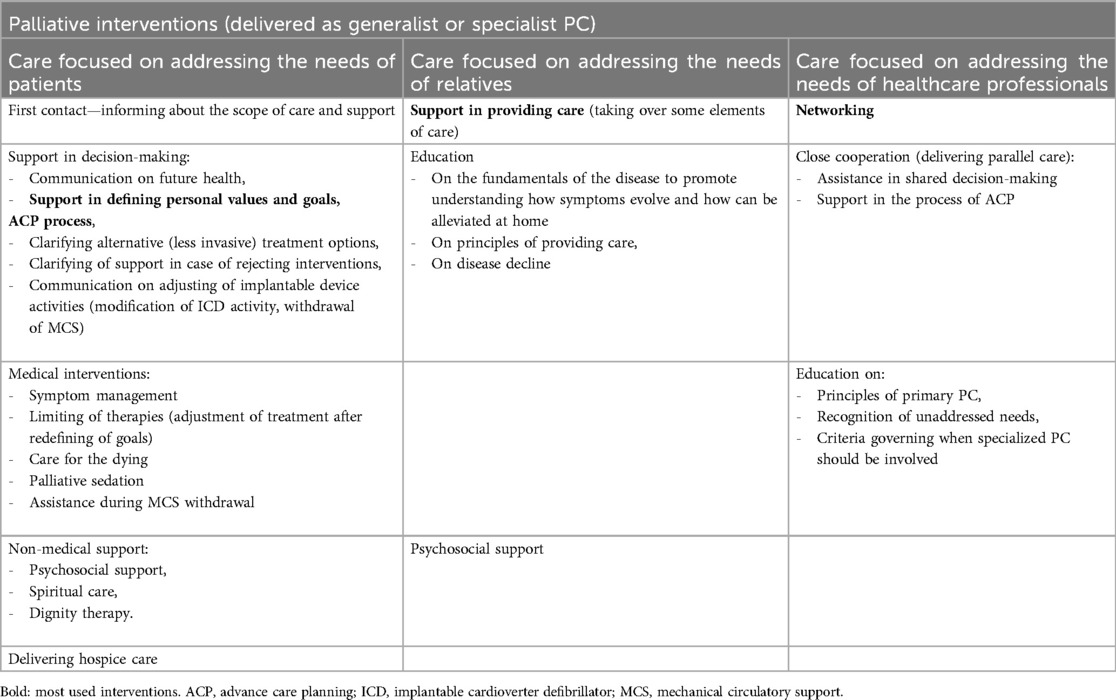
Table 2. Palliative interventions relevant to caring for people living with heart failure, their relatives, and healthcare professionals.
The interventions dedicated to the family and other informal caregivers include support in caring for patients and ensuring the wellbeing of caregivers themselves (Table 2).
Increasing awareness of the impact of PC on the QoL and the benefits of integrating PC early in the HF management by emphasizing that PC complements rather than replaces diesease-modifying therapies among healthcare providers, patients, families, informal caregivers and the general population.
Initiatives:
a. Organising public health campaigns supported by organisations like the Swiss Heart Foundation, to inform affected people and the general population about the benefits of PC.
b. Training for healthcare professionals (eg., cardiologists, internists, GPs) on the basics of PC and on timely recognition of unaddressed needs.
Empowering GPs as primary care providers, who can apply elements of PC, and coordinate collaboration with specialists, including PC.
Initiatives:
a. Training GPs on the identification of unaddressed PC needs, providing primary PC interventions, and recognising triggers for contacting specialized PC.
b. Facilitation a collaborative relationship among GPs and all specialists through regular communication and active involvement in care planning.
Overcoming main barriers to PC integration in HF management which consists of misconeptions about PC and limited access to specialised PC services.
Initiatives:
a. Educating patients and healthcare professionals on modern PC concepts.
b. Adjusting the usual HF-related communication focused on prolonging life and implementing GDMT by incorporating anticipatory communication on diesease progression.
c. Ensuring easy access to PC services for people with HF by referring them to larger centres, utilising teleconsultations, and increasing the availability of PC providers used in caring for individuals with living HF, if such services are lacking in the usual care centres.
Cross-training for interdisciplinary collaboration between cardiology and PC to enhance mutual understanding, cooperation and skills sharing.
Initiatives:
a. Regular case discussions and joint consultations.
b. Developing collaborative care plans clearly defining roles and responsibilities among providers.
c. Ensuring care decisions are guided by patients` preferences and values, with regular reassessments to adapt if they are changing.
Facilitating interdisciplinary collaboration.
Initiatives:
a. Establishing multidisciplinary teams, including PC specialists, cardiologists, GPs, nurses, social workers, psychologists, and other specialists.
b. Streamlining communication pathways and holding regular meetings for information exchange.
c. Prioritizing a person-centred approach by involving patients and families in care discussions to respect their values, preferences are goals.
Research on the management of most relevant (dyspnoea, pain), refractory symptoms (i.e., persisting with inacceptable intensity or duration for the given patient, despite optimal, adequate and GDMT for this person) in patients with HF:
a. The efficacy and safety of non-pharmacological interventions (such as cognitive behavioural training, hypnosis, virtual reality, and physiotherapy),
b. The efficacy and safety of medical management (non-opioids and different opioids).
Comparison of organizational efficacy, quality and cost-efficiency between generalist PC delivered by a cardiology team (usually a cardiology nurse trained in PC with a specialized PC as a back-up in case of the persistence of unaddressed needs), vs. the usual care (PC delivered on demand).
a. Assessment of the utilization of medical resources (GP visits, emergency room visits, and hospital admissions, or intensive care unit admissions, use of invasive care at the EoL), frequency of shared decision-making and advance care planning discussions, concordance between received and preferred care.
b. Assessment of the cost-effectiveness of primary PC with specialist PC back-up vs. usual care (PC delivered on demand).
c. Defining referral criteria/needs assessment tools which are the most appropriate for providing optimal PC. Of particular relevance for Switzerland is the translation of those tools into all of the national languages in order to unify standards throughout the country.
Comparison of clinical efficacy of different forms of PC (primary with specialist back-up vs. standard care: optimal cardiologic care, PC delivered on demand) on the suffering of people living with HF, the burden of their informal caregivers, and satisfaction from care.
a. Review of the literature to compare the satisfaction of patients and informal caregivers with care in different care models.
b. Setting-up an interventional trial to test whether the results from the literature review can be implemented in the clinical reality in Switzerland, including a comparison of the perspective of the individual patient and the care providing team.
HF is a common and serious condition characterized by progressive decline, high symptom burden, and shortened life expectancy, even with GDMT. HF is thus a disease warranting access to PC. Many affected people could benefit from receiving PC with the improvement of QoL, symptom burden, and support in the psychosocial, existential and spiritual dimensions; however, the need for PC involvement remains underrecognized (28). The Swiss Societies of Cardiology (SSC) and for Palliative Care (palliative.ch) working group has selected tools which should be used to identify unmet needs, proposed triggers when those tools should be applied, and summarized the PC interventions most relevant in care for people living with HF. In-depth communication on living with disease, which prepares affected people for more active participation in medical decision-making (e.g., shared decision making) and the promotion of anticipatory care planning (e.g., ACP) is increasingly important. This improves the concordance between care wished and received, especially at the EoL, and in this way secures greater satisfaction with and from care.
This document encourages collaboration between cardiologists and PC professionals by identifying existing barriers and proposing strategies to overcome them. Further steps in the development of palliative cardiology, such as examining the efficacy of the approach and setting a future research agenda have also been proposed.
Published with endorsement of the Swiss Society of Cardiology and the Swiss Society for Palliative Care.
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
PS: Conceptualization, Data curation, Methodology, Project administration, Visualization, Writing – original draft, Writing – review & editing. MD: Conceptualization, Writing – original draft, Writing – review & editing. SE: Conceptualization, Writing – original draft, Writing – review & editing. TF-S: Conceptualization, Writing – original draft, Writing – review & editing. JG: Conceptualization, Writing – original draft, Writing – review & editing. VG-J: Writing – original draft, Writing – review & editing, Conceptualization. LH: Conceptualization, Writing – original draft, Writing – review & editing. CH: Conceptualization, Writing – original draft, Writing – review & editing. RH: Conceptualization, Writing – original draft, Writing – review & editing. LH: Conceptualization, Writing – original draft, Writing – review & editing. PL: Conceptualization, Writing – review & editing. J-BM: Conceptualization, Writing – original draft, Writing – review & editing. PM: Conceptualization, Writing – original draft, Writing – review & editing. GM: Conceptualization, Writing – original draft, Writing – review & editing. MP: Conceptualization, Writing – original draft, Writing – review & editing. OP: Conceptualization, Writing – review & editing.
The author(s) declare that financial support was received for the research and/or publication of this article. The article processing fee has been funded by the Swiss Society of Cardiology, the Swiss Society for Palliative Care, and Spital Schwyz, Schwyz, Switzerland.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The author(s) declare that no Generative AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fcvm.2025.1548595/full#supplementary-material
1. Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, Colvin MM, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association joint committee on clinical practice guidelines. Circulation. (2022) 145(18):e895–1032. doi: 10.1161/CIR.0000000000001063
2. Sobanski PZ, Alt-Epping B, Currow DC, Goodlin SJ, Grodzicki T, Hogg K, et al. Palliative care for people living with heart failure: European association for palliative care task force expert position statement. Cardiovasc Res. (2020) 116(1):12–27. doi: 10.1093/cvr/cvz200
3. Radbruch L, De Lima L, Knaul F, Wenk R, Ali Z, Bhatnaghar S, et al. Redefining palliative care—a new consensus-based definition. J Pain Symptom Manage. (2020) 60(4):754–64. doi: 10.1016/j.jpainsymman.2020.04.027
4. Rogers JG, Patel CB, Mentz RJ, Granger BB, Steinhauser KE, Fiuzat M, et al. Palliative care in heart failure. J Am Coll Cardiol. (2017) 70(3):331–41. doi: 10.1016/j.jacc.2017.05.030
5. Kavalieratos D, Gelfman LP, Tycon LE, Riegel B, Bekelman DB, Ikejiani DZ, et al. Palliative care in heart failure. J Am Coll Cardiol. (2017) 70(15):1919–30. doi: 10.1016/j.jacc.2017.08.036
6. Temel JS, Greer JA, Muzikansky A, Gallagher ER, Admane S, Jackson VA, et al. Early palliative care for patients with metastatic non-small-cell lung cancer. Randomized controlled trial research support, non-U.S. Gov't. N Engl J Med. (2010) 363(8):733–42. doi: 10.1056/NEJMoa1000678
7. Sue AQR, Sorensen A, Lo S, Pope A, Swami N, Rodin G, et al. Palliative care physicians’ perceptions of conditions required to provide early palliative care. J Pain Symptom Manage. (2023) 66(2):93–101. doi: 10.1016/j.jpainsymman.2023.04.008
8. Murray S, Boyd K. Using the ‘surprise question’ can identify people with advanced heart failure and COPD who would benefit from a palliative care approach. Palliat Med. (2011) 25(4):382. doi: 10.1177/0269216311401949
9. Gomez-Batiste X, Martinez-Munoz M, Blay C, Amblas J, Vila L, Costa X, et al. Identifying patients with chronic conditions in need of palliative care in the general population: development of the NECPAL tool and preliminary prevalence rates in catalonia. BMJ Support Palliat Care. (2013) 3(3):300–8. doi: 10.1136/bmjspcare-2012-000211
10. Thoonsen B, Engels Y, Van Rijswijk E, Verhagen S, Van Weel C, Groot M, et al. Early identification of palliative care patients in general practice: development of RADboud indicators for PAlliative care needs (RADPAC). Br J Gen Pract. (2012) 62(602):e625–31. doi: 10.3399/bjgp12X654597
11. Highet G, Crawford D, Murray SA, Boyd K. Development and evaluation of the supportive and palliative care indicators tool (SPICT): a mixed-methods study. BMJ Support Palliat Care. (2014) 4(3):285–90. doi: 10.1136/bmjspcare-2013-000488
12. George N, Barrett N, McPeake L, Goett R, Anderson K, Baird J. Content validation of a novel screening tool to identify emergency department patients with significant palliative care needs. Acad Emerg Med. (2015) 22(7):823–37. doi: 10.1111/acem.12710
13. Luthi FT, Bernard M, Gamondi C, Ramelet AS, Borasio GD. ID-PALL: an instrument to help you identify patients in need of palliative care. Praxis. (2021) 110(15):839–44. doi: 10.1024/1661-8157/a003788
14. Davidson PM, Cockburn J, Newton PJ. Unmet needs following hospitalization with heart failure. J Cardiovasc Nurs. (2008) 23(6):541–6. doi: 10.1097/01.JCN.0000338927.43469.35
15. Kane PM, Daveson BA, Ryan K, Ellis-Smith CI, Mahon NG, Mcadam B, et al. Feasibility and acceptability of a patient-reported outcome intervention in chronic heart failure. BMJ Support Palliat Care. (2017) 7(4):470–9. doi: 10.1136/bmjspcare-2017-001355
16. Teike Luthi F, Bernard M, Vanderlinden K, Ballabeni P, Gamondi C, Ramelet AS, et al. Measurement properties of ID-PALL, a new instrument for the identification of patients with general and specialized palliative care needs. J Pain Symptom Manage. (2021) 62(3):e75–84. doi: 10.1016/j.jpainsymman.2021.03.010
17. Waller A, Girgis A, Davidson PM, Newton PJ, Lecathelinais C, Macdonald PS, et al. Facilitating needs-based support and palliative care for people with chronic heart failure: preliminary evidence for the acceptability, inter-rater reliability, and validity of a needs assessment tool. J Pain Symptom Manage. (2013) 45(5):912–25. doi: 10.1016/j.jpainsymman.2012.05.009
18. Ament SM, Couwenberg IM, Boyne JJ, Kleijnen J, Stoffers HE, Van Den Beuken MH, et al. Tools to help healthcare professionals recognize palliative care needs in patients with advanced heart failure: a systematic review. Palliat Med. (2021) 35(1):45–58. doi: 10.1177/0269216320963941
19. Moons P, Norekval TM, Arbelo E, Borregaard B, Casadei B, Cosyns B, et al. Placing patient-reported outcomes at the centre of cardiovascular clinical practice: implications for quality of care and management. Eur Heart J. (2023) 44(36):3405–22. doi: 10.1093/eurheartj/ehad514
20. Waller A, Hobden B, Fakes K, Clark K. A systematic review of the development and implementation of needs-based palliative care tools in heart failure and chronic respiratory disease. Front Cardiovasc Med. (2022) 9:878428. doi: 10.3389/fcvm.2022.878428
21. Gonzalez-Jaramillo V, Guyer J, Luethi N, Sobanski P, Zbinden R, Rodriguez E, et al. Validation of the German version of the needs assessment tool: progressive disease-heart failure. Health Qual Life Outcomes. (2021) 19(1):214. doi: 10.1186/s12955-021-01817-6
22. Blum M, Gelfman LP, McKendrick K, Pinney SP, Goldstein NE. Enhancing palliative care for patients with advanced heart failure through simple prognostication tools: a comparison of the surprise question, the number of previous heart failure hospitalizations, and the Seattle heart failure model for predicting 1-year survival. Front Cardiovasc Med. (2022) 9:836237. doi: 10.3389/fcvm.2022.836237
23. Pattison M, Romer AL. Improving care through the end of life: launching a primary care clinic-based program. J Palliat Med. (2001) 4(2):249–54. doi: 10.1089/109662101750290335
24. Gonzalez-Jaramillo V, Arenas Ochoa LF, Saldarriaga C, Krikorian A, Vargas JJ, Gonzalez-Jaramillo N, et al. The ‘surprise question’ in heart failure: a prospective cohort study. BMJ Support Palliat Care. (2024) 14(1):68–75. doi: 10.1136/bmjspcare-2021-003143
25. Campbell RT, Petrie MC, Jackson CE, Jhund PS, Wright A, Gardner RS, et al. Which patients with heart failure should receive specialist palliative care? Eur J Heart Fail. (2018) 20(9):1338–47. doi: 10.1002/ejhf.1240
26. Hentsch L, Sobanski PZ, Escher M, Pautex S, Meyer P. Palliative care provision for people living with heart failure: the Geneva model. Front Cardiovasc Med. (2022) 9:933977. doi: 10.3389/fcvm.2022.933977
27. Hentsch L, Sobanski PZ, Escher M, Pautex S, Meyer P. Integration of a palliative approach into heart failure care: a European society of cardiology heart failure association position paper. Eur J Heart Fail. (2020) 22:2327–39. doi: 10.1002/ejhf.1994
28. Antonione R, Sinagra G, Moroni M, Correale M, Redaelli D, Scrutinio D, et al. Palliative care in the cardiac setting: a consensus document of the Italian society of cardiology/Italian society of palliative care (SIC/SICP). G Ital Cardiol (Rome). (2019) 20(1):46–61. Documento di Consenso Sulle Cure Palliative in Ambito Cardiologico a Cura del Gruppo di Lavoro Congiunto Della Societa Italiana di Cardiologia (SIC) e Della Societa Italiana di Cure Palliative (SICP). doi: 10.1714/3079.30720
Keywords: palliative care, heart failure, needs assessment, quality of life, national strategy
Citation: Sobanski PZ, De Perna ML, Eckstein S, Fusi-Schmidhauser T, Gaertner J, Gonzalez-Jaramillo V, Hentsch L, Hertler C, Hullin R, Hunziker L, Larkin P, Mercoli J-B, Meyer P, Moschovitis G, Paul M and Pfister O (2025) National strategy for integrating palliative care into standard cardiac care for people living with heart failure: a position statement from the joint working group of the Swiss Societies of Cardiology and Palliative Care. Front. Cardiovasc. Med. 12:1548595. doi: 10.3389/fcvm.2025.1548595
Received: 19 December 2024; Accepted: 29 January 2025;
Published: 28 March 2025.
Edited by:
Katerina Philippou, Cyprus University of Technology, CyprusReviewed by:
Wandy Chan, Prince Charles Hospital, AustraliaCopyright: © 2025 Sobanski, De Perna, Eckstein, Fusi-Schmidhauser, Gaertner, Gonzalez-Jaramillo, Hentsch, Hertler, Hullin, Hunziker, Larkin, Mercoli, Meyer, Moschovitis, Paul and Pfister. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Piotr Z. Sobanski, cGlvdHIuc29iYW5za2lAc3BpdGFsLXNjaHd5ei5jaA==
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.