- 1College of Medicine, Mohammed Bin Rashid University of Medicine and Health Sciences, Dubai Healthcare City, Dubai, United Arab Emirates
- 2Department of General Surgery, Mediclinic City Hospital, Dubai Healthcare City, Dubai, United Arab Emirates
- 3Department of Urology, Mediclinic City Hospital, Dubai Healthcare City, Dubai, United Arab Emirates
Background: As the demand for kidney transplants continues to increase globally, healthcare institutions face a challenge to bridge the gap between patients waitlisted for kidney transplants and the number of donors. A major factor influencing the donor's decision is the operative risk and potential complications of the surgery. Open surgical approaches have been vastly replaced with laparoscopic donor nephrectomies as the standard of practice. However, there is a growing body of evidence pointing towards its potential superiority over laparoscopic methods. In this study, we aim to present our experience on outcomes of Robotic-Assisted Live Donor Nephrectomies (RALDN), the first series of its kind in the United Arab Emirates (UAE).
Methods: We retrospectively collected data from patients who underwent RALDN at Mediclinc City Hospital. Demographic data, laboratory investigations, and operative details were collected and analyzed.
Results: Seven patients underwent RALDN between 2021 and April 2022 at our facility. Four donors were male while three were female. Median length of hospital stay was 4 days. In our study, one of the patients suffered from a Clavien-Dindo grade IV complication which necessitated prolonged admission.
Conclusion: We conclude that RALDN is a safe method for donor kidney procurement, carrying a low risk of morbidity and mortality. This method could potentially evolve the number of kidney donors to address the issue of high kidney transplant demand.
Introduction
For many years, live donor nephrectomy was performed only with an open surgical approach and thereby many potential donors were reluctant to donate due to the morbidity associated with the procedure. In 1995, Ratner et al. performed the first Laparoscopic Donor Nephrectomy (LDN) which demonstrated several improvements over Open Donor Nephrectomy (ODN) such as decreased postoperative pain, length of stay (LOS), and perioperative blood loss. Due to these advantages, LDN has become the standard of care. In 2000, Horgan et al. performed for the first time a Robotic-Assisted Donor Nephrectomy (RALDN) (1). Since then, it has been adopted by several institutions worldwide and the amount of evidence has progressively increased (2). To date, RALDN represents an evolving field.
Unlike most surgical procedures, live donor nephrectomy is a unique, elective procedure, where a subject undergoes surgery for the sole benefit of another. Therefore, it is of great importance to keep the morbidity and mortality of the procedure as low as possible. Moreover, efforts should be made to procure the kidneys in optimal conditions for transplantation. The value of this study is compounded by the fast evolution of our local kidney transplantation scene.
In this study, we aim to evaluate the effectiveness of utilizing RALDN in our practice in Dubai by comparing our results from this first-ever case series to our local standard in addition to reviewing the resemblance of our data to international standards.
Methods
We have retrospectively reviewed electronic patient records at Mediclinic City Hospital, who underwent RALDN during the year 2021 and up to April 2022. Demographic and patient-related data regarding age, gender, BMI and heigh were extracted. In addition, operation details such as operating time, estimated blood loss, renal vasculature anatomy, neohrectomy site, length of hospital stay, and complications rate were recorded. Relevant laboratory data such as pre-op and post-op creatinine were collected as well. All data were extracted into an Excel sheet for subsequent analysis. Descriptive statistics were adopted using Excel formulas.
Technique
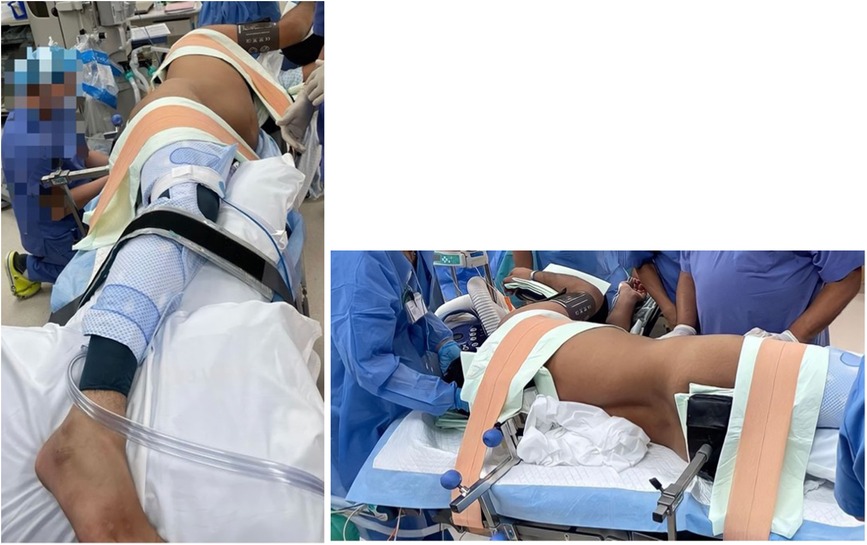
The retroperitoneal robot-assisted technique was first described by Akin et al., and has been adopted by out institution quite recently (2). After general anesthesia, the patient is positioned in the lateral decubitus position, with the operating table minimally flexed at about 30 degrees for ease of access to intended intra-abdominal anatomy. All the pressure points are carefully padded (Figure 1).
Our facility uses the DaVinci Xi Robot, which allows insertion of four ports. The positions of the robotic ports are first marked, which consists of a 12 mm camera port in the periumbilical region and another three 8 mm ports, in a linear fashion, from the subcostal mid-clavicular line, with about 7 cm of space between each port (Figure 2).

Figure 2. Robotic port marking. Green circle: 12 mm Camera port; Blue, red and yellow circles: operating ports, including retractors; Orange arrow: Pfannenstiel incision, and Alexis Port insertion point (Perpendicular line from the umbilicus is for surgeon's guidance only).
Initially, a 5–6 cm Pfannenstiel incision was made, which serves as the point of kidney procurement. The retroperitoneal space was then accessed by splitting the two rectus muscles. Using blunt hand dissection, the retroperitoneum is then retracted, and a space is created for the first port insertion, which is the camera port. The retroperitoneal space is then inflated. Once the peritoneal space is inflated, the remaining ports are inserted under direct visualization, perpendicular to the kidney axis. Alexis Wound Protector (Applied Medical, Rancho Santa Margarita, Calif, United States) was inserted into the Pfannenstiel incision, which has an added benefit of providing an additional 12 mm working port. The robot was then docked, with the port 1 and 3 utilised as working ports, port 2 as the camera port and port 4 for retraction.
The first step of the procedure involves dissection of the perinephric fat off of Gerota's fascia mobilizing it to the lower retroperitoneum. Next, to expose the kidney, Gerota's fascia is incised above and along the psoas muscle. The kidney is then on the lateral and inferior aspect. The ureter is then usually visualized anterior to the psoas muscle, medial to the Gerota's fascia, continuing superiorly into the hilum. The ureter was held up and dissection was carried out towards the hilum of the kidney. The left gonadal vein was identified, which was then divided by LigaSure. Next, anterior surface of the vein was dissected free until the left renal vein was identified. The suprarenal vein was identified at its insertion into the renal vein and was dissected free, and was further divided with LigaSure. Following dissection of the adrenal gland from the kidney, both branches of the renal artery is identified and dissected free from the anterior and posterior surface. Following mobilization of the ureter inferiorly, it was divided between clips and was therefore completely freed. Renal vasculature were held up and then divided with the robotic 45 stapler using white cartridges in that order. The kidney was delivered through the Pfannenstiel incision and inserted immediately in ice. The stump of renal artery and vein were carefully inspected to ensure hemostasis. The wound was then closed with Stratafux for the sheath of the Pfannenstiel incision, and 2'0 Vicryl for the subcutaneous tissue of this incision. All the remaining skin incisions were closed using 4'0 Monocryl with subcuticular incision. The kidney was perfused on the back table with HTK solution to ensure that the kidney was thoroughly cleaned of all the blood. The kidney was then packed in ice and was carried across for implantation.
Results
A total of seven patients underwent RALDN at Mediclinic City Hospital between September 2021 and April 2022 (Table 1). Of those, three patients were female, and four were males with a mean age of 37 years old. Surgical approaches are influenced by several patient factors including their BMI and height. The mean BMI amongst our seven patients was 24.85 kg/m2 (Range 19.88–31.73) and the mean height of the seven patients were 167 cm (Range 157–182). In our patient cohort, six patients had their left kidney removed compared to one who had their right kidney removed due to the complicated left renal vasculature nature as described in Table 1. The average pre-operative donor creatinine was 73.6 umol/L (Range 61–118), while average post-operative creatinine was 107.9 umol/L (Range 82–136). The mean operative time was 4 h 20 min (Range 03:27–05:45). Estimated Blood Loss ranged from 5 to 50 ml with 50 ml in the first procedure conducted and a downward trend in the subsequent procedures. Due to the outlier value present in the length of the hospital stay for patient number 7, a median value, instead of mean was calculated as 4 days (Range 3–30). Since our last patient encountered a major surgical complication, he was required to be admitted to the ICU to receive appropriate level of care, prolonging his stay to up to 30 days.
Discussion
In this case series, we report our experience on the first ever RALDN cases within the United Arab Emirates. Although RALDN is a rapidly emerging technique for donor nephrectomies, to our knowledge, no countries within the region have reported such cases and the literature contains scarce and perhaps controversial information which requires careful evaluation.
Laparoscopic Donor Nephrectomies (LDN) has been the dominant method of donor kidney procurement since it was first introduced in 1995 (3). This has crucially impacted the number of kidney donations globally due to its superiority in safety over the open surgical method. Open surgical methods were associated with significantly longer hospital stay vs. the laparoscopic method which offers longer warm ischemia time, less intraoperative blood loss, less perioperative pain, lower graft rejection rates, and quicker rehabilitation for previously healthy donors (4–9). Laparoscopic techniques therefore remarkably revolutionized donor nephrectomies, contributing significantly to the living kidney donor pool, however, significant discrepancies still exist between patients waitlisted for kidney transplantation and the number of donors. This calls for the implementation of advanced strategies to address this high demand.
Kidney donation is an entirely altruistic act, hence the utmost care should be taken to provide the donor with the safest and most comfortable experience. In the field of urology, robotic surgeries have been well established for a variety of pathologies, offering an excellent replacement for laparoscopic techniques (10, 11). Horgan et al., were the pioneers in RALDN, performing for the first time globally in 2001, on 10 patients (1). Ever since then, various other centers adopted the method and reported on their experience in the literature (2, 12–14).
A significant advantage of utilizing robots for donor nephrectomies is decreasing the length of hospital stay. We observed a shorter mean length of stay, compared to other studies conducted- 3 days, vs. 5 days in the studies conducted by Giacomoni et al., Hubert et al., Akin et al., and Laplace et al., (2, 12, 14–16). This shorter length of stay could be attributed to the robotic technique itself which reduces peritoneal disruption, better visualization and dissection of tissue planes, and better control of minor blood vessel injuries if any encountered during the procedure (15, 17). In our investigation, we report a LOS of 7.3 days which is higher than the mean LOW for laparoscopic method, however this can be explained as an outlier which skewed the result. Other analysis excluding the outlier results in a LOS of 3.5 days. Moreover, it has been previously reported that patients who underwent minimally invasive techniques experience less pain post-operatively, and have a smoother and speedy recovery, which further factors into a shorter hospital admission period (18). This can be also confirmed by the fact that none of the donor patients had presented to the emergency department nor had been re-admitted post-procedure for pain.
We have discovered that the operative time for our study was 260 min which is higher than the standard for RALDN which stands at 175 min. This could be explained by the growing level of experience of our team in conducting this technique. We can observe the decreasing trend in operative time from patients One to Six indicating that with a rapidly developing experience with this technique, we would be able to achieve a similar operative time. This trend was also observed by Horgan et al. and many others who have adopted their institution. In our case, this rather prolonged OT time has not resulted in any complications for the patient.
When comparing RALDN against LDN, studies suggest superiority of RALDN in terms of morbidity rates, or comparably as safe as LDN with the main drawbacks of the latter being diminished vision and control, both of which are vastly rectified by the robotic approach. Donors required less post-operative pain management, had a shorter length of stay, and minimal peri-operative complications were reported (19–22).
For all of our donors, we have adopted the retroperitoneal approach to kidney procurement. Although retroperitoneal partial nephrectomies were established in the literature, Akin et al., were the first to introduce the retroperitoneal (RP) approach for live donor nephrectomies (2). Several studies have evaluated surgical outcomes of transperitoneal (TP) approach compared to the retroperitoneal. One of the most significant advantages of which is consistent amongst almost all studies is the shorter operative time associated with RP approach (23–25). This is best explained by the RP approach eliminating the need to mobilize the bowel or the kidney during the surgery (23, 24). Eraky et al., were the first to also confirm the shorter time to access the renal hilum, which could serve as another reason for the shorter operative times observed by the RP approach (26). Another added benefit of the RP approach is the decreased blood loss and subsequently the need for blood transfusion (23, 24). The ease of access to the renal hilum due to the lesser need for dissection, could be a potential reason for this observed outcome (23, 27). Additionally, the RP approach could contain any hemorrhage or urine leak, which could be another reason for less blood loss observed (2). Furthermore, RP approach can be safely used for patients with previous adhesions or scars from past surgeries, which is a limitation of the TP approach (23). With regards to complications, the incidences of both major and minor complications seemed comparable between the two approaches (23–25).
Although no randomized control studies (RCT) exist to confidently determine the superiority of either method, Zhou et al. have performed an updated meta-analysis on the available literature (28). The results of the meta-analysis exhibit an agreement with the previous studies in terms of superiority of RP on operation duration, and less blood loss. Moreover, they have observed a shorter postoperative hospital stay. This has also been explained by the lack of need of bowel and mobilization and peritoneal manipulation, which subsequently translates into protection of the abdominal organs from hematoma and urine leaks, as well as postoperative ileus, enhancing the postoperative recovery period (28). However, similar to aforementioned studies, neither approach exhibited superiority regarding postoperative complications (28).
It is worth noting that all the aforementioned studies are conducted for robotic partial nephrectomies for renal tumours. To the knowledge of authors, no studies to this date exist comparing TP and RP approaches in robotic living donor nephrectomies, which could serve as a potential area of further research.
As is the case for all surgical procedures, there are still complications and pitfalls of RALDN especially given the relative novelty of this procedure. The most commonly reported intra-operative complication was bleeding, most frequently of the renal arteries (17, 19, 29). To our knowledge, no bowel perforation cases have been reported in the literature following RALDN. However, bowel perforation has been reported across several studies, following laparoscopic live donor nephrectomies (30–32). Most commonly, these perforations and bowel injuries were observed to be a result of instrumental lesion or injuries sustained by the stapler (8, 32). In the case of this patient, developing a Clavien-Dindo grade IVa complication given the procedure and approach and technique is almost unheard of. A key strength of the retroperitoneal approach is the lack of need to mobilize the colon during dissection which limits the chances of bowel injury, from our patient we can certainly conclude that the chances are not zero. It is postulated that even though the colon was not directly mobilized by the robotic arms, the heat generated by the electrocautery system in the robotic hands may have caused the colonic perforation in the case of our patient.
Thus, we should critically highlight this scenario to draw on the lessons from it and spread awareness to the wider medical community.
Surgeon's experience plays a crucial role in preventing untoward donor-related complications, where most of the complications are believed to occur at the beginning of the learning curve. As observed in previous studies, with increased number of RALDNs carried out, the number of major complications, namely bleeding and the need to convert to open surgery has been significantly reduced over time (29, 33).
Additionally, RALDN has been postulated to have significant strength when it comes to complex cases such as those with an additional renal artery or lumbar vein. Pre-operative angiogram could be the decision-maker for the technique of choice for pre-operative planning of donor nephrectomies in which the robotic approach presents better safety to the donor (Tae young shin). Gorodner et al., compared the safety of the procedure in two groups of patients, with and without renal vascular anomalies. In their study, they concluded that there was no significant difference regarding blood loss, LOS, or conversion to open operation in the group of vascular anomaly vs. the control.
Moreover, laparoscopic surgeries may potentially carry a risk of intra-operative blood loss, however, as reported in our experience, there was minimal difference in pre- and post-op hemoglobin levels (9, 22). This was consistent in other studies as well, further affirming the low risk of operative complications with RALDN.
In our investigation, we have encountered several limitations which should be addressed. Firstly, the authors acknowledge the small sample size with the single center scope. However, in the Middle East, the donor pools are relatively less compared to the West, and additionally, robotic methods of kidney retrieval is still a novel approach in Dubai, as well as within the region and as mentioned previously, to our knowledge, this study is the first of its kind within the region. Additionally, our sample did not contain any patients with comorbidities that could complicate the procedure such as obesity, smoking, or diabetes mellitus. We would encourage future studies to take into account those patients who have impaired wound healing ability and conduct studies with multivariate analysis to evaluate these populations, which later could increase the external validity of the study.
Conclusion
This is the first-ever study reporting on RALDN in the UAE and within the region. Given our results amongst the first 6 patients who underwent RALDN, we conclude that RALDN is a safe, effective way of donor kidney retrieval carrying a low risk of morbidity. In times of high demand for donor kidneys, RALDN implementation should be highly encouraged across the region, in an attempt to increase the body of kidney donations. We hope that the data generated from this experience will be beneficial to academic medical institutions globally and pose a possible strategy for constantly rethinking resource management and optimizing patient care.
Data availability statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics statement
The studies involving human participants were reviewed and approved by Mediclinic City Hospital. The patients/participants provided their written informed consent to participate in this study.
Author contributions
RR was involved in data collection and manuscript sysnthesis. MG was involved in data collection and manuscript sysnthesis. WC was involved in manuscript ideation, sysnthesis and revision. HV was involved in manuscript ideation, sysnthesis and revision. FJ was involved in manuscript ideation, sysnthesis, revision as well as supervising the manuscript synthesis process. All authors contributed to the article and approved the submitted version.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Horgan S, Vanuno D, Benedetti E. Early experience with robotically assisted laparoscopic donor nephrectomy. Surg Laparosc Endosc Percutan Tech. (2002) 12(1):64–70. doi: 10.1097/00129689-200202000-00011
2. Akin EB, Aydogdu I, Barlas IS. Introducing robot-assisted laparoscopic donor nephrectomy after experience in hand-assisted retroperitoneoscopic approach. Transplant Proc. (2019) 51(7):2221–4. doi: 10.1016/j.transproceed.2019.02.041
3. Ratner LE, Ciseck LJ, Moore RG, Cigarroa FG, Kaufman HS, Kavoussi LR. Laparoscopic live donor nephrectomy. Transplantation. (1995) 60(9):1047–9.7491680
4. Wilson CH, Bhatti AA, Rix DA, Soomro NA. Comparison of laparoscopic and open donor nephrectomy: UK experience. BJU Int. (2005) 95(1):131–5. doi: 10.1111/j.1464-410X.2004.05264.x
5. Vernadakis S, Marinaki S, Darema M, Soukouli I, Michelakis IE, Beletsioti C, et al. The evolution of living donor nephrectomy program at A hellenic transplant center. Laparoscopic vs. open donor nephrectomy: single-center experience. J Clin Med. (2021) 10(6):1195. doi: 10.3390/jcm10061195
6. Brook NR, Gibbons N, Nicol DL, McDonald SP. Open and laparoscopic donor nephrectomy: activity and outcomes from all australasian transplant centers. Transplantation. (2010) 89(12):1482–8. doi: 10.1097/TP.0b013e3181dd35a0
7. Nicholson ML, Kaushik M, Lewis GR, Brook NR, Bagul A, Kay MD, et al. Randomized clinical trial of laparoscopic versus open donor nephrectomy. Br J Surg. (2010) 97(1):21–8. doi: 10.1002/bjs.6803
8. Fonouni H, Mehrabi A, Golriz M, Zeier M, Müller-Stich BP, Schemmer P, et al. Comparison of the laparoscopic versus open live donor nephrectomy: an overview of surgical complications and outcome. Langenbecks Arch Surg. (2014) 399(5):543–51. doi: 10.1007/s00423-014-1196-4
9. Minnee RC, Idu MM. Laparoscopic donor nephrectomy. Neth J Med. (2010) 68(5):199–206. PMID: 20508268
10. Hemal AK, Menon M. Robotics in urology. Curr Opin Urol. (2004) 14(2):89–93. doi: 10.1097/00042307-200403000-00007
11. Kaul S, Menon M. Robotics in laparoscopic urology. Minim Invasive Ther Allied Technol. (2005) 14(2):62–70. doi: 10.1080/13645700510010872
12. Hubert J, Renoult E, Mourey E, Frimat L, Cormier L, Kessler M. Complete robotic-assistance during laparoscopic living donor nephrectomies: an evaluation of 38 procedures at a single site. Int J Urol. (2007) 14(11):986–9. doi: 10.1111/j.1442-2042.2007.01876.x
13. Louis G, Hubert J, Ladriere M, Frimat L, Kessler M. Robotic-assisted laparoscopic donor nephrectomy for kidney transplantation. An evaluation of 35 procedures. Nephrol Ther. (2009) 5(7):623–30. doi: 10.1016/j.nephro.2009.06.008
14. Laplace B, Ladrière M, Claudon M, Eschwege P, Kessler M, Hubert J. Robotic assisted laparoscopic living donor nephrectomy: preoperative assessment and results of 100 cases. Prog Urol. (2014) 24(5):288–93. doi: 10.1016/j.purol.2013.09.024
15. Giacomoni A, Di Sandro S, Lauterio A, Mangoni I, Mihaylov P, Concone G, et al. Initial experience with robot-assisted nephrectomy for living-donor kidney transplantation: feasibility and technical notes. Transplant Proc. (2013) 45(7):2627–31. doi: 10.1016/j.transproceed.2013.07.038
16. Shin TY, Lee YS. Robot-assisted laparoscopic donor nephrectomy: surgical feasibility and technique. Heliyon. (2019) 5(8):e02204. doi: 10.1016/j.heliyon.2019.e02204
17. Cohen AJ, Williams DS, Bohorquez H, Bruce DS, Carmody IC, Reichman T, et al. Robotic-assisted laparoscopic donor nephrectomy: decreasing length of stay. Ochsner J. (2015) 15(1):19–24. PMID: 25829876; PMCID: PMC436584125829876
18. Perry KT, Freedland SJ, Hu JC, Phelan MW, Kristo B, Gritsch AH, et al. Quality of life, pain and return to normal activities following laparoscopic donor nephrectomy versus open mini-incision donor nephrectomy. J Urol. (2003) 169(6):2018–21. doi: 10.1097/01.ju.0000067975.59772.b6
19. Spaggiari M, Garcia-Roca R, Tulla KA, Okoye OT, Di Bella C, Oberholzer J, et al. Robotic assisted living donor nephrectomies: a safe alternative to laparoscopic technique for kidney transplant donation. Ann Surg. (2022) 275(3):591–5. doi: 10.1097/SLA.0000000000004247
20. Giffen ZC, Cairl N, Ortiz J, Sindhwani P, Ekwenna O. Robotic-assisted donor nephrectomy: as safe as laparoscopic donor nephrectomy. Surg Technol Int. (2020) 37:171–4. PMID: 32520390
21. Wang H, Chen R, Li T, Peng L. Robot-assisted laparoscopic vs laparoscopic donor nephrectomy in renal transplantation: a meta-analysis. Clin Transplant. (2019) 33(1):e13451. doi: 10.1111/ctr.13451
22. Bhattu AS, Ganpule A, Sabnis RB, Murali V, Mishra S, Desai M. Robot-Assisted laparoscopic donor nephrectomy vs standard laparoscopic donor nephrectomy: a prospective randomized comparative study. J Endourol. (2015) 29(12):1334–40. doi: 10.1089/end.2015.0213
23. Mittakanti HR, Heulitt G, Li HF, Porter JR. Transperitoneal vs. Retroperitoneal robotic partial nephrectomy: a matched-paired analysis. World J Urol. (2020) 38(5):1093–9. doi: 10.1007/s00345-019-02903-7
24. Arora S, Heulitt G, Menon M, Jeong W, Ahlawat RK, Capitanio U, et al. Retroperitoneal vs. transperitoneal robot-assisted partial nephrectomy: comparison in a multi-institutional setting. Urology. (2018) 120:131–7. doi: 10.1016/j.urology.2018.06.026
25. Harke NN, Darr C, Radtke JP, von Ostau N, Schiefelbein F, Eraky A, et al. Retroperitoneal versus transperitoneal robotic partial nephrectomy: a multicenter matched-pair analysis. Eur Urol Focus. (2021) 7(6):1363–70. doi: 10.1016/j.euf.2020.08.012
26. Eraky A, Hamann C, Harke NN, Tropmann-Frick M, Junemann KP, Osmonov D. Robot-assisted partial nephrectomy: a single-center matched-pair analysis of the retroperitoneal versus the transperitoneal approach. Turk J Urol. (2021) 47(4):305–12. doi: 10.5152/tud.2021.21008
27. Ghani KR, Porter J, Menon M, Rogers C. Robotic retroperitoneal partial nephrectomy: a step-by-step guide. BJU Int. (2014) 114(2):311–3. doi: 10.1111/bju.12709
28. Zhou J, Liu Z, Cao D, Peng Z, Song P, Yang L, et al. Retroperitoneal or transperitoneal approach in robot-assisted partial nephrectomy, which one is better? Cancer Med. (2021) 10(10):3299–308. doi: 10.1002/cam4.3888
29. Geffner S, Klaassen Z, Tichauer M, Chamberlain RS, Paragi PR. Robotic-assisted laparoscopic donor nephrectomies: early experience and review of the literature. J Robot Surg. (2011) 5(2):115–20. doi: 10.1007/s11701-011-0245-z
30. Chan DY, Fabrizio MD, Ratner LE, Kavoussi LR. Complications of laparoscopic live donor nephrectomy: the first 175 cases. Transplant Proc. (2000) 32(4):778. doi: 10.1016/S0041-1345(00)00979-9
31. Hirose T, Hotta K, Iwami D, Harada H, Morita K, Tanabe T, et al. Safety and efficacy of retroperitoneoscopic living donor nephrectomy: comparison of early complication, donor and recipient outcome with hand-assisted laparoscopic living donor nephrectomy. J Endourol. (2018) 32(12):1120–4. doi: 10.1089/end.2018.0669
32. Øyen O, Andersen M, Mathisen L, Kvarstein G, Edwin B, Line PD, et al. Laparoscopic versus open living-donor nephrectomy: experiences from a prospective, randomized, single-center study focusing on donor safety. Transplantation. (2005) 79(9):1236–40. doi: 10.1097/01.TP.0000161669.49416.BA
Keywords: robot assisted live donor nephrectomy, live donor nephrectomy, kidney transplant, bowel perforation, minimally invasive technique
Citation: Rowaiee R, Gholami M, Concepcion W, Vedayar H and Janahi F (2023) Retroperitoneal robot-assisted live-donor nephrectomy: A single-center study. Front. Transplant. 2:1062240. doi: 10.3389/frtra.2023.1062240
Received: 5 October 2022; Accepted: 10 April 2023;
Published: 26 April 2023.
Edited by:
Michael Kueht, University of Texas Medical Branch at Galveston, United StatesReviewed by:
Bulang He, Austin Hospital, AustraliaSantosh Nagaraju, Charleston Area Medical Center, United States
© 2023 Rowaiee, Gholami, Concepcion, Vedayar and Janahi. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Farhad Janahi RmFyaGFkLkphbmFoaUBtYnJ1LmFjLmFl
 Rashed Rowaiee1
Rashed Rowaiee1 Mandana Gholami
Mandana Gholami