
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Public Health , 07 March 2025
Sec. Environmental Health and Exposome
Volume 13 - 2025 | https://doi.org/10.3389/fpubh.2025.1504411
This article is part of the Research Topic Evaluating Public Health Strategies for Climate Change: Risk and Opportunities View all 3 articles
 Zaiyong Zheng1,2,3
†
Zaiyong Zheng1,2,3
† Yanman Li4
†
Yanman Li4
† Qinglu Jiang4
†
Qinglu Jiang4
† Fangfang Zang1,2,3
Fangfang Zang1,2,3 Yang Yu1,2,3
Yang Yu1,2,3 Rongchuan Yue4
Rongchuan Yue4 Houxiang Hu4*
Houxiang Hu4* Chunxiang Zhang1,2,3*
Chunxiang Zhang1,2,3*Objective: To investigate the acute effects of air pollution on the daily hospitalizations for cardiovascular disease.
Methods: Data of daily hospitalization for cardiovascular disease were collected from the hospital electronic health record system in Nanchong. The air pollutants and meteorological data were obtained from the fixed monitoring stations. We performed over-dispersed Poisson regression incorporated with distributed lag models to assess associations between short-term exposure to air pollutants and the risk of cardiovascular disease hospitalizations.
Results: A total of 373,390 hospitalizations for cardiovascular diseases were identified. We found that a 10 μg/m3 increase in 7-day average concentrations of PM2.5 and PM10 was associated with 1.15% (95%CI: 0.55–1.76%) and 0.51% (95%CI: 0.19–0.82%) higher cardiovascular disease admissions. NO2 presents the largest adverse effect. The risk of cardiovascular disease admission increased by 6.26% with per 10 μg/m3 increase in NO2 for lag07.
Conclusion: Short-term exposures to high concentrations of air pollutants increased the risk of hospitalization for cardiovascular disease. Policymakers need to develop policies and strategic plans to combat air pollution.
Air pollution has been a global public concern. According to the World Health Organization (WHO), more than 99% of the global population lives in area with air pollution (1). In 2021, particulate matter air pollution was identified as the leading factor contributing to the global disease burden (2), accounting for 6.7 million premature deaths annually on a worldwide scale (3). Approximately 4.2 million deaths are attributed to ambient air pollution, with 25% of these fatalities linked to ischemic heart disease (4). In China, the mortality rate from CVD due to ambient particulate matter pollution has shown a consistent increase from 1990 to 2019 (5). Reports from the National Center for Cardiovascular Disease of China indicated that in 2019, more than 1.42 million excess deaths were associated with ambient particulate matter pollution (3). The high exposure risks and limited regenerative capability make the cardiovascular system become vulnerable to the hazardous effects of air pollution. Exposure to air pollution, such as particulate matters (PM10 and PM2.5), SO2, NO2, O3 and CO, has been associated with a significant increase in the risk of CVD (1). A nationwide cohort study conducted in China demonstrated that each 10 μg/m3 increment in PM2.5 exposure, corresponded to a 25.1% increase in CVD and a 16.4% rise in CVD mortality (6). Recent empirical evidence also indicates that maternal exposure to air pollution is associated with an elevated risk of congenital heart defects in newborns. A nationwide study of 1,434,998 births found a 2% increase in risk of congenital heart defects for every 10 μg/m3 rise in PM2.5 exposure (7, 8). These results underscore the significant hazards that air pollution poses to CVD. Therefore, investigating the impact of air pollution on cardiovascular health is important. Given the vast geographical span of China, air quality exhibits considerable variation across different regions. It is crucial to analyze localized data and evaluate the detrimental effects of air pollutants in specific areas. Moreover, the relationship between air pollution and CVD has not been previously documented in Nanchong. In this study, we utilized hospital medical records from Nanchong to assess the influence of air pollutants on hospital admissions related to cardiovascular disease.
Data of hospitalization admission for cardiovascular disease, encompassing both initial and recurrent cases, were retrieved from the electronic health record system of the affiliated hospital of North Sichuan Medical College from June 1, 2015, to December 31, 2023. Patients with discharge diagnoses containing cardiovascular disease according to ICD-10 (ICD-10: I00-I99) were included. I00-I99 contains: I00-I02: Acute rheumatic fever; I05-I09: Chronic rheumatic heart diseases; I10-I15: Hypertensive diseases; I20-I25: Ischemic heart diseases; I26-I28: Pulmonary heart disease and diseases of pulmonary circulation; I30-I52:Other forms of heart disease; I60-I69: Cerebrovascular diseases; I70-I79: Diseases of arteries, arterioles and capillaries; I80-I89: Diseases of veins, lymphatic vessels and lymph nodes, not elsewhere classified; I95-I99: Other and unspecified disorders of the circulatory system.
Nanchong is situated in the southwest region of China, and due to the barrier of the Qinling mountains, Nanchong avoids impacts of dust storm from the Northwest China. The urban area of Nanchong consists of the Shunqing, Gaoping, and Jialing districts. Covering an area of 2,637 square kilometers, the urban area of Nanchong is home to 2.101 million inhabitants. There are four air quality monitoring stations located in the urban area of Nanchong (Figure 1). Air quality data for each patient were matched with the nearest station. As no further detail can be provided, patients from the Shunqing district had their data averaged from the three stations within the district’s jurisdiction: LianYouChang station, Shiwei Jiance station and ShiWei station. Since some patients registered their address as Shixiaqu, an old name for the urban area of Nanchong, the air pollutant data for Shixiaqu was matched with the average data for the entire urban area of Nanchong. Additionally, on May 10, 2021, the Affiliated Hospital of North Sichuan Medical College moved from its former location at the southern part (Affiliated Hospital of NSMC-WH campus) to the northern part (Affiliated Hospital of NSMC-MY campus) of Shunqing district.
We collected daily data on air pollutants and climate factors from the PM2.5 historical database.1 The air pollutants include PM2.5, PM10, CO, SO2, NO2, and O3, while climate factors encompass temperature, wind, relative humidity and precipitation. The exposure levels of air pollution for each patient were matched from the monitoring station closet to their home address. The study was approved by the Human Ethics Committee of the Affiliated Hospital of North Sichuan Medical College (NUMBER). Informed consent was not specifically required since personal identifiers were not involved.
Spearman correlation coefficients was calculated to explore the relationship between air pollutants and meteorological factors. As the daily admission followed an overdispersion Poisson distribution, we applied quasi-Poisson regression models to estimate the impact of short-term exposure of air pollutants on daily hospitalizations for cardiovascular disease. Air pollutants included PM2.5, PM10, SO2, O3, NO2, and CO, while meteorological factors comprised daily average temperature (Ave.Temp.), wind speed, relative humidity, and precipitation were included in the regression model.
In Equation 1, Yt represents the daily hospitalization count for circulatory diseases on day t, E(Yt) denotes the expected daily number of cardiovascular disease hospitalizations on day t, α represents the intercept, β stands for the regression coefficient, represents the air pollutants, ns() refers to a nonlinear spline function, and df indicates the degree of freedom (9–11).
The excess risk (ER) of each air pollutant was estimated using the relative risk calculated from Equation 2. The ER of cardiovascular disease hospitalizations for every 10-unit increase in air pollutants was calculated as follows:
In Equation 2, β represents the exposure-response coefficient obtained from quasi-Poisson regression, indicating the association between cardiovascular disease hospitalization and air pollutants. This coefficient reflects the change in the risk of cardiovascular disease hospitalizations for each unit increase in air pollutants.
p < 0.05 was considered statistically significant. All statistical analyses were conducted in R software (version 4.1.2). The effects are described as the percent changes and 95% CI in daily count on admissions for CVD per 10 μg/m3.
Table 1 presents the characteristic of participants stratified by gender. A total of 373,390 hospitalization records of cardiovascular disease were documented from June 1, 2015, to December 31, 2023. Among these records, the male-to-female ratio was 1.27:1 (209,233 males vs. 164,157 females), with males accounting for 56.04%. The majority of patients were over 70 years old (41.93%). The most common comorbidity observed were hypertension (169,061 cases, 45.28%), followed by diabetes (86,864 cases, 23.26%), cerebral infarction (82,441 cases, 22.08%), coronary heart disease (68,706 cases, 18.40%) and electrolyte imbalance (63,506 cases, 17.01%).
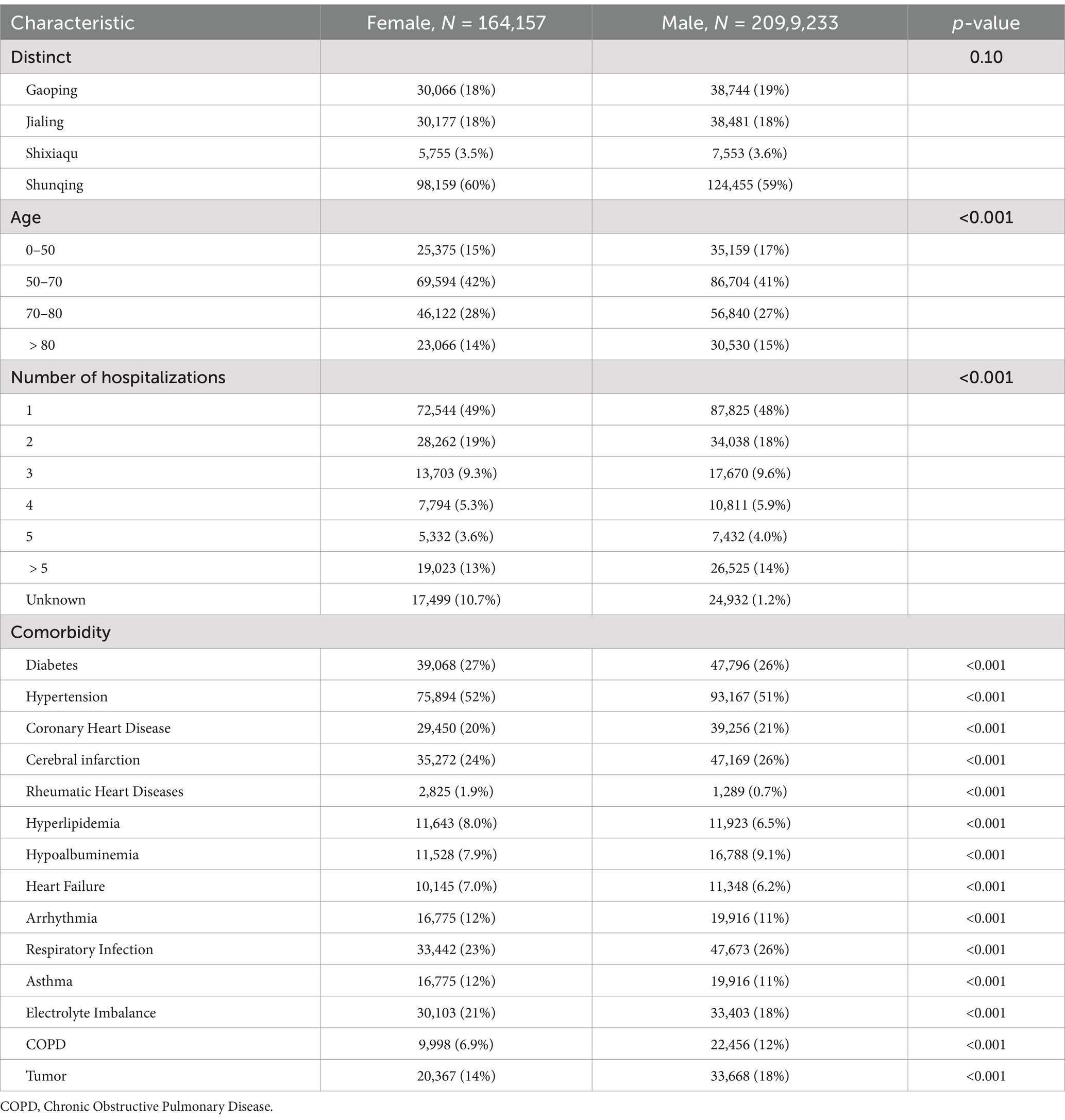
Table 1. Summary statistics of hospitalization records of cardiovascular disease from June 1, 2015, to December 31, 2023.
Table 2 presents the distributions of meteorological parameters and air pollutants. The daily average temperature was 17.88°C, with a daily maximum temperature of 42.80°C and a minimum daily temperature of −2.9°C.
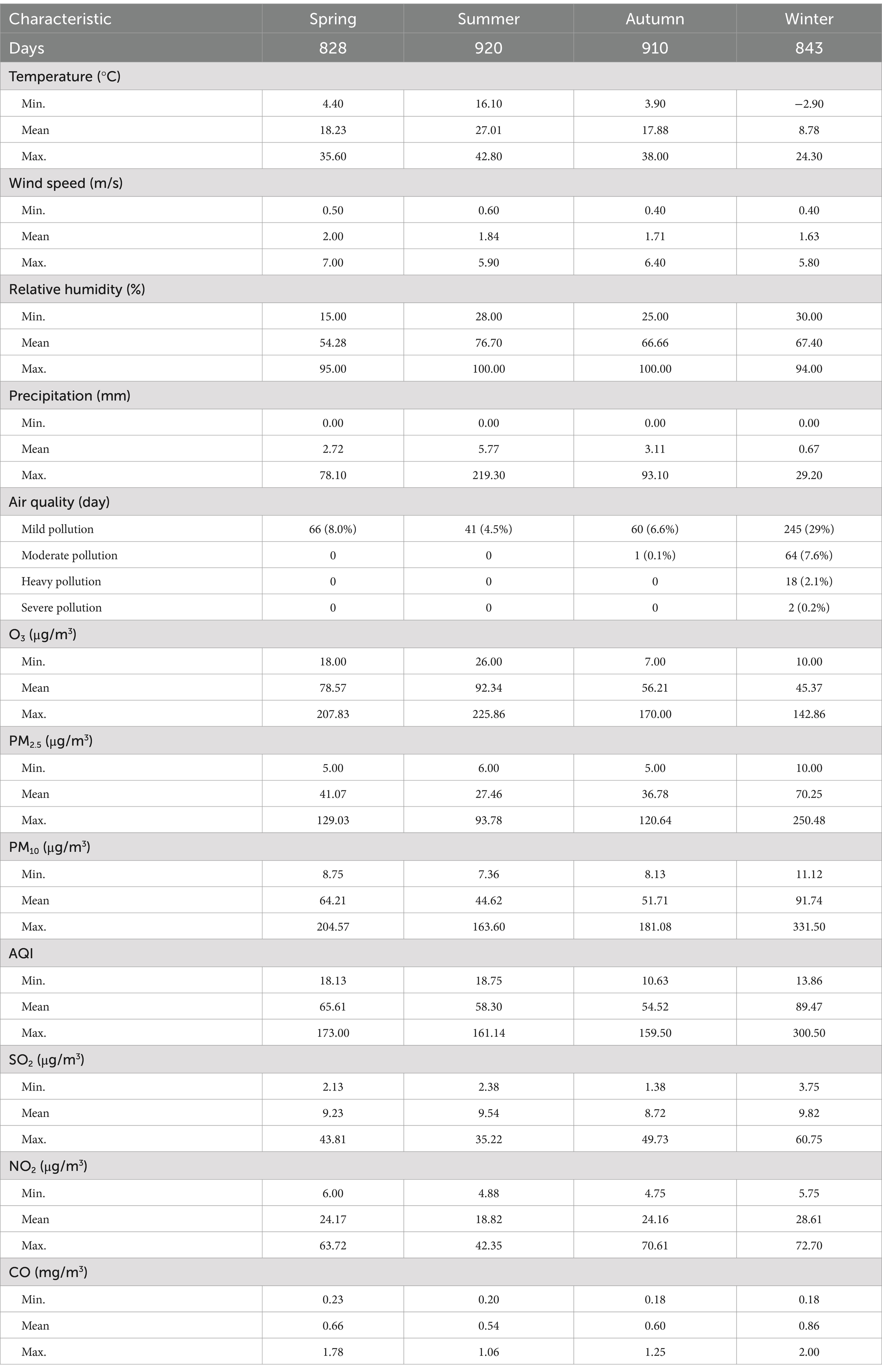
Table 2. Baseline data for meteorological parameters and air pollutants in Nanchong, June 1, 2015, to December 31, 2023.
During the study period, the daily average concentrations of air pollutants were as follows: PM2.5 (42.39 ± 28.68 μg/m3), PM10 (63.70 ± 40.21 μg/m3), SO2 (9.45 ± 6.94 μg/m3), NO2 (24.18 ± 11.09 μg/m3), CO (0.67 ± 0.27 mg/m3), and O3 (68.77 ± 35.97 μg/m3). Among different seasons, winter exhibits the highest concentrations of air pollutants such as PM2.5, PM10, AQI, SO2, NO2, and CO, while spring demonstrates the highest levels of O3, with winter conversely showcasing the lowest O3 levels. According to the Technical Regulation on Ambient Air Quality Index (on trial) (HJ 633—2012) of China, air quality is categorized as mild pollution for an AQI range of 101–150, moderate pollution for an AQI range of 151–200, heavy pollution for an AQI range of 201–300, and severe pollution for an AQI exceeding 300. Nanchong experiences the highest number of pollution days during winter, with 2 days (0.2%) of severe pollution heavy pollution, 18 days (2.1%) of moderate pollution, 64 days (7.6%) of moderate pollution, and 245 days (29%) of mild pollution.
The Spearman correlation analysis was showed in Supplementary Table S1, daily average temperatures are negatively correlated with PM2.5 (r = −0.352), PM10 (r = −0.295), NO2 (r = −0.271), and CO (r = −0.336), while positively correlated with O3 (r = 0.592). Strong correlations are observed between air pollutants, particularly between PM2.5 and PM10 (r = 0.963). However, in contrast to areas affected by dust storms, wind speeds exhibit a negative relationship with PM2.5(r = −0.346) and PM10 (r = −0.311) (12).
Figure 2 represents meteorological parameters, air pollutants, and the number of cardiovascular disease patients from June 1, 2015, to December 31, 2023. In Nanchong, there was significant precipitation and higher temperatures in summer, as well as stronger winds in spring. Additionally, air pollutants have been decreasing since 2018.
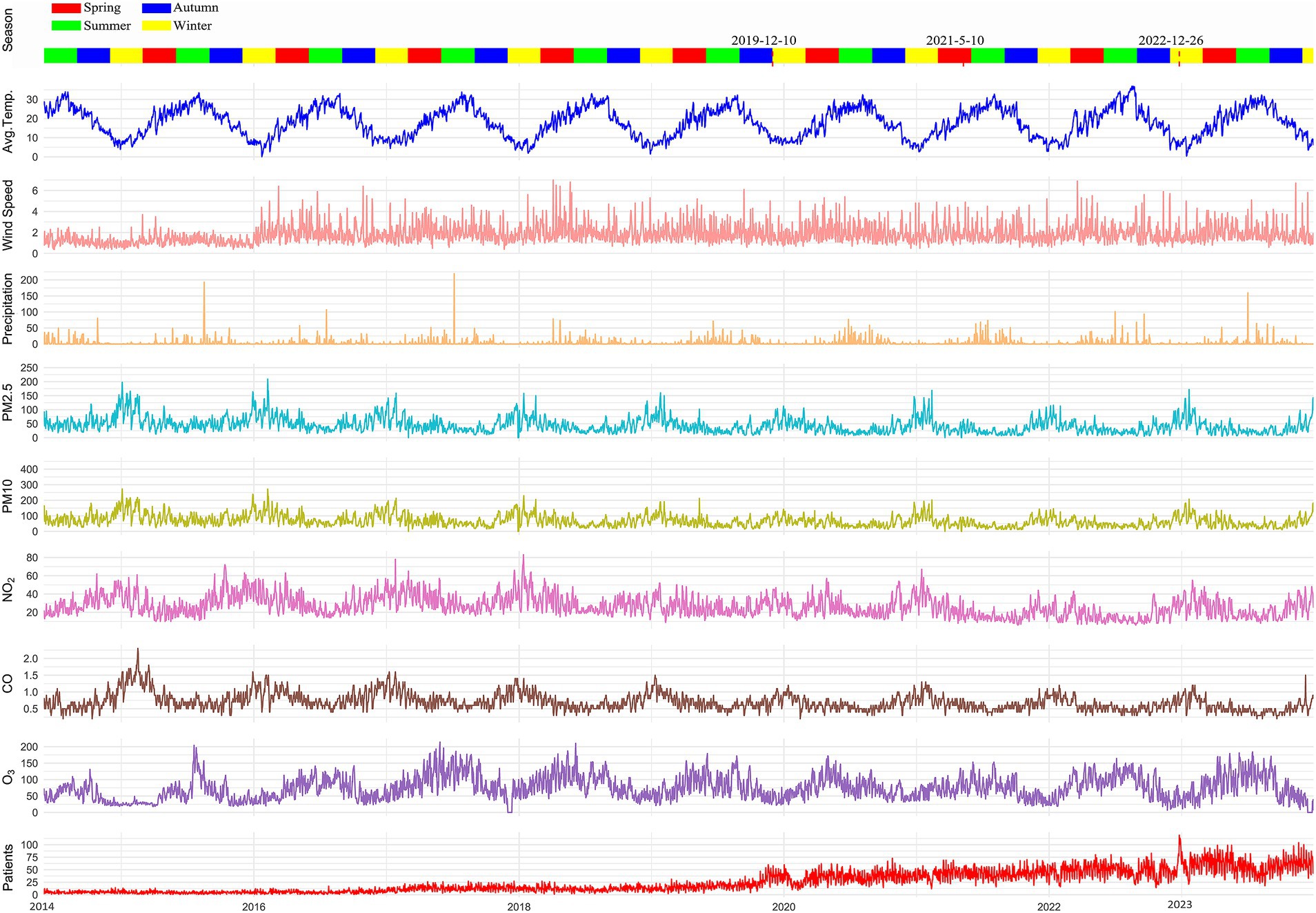
Figure 2. Local meteorological parameters and air pollutants in Nanchong from 2014 to 2023. During the COVID-19 pandemic period from December 10, 2019, to December 26, 2022, the Affiliated Hospital of North Sichuan Medical College relocated to a new campus on May 10, 2021.
The lag effects of air pollutants on the hospitalization of cardiovascular disease were displayed in Figure.3. The concentration of PM2.5 showed significant cumulative effect (lag07-lag03) and lag effects (lag2-lag5) on cardiovascular disease patients. The number of cardiovascular disease hospitalization increased by 1.15% (95%CI: 0.55–1.76%) for every 10 μg/m3 increase in the average concentration of PM2.5 for previous 7 days (lag07). At the same time, PM2.5 showed a significant lag effect from lag2 to lag6. As shown in the Figure 3, PM10 showed a stronger cumulative and lag effect. Among all patients, both the average level of PM10 over the previous 7 days (lag01-lag07) and each individual day’s level over the same period (lag1-lag7) increase the risk of cardiovascular disease hospitalization. The number of cardiovascular disease hospitalization increased by 1.17% (95%CI: 0.74–1.61%) for every 10 μg/m3 increase in the average concentration of PM10 over the previous 7 days (lag07), and by 0.51% (95%CI: 0.19–0.82%) for every 10 μg/m3 increase in PM10 increase on the seventh day prior. However, females were not sensitive to the concentration of PM10 on lag01 and lag1. The concentration of SO2 and CO in Nanchong did not affect the hospitalization of cardiovascular disease. Cumulative and single exposure to high levels of NO2 increased the risk of cardiovascular disease hospitalization. The risk increased by 6.26% (95% CI: 4.84–7.70%) for every 10 μg/m3 increase in the concentration of NO2 for lag07, and by 2.93% (95% CI: 1.90–4.02%). For all patients, O3 showed short-term cumulative effects (lag01 and lag02) and lag effects (lag1) on cardiovascular disease hospitalization. Female patients can be affected by the concentration of O3 in the previous 7 days, while males are not.

Figure 3. Excess risk (95% CI) of hospitalization for cardiovascular disease associated with an increase of 10 units of pollutant at different lag days using single-pollutant models in Nanchong, June 1, 2015, to December 31, 2023.
To assess the influence of PM2.5 and PM10 on inpatients visits for CVD across different age and gender groups. The stratified analysis was performed based on sex and age at lag0 day. Figure 4 depicted that the risk of admission for CVD among male increased by 0.48% (95%CI:0.12–0.84%) for every 10 μg/m3 increase in PM10. However, we did not observe significant associations among female. In age-specific analysis, for CVD patients aged 70 to 80 years old, the risk of hospitalization increased by 0.81%(95%CI:0.17–1.50%) and 0.72%(95% CI: 0.26–1.18%) for every 10 μg/m3 increase in PM2.5 and PM10, respectively.
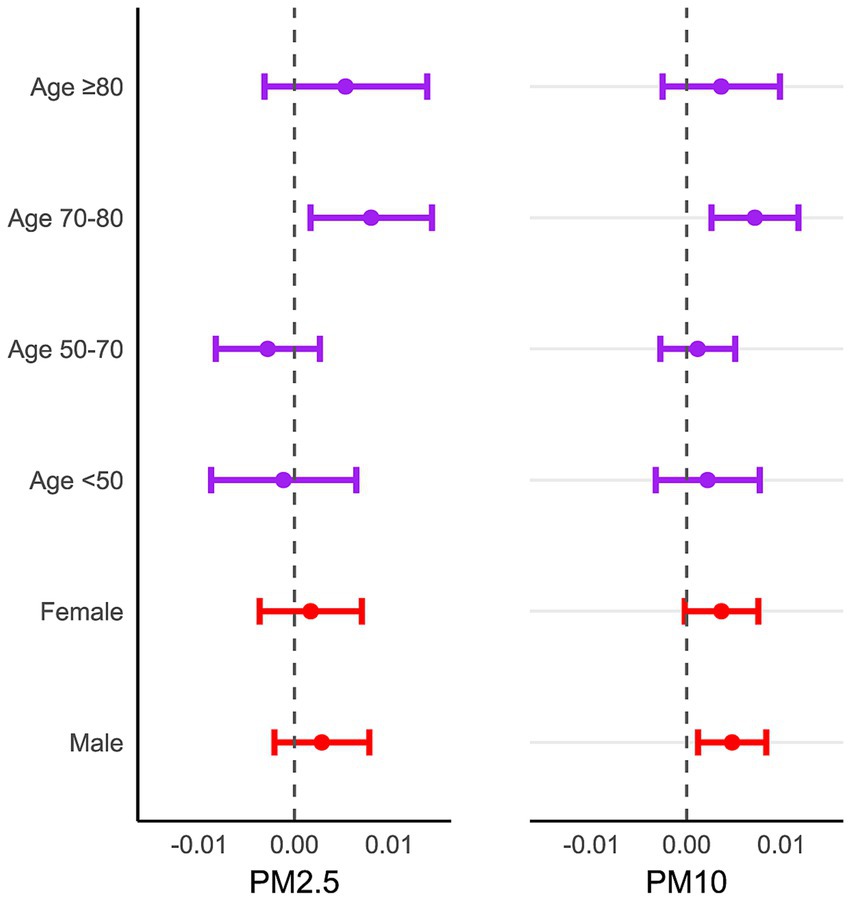
Figure 4. The excess risk (95% CI) of age and sex group in overall hospitalization for cardiovascular disease associated with a 10 μg/m3 increase in PM2.5 and PM10 on lag0 in Nanchong from June 1, 2015, to December 31, 2023.
This study represents the first attempt in Nanchong to investigate the association between air pollution and cardiovascular health. Generally, this study showed that short exposure to air pollution includes PM10, SO2, NO2 and O3 were associated with increased risk of admission among patients with cardiovascular disease. Furthermore, the effect of PM10 and SO2 on cardiovascular disease are varied by sex.
Particle matter has been adapted as a main indicator of air pollution worldwide. Particles pollutants PM10 and PM2.5 are named according to their aerodynamic diameters. The source of particles varies among different areas. For example, compared to developed counties, Pakistan suffered a higher PM2.5 concentration, in which also contain more heavy metal elements (13). Among the arid regions around the deserts such as Northern Africa, the Arabian Peninsula, Central Asia, the dust storms contribute significantly to local particle pollutant. Particles originating from dust storms typically contain mineral dust, whereas particulate matter emission by human activities is usually more complex and contains a higher proportion of organic and metal components (14, 15). However, due to the geographical location, air quality of Nanchong rarely affected by sandstorms. Therefore, the relationship between particles pollutant and wind speed in Nanchong is opposite with cities near sandstorms. In Nanchong, the wind can facilitate the dispersion of air pollutants, resulting in pollutant concentrations decreased in urban areas. Similar with most of the country, the concentration of particles matters peak during winter. This may be due to the dryness in winter promote the formation of particles matters, while adequate precipitation captures and remove aerosol particles from the atmosphere in summer (16). According to the update guidelines, WHO recommends a stricter criterion in which the recommendation daily concentration of PM2.5 was 15 μg/m3 and 45 μg/m3 for PM10 (17). Over the past 10 years in Nanchong, although the concentration of particles has continued to decrease, the average daily concentration of PM2.5 is 42.39 μg/m3, which remains significantly higher than the standard. PM10 and PM2.5 shown a great effect on human hearth due to that they can penetrate respiratory system and deposited in organ and tissues following the blood follow, especially in heart. Different from the other organs, heart is characterized as high energy demand and low repair capacity. On the one hand, PM disturb the oxidative respiratory chain and oxidation–reduction system, resulting in oxidative stress in heart. On the other hand, as a foreign substance, PM arouse inflammation response, however, inflammation response does not always clear they, resulting in continuous and excessive inflammation which promote heart disease. At the same time, particle matters also disturb the coagulation system and promote the aggravation of myocardial ischemia in coronary heart disease patients. A time-series analysis conducted in New York state also revealed that a 10 μg/m3 increment in PM2.5 concentrations contribute 1.37% increase in cardiovascular disease hospitalization (18). A prospective longitudinal cohort study conducted in Ohio found that exposure to PM2.5 increased risk of incident myocardial infarction (19). Another research conducted by Ma et al. (20) found that 10 μg/m3 increase on the concentration of PM10 was related with 14% increase in cardiovascular disease hospitalization on lag1. Furthermore, our results showed that PM2.5 has a stronger effect on cardiovascular disease compared to PM10. The greater impact of PM2.5 may be due to its smaller particles size, which results in a higher surface area. This make PM2.5 particles more likely to reach cardiovascular and exhibit higher reactivity ability (21, 22).
Since there are no volcanoes and heavy industry in Nanchong, the main source of SO2 and NO2 is the burning of fossil fuels, especially from transportation vehicles. WHO recommends 40 μg/m3 and 25 μg/m3of daily average concentrations for SO2 and NO2, respectively. In Nanchong, the daily average concentrations of SO2 and NO2 are lower than this standard. However, we also found that short exposure to SO2 and NO2 also can increase the number of hospitalizations count of cardiovascular disease patients. A study conducted in western China reported that cardiovascular admissions increased by 4.5%(95% CI 1–8.2%) for every 10 μg/m3 increase in SO2 in non-dust days (20). Mechanistic investigation revealed that SO2 induce mitochondrial and oxidation–reduction system through grapes transcriptome (23). Likewise, with pungent odor, SO2 will induce acute lung response and inflammation, which also can affect heart function through autonomic nervous system. Furthermore, most NO2 is quickly formed in the atmosphere from NO emissions by vehicles. A global assessment revealed that a 10 μg/m3 increase in NO2 concentration was associated 0.37% cardiovascular mortality among 398 cities (24). A Meta-analysis enrolled 204 time-series reported that a 10 μg/m3 increase of NO2 associated with 0.88% cardiovascular mortality (25). A prospective longitudinal observational cohort study conducted in England reported that NO2 promotes the development of cardiac remodeling and decrease cardiac pumping function (26). Moreover, NO2 has been implicated in promoting airway inflammation and increasing the airways’ vulnerability to viral infections (27). Among asthmatic children, NO2 increase the risk of respiratory viral infection and resulting in severity asthmatic (28, 29). This also contributes to the development of cardiovascular disease, especially for patients with previous heart disease.
Different from other air pollutant, O3 is not directly emitted by primary source. Nitrogen dioxide and volatile organic compounds works as a precursor in atmospheric and promote the formation of O3, in which UV radiation or thunderstorm activity is needed (30). Therefore, we can easily be found in Figure 2 that the concentration keeps a high concentration in summer and spring. The Ozone layer in atmosphere protects human from the UV radiation; however, excessive ground-level ozone is harmful to human health. Cumulative and lag effect also have been revealed in O3. The WHO recommended concentration of O3 is 60 μg/m3. In Nanchong, the average concentration of O3 is 69.63. μg/m3. A nationwide cohort conducted in China reported that per 10 μg/m3 increase in ozone concentrations related to 18.4% increase in cardiovascular disease mortality (31). As a strongly oxidative and highly reactive pollutant, O3 may induce coronary artery spasm and trigger acute episodes of ischemic heart disease (32). Furthermore, O3 also induce oxidative stress and inflammatory (33).
Consistent with previous studies, our results suggest that elder adults are more susceptible to air pollution, especially for 70–80 years old (34). Older adults are more likely suffer from chronic disease including CVD. Air pollution can trigger acute episode of CVD, leading to an increased need for urgent hospitalization. Furthermore, patients over the age of 80 usually have less outdoor activity and receive more care, which protect them from the hazards of air pollution. Compared to females, males show greater vulnerability to PM10, possibly related to that males are more likely to work outdoor, increasing their exposure to high level of particles matter. Additionally, our results reveal that the effect estimates for moving average lags were much higher than those for single day lags. This significantly indicated that the hazardous of air pollution to CVD exhibit a cumulative effect. It’s also underscores that efforts to reduce continuous exposure to air pollution yield substantial benefits.
In this study, we employed patients’ addresses from medical records to assess air pollution exposure, which may lead to exposure misclassification. Migrant workers who provided domicile addresses rather than actual residential addresses were excluded, potentially underestimating the impact of air pollution on cardiovascular disease. Additionally, factors such as traffic volume, mask-wearing, and mode of transportation were not fully accounted for, which could introduce bias. The potential impact of participant mobility within urban areas during the study period was also not addressed. While a single-pollutant model was used for simplicity, multiple-pollutant models are needed in future research to better capture real-world exposure. Finally, since the study was limited to Nanchong, caution should be exercised when generalizing the results to other regions.
Our study assesses the impact of air pollution on CVD patients in Nanchong, a region with a subtropical humid monsoon climate and mild air pollution. Our findings reveal short exposure to high concentrations of air pollution increases the risk of hospital admission for CVD. Efforts should be devoted to avoiding exposure to high and consistent levels of air pollution, especially for elder patients.
At the same time, medical institutions should prepare enough medical sources. Furthermore, patients aged 70–80 years old are more vulnerable to high air pollutant. These results suggest that older adult patients require additional care and further precautions to avoid exposure to high pollution levels. Policymakers need to develop policies to combat air pollution and ensure sufficient medical resources are available after severe air pollution days.
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding authors.
The studies involving humans were approved by Ethics Committee of the Affiliated Hospital of North Sichuan Medical College. The studies were conducted in accordance with the local legislation and institutional requirements. Written informed consent for participation was not required from the participants or the participants’ legal guardians/next of kin in accordance with the national legislation and institutional requirements. Written informed consent was not obtained from the individual(s) for the publication of any potentially identifiable images or data included in this article because since the study involved only retrospective analysis of previous clinical data, the requirement for informed consent was waived by the Ethics Committee of the Affiliated Hospital of North Sichuan Medical College.
ZZ: Data curation, Software, Supervision, Writing – original draft, Writing – review & editing. YL: Data curation, Investigation, Writing – original draft. QJ: Data curation, Investigation, Writing – original draft. FZ: Data curation, Investigation, Writing – original draft. YY: Data curation, Investigation, Writing – original draft. RY: Conceptualization, Data curation, Writing – original draft. HH: Conceptualization, Funding acquisition, Software, Supervision, Writing – review & editing. CZ: Conceptualization, Funding acquisition, Supervision, Writing – review & editing.
The author(s) declare that financial support was received for the research, authorship, and/or publication of this article. This work was supported by National Natural Science Foundation of China (Grant Nos. 82030007 and U23A20398), The Central Government Guides Local Science and Technology Development Project (Grant No. 2022ZYD0057), Major Projects of Sichuan Provincial Health Commission (21ZD004).
We are grateful to Rongrong Xu from the Chinese Research Academy of Environmental Sciences for his assistance with statistics and his valuable comments on various versions of the manuscript. We would also like to thank the reviewers for their insightful feedback, which has provided many practical suggestions for this study and future research.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The authors declare that no Gen AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fpubh.2025.1504411/full#supplementary-material
2. GBD 2021 Risk Factors Collaborators . Global burden and strength of evidence for 88 risk factors in 204 countries and 811 subnational locations, 1990-2021: a systematic analysis for the global burden of disease study 2021. Lancet. (2024) 403:2162–203. doi: 10.1016/S0140-6736(24)00933-4
3. The National Center for Cardiovascular Disease . Annual reports on cardiovascular health and disease in China. Beijing, China: Peking Union Medical College Press (2022).
4. WHO . WHO global air quality guidelines: Particulate matter (PM2. 5 and PM10), ozone, nitrogen dioxide, sulfur dioxide and carbon monoxide: Executive summary. Geneva: WHO (2021).
5. Nawsherwan, N, Mubarik, S, Naeem, S, Mubarak, R, Yu, C, Yan, W, et al. Epidemiological trends and age-period-cohort effects on cardiovascular diseases burden attributable to ambient air pollution across BRICS. Sci Rep. (2024) 14:11464. doi: 10.1038/s41598-024-62295-6
6. Liang, F, Liu, F, Huang, K, Yang, X, Li, J, Xiao, Q, et al. Long-term exposure to fine particulate matter and cardiovascular disease in China. J Am Coll Cardiol. (2020) 75:707–17. doi: 10.1016/j.jacc.2019.12.031
7. Yan, F, Liu, H, Zhang, H, Yi, L, Wu, Y, Deng, C, et al. Association between maternal exposure to gaseous pollutants and atrial septal defect in China: a nationwide population-based study. Environ Res. (2021) 200:111472. doi: 10.1016/j.envres.2021.111472
8. Yuan, X, Liang, F, Zhu, J, Huang, K, Dai, L, Li, X, et al. Maternal exposure to PM(2.5) and the risk of congenital heart defects in 1.4 million births: a Nationwide surveillance-based study. Circulation. (2023) 147:565–74. doi: 10.1161/CIRCULATIONAHA.122.061245
9. Wang, Z, Peng, J, Liu, P, Duan, Y, Huang, S, Wen, Y, et al. Association between short-term exposure to air pollution and ischemic stroke onset: a time-stratified case-crossover analysis using a distributed lag nonlinear model in Shenzhen. China Environ Health. (2020) 19:1. doi: 10.1186/s12940-019-0557-4
10. Zhong, P, Huang, S, Zhang, X, Wu, S, Zhu, Y, Li, Y, et al. Individual-level modifiers of the acute effects of air pollution on mortality in Wuhan. China Glob Health Res Policy. (2018) 3:27. doi: 10.1186/s41256-018-0080-0
11. Zhou, L, Wang, Y, Wang, Q, Ding, Z, Jin, H, Zhang, T, et al. The interactive effects of extreme temperatures and PM(2.5) pollution on mortalities in Jiangsu Province, China. Sci Rep. (2023) 13:9479. doi: 10.1038/s41598-023-36635-x
12. Liu, Y, Zhou, Y, and Lu, J. Exploring the relationship between air pollution and meteorological conditions in China under environmental governance. Sci Rep. (2020) 10:14518. doi: 10.1038/s41598-020-71338-7
13. Lu, Y, Lin, S, Fatmi, Z, Malashock, D, Hussain, MM, Siddique, A, et al. Assessing the association between fine particulate matter (PM2.5) constituents and cardiovascular diseases in a mega-city of Pakistan. Environ Pollut. (2019) 252:1412–22. doi: 10.1016/j.envpol.2019.06.078
14. Chen, S, Chen, J, Zhang, Y, Lin, J, Bi, H, Song, H, et al. Anthropogenic dust: sources, characteristics and emissions. Environ Res Lett. (2023) 18:479. doi: 10.1088/1748-9326/acf479
15. Yu, Y, and Cao, J. Chemical fingerprints and source profiles of PM10 and PM2.5 from agricultural soil in a typical polluted region of Northwest China. Aerosol Air Qual Res. (2023) 23:220419. doi: 10.4209/aaqr.220419
16. Sun, Y, Zhao, C, Su, Y, Ma, Z, Li, J, Letu, H, et al. Distinct impacts of light and heavy precipitation on PM2.5 mass concentration in Beijing. Earth Space Sci. (2019) 6:1915–25. doi: 10.1029/2019EA000717
17. WHO . WHO global air quality guidelines. Particulate matter (PM2.5 and PM10), ozone, nitrogen dioxide. Sulfur dioxide and carbon monoxide. Geneva: WHO (2021).
18. Hsu, WH, Hwang, SA, Kinney, PL, and Lin, S. Seasonal and temperature modifications of the association between fine particulate air pollution and cardiovascular hospitalization in New York State. Sci Total Environ. (2017) 578:626–32. doi: 10.1016/j.scitotenv.2016.11.008
19. Hartiala, J, Breton, CV, Tang, WHW, Lurmann, F, Hazen, SL, Gilliland, FD, et al. Ambient air pollution is associated with the severity of coronary atherosclerosis and incident myocardial infarction in patients undergoing elective cardiac evaluation. J Am Heart Assoc. (2016) 5:e003947. doi: 10.1161/JAHA.116.003947
20. Ma, Y, Zhang, H, Zhao, Y, Zhou, J, Yang, S, Zheng, X, et al. Short-term effects of air pollution on daily hospital admissions for cardiovascular diseases in western China. Environ Sci Pollut Res Int. (2017) 24:14071–9. doi: 10.1007/s11356-017-8971-z
21. Chen, YH, Nguyen, D, Brindley, S, Ma, T, Xia, T, Brune, J, et al. The dependence of particle size on cell toxicity for modern mining dust. Sci Rep. (2023) 13:5101. doi: 10.1038/s41598-023-31215-5
22. Marchini, T, Zirlik, A, and Wolf, D. Pathogenic role of air pollution particulate matter in Cardiometabolic disease: evidence from mice and humans. Antioxid Redox Signal. (2020) 33:263–79. doi: 10.1089/ars.2020.8096
23. Chirumbolo, S, and Bjørklund, G. Commentary: sulfur dioxide contributes to the cardiac and mitochondrial dysfunction in rats. Front Cardiovasc Med. (2016) 3:15. doi: 10.3389/fcvm.2016.00015
24. Meng, X, Liu, C, Chen, R, Sera, F, Vicedo-Cabrera, AM, Milojevic, A, et al. Short term associations of ambient nitrogen dioxide with daily total, cardiovascular, and respiratory mortality: multilocation analysis in 398 cities. BMJ. (2021) 372:n534. doi: 10.1136/bmj.n534
25. Mills, IC, Atkinson, RW, Kang, S, Walton, H, and Anderson, HR. Quantitative systematic review of the associations between short-term exposure to nitrogen dioxide and mortality and hospital admissions. BMJ Open. (2015) 5:e006946–6. doi: 10.1136/bmjopen-2014-006946
26. Fecht, D, Chadeau-Hyam, M, Owen, R, Gregson, J, Halliday, BP, Lota, AS, et al. Exposure to elevated nitrogen dioxide concentrations and cardiac remodeling in patients with dilated cardiomyopathy. J Card Fail. (2022) 28:924–34. doi: 10.1016/j.cardfail.2021.11.023
27. Frampton, MW, Boscia, J, Roberts, NJ, Azadniv, M, Torres, A, Cox, C, et al. Nitrogen dioxide exposure: effects on airway and blood cells. Am J Phys Lung Cell Mol Phys. (2002) 282:L155–65. doi: 10.1152/ajplung.2002.282.1.L155
28. Chauhan, AJ, Inskip, HM, Linaker, CH, Smith, S, Schreiber, J, Johnston, SL, et al. Personal exposure to nitrogen dioxide (NO2) and the severity of virus-induced asthma in children. Lancet. (2003) 361:1939–44. doi: 10.1016/S0140-6736(03)13582-9
29. Kirwa, K, Eckert, CM, Vedal, S, Hajat, A, and Kaufman, JD. Ambient air pollution and risk of respiratory infection among adults: evidence from the multiethnic study of atherosclerosis (MESA). BMJ open. Respir Res. (2021) 8:e000866. doi: 10.1136/bmjresp-2020-000866
30. National Academies Press . Rethinking the Ozone Problem in Urban and Regional Air Pollution. Washington, DC: National Academies Press (1991).
31. Niu, Y, Zhou, Y, Chen, R, Yin, P, Meng, X, Wang, W, et al. Long-term exposure to ozone and cardiovascular mortality in China: a nationwide cohort study. Lancet Planet Health. (2022) 6:e496–503. doi: 10.1016/S2542-5196(22)00093-6
32. Srebot, V, Gianicolo, EAL, Rainaldi, G, Trivella, MG, and Sicari, R. Ozone and cardiovascular injury. Cardiovasc Ultrasound. (2009) 7:30. doi: 10.1186/1476-7120-7-30
33. Mirowsky, JE, Carraway, MS, Dhingra, R, Tong, H, Neas, L, Diaz-Sanchez, D, et al. Ozone exposure is associated with acute changes in inflammation, fibrinolysis, and endothelial cell function in coronary artery disease patients. Environ Health. (2017) 16:126. doi: 10.1186/s12940-017-0335-0
34. Dehghani, S, Vali, M, Jafarian, A, Oskoei, V, Maleki, Z, and Hoseini, M. Ecological study of ambient air pollution exposure and mortality of cardiovascular diseases in elderly. Sci Rep. (2022) 12:21295. doi: 10.1038/s41598-022-24653-0
Keywords: air pollutants, cardiovascular disease, environmental epidemiology, human health, cardiovascular disease hospitalization
Citation: Zheng Z, Li Y, Jiang Q, Zang F, Yu Y, Yue R, Hu H and Zhang C (2025) Associations between air pollution and hospitalization for cardiovascular disease: a time series study in Nanchong. Front. Public Health. 13:1504411. doi: 10.3389/fpubh.2025.1504411
Received: 30 September 2024; Accepted: 25 February 2025;
Published: 07 March 2025.
Edited by:
Fabio Scarpa, University of Sassari, ItalyReviewed by:
Priyanka Shah, Indian Institute of Public Health Gandhinagar (IIPHG), IndiaCopyright © 2025 Zheng, Li, Jiang, Zang, Yu, Yue, Hu and Zhang. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Chunxiang Zhang, emhhbmdjaHg5OTlAMTYzLmNvbQ==; Houxiang Hu, aGh4aWFuZ0Buc21jLmVkdS5jbg==
†These authors have contributed equally to this work
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.