- Department of Nursing, The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, China
Background: Patients with prostate cancer (PCa) benefit significantly from pelvic floor exercises, but recent results indicate that these exercises have not been fully promoted in clinical settings. This scoping review aimed to identify the facilitators of and barriers to pelvic floor muscle training (PFMT) in PCa survivors.
Methods: A scoping review was conducted in November 2022. Relevant studies were identified from CINAHL, Embase, PubMed, PsycINFO, and Web of Science databases from their inception to 20 November 2022. Data were analyzed and extracted by two formally trained researchers.
Results: A total of 53 studies were included, most of which were randomized controlled trials. The Tailored Implementation for Chronic Diseases (TICD) model framework was used to identify the contents of seven barriers and promotion areas, as well as a series of sub-domains. The most common barriers to implementing pelvic floor muscle training (PFMT) included the following: the lack of a common scheme in guidelines and the measurement of common standardized outcomes, inadequate self-monitoring or feedback from healthcare professionals to improve PFMT compliance, poor patient compliance, and a lack of implementation equipment and financial support. Good treatment effects and easy operation were the facilitators of PFMT.
Conclusion: The implementation of PFMT faces several challenges and opportunities that should be understood thoroughly before implementation. In terms of guidelines and clinical practice, more work is needed, and the possibility of PFMT implementation in various hospitals and community health centers or clinics should be considered.
1. Introduction
In 2021, prostate cancer (PCa) surpassed lung cancer as the second most prevalent tumor-specific cause of death among men globally (1). In 2020, it was predicted to cause 1.4114 million new cases and 375,000 fatalities worldwide (2). The incidence rates are rising globally, particularly in Asia, Northern Europe, and Western Europe (3). Although radical prostatectomy can increase a patient’s chance of survival, it can also disrupt their body’s natural function, reduce masculinity (4), and result in poor quality of life (QoL) (5). Despite improved treatment regimes, PCa treatment has several side effects. Urinary incontinence (UI) and erectile dysfunction (ED) were the most common complications of radical prostate resection (6). UI frequently occurs after catheter removal, and it has a significantly negative impact on a patient’s function and health-related QoL, particularly in the first 6 months after surgery. Patients who have UI after radical prostatectomy are typically advised to seek conservative treatment. Common conservative treatment strategies include behavior modification and pelvic floor muscle exercises (PFMEs), lifestyle education, artificial urinary sphincter, and pharmacological treatments (7). All conservative treatment trials after radical prostatectomy show moderate evidence that pelvic floor muscle training (PFMT) has an overall benefit in reducing UI compared with control management (8).
PFMT is an affordable and uncomplicated procedure that can help with bladder control, bowel control, and sexual function, and it can reduce the likelihood of UI. To prevent an increase in intra-abdominal pressure, PFMT is provided to participants to teach them how to use biofeedback to synchronize their voluntary pelvic floor muscle contractions and time them precisely (8). Biofeedback refers to the use of specific equipment for visual and auditory feedback training during pelvic floor muscle functional exercises to strengthen the muscles involved. The theory behind PFMT is that the pelvic floor may become stronger and more effective if specific pelvic floor muscles are repeatedly and voluntarily contracted during increased intra-abdominal pressure, which will inhibit detrusor activity (9). Additionally, PFMT may cause the periurethral tissues to increase external mechanical urethral pressure (10). It is believed that repeated contractions can improve voiding control by increasing support for the detrusor and urethral sphincter muscles. PFMT includes different modalities such as simple Kegel exercises, biofeedback (verbal or machine-mediated), electrical stimulation (ES) via surface electrodes, and extracorporeal magnetic innervation (8). These interventions can be compared with each other—individually or in combination—and to no treatment.
The advantages of pelvic floor rehabilitation exercise after PCa diagnosis include improvements in continence in the short term (11), reductions in nocturia and decreased use of pads (12), improvements in ED results (13), and rapid improvements in QoL (14). It has been shown that exercise of the pelvic floor muscles is safe for older PCa patients with signs of advanced disease, such as bone metastases. PFMT is a critical intervention for cancer patients since it significantly reduces certain adverse effects of treatment (15). Active pelvic floor exercises help avoid UI by improving muscle strength and endurance. Guidelines (16, 17) suggest that PFMT alone or combined with biofeedback or ES is effective in treating postprostatectomy incontinence (PPI). The timing of pelvic floor muscle functional exercises for PCa includes preoperative and postoperative radical prostatectomy for PCa, and both preoperative and postoperative PFMT can improve UI (15).
Despite extensive research in recent years indicating that PFMT can help reduce UI after prostatectomy, it has not been widely promoted in a significant proportion of hospitals and communities due to human and social factors. During clinical care rehabilitation, there is a significant gap between postoperative exercises for PCa and evidence-recommended practices of guidelines. This review aimed to understand the promotion, motivations, preferences, and barriers to PTME participation among men after PCa surgery by conducting a thorough literature search.
2. Methods
We conducted a scoping review of the literature on PFMT among men with PCa, following the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines (18). The scoping review is a rigorous method for mapping research and presenting results in a format that is accessible to knowledge users and is an increasingly common approach to mapping broad topics. The six-step framework prescribed by Arksey and O’Malley, advanced by Levec et al. (19), includes (1) identifying the research question, (2) identifying relevant literature, (3) selecting the relevant study, (4) charting the data, and (5) collating, summarizing, and reporting the data. The review team included knowledge users and a PCa survivor involved in the consultation process. The team was formed to ensure that the findings are relevant to physical activity and exercise provision efforts and to facilitate the dissemination of findings.
2.1. Identifying the research question
The researchers discovered the research problem through an early literature review. Our research topic focused on the factors, preferences, and barriers to PFMT in men with PCa. PFMT, previously also known as Kegel exercises, is a behavioral training method to prevent and treat UI by strengthening the pelvic floor muscle that supports the pelvic organs through the voluntary and repetitive contraction and relaxation of the pelvic floor muscles. For the purposes of this review, the following forms of functional exercises for the pelvic floor muscles were included: PFMT alone, PFMT with biofeedback, ES with PFMT and biofeedback, and pelvic floor education.
2.2. Identifying relevant literature
The search strategy was developed after consulting a reference librarian who suggested using MeSH terms to find the most relevant studies and public health specialists in systematic reviews. It was developed in consultation with a health sciences librarian specialized in PFMT after PCa surgery to ensure an appropriate and thorough search of the literature. Articles were searched in PubMed, CINAHL, Embase, PsycINFO, and Web of Science databases. The timeframe of the literature search was from the database inception to 20 November 2022. The following key search terms were searched in each database: (PCa OR prostate neoplasm OR prostatic neoplasms OR prostate tumor) AND (pelvic floor muscle training OR pelvic floor muscle exercise OR pelvic floor muscle strengthening OR Kegel exercise OR PFMT/PFE/PFME). Hand searching the reference lists of included studies identified additional pertinent articles for evaluation. All included studies were limited to those published in English language.
2.3. Selecting the relevant study
The following principles governed the inclusion and exclusion criteria of the review. The subjects were patients undergoing radical prostatectomy. The interventions included pelvic floor muscle training to prevent UI or to improve sexual function, QoL, and other outcome indicators. The type of research articles included were original peer-reviewed publications (randomized controlled trials, cross-sectional studies, and mixed-methods studies); meta-analyses, reviews, study protocols, abstracts, posters, conference papers, fertility studies, animal studies, and editorial comments were excluded.
2.4. Charting of the data
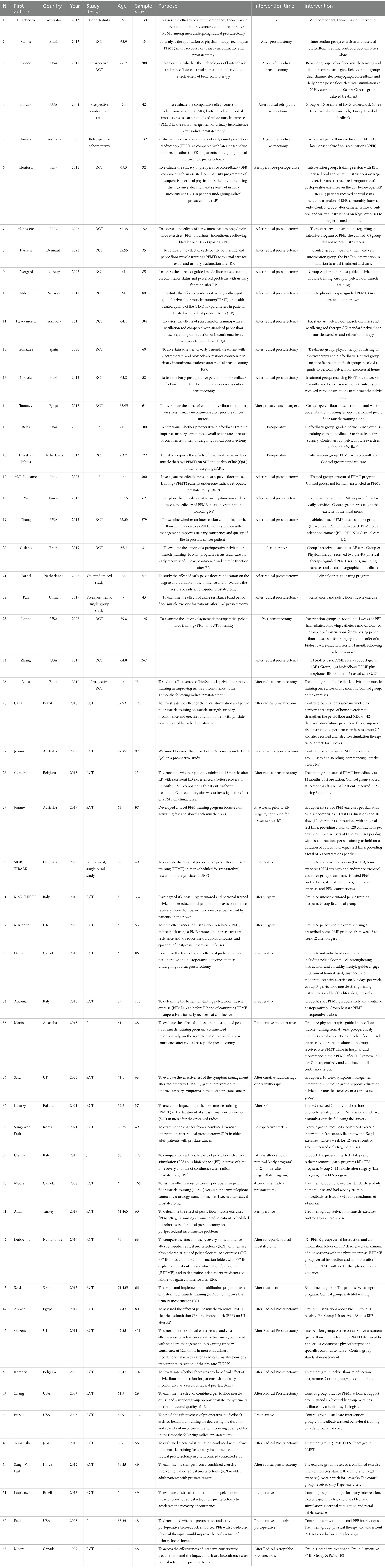
Two authors (LJ and YQ) independently screened the titles of the identified references and excluded ineligible studies. One author (LJ) screened all the abstracts and ranked them as relevant, irrelevant, or unsure. The second author (YQ) double-screened 50% of the abstracts to ensure consistent application of the eligibility criteria. Two authors extracted data using standardized checklists to assess the quality of studies and evidence synthesis. A third author (ZY) arbitrated studies when the first two authors were uncertain about their eligibility. Studies ranked as irrelevant by both reviewers were excluded. The following information was extracted: first author, country, year, study design, age, sample size, the purpose of the study, intervention time, and details of intervention methods. Any differences in opinion were resolved through discussion.
2.5. Collating, summarizing, and reporting the data
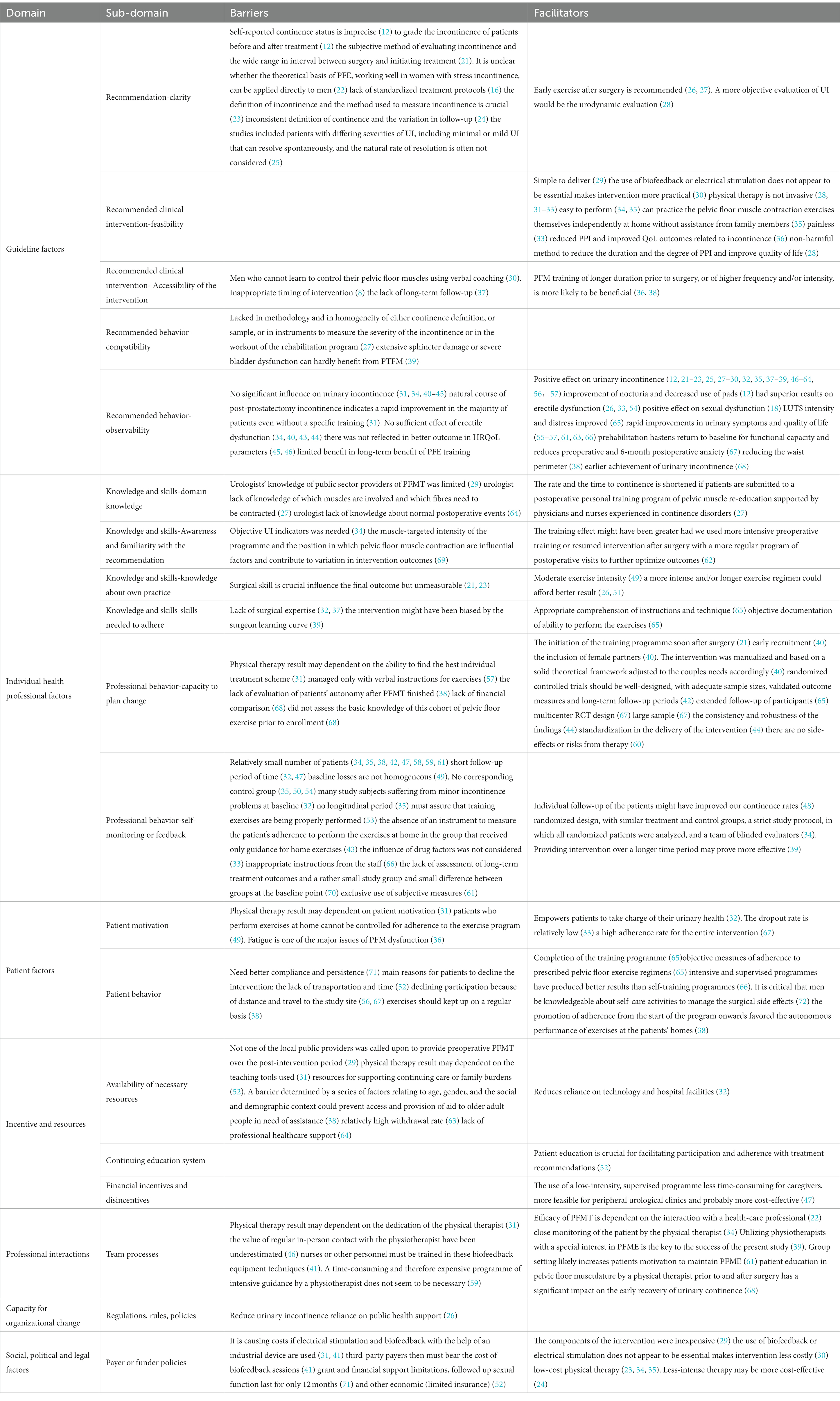
The research team created a summary of all the facilitators and barriers in accordance with the framework of the Tailored Implementation for Chronic Diseases (TICD) (20) to identify the important practice factors (see Table 1). The concept of practice determinants is categorized into seven TICD domains, namely, guidelines factors, personal health professional factors, patient factors, professional interactions, incentives and resources, organizational change capabilities, and social, political, and legal variables. According to the research team, the framework is ideal for summarizing the application and implementation of an intervention strategy. We identified and coded promoters and obstacles using deductive and inductive topic methods to map the data (73). From the findings of each publication, one of the authors (YQ) retrieved the barriers or facilitators that were initially gathered. Thematic synthesis was used to arrange the facilitators and barriers into recurrent themes in the studies, considering the frequency of reports (Table 1) or the number of times they were designated as relevant issues in specific investigations. The quantity of replies usually determines the frequency of barriers or facilitators in quantitative studies (questionnaires). Therefore, the more prevalent subjects in the literature are viewed as the typical deterrents or promoters of PFME modifications.
3. Results
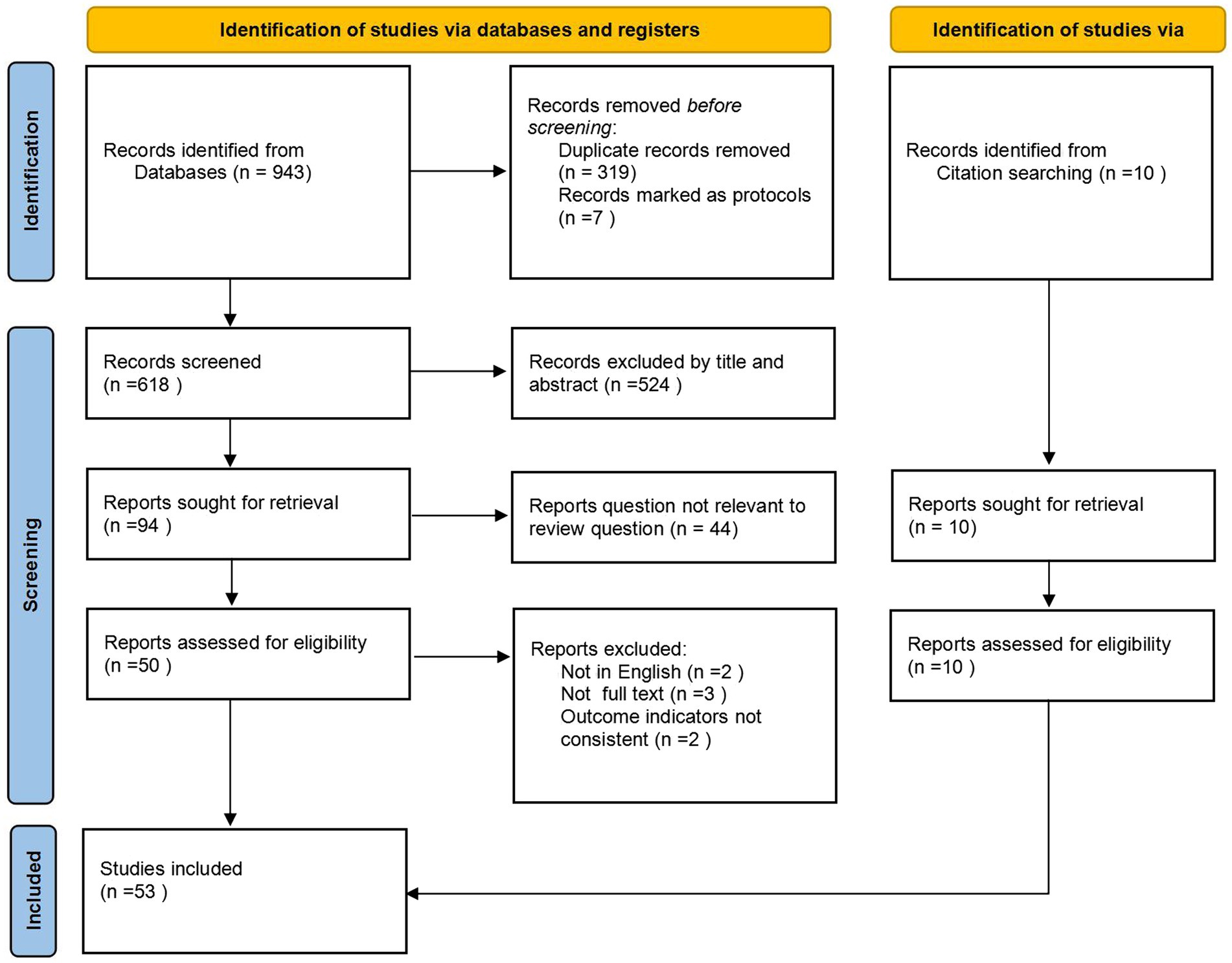
The search yielded 943 individual citations after removing 319 duplicate citations. Following the screening of titles and abstracts, 94 articles were selected for full-text review. Fifty-three met the inclusion criteria and are represented in this scoping review. See Figure 1 for the PRISMA flowchart.
Of these 53 studies, nine studies were from the United States, six from Brazil, six from Italy, four from Australia, three from the Netherlands, three from the United Kingdom, three from Canada, two from Germany, Denmark, Norway, Spain, Egypt, and South Korea, and one each from China, Taiwan, Poland, Japan, and Turkey. There were 41 randomized controlled trials, two cohort studies, and six articles that did not specify the study design. The three included studies were published by the same person, two studies were published by three others, and the two articles by Joanne were based on the same study. Therefore, data from these studies were counted only once in the total sample size calculation. In all 42 studies where age was reported, the mean age of all patients was 63.77 years. The cumulative number of participants was 5,521. The characteristics of the included studies are given in Table 2.
3.1. Guideline factors
3.1.1. Barriers
Inconsistent definition, measurement criteria, and treatment: Four studies mentioned inconsistent definition, measurement, and treatment (12, 23, 24, 42). Many of the mentioned trials lacked standardized outcome measures (23). The definition of UI varied in almost all studies. The means of measuring QoL were different, and the type of pad test was also different (20 min, 1 h, 24 h, number of pads, weight of pads, and number of men using pads, etc.). Only by aligning these definitions to the guidelines can the degree of improvement in incontinence following PFMT be measured more accurately.
Various influencing factors of the intervention effect: When establishing a clinical intervention program, the program’s accessibility and the appropriate duration of the intervention should be considered. Verbal instruction in PFMT for postoperative PCa patients is insufficient (30). The compatibility of the recommended behavior refers to how closely the recommended behavior matches the actual behavior. People with certain functional impairments who are unlikely to benefit from PTFM should also be excluded.
PFMT was found to be ineffective in improving UI in eight studies (31, 34, 40–45) and ED in four studies (34, 40, 43, 44); two other studies (45, 46) concluded that pelvic floor muscles were ineffective in improving patients’ QoL (see Table 1).
3.1.2. Facilitators
3.1.2.1. Simple and practical intervention
PFMT has significant advantages in terms of feasibility, including the simplicity of pelvic floor exercises (29), the non-invasive nature of the physiotherapy approach (33), and the fact that some studies indicate that the use of biofeedback or ES does not appear to matter, making the intervention more practical (30).
3.1.2.2. Obvious benefits of intervention
Thirty-five studies concluded that pelvic floor exercises are effective in improving UI in patients, three studies found that PFMT improves ED, and six studies found that PFMT improves QoL in postoperative patients. Studies have shown that exercise improves anxiety and depression in patients. Prior to surgery, PFMT of greater duration, frequency, or intensity is more likely to be beneficial (see Table 1).
3.2. Individual health professional factors
3.2.1. Barriers
Limited healthcare professionals’ knowledge and skills: A lack of knowledge or expertise among target healthcare professionals, especially urologists, about the target condition affects the conduct of clinical PFMT (29). The extent to which the target healthcare professionals understand and are familiar with the recommendations affects the conduct of PFMT, such as the intensity of the program and the position in which pelvic floor muscles contract. Interventions may be biased due to the surgeon’s learning curve.
Targeted healthcare professionals can self-monitor or provide feedback to enhance compliance with recommendations. The main problems presented here include issues with the experimental setup during PFMT, the relatively small number of patients (34, 35, 38, 42, 47, 58, 59, 61), and the short follow-up period, among others.
Lack of optimal individual treatment: Healthcare professionals can plan the necessary changes to which they can adhere to. However, this can be a hindrance when healthcare professionals conduct PFMT with problems in the setting of the experiment, such as the failure to establish an optimal individual exercise regimen.
3.2.2. Facilitators
Experienced physicians and nurses: The support of physicians and nurses experienced in voiding disorders can shorten the speed and time to achieve voiding (26). Surgeons with a thorough understanding of instructions and techniques can greatly assist patients in adequately performing PFMT.
The facilitating factors were analyzed using a rigorous study protocol with all randomized patients, and an evaluation panel that was blinded and provided the intervention over as long a period as possible was shown to be more effective. Randomized controlled trials should be well-designed, involving multicenter trials with adequate sample sizes; they should utilize validated outcome measures and implement long-term follow-up procedures (67). Sophisticated experimental designs will result in better PFMT exercise.
3.3. Patient factors, patient motivation, and patient behavior
3.3.1. Barriers
PFMT results may depend on patients’ motivation (31). Failure to ensure patient compliance and adherence to exercise leads to uncertainty in the effectiveness of exercise (49, 71). Four studies highlighted fatigue, lack of transportation and time, and long distance to study sites as reasons why patients at home declined to exercise consistently (36, 52, 56, 67). Physical exercise requires better compliance and persistence and should be performed regularly.
3.3.2. Facilitators
Patients take charge of their urinary health, and self-care activities contribute to improving compliance and adherence to exercise (32, 72). Moreover, intensive and supervised programs have produced better results than self-training programs (66).
3.4. Incentive and resources
3.4.1. Barriers
Three studies reported that the lack of professional healthcare, continuing care, and family burden hindered PFMT implementation (38, 55, 64). For instance, a study reported that no local public provider was called upon to provide preoperative PFMT over the post-intervention period (29). Furthermore, a range of factors related to age, gender, social, and demographic background may prevent the accessibility and availability of assistance and the lack of professional healthcare support for older adults in need (64).
3.4.2. Facilitators
The characteristics of PFMT exercise make it less dependent on technology and hospital facilities (32). A continuing education system is crucial to facilitate participation and adherence to treatment recommendations. The use of a low-intensity, supervised program will be more cost-effective for peripheral urological clinics.
3.5. Professional interactions
3.5.1. Barriers
Team processes of PFMT as a teamwork operation: The results depend considerably on the unity and cooperation among the members. Some studies suggest frequent collaboration with a physiatrist (31), while others argue that it is unnecessary (59). Physical therapy is dominated by physical therapists, so the results are often related to the dedication of physical therapists (31). Intensive instruction from a physical therapist is often time-consuming and expensive, which seems unnecessary (59). As the professionals closest to the patients, nurses who lack knowledge about or experience in biofeedback equipment techniques should be trained (41).
3.5.2. Facilitators
Physiotherapists who educate patients about pelvic floor muscles before and after surgery have a significant impact on early recovery from incontinence (64). Close monitoring by physiotherapists and physiotherapists’ interests are significant factors in the effectiveness of PFMT (39). Moreover, effective interaction between patients and healthcare professionals contributes to the effectiveness of PFMT (51).
3.6. Capacity for organizational change
Regulations, rules, and policy barriers: Some studies believe that the public health sector has limited support for pelvic floor exercise (26). Therefore, healthcare personnel should reduce UI reliance on public health support.
3.7. Social, political, and legal factors
3.7.1. Barriers
The payer or funder policy may affect the implementation of necessary changes if using ES and biofeedback. Additional expenses may be incurred because of specialized equipment (31, 41).
Third-party payers must bear the cost of biofeedback sessions (41). Funding and financial support are limited by a follow-up of sexual function lasting only 12 months (71) and other economic factors (limited insurance) (52).
3.7.2. Facilitators
Regardless of biofeedback or ES, pelvic floor exercises and psychotherapy are inexpensive, and even less-intense interventions can be effective (23, 24, 29, 30, 34, 35).
4. Discussion
This scoping review aimed to map the literature on the implementation of PFMT in PCa and provide an opportunity to identify research gaps, types, and sources of evidence to guide clinical practice. It highlights the barriers and facilitators affecting PFMT implementation in clinical practice. The findings of this review show that men diagnosed with PCa can encounter personal and social enhancements on the one hand, but on the other hand, they also need to face some obstacles in the process of participation. These barriers and facilitators mainly originate from four aspects: the design of research schemes, healthcare professionals, patient factors, and policy or social support. Many of the factors identified as barriers were also facilitators—healthcare professionals with extensive experience may be helpful for study development and for improving patient adherence (27), but healthcare professionals can also hinder patient adherence when their knowledge and skills are limited (64). This scoping review also identified that men PCa patients face similar obstacles to other older adult cancer patients when participating in PFMT exercises, such as cancer treatment side effects, age-related functional decline, a lack of time, and long distances from medical institutions (52, 67). A multidisciplinary team (MDT) including physiotherapists, nurses, and clinical scientists is essential for effective PFMT implementation and coordination. It has been reported that a group setting may increase patients’ motivation to maintain PFME and improve their enthusiasm for participation (61).
4.1. Unified standards
Most trials included in this review followed different protocols in terms of intervention type, duration, and intensity. A large and powerful test using the general scheme and the general standardized outcome measurement is required to determine the effect of the PFMT of a specific scheme. A replication study using similar protocols in different populations can also help determine the populations that may benefit from specific conservative management methods (12). The definition and measurement of outcomes differed between the included tests. Future trials should use widely accepted and validated outcome indicators, such as those of the International Continence Society (ICS) (25). The main outcome indicator should be the self-reported user interface of participants or its impact on their QoL (74). Other objective measurement methods, such as the urine pad test or a urine diary, can determine whether urine control has been achieved. Details on the implementation of specific PFMT and the measurement criteria should be considered when formulating the guidelines. In summary, carefully designed clinical trials are needed to clarify the role of PFMT.
4.2. Guidance from healthcare professionals
Implementing a recommendation based on knowledge and skill may require targeted efforts to disseminate that new knowledge or skill (20). The targeted healthcare professionals may relapse to previous behaviors, forget to adhere, lack the necessary support or resources to maintain adherence, or lack time or skills to plan necessary changes. Therefore, before developing an intervention program for implementation, it is essential to gather routinely collected data on human resources for health, conduct interviews, or hold focus group discussions with targeted healthcare professionals.
4.3. Personalized exercise program
According to the literature, the exercise prescription recommended by tumor team members (such as doctors or nurses) can help improve cancer patients’ exercise compliance (75, 76). In clinical practice, however, doctors and nurses rarely guide patients through detailed PFMT, often limiting their instructions to oral guidance only. From a research standpoint, given the specific needs of PCa patients, we should emphasize the adjustment and adaptation of personalized preferences and needs. Additionally, considering the challenges and obstacles related to the side effects of treatment and functional decline, further research is needed to examine the factors related to the persistence of exercise in this population and to explore more feasible and convenient operation sites and methods. Furthermore, it is necessary to broaden the scope, including investigating group-based, supervised, and remote online exercise programs at home and to remove barriers for PFMT implementation related to acceptability, preferences, and potential obstacles.
4.4. Assistance with equipment
This study found that the patient transfer and communication process between different levels of care—between health and social services and between target healthcare professionals and target patients—is critical for successfully implementing PFMT. PFMT intervention strategies are frequently resource-intensive, necessitating personnel, equipment, and clinic space (76). When performing contraction exercises, patients frequently struggle to determine whether the contraction mode is correct. Consequently, some equipment and instruments are critical for patients following PCa surgery (41). Teamwork is essential for the correct and standardized implementation of PFMT, particularly physical rehabilitation assistance. Some studies believe that the efficacy of PFMT depends on interactions with healthcare professionals (51) because exercise in interaction and motivation improves enthusiasm. Regarding regulations, rules, policies, and payers or funders, the rehabilitation costs of PFMT should be considered in the scope of medical insurance as soon as possible. Many hospitals and communities have struggled to implement PFMT due to the lack of specialized equipment for measuring ES, biofeedback, and patient muscle contraction strength.
4.5. Patient’s mastery of their condition
Studies have confirmed the importance of patients’ motivation to participate in the exercise process (31). In a randomized controlled clinical trial, patients with persistent UI and PCa implemented PFME practice and symptom self-management under peer support. The results showed that the symptoms and incontinence problems in the intervention group were less severe than those in the control group. This patient-centered approach reduces the dependence on technology and hospital facilities and enables patients to be responsible for their urinary health (32). Furthermore, the ability or perceived ability of targeted healthcare professionals to motivate patients to adhere is also critical.
In summary, PFMT is still in the initial stage of application in domestic patients with PCa after surgery and faces many obstacles in the promotion process. It is necessary for medical staff and health management departments to overcome the obstacles together and promote its clinical application in PCa to improve postoperative UI and patients’ QoL.
This scoping review adds to the existing literature and highlights new findings, closing the knowledge–practice gap. Future research on overcoming barriers and maximizing facilitators is needed to improve, modify, or complement existing evidence on PFMT implementation practices.
5. Limitations
First, although we conducted a thorough search using broad selection criteria, we might have missed some published papers in this field. We could not screen titles and abstracts independently due to resource constraints, which might have affected the included research. Second, not all the studies included in this article were subjected to rigorous quality control, and there is the possibility of an uneven hierarchy in the study settings. Third, although two researchers summarized all the factors that promoted or hindered PFMT implementation, some personal subjectivity might have affected the results when summarizing descriptive information.
6. Conclusion
Our study identified multiple barriers to and facilitators of PFMEs in PCa patients in a practical environment. This study is an important step toward rationally designing intervention measures. To promote PFMEs among PCa patients, targeted public health intervention measures should use social relations and social support to exercise pelvic floor muscles in PCa patients after surgery.
Data availability statement
The original contributions presented in the study are included in the article/supplementary material, further inquiries can be directed to the corresponding author.
Author contributions
LW wrote the manuscript, analysis and interpretation of the data. YL drafting the article or revising it critically for important intellectual content. ZQ helped final approval of the version to be submitted. WW formed the conception and design of the study. All authors contributed to the article and approved the submitted version.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Siegel, RL, Miller, KD, Fuchs, HE, and Jemal, A. Cancer statistics, 2021. CA Cancer J Clin. (2021) 71:7–33. doi: 10.3322/caac.21654
2. Sung, H, Ferlay, J, Siegel, RL, Laversanne, M, Soerjomataram, I, Jemal, A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. (2021) 71:209–49. doi: 10.3322/caac.21660
3. Bray, F, Ferlay, J, Soerjomataram, I, Siegel, RL, Torre, LA, and Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries [J]. CA Cancer J Clin. (2018) 68:394–424. doi: 10.3322/caac.21492
4. Green, R. Maintaining masculinity: moral positioning when accounting for prostate cancer illness. Health (London). (2021) 25:399–416. doi: 10.1177/1363459319851555
5. Park, SW, Kim, TN, Nam, JK, Ha, HK, Shin, DG, Lee, W, et al. Recovery of overall exercise ability, quality of life, and continence after 12-week combined exercise intervention in elderly patients who underwent radical prostatectomy: a randomized controlled study. Urology. (2012) 80:299–306. doi: 10.1016/j.urology.2011.12.060
6. Marchioni, M, Primiceri, G, Castellan, P, Schips, L, Mantica, G, Chapple, C, et al. Conservative management of urinary incontinence following robot-assisted radical prostatectomy. Minerva Urol Nefrol. (2020) 72:555–62. doi: 10.23736/S0393-2249.20.03782-0
7. Kirages, Daniel J. PT, DPT, OCS, FAAOMPT; Johnson, Eileen V. PT, DPT, WCS. Pelvic floor muscle rehabilitation to improve sexual function in geriatric men. Top Geriat Rehabilit. 32:174–81.
8. Anderson, CA, Omar, MI, Campbell, SE, Hunter, KF, Cody, JD, and Glazener, CM. Conservative management for postprostatectomy urinary incontinence. Cochrane Database Syst Rev. (2015) 1:CD001843. Published 2015 Jan 20. doi: 10.1002/14651858.CD001843.pub5
9. Hodges, PW, Stafford, RE, Hall, L, Neumann, P, Morrison, S, Frawley, H, et al. Reconsideration of pelvic floor muscle training to prevent and treat incontinence after radical prostatectomy. Urol Oncol. (2020) 38:354–71. doi: 10.1016/j.urolonc.2019.12.007
10. Kübler, HR, Tseng, TY, Sun, L, Vieweg, J, Harris, MJ, and Dahm, P. Impact of nerve sparing technique on patient self-assessed outcomes after radical perineal prostatectomy. J Urol. (2007) 178:488–92. doi: 10.1016/j.juro.2007.03.100
11. Radadia, KD, Farber, NJ, Shinder, B, Polotti, CF, Milas, LJ, and Tunuguntla, HSGR. Management of postradical prostatectomy urinary incontinence: a review. Urology. (2018) 113:13–9. doi: 10.1016/j.urology.2017.09.025
12. Santos, NA, Saintrain, MV, Regadas, RP, da Silveira, RA, and de Menezes, FJ. Assessment of physical therapy strategies for recovery of urinary continence after prostatectomy. Asian Pac J Cancer Prev. (2017) 18:81–6. Published 2017 Jan 1. doi: 10.26417/ejnm.v1i1.p53-58
13. Lin, YH, Yu, TJ, Lin, VC, Wang, HP, and Lu, K. Effects of early pelvic-floor muscle exercise for sexual dysfunction in radical prostatectomy recipients. Cancer Nurs. (2012) 35:106–14. doi: 10.1097/NCC.0b013e3182277425
14. Mariotti, G, Salciccia, S, Innocenzi, M, Gentilucci, A, Fasulo, A, Gentile, V, et al. Recovery of urinary continence after radical prostatectomy using early vs late pelvic floor electrical stimulation and biofeedback-associated treatment. Urology. (2015) 86:115–21. doi: 10.1016/j.urology.2015.02.064
15. Mungovan, SF, Carlsson, SV, Gass, GC, Graham, PL, Sandhu, JS, Akin, O, et al. Preoperative exercise interventions to optimize continence outcomes following radical prostatectomy. Nat Rev Urol. (2021) 18:259–81. doi: 10.1038/s41585-021-00445-5
16. Gacci, M, Sakalis, VI, Karavitakis, M, Cornu, JN, Gratzke, C, Herrmann, TRW, et al. European association of urology guidelines on male urinary incontinence. Eur Urol. (2022) 82:387–98. doi: 10.1016/j.eururo.2022.05.012
17. Sandhu, JS, Breyer, B, Comiter, C, Eastham, JA, Gomez, C, Kirages, DJ, et al. Incontinence after prostate treatment: AUA/SUFU guideline. J Urol. (2019) 202:369–78. doi: 10.1097/JU.0000000000000314
18. Colquhoun, HL, Levac, D, O'Brien, KK, Straus, S, Tricco, AC, Perrier, L, et al. Scoping reviews: time for clarity in definition, methods, and reporting. J Clin Epidemiol. (2014) 67:1291–4. doi: 10.1016/j.jclinepi.2014.03.013
19. Tricco, AC, Lillie, E, Zarin, W, O'Brien, KK, Colquhoun, H, Levac, D, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. (2018) 169:467–73. doi: 10.7326/M18-0850
20. Flottorp, SA, Oxman, AD, Krause, J, Musila, NR, Wensing, M, Godycki-Cwirko, M, et al. A checklist for identifying determinants of practice: a systematic review and synthesis of frameworks and taxonomies of factors that prevent or enable improvements in healthcare professional practice. Implement Sci. (2013) 8:35. doi: 10.1186/1748-5908-8-35
21. Floratos, DL, Sonke, GS, Rapidou, CA, Alivizatos, GJ, Deliveliotis, C, Constantinides, CA, et al. Biofeedback vs verbal feedback as learning tools for pelvic muscle exercises in the early management of urinary incontinence after radical prostatectomy. BJU Int. (2002) 89:714–9. doi: 10.1046/j.1464-410X.2002.02721.x
22. Manassero, F, Traversi, C, Ales, V, Pistolesi, D, Panicucci, E, Valent, F, et al. Contribution of early intensive prolonged pelvic floor exercises on urinary continence recovery after bladder neck-sparing radical prostatectomy: results of a prospective controlled randomized trial. Neurourol Urodyn. (2007) 26:985–9. doi: 10.1002/nau.20442
23. Cornel, EB, de Wit, R, and Witjes, JA. Evaluation of early pelvic floor physiotherapy on the duration and degree of urinary incontinence after radical retropubic prostatectomy in a non-teaching hospital. World J Urol. (2005) 23:353–5. doi: 10.1007/s00345-005-0003-9
24. Moore, KN, Valiquette, L, Chetner, MP, Byrniak, S, and Herbison, GP. Return to continence after radical retropubic prostatectomy: a randomized trial of verbal and written instructions versus therapist-directed pelvic floor muscle therapy. Urology. (2008) 72:1280–6. doi: 10.1016/j.urology.2007.12.034
25. Yamanishi, T, Mizuno, T, Watanabe, M, Honda, M, and Yoshida, K. Randomized, placebo controlled study of electrical stimulation with pelvic floor muscle training for severe urinary incontinence after radical prostatectomy. J Urol. (2010) 184:2007–12. doi: 10.1016/j.juro.2010.06.103
26. Prota, C, Gomes, CM, Ribeiro, LH, de Bessa, J Jr, Nakano, E, Dall'Oglio, M, et al. Early postoperative pelvic-floor biofeedback improves erectile function in men undergoing radical prostatectomy: a prospective, randomized, controlled trial. Int J Impot Res. (2012) 24:174–8. doi: 10.1038/ijir.2012.11
27. Marchiori, D, Bertaccini, A, Manferrari, F, Ferri, C, and Martorana, G. Pelvic floor rehabilitation for continence recovery after radical prostatectomy: role of a personal training re-educational program. Anticancer Res. (2010) 30:553–6.
28. Ahmed, MT, Mohammed, AH, and Amansour, A. Effect of pelvic floor electrical stimulation and biofeedback on the recovery of urinary continence after radical prostatectomy. Turk J Phys Med Rehab. (2012) 58:170–6. doi: 10.4274/tftr.66588
29. Hirschhorn, AD, Kolt, GS, and Brooks, AJ. A multicomponent theory-based intervention improves uptake of pelvic floor muscle training before radical prostatectomy: a 'before and after' cohort study. BJU Int. (2014) 113:383–92. doi: 10.1111/bju.12385
30. Goode, PS, Burgio, KL, Johnson TM 2nd,, Clay, OJ, Roth, DL, Markland, AD, et al. Behavioral therapy with or without biofeedback and pelvic floor electrical stimulation for persistent postprostatectomy incontinence: a randomized controlled trial. JAMA. (2011) 305:151–9. doi: 10.1001/jama.2010.1972
31. Pannek, J, and König, JE. Clinical usefulness of pelvic floor reeducation for men undergoing radical prostatectomy. Urol Int. (2005) 74:38–43. doi: 10.1159/000082707
32. Zhang, AY, Bodner, DR, Fu, AZ, Gunzler, DD, Klein, E, Kresevic, D, et al. Effects of patient centered interventions on persistent urinary incontinence after prostate cancer treatment: a randomized, controlled trial. J Urol. (2015) 194:1675–81. doi: 10.1016/j.juro.2015.07.090
33. Geraerts, I, Van Poppel, H, Devoogdt, N, De Groef, A, Fieuws, S, and Van Kampen, M. Pelvic floor muscle training for erectile dysfunction and climacturia 1 year after nerve sparing radical prostatectomy: a randomized controlled trial. Int J Impot Res. (2016) 28:9–13. doi: 10.1038/ijir.2015.24
34. de Lira, GHS, Fornari, A, Cardoso, LF, Aranchipe, M, Kretiska, C, and Rhoden, EL. Effects of perioperative pelvic floor muscle training on early recovery of urinary continence and erectile function in men undergoing radical prostatectomy: a randomized clinical trial. Int Braz J Urol. (2019) 45:1196–203. doi: 10.1590/s1677-5538.ibju.2019.0238
35. Pan, LH, Lin, MH, Pang, ST, Wang, J, and Shih, WM. Improvement of urinary incontinence, life impact, and depression and anxiety with modified pelvic floor muscle training after radical prostatectomy. Am J Mens Health. (2019) 13:1557988319851618. doi: 10.1177/1557988319851618
36. Milios, JE, Ackland, TR, and Green, DJ. Pelvic floor muscle training in radical prostatectomy: a randomized controlled trial of the impacts on pelvic floor muscle function and urinary incontinence. BMC Urol. (2019) 19. Published 2019 Nov 15. doi: 10.1186/s12894-019-0546-5
37. Heydenreich, M, Puta, C, Gabriel, HH, Dietze, A, Wright, P, and Zermann, DH. Does trunk muscle training with an oscillating rod improve urinary incontinence after radical prostatectomy? A prospective randomized controlled trial. Clin Rehabil. (2020) 34:320–33. doi: 10.1177/0269215519893096
38. Serdà, BC, and Marcos-Gragera, R. Urinary incontinence and prostate cancer: a progressive rehabilitation program design. Rehabil Nurs. (2014) 39:271–80. doi: 10.1002/rnj.110
39. Patel, MI, Yao, J, Hirschhorn, AD, and Mungovan, SF. Preoperative pelvic floor physiotherapy improves continence after radical retropubic prostatectomy. Int J Urol. (2013) 20:986–92. doi: 10.1111/iju.12099
40. Karlsen, RV, Bidstrup, PE, Giraldi, A, Hvarness, H, Bagi, P, Lauridsen, SV, et al. Couple counseling and pelvic floor muscle training for men operated for prostate Cancer and for their female partners: results from the randomized ProCan trial. Sex Med. (2021) 9:100350. doi: 10.1016/j.esxm.2021.100350
41. Bales, GT, Gerber, GS, Minor, TX, Mhoon, DA, McFarland, JM, Kim, HL, et al. Effect of preoperative biofeedback/pelvic floor training on continence in men undergoing radical prostatectomy. Urology. (2000) 56:627–30. doi: 10.1016/S0090-4295(00)00687-7
42. Dijkstra-Eshuis, J, van den Bos, TWL, Splinter, R, Bevers, RFM, Zonneveld, WCG, Putter, H, et al. Effect of preoperative pelvic floor muscle therapy with biofeedback versus standard care on stress urinary incontinence and quality of life in men undergoing laparoscopic radical prostatectomy: a randomised control trial. Neurourol Urodyn. (2015) 34:144–50. doi: 10.1002/nau.22523
43. Laurienzo, CE, Magnabosco, WJ, Jabur, F, Faria, EF, Gameiro, MO, Sarri, AJ, et al. Pelvic floor muscle training and electrical stimulation as rehabilitation after radical prostatectomy: a randomized controlled trial. J Phys Ther Sci. (2018) 30:825–31. doi: 10.1589/jpts.30.825
44. Glazener, C, Boachie, C, Buckley, B, Cochran, C, Dorey, G, Grant, A, et al. Conservative treatment for urinary incontinence in Men after Prostate Surgery (MAPS): two parallel randomised controlled trials. Health Technol Assess. (2011) 15:1–iv. doi: 10.3310/hta15240
45. Laurienzo, CE, Sacomani, CA, Rodrigues, TR, Zequi Sde, C, Guimarães, GC, and Lopes, A. Results of preoperative electrical stimulation of pelvic floor muscles in the continence status following radical retropubic prostatectomy. Int Braz J Urol. (2013) 39:182–8. doi: 10.1590/S1677-5538.IBJU.2013.02.05
46. Nilssen, SR, Mørkved, S, Overgård, M, Lydersen, S, and Angelsen, A. Does physiotherapist-guided pelvic floor muscle training increase the quality of life in patients after radical prostatectomy? A randomized clinical study. Scand J Urol Nephrol. (2012) 46:397–404. doi: 10.3109/00365599.2012.694117
47. Tienforti, D, Sacco, E, Marangi, F, D'Addessi, A, Racioppi, M, Gulino, G, et al. Efficacy of an assisted low-intensity programme of perioperative pelvic floor muscle training in improving the recovery of continence after radical prostatectomy: a randomized controlled trial. BJU Int. (2012) 110:1004–10. doi: 10.1111/j.1464-410X.2012.10948.x
48. Overgård, M, Angelsen, A, Lydersen, S, and Mørkved, S. Does physiotherapist-guided pelvic floor muscle training reduce urinary incontinence after radical prostatectomy? A randomised controlled trial. Eur Urol. (2008) 54:438–48. doi: 10.1016/j.eururo.2008.04.021
49. Soto González, M, Da Cuña, CI, Gutiérrez Nieto, M, López García, S, Ojea Calvo, A, and Lantarón Caeiro, EM. Early 3-month treatment with comprehensive physical therapy program restores continence in urinary incontinence patients after radical prostatectomy: a randomized controlled trial. Neurourol Urodyn. (2020) 39:1529–37. doi: 10.1002/nau.24389
50. Tantawy, SA, Elgohary, HMI, Abdelbasset, WK, and Kamel, DM. Effect of 4 weeks of whole-body vibration training in treating stress urinary incontinence after prostate cancer surgery: a randomised controlled trial. Physiotherapy. (2019) 105:338–45. doi: 10.1016/j.physio.2018.07.013
51. Filocamo, M, Limarzi, V, Popolo, G, Cecconi, F, Marzocco, M, Tosto, A, et al. Effectiveness of early pelvic floor rehabilitation treatment for post-prostatectomy incontinence. Eur Urol. (2005) 48:734–8. doi: 10.1016/j.eururo.2005.06.004
52. Zhang, AY, Fu, AZ, Moore, S, Zhu, H, Strauss, G, Kresevic, D, et al. Is a behavioral treatment for urinary incontinence beneficial to prostate cancer survivors as a follow-up care? J Cancer Surviv. (2017) 11:24–31. doi: 10.1007/s11764-016-0557-0
53. Ribeiro, LH, Prota, C, Gomes, CM, de Bessa, J, Boldarine, MP, Dall'Oglio, MF, et al. Long-term effect of early postoperative pelvic floor biofeedback on continence in men undergoing radical prostatectomy: a prospective, randomized, controlled trial. J Urol. (2010) 184:1034–9. doi: 10.1016/j.juro.2010.05.040
54. Milios, JE, Ackland, TR, and Green, DJ. Pelvic floor muscle training and erectile dysfunction in radical prostatectomy: a randomized controlled trial investigating a non-invasive addition to penile rehabilitation. Sex Med. (2020) 8:414–21. doi: 10.1016/j.esxm.2020.03.005
55. Centemero, A, Rigatti, L, Giraudo, D, Lazzeri, M, Lughezzani, G, Zugna, D, et al. Preoperative pelvic floor muscle exercise for early continence after radical prostatectomy: a randomised controlled study. Eur Urol. (2010) 57:1039–44. doi: 10.1016/j.eururo.2010.02.028
56. Park, SW, Kim, TN, Nam, JK, Ha, HK, Shin, DG, Lee, W, et al. Recovery of overall exercise ability, quality of life, and continence after 12-week combined exercise intervention in elderly patients who underwent radical prostatectomy: a randomized controlled study. Urology. (2012) 80:299–306. doi: 10.1016/j.urology.2011.12.060
57. Mariotti, G, Salciccia, S, Innocenzi, M, Gentilucci, A, Fasulo, A, Gentile, V, et al. Recovery of urinary continence after radical prostatectomy using early vs late pelvic floor electrical stimulation and biofeedback-associated treatment. Urology. (2015) 86:115–21. doi: 10.1016/j.urology.2015.02.064
58. Aydın Sayılan, A, and Özbaş, A. The effect of pelvic floor muscle training on incontinence problems after radical prostatectomy. Am J Mens Health. (2018) 12:1007–15. doi: 10.1177/1557988318757242
59. Dubbelman, Y, Groen, J, Wildhagen, M, Rikken, B, and Bosch, R. The recovery of urinary continence after radical retropubic prostatectomy: a randomized trial comparing the effect of physiotherapist-guided pelvic floor muscle exercises with guidance by an instruction folder only. BJU Int. (2010) 106:515–22. doi: 10.1111/j.1464-410X.2010.09159.x
60. Van Kampen, M, De Weerdt, W, Van Poppel, H, De Ridder, D, Feys, H, and Baert, L. Effect of pelvic-floor re-education on duration and degree of incontinence after radical prostatectomy: a randomised controlled trial. Lancet. (2000) 355:98–102. doi: 10.1016/S0140-6736(99)03473-X
61. Zhang, AY, Strauss, GJ, and Siminoff, LA. Effects of combined pelvic floor muscle exercise and a support group on urinary incontinence and quality of life of postprostatectomy patients. Oncol Nurs Forum. (2007) 34:47–53. doi: 10.1188/07.ONF.47-53
62. Burgio, KL, Goode, PS, Urban, DA, Umlauf, MG, Locher, JL, Bueschen, A, et al. Preoperative biofeedback assisted behavioral training to decrease post-prostatectomy incontinence: a randomized, controlled trial. J Urol. (2006) 175:196–201. doi: 10.1016/S0022-5347(05)00047-9
63. Park, SW, Kim, TN, Nam, JK, Ha, HK, Shin, DG, Lee, W, et al. Recovery of overall exercise ability, quality of life, and continence after 12-week combined exercise intervention in elderly patients who underwent radical prostatectomy: a randomized controlled study. Urology. (2012) 80:299–306. doi: 10.1016/j.urology.2011.12.060
64. Moore, KN, Griffiths, D, and Hughton, A. Urinary incontinence after radical prostatectomy: a randomized controlled trial comparing pelvic muscle exercises with or without electrical stimulation. BJU Int. (1999) 83:57–65. doi: 10.1046/j.1464-410x.1999.00894.x
65. Robinson, JP, Bradway, CW, Nuamah, I, Pickett, M, and McCorkle, R. Systematic pelvic floor training for lower urinary tract symptoms post-prostatectomy: a randomized clinical tria. Int J Urolo Nurs. (2008) 2:3–13. doi: 10.1111/j.1749-771X.2007.00033.x
66. Tibaek, S, Gard, G, Dehlendorff, C, Iversen, HK, Biering-Soerensen, F, and Jensen, R. Is pelvic floor muscle training effective for men with poststroke lower urinary tract symptoms? A single-blinded randomized, controlled trial. Am J Mens Health. (2017) 11:1460–71. doi: 10.1177/1557988315610816
67. Santa Mina, D, Hilton, WJ, Matthew, AG, Awasthi, R, Bousquet-Dion, G, Alibhai, SMH, et al. Prehabilitation for radical prostatectomy: a multicentre randomized controlled trial. Surg Oncol. (2018) 27:289–98. doi: 10.1016/j.suronc.2018.05.010
68. Parekh, AR, Feng, MI, Kirages, D, Bremner, H, Kaswick, J, and Aboseif, S. The role of pelvic floor exercises on post-prostatectomy incontinence. J Urol. (2003) 170:130–3. doi: 10.1097/01.ju.0000072900.82131.6f
69. Faithfull, S, Cockle-Hearne, J, Lemanska, A, Otter, S, and Skene, SS. Randomised controlled trial to investigate the effectiveness of the symptom management after radiotherapy (SMaRT) group intervention to ameliorate lower urinary tract symptoms in men treated for prostate cancer. Support Care Cancer. (2022) 30:3165–76. doi: 10.1007/s00520-021-06749-x
70. Strojek, K, Weber-Rajek, M, Strączyńska, A, Piekorz, Z, Pilarska, B, Jarzemski, P, et al. Randomized-controlled trial examining the effect of pelvic floor muscle training in the treatment of stress urinary incontinence in men after a laparoscopic radical prostatectomy pilot study. J Clin Med. (2021) 10:2946. doi: 10.3390/jcm10132946
71. Lin, YH, Yu, TJ, Lin, VC, Wang, HP, and Lu, K. Effects of early pelvic-floor muscle exercise for sexual dysfunction in radical prostatectomy recipients. Cancer Nurs. (2012) 35:106–14. doi: 10.1097/NCC.0b013e3182277425
72. Mathewson-Chapman, M. Pelvic muscle exercise/biofeedback for urinary incontinence after prostatectomy: an education program. J Cancer Educ. (1997) 12:218–23.
73. Levac, D, Colquhoun, H, and O'Brien, KK. Scoping studies: advancing the methodology. Implement Sci. (2010) 5:69. doi: 10.1186/1748-5908-5-69
74. Murphy, KM, Sauer, C, Yang, D, Hass, N, Novakovic, K, Helfand, B, et al. The development of iManage-PC, an online symptom monitoring and self-management tool for men with clinically localized prostate cancer. Cancer Nurs. (2022) 45:E309–19. doi: 10.1097/NCC.0000000000000948
75. Ones, LW, Courneya, KS, Fairey, AS, and Mackey, JR. Effects of an oncologist's recommendation to exercise on self-reported exercise behavior in newly diagnosed breast cancer survivors: a single-blind, randomized controlled trial. Ann. Behav. Med. (2004) 28:105–13. doi: 10.1207/s15324796abm2802_5
Keywords: prostate cancer, barriers, facilitators, pelvic floor muscle training, scoping review
Citation: Wang L, Li Y, Qi Z and Wang W (2023) Barriers and facilitators of the implementation of the application of pelvic floor muscle training in patients with prostate cancer: a scoping review. Front. Public Health. 11:1191508. doi: 10.3389/fpubh.2023.1191508
Edited by:
Walid Kamal, University of Sharjah, United Arab EmiratesReviewed by:
Binghao Bao, Beijing University of Chinese Medicine, ChinaSafaa Elkholi, Princess Nourah bint Abdulrahman University, Saudi Arabia
Copyright © 2023 Wang, Li, Qi and Wang. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Wei Wang, d2FuZ3cyMDA1QHpqdS5lZHUuY24=
 Lijuan Wang
Lijuan Wang Yaqin Li
Yaqin Li Ziyi Qi
Ziyi Qi Wei Wang
Wei Wang