- 1Department of Psychiatry, Chonnam National University Medical School, Gwangju, Republic of Korea
- 2Mindlink, Gwangju Bukgu Mental Health Center, Gwangju, Republic of Korea
Introduction: Suicide is a major concern for patients with recent-onset schizophrenia. We hypothesized that preserved cognitive function might be associated with a higher level of suicidality in patients with schizophrenia. We investigated the associations between cognitive function and suicidal ideation (SI) in young patients recently diagnosed with a psychotic disorder.
Methods: This study analyzed data from a naturalistic clinical cohort study that comprised 402 patients with schizophrenia spectrum disorder. Patients with a treatment duration of ≤5 years and an age range of 15–39 years were enrolled. Participants were categorized into two groups based on SI as assessed by the Columbia Suicidal Severity Rating Scale. We collected demographic and clinical data and administered psychiatric, neurocognitive, and social cognitive measures.
Results: Among participants, 52% reported experiencing SI. Patients with SI were significantly younger and had a longer duration of untreated psychosis (DUP) than those without it. The Positive and Negative Syndrome Scale-general psychopathology score was significantly higher in the SI group. Scores on the Calgary Depression Scale for Schizophrenia, Perceived Stress Scale, Beck Depression Inventory (BDI), and Beck Hopelessness Scale were significantly higher among patients with SI, while scores on the Subjective Well-being Under Neuroleptics-Short Form and Brief Resilience Scale were significantly lower compared to those without it. Patients with SI demonstrated significantly higher scores on the verbal and visual learning test, false belief task, picture stories task, and Controlled Oral Word Association Test. They also completed the Trail Making Test (TMT) parts A and B in significantly less time than those without it. After adjusting for age, DUP, and scores on the BDI, group differences in scores on the verbal and visual learning tests, TMT (parts A and B), and the false belief task, and the picture story task remained significant.
Discussion: Our results suggest that along with traditional risk factors, better cognitive function may also be a major risk factor for suicidality in patients with schizophrenia. Providing psychological support and cognitive interventions is essential for young patients with recent-onset schizophrenia spectrum disorders, particularly those with high levels of depression, hopelessness, perceived stress, low resilience, and good cognitive function.
Introduction
Suicide ranks as the fifth leading cause of death in South Korea (1) and imposes a significant socioeconomic burden (2). In individuals with schizophrenia, suicide is a tragic outcome, accounting for early mortality in nearly 5% of patients, with 25–50% attempting suicide during their lifetime (3, 4). Despite the gravity of this issue, the relatively low incidence of completed suicide in this population makes comprehensive investigation challenging (5). Suicidal behaviors, encompassing both suicide attempts and suicidal ideation (SI), are prevalent among individuals with schizophrenia and are recognized as substantial risk factors for suicide (6, 7). Hence, the identification of factors associated with suicidal behavior in patients with schizophrenia plays a crucial role in suicide prevention efforts. Previous research has revealed that factors such as previous suicide attempts, the choice of more lethal methods, feelings of hopelessness, and the presence of depressive symptoms significantly contribute to suicide risk in individuals with schizophrenia, and these results are similar to those found in the general population (8–14).
Cognitive function is one of the domains predominantly affected in patients with schizophrenia spectrum disorder (14). Cognitive functions, such as attention, executive function, working memory, and episodic memory, are impaired in patients with schizophrenia (15). Previous studies have reported that preserved cognitive function in schizophrenia is a risk factor for suicidality (16, 17). However, these studies were conducted in patients with chronic schizophrenia. Young patients with schizophrenia face a significantly higher risk of suicidality (18–23). Additionally, the highest risk of suicide occurs within the first 5 years after diagnosis (4, 24). Therefore, it is crucial to identify the risk factors for suicidality in young patients with recently diagnosed schizophrenia.
In young patients with psychotic disorders, suicidal thoughts are strongly linked to actual suicidal behavior and even death by suicide (20–22). When patients experience SI, they may be at an elevated risk of taking further steps toward suicide. Furthermore, SI is a crucial element in the overall understanding of how individuals progress from having thoughts of suicide to engaging in suicidal behaviors. Thus, for effective suicide prevention in patients with early psychosis, it is necessary to investigate the pathogenesis of SI.
We hypothesized that preserved cognitive function might be associated with a higher level of suicidality in patients recently diagnosed with schizophrenia. Most previous studies examining the relationship between neurocognitive function and suicidality were conducted in patients with chronic schizophrenia and did not incorporate measures assessing social cognition and theory of mind. Therefore, in this study, we investigated the associations between cognitive function, including social cognition, and SI in young patients recently diagnosed with a schizophrenia spectrum disorder.
Materials and methods
Study design
We analyzed the data from a naturalistic clinical cohort study conducted at the Gwangju Early Treatment and Intervention Team of Chonnam National University Hospital (25). All participants were consecutively recruited from patients who recently developed psychotic symptoms and visited Chonnam National University Hospital. In this study, inclusion criteria were a treatment duration of ≤5 years and an age range of 15–39 years. Furthermore, a qualified research psychiatrist established the clinical diagnosis for each participant, ensuring that all patients met the criteria for ‘Schizophrenia Spectrum Disorder and Other Psychotic Disorders’ in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (26). Patients with a substance-or medication-induced psychotic disorder, psychotic disorder due to another medical condition, or severe neurological or medical disorder were excluded. The study was conducted from September 2015 to December 2022, during which a total of 402 participants met the inclusion criteria. This study was approved by the Chonnam National University Hospital Institutional Review Board, and all subjects provided written informed consent before participating.
Demographic and clinical measures
Baseline sociodemographic and clinical data were collected, including age, sex, education level, occupation, body mass index (BMI), duration of treatment, diagnosis, and duration of untreated psychosis (DUP; time between the appearance of the initial psychotic symptoms and the start of antipsychotic treatment or psychiatric hospitalization) (27). The doses of prescribed antipsychotics were converted into chlorpromazine (CPZ)-equivalent dose (28).
Suicidal behavior was assessed using a semi-structured interview with the Columbia Suicidal Severity Rating Scale (C-SSRS) administered by a trained researcher (29, 30). At the baseline assessment, the C-SSRS was used to evaluate lifetime suicidal behavior. Patients who responded affirmatively to any item indicative of suicidal ideation (SI) were categorized into the SI group. Psychiatric symptoms were evaluated using the Positive and Negative Syndrome Scale (PANSS) (31, 32). We utilized three subscales (positive, negative, and general psychopathology) as well as total scores as variables. For exploratory analysis, we also examined the 12th item of the general psychopathology subscale (lack of insight and judgment; G12). Other objective psychiatric measures included Social and Occupational Functioning Assessment Scale (SOFAS; used to evaluate general functioning) (33) and Calgary Depression Scale for Schizophrenia (CDSS; used to analyze depressive symptoms) (34, 35).
We employed several subjective self-report measures, including the Beck Depression Inventory (BDI; used to assess depressive symptoms) (36, 37), Beck Hopelessness Scale (BHS; used to evaluate hopelessness) (38, 39), Perceived Stress Scale (PSS; used to assess subjective stress) (40, 41), Brief Resilience Scale (BRS; used to quantify the ability to recover from stress) (42), and Subjective Well-being Under Neuroleptics-Short Form (SWN-K; used to evaluate subjective health-related quality of life) (43). Higher scores on the BRS and SWN-K, and lower scores on the BHS, BDI, and PSS, indicate better outcomes.
Neurocognitive measures
We assessed neurocognitive function using a computerized neurocognitive test battery standardized for the Korean population, including individuals with psychotic disorders. Research nurses, who were unaware of the study’s objectives, administered six neurocognitive tests. The Digit Span test was used to assess attention span; higher scores indicate superior attention and vigilance (44–46). The modified Rey Auditory Verbal Learning Test was used to assess immediate and delayed verbal memory; the outcome measure is the total number of recalls (46, 47). The visual learning test was administered to assess immediate and delayed visual memory. The outcome measure was the total number of recalls, and a higher score indicated better memory (48). The Wisconsin Card Sorting Test was administered to assess executive function; the outcome measure is the number of categories completed, and a higher score indicates better executive function and cognitive flexibility (49–51). The Continuous Performance Test (CPT) was administered to measure the ability to sustain attention (vigilance) to a stimulus; the outcome measures are reaction time and number of correct responses, where faster reaction times and more correct responses indicate superior attention (52–54). Finally, the Trail Making Test (TMT) was used to assess visuomotor coordination. The TMT consists of two parts that measure executive function and visuospatial working memory (A and B, respectively), and the outcome measure is the time taken (in seconds) to complete both parts (54–56). In addition, we used the Mini-Mental Status Examination (MMSE) to assess global cognitive function (57–59) and the Controlled Oral Word Association Test (COWAT) to evaluate verbal fluency and cognitive speed (60, 61).
Social cognitive measures
The false belief task of Wimmer and Perner was administered to assess social cognition (62, 63). Patients are required to infer the thoughts of characters in four stories. The maximum total score is 12 points, and higher scores indicate the superior theory of mind (ToM) and social cognition. Picture stories task developed by Brüne were used to assess ToM, which is the ability to infer others’ mental states and emotions (64, 65). Six cartoons are presented to the patient without a background story description, and the patient is then required to answer questions related to ordering and mind-reading. This task represents a more complex and higher-order ToM test. Total ordering (36 points) and mind-reading (23 points) scores are calculated; higher scores indicate superior ToM (65).
Statistical analysis
The dependent variable in this study was lifetime suicidal ideation, assessed using the C-SSRS. Participants were divided into two groups based on the presence of SI. Sociodemographic and clinical characteristics, as well as cognitive function, were compared between these two groups. We used the chi-square test for categorical variables, the independent t-test for normally distributed variables, and the Mann–Whitney U test for variables that did not follow a normal distribution, as appropriate. To control for the potential confounding effects of age, DUP, and BDI scores, which showed significant associations with SI in the univariate analyses, we included them as covariates in logistic regression analysis along with each cognitive measure that demonstrated a significant association with SI in the univariate analyses. DUP and BDI scores, which were not normally distributed, were log-transformed before entering them into the model. TMT part A and B times, also not normally distributed, were transformed into 10-point scales based on ten percentiles before inclusion in the logistic regression analysis. For exploratory analysis, we calculated Pearson’s or Spearman’s correlation coefficients between the PANSS G12 score and measures of clinical status and ToM. All statistical tests were two-tailed, and p < 0.05 was taken to indicate statistical significance. The statistical analysis was performed using SPSS software (version 25.0; IBM Corp., Armonk, NY, United States).
Results
In total, 402 patients (males, 49.2%; females, 50.2%) with recent-onset psychosis were included in the analysis. The mean (standard deviation) age at baseline was 24.4 (5.7) years. The most common diagnosis was schizophrenia (n = 244, 65.9%), followed by schizophreniform disorder (n = 78, 21.1%), other specified schizophrenia spectrum disorder (n = 34, 9.2%), and schizoaffective disorder (n = 14, 3.8%). Approximately half of the patients (52.0%) reported experiencing SI.
Table 1 shows the participants’ sociodemographic and clinical characteristics according to the presence of SI. Patients with SI were significantly younger and had longer DUP than those without it. There was no significant group difference in sex, marital status, education level, occupation, BMI, duration of treatment, diagnosis, or CPZ equivalent dose.
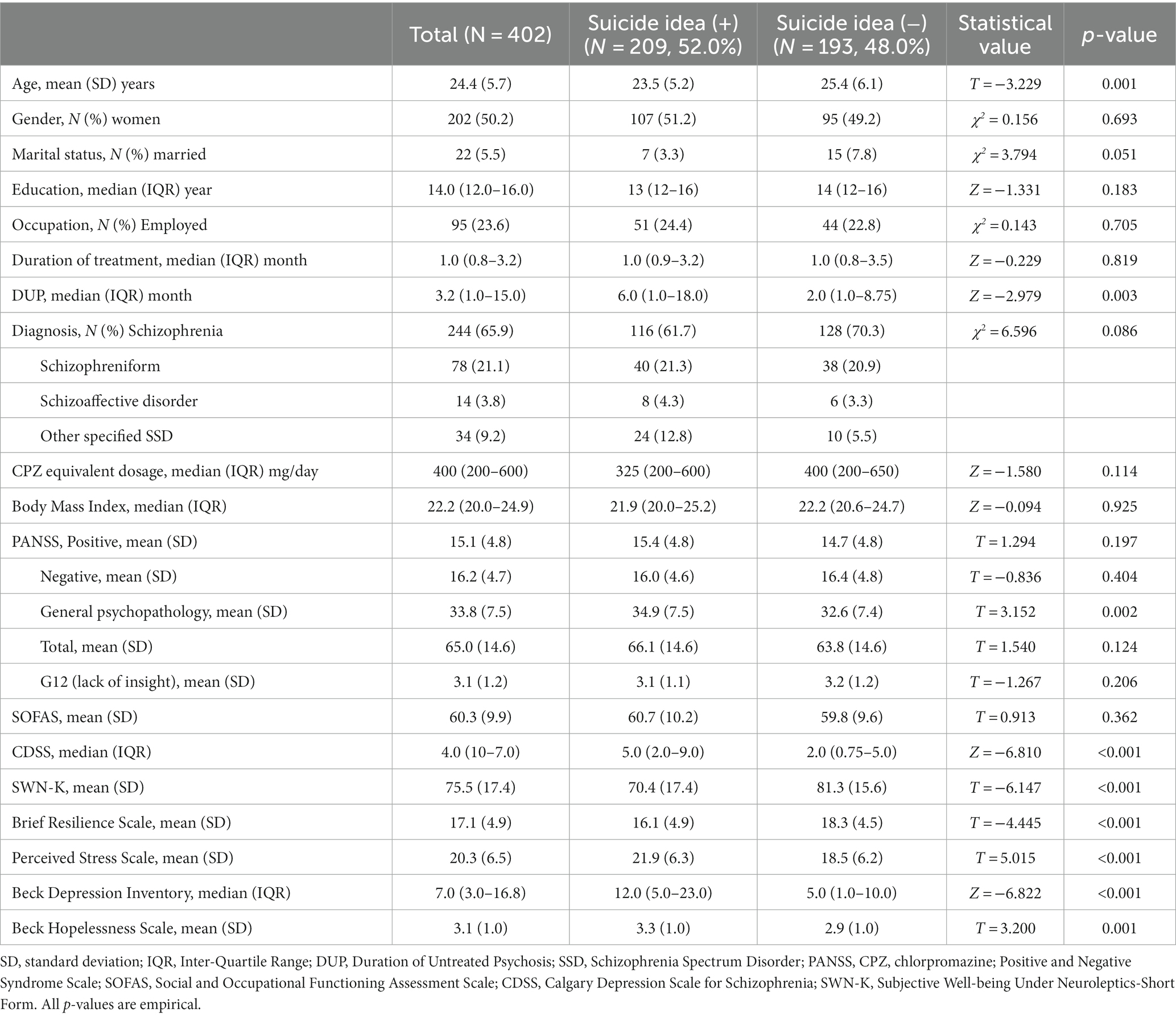
Table 1. Comparison of the sociodemographic and clinical characteristics of participants according to the presence of suicide idea.
The PANSS positive, negative, G12, and total scores did not differ according to SI, but the general psychopathology score was significantly higher in the SI group. Scores on the CDSS, PSS, BDI, and BHS were significantly higher in patients with SI compared to those without it, whereas scores on the SWN-K and BRS were significantly lower. There were no significant associations found between G12 and other clinical measures (data not shown). However, the PANSS G12 score was significantly correlated with scores on the picture stories task and the false belief task (r = −0.130, p = 0.009, and r = −0.117, p = 0.019, respectively).
Table 2 shows the neurocognitive and social-cognitive outcomes according to the presence of SI. The patients with SI had significantly higher scores on the verbal and visual learning test, false belief task, picture stories task, and COWATT, and took significantly less time to complete TMT parts A and B, than those without it. They also completed more categories, although the difference was not statistically significant (p = 0.084). The two groups had no significant differences in scores on the digit span test, CPT, or MMSE.
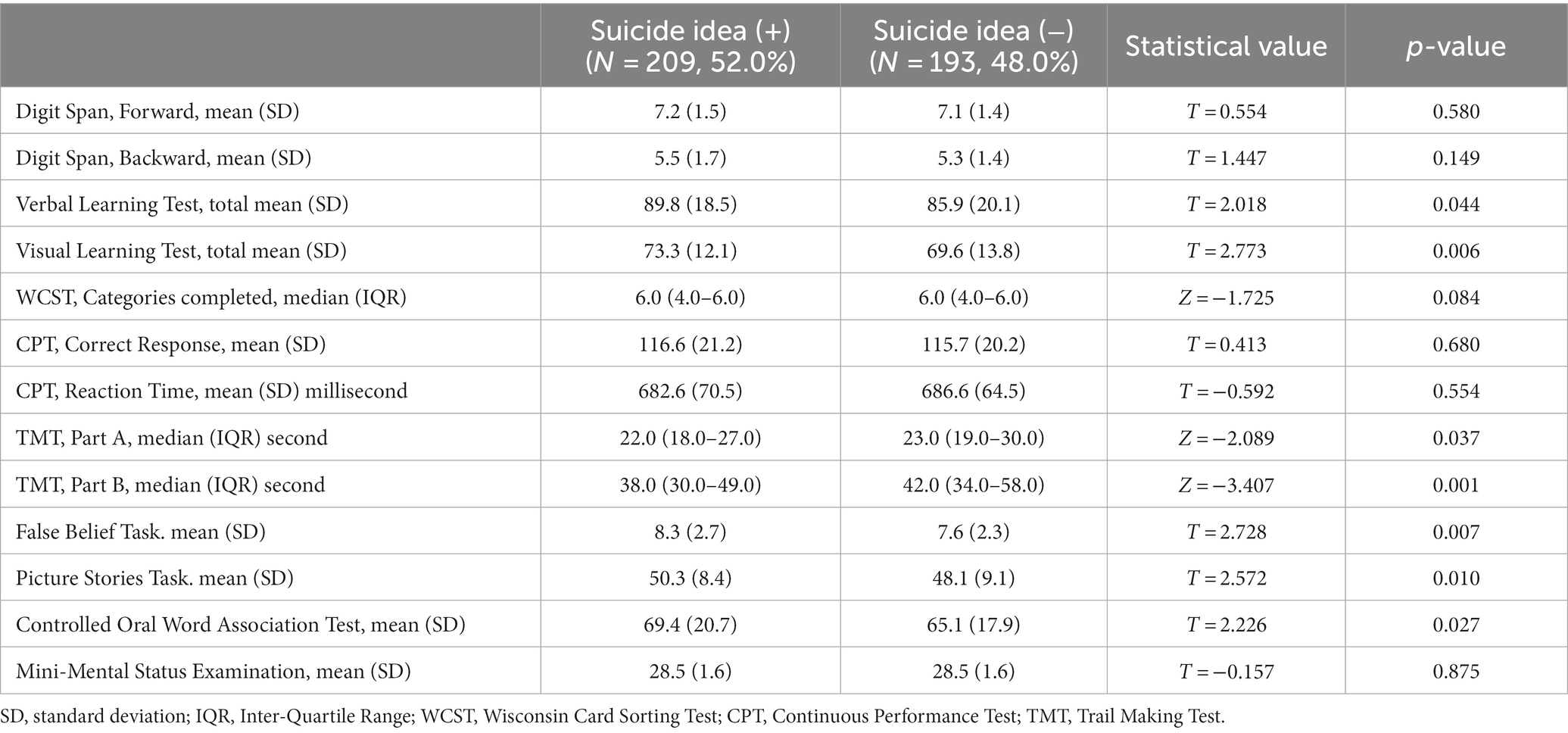
Table 2. Comparison of neurocognitive and social cognitive outcomes of participants according to the presence of suicide idea.
Table 3 shows the results of adjusted logistic regression analyses. After controlling for age, DUP, and scores on the BDI, significant differences between groups remained evident in scores on the verbal and visual learning tests, TMT (parts A and B), the false belief task, and the picture story task. However, the group differences in COWATT scores lost statistical significance after adjusting for the confounding variables.
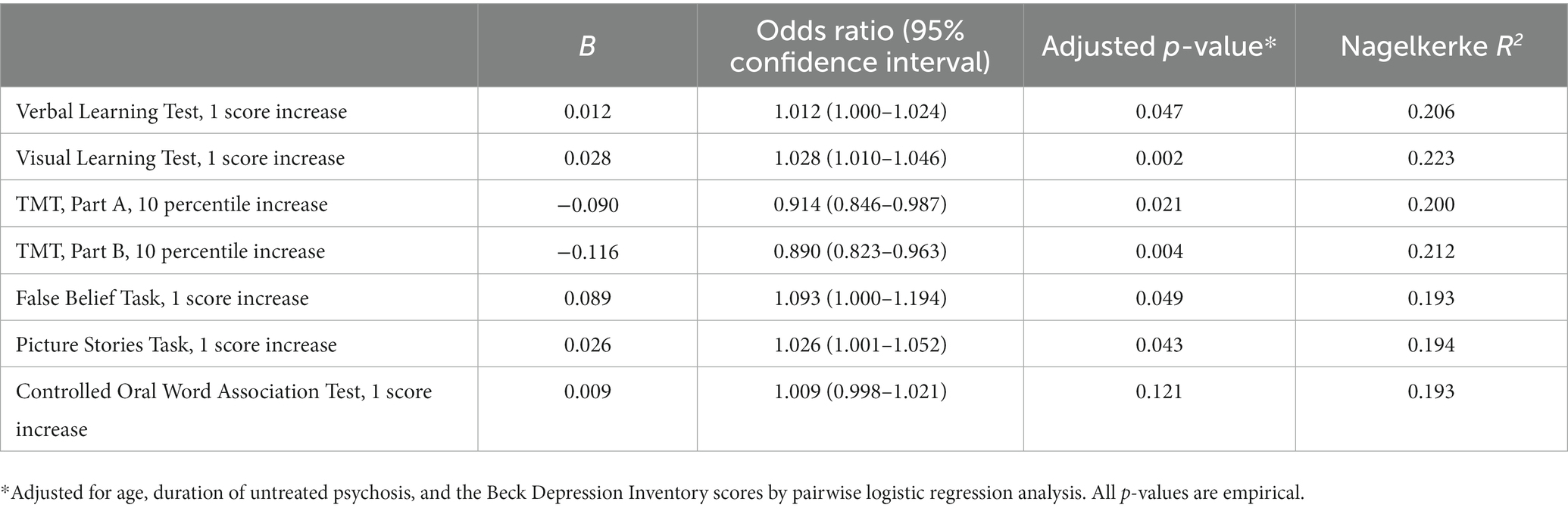
Table 3. Adjusted analysis for associations between neurocognitive and social cognitive outcomes and suicidal ideation.
Discussion
This study investigated the risk factors for SI in young patients with recent-onset schizophrenia and examined their association with cognitive function. Patients with SI had superior neurocognitive and social-cognitive function than those without it. In addition, they showed higher levels of depression, perceived stress, and hopelessness and lower levels of resilience and subjective well-being. These results suggest that, along with traditional risk factors such as depression, perceived stress, and hopelessness (8, 9), better cognitive function may also be a major risk factor for suicidality. A better understanding of SI may help prevent suicidal behavior in patients with recent-onset schizophrenia.
The SI group in this study was significantly younger than the group without SI. This finding aligns with the nationwide Danish OPUS trial, which investigated the effectiveness of early intervention programs for schizophrenia spectrum disorders and demonstrated that younger age was a risk factor for suicidality (21). Notably, there is a trend toward a higher risk of suicide at a younger age in patients with schizophrenia compared to the general population, where the risk for suicide tends to be higher among older individuals (23). Individuals diagnosed with schizophrenia often undergo a mourning process as they grapple with the losses experienced upon the onset of their illness (66). The risk of suicide may increase when young individuals with schizophrenia experience demoralization stemming from their pessimistic outlook on a future characterized by long-term treatment demands. Additionally, individuals experiencing their first episode of schizophrenia in life often find themselves in a more unstable situation, as they are unfamiliar with the disorder and, as adolescents, face the typical problems and conflicts that come with beginning a new phase in life (18). Therefore, it is crucial to assess the risk of suicidality when treating young patients with early psychosis, particularly those in their late teens and early twenties.
Longer DUP, a prognostic factor associated with poorer overall outcomes in patients with schizophrenia (67, 68), was observed in the group with SI in this study. SI may occur as a result of protracted psychotic symptoms when the DUP is extended (22). Several studies have demonstrated that a long DUP is a risk factor for suicidality (69, 70), and this association may be mediated by depressive symptoms (71, 72). Furthermore, patients with an extended DUP might experience great distress due to psychotic symptoms, which, in turn, could increase the risk of SI.
As in previous studies of patients with schizophrenia and the general population, the individuals in this study who had experienced SI showed significantly higher levels of depression and hopelessness (11, 73–76). A higher general psychopathology PANSS score in patients with SI might be associated with depressive symptoms. Depression is common in patients with schizophrenia (77), and it should be managed to prevent suicide (78). Hopelessness is a major psychological risk factor and a clinical endophenotype for suicidality in the general population. Hopelessness plays a role in the development of suicidal thoughts and behaviors, and it also mediates the relationship between SI and suicidality (75). Demoralization, which is associated with hopelessness (79), is important in the context of the current study, which explored the link between cognitive function and SI. People who experience hopelessness tend to isolate themselves and not seek help (75). Life stressors can reduce the will to live, and it is intuitive that hopelessness plays an important role in the suicidality of patients with schizophrenia (79).
In recent studies, perceived stress was found to be significantly associated with suicidality in patients with schizophrenia spectrum disorder (80, 81), and resilience is a major protective factor for suicidality. In one study, early psychosis patients with comorbid depression showed lower resilience. Resilience in patients with schizophrenia spectrum disorders was associated with symptom remission, recovery, better social and interpersonal functioning, and higher quality of life, all of which may have reduced SI (82).
In this study, the group with SI demonstrated better performance on several neurocognitive and social-cognitive tasks. Higher levels of verbal and visual learning ability, visuospatial working memory, and ToM were observed in individuals with high suicidality, while attention span, sustained attention, and verbal fluency showed no significant differences between groups. These findings suggest that complex cognitive processes, such as working memory and social cognition, are more strongly associated with suicidality than simple attention.
ToM refers to the ability to understand and represent another person’s mental state and use these representations to explain and predict human interactions (83). It is associated with cognitive flexibility (84, 85), which generally exhibits an inverse association with suicidality (86). However, in this study, the SI group displayed superior ToM even after adjusting for confounding variables. It is possible that patients with high mental reasoning abilities were more aware of the difficulties that can arise during interpersonal and social situations, which could lead to psychological strain (12, 66). This aligns with the significant increase in suicide attempts observed among patients shortly after discharge, when real-world life challenges may escalate (87). Clinical insight, which refers to an individual’s awareness of having a mental illness that requires treatment, can be associated with ToM (88). In this study, ToM was significantly linked to higher levels of insight and judgment, even though there was not difference based on the presence of SI.
Higher levels of insight in patients with schizophrenia can also be connected to increased severity of depression and hopelessness (16, 89). While this study did not demonstrate these associations, it can be inferred that SI may manifest in patients who recognize their own condition, especially those who struggle to maintain social relationships. Providing care for individuals with schizophrenia who are aware of their condition is essential to help them adapt to society, mitigate depressive responses, and reduce the risk of suicide (78). Cognitive therapy and psychological support for patients with early psychosis, particularly those with good cognitive function, are essential to prevent suicidality.
No significant differences in indicators of disease severity, such as the PANSS positive symptoms score, medication dosage, and social functioning, were observed between the groups in this study with and without SI. In previous studies, severe psychotic symptoms such as command hallucinations were associated with suicidality in patients with schizophrenia (23, 90). Relatively low scores on the PANSS among our patients in the early stages of schizophrenia might explain this discrepancy.
This study had some limitations. First, it used a cross-sectional design such that causal relationships could not be established. Therefore, longitudinal studies are needed. Second, a control group of healthy individuals was not included; doing so may have helped us achieve a deeper understanding of the impact of social cognition on suicidality in patients with schizophrenia through comparison with the general population. Third, the generalizability of the results to chronic schizophrenia patients with more severe cognitive impairment may be limited. Fourth, in this study, we used lifetime SI as a key variable for assessing suicidality. Future research should consider incorporating the severity of suicidal behavior. Finally, the potential type I errors should be considered because this study employed empirical value of p-values without correction for multiple testing. Nevertheless, our results serve as a basis for future investigations into the relationship between suicidality and cognitive function in young patients with psychosis. We believe that our study contributes to a deeper understanding of suicidal behavior in young patients going through their first episode of schizophrenia and can aid in the development of suicide prevention strategies for this population.
In conclusion, our findings suggest that patients with recent-onset psychosis, who exhibit relatively high cognitive abilities, especially in complex functions and social cognition, are more prone to experiencing suicidal thoughts, potentially leading to increased suicidality. It is crucial to pay greater attention to suicidality among younger patients who demonstrate a better ability to understand others’ perspectives and adapt to social situations. Moreover, providing psychological support with empathy and cognitive interventions is essential for young patients with recent-onset schizophrenia spectrum disorders, particularly those with elevated levels of depression, hopelessness, perceived stress, low resilience, and good cognitive function.
Data availability statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
Ethics statement
The studies involving humans were approved by Chonnam National University Hospital Institutional Review Board. The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
Author contributions
JSK: Writing – original draft, Data curation, Investigation. SHB: Data curation, Investigation, Methodology, Writing – review & editing. HK: Data curation, Investigation, Writing – review & editing. JWK: Data curation, Investigation, Writing – review & editing. HJK: Writing – review & editing, Conceptualization, Supervision. SR: Supervision, Writing – review & editing, Data curation, Formal analysis. JYL: Supervision, Writing – review & editing. JMK: Supervision, Writing – review & editing. SWK: Writing – review & editing, Conceptualization, Formal analysis, Funding acquisition, Methodology, Writing – original draft.
Funding
The author(s) declare financial support was received for the research, authorship, and/or publication of this article. This research was supported by a grant of the Patient-Centered Clinical Research Coordinating Center (PACEN) (grant numbers: HI19C0481 and HC19C0316) and a grant of the Korean Mental Health Technology R&D Project (HM15C1140) funded by the Ministry of Health & Welfare, Republic of Korea.
Acknowledgments
We thank Anna Jo, Mi-Young Lee, Yoon-A Choi, Da-Hye Jeon, and Chaewon Park for their assistance in subject recruitment and data collection.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher’s note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
References
1. Korea National Statistical Office. Annual report on the cause of death statistics 2021. (2022). Available at: https://kostat.go.kr/boardDownload.es?bid=218&list_no=420715&seq=6 (Accessed August 5, 2023).
2. Hyun, GR, Choi, GC, Lee, SM, and Lee, SY. National Health Insurance Service of Korea, analysis of socioeconomic costs of major diseases for health security policy establishment. Wonju: National Health Insurance Service of Korea (2017).
3. Nordentoft, M, Laursen, TM, Agerbo, E, Qin, P, Høyer, EH, and Mortensen, PB. Change in suicide rates for patients with schizophrenia in Denmark, 1981-97: nested case-control study. BMJ. (2004) 329:261. doi: 10.1136/bmj.38133.622488.63
4. Berardelli, I, Rogante, E, Sarubbi, S, Erbuto, D, Lester, D, and Pompili, M. The importance of suicide risk formulation in schizophrenia. Front Psych. (2021) 12:779684. doi: 10.3389/fpsyt.2021.779684
5. Palmer, BA, Pankratz, VS, and Bostwick, JM. The lifetime risk of suicide in schizophrenia: a reexamination. Arch Gen Psychiatry. (2005) 62:247–53. doi: 10.1001/archpsyc.62.3.247
6. Hocaoglu, C, and Babuc, ZT. Suicidal ideation in patients with schizophrenia. Isr J Psychiatry Relat Sci. (2009) 46:195–203.
7. Carlborg, A, Winnerbäck, K, Jönsson, EG, Jokinen, J, and Nordström, P. Suicide in schizophrenia. Expert Rev Neurother. (2010) 10:1153–64. doi: 10.1586/ern.10.82
8. Cassidy, RM, Yang, F, Kapczinski, F, and Passos, IC. Risk factors for suicidality in patients with schizophrenia: a systematic review, Meta-analysis, and Meta-regression of 96 studies. Schizophr Bull. (2018) 44:787–97. doi: 10.1093/schbul/sbx131
9. Sher, L, and Kahn, RS. Suicide in schizophrenia: An educational overview. Medicina (Kaunas). (2019) 55:361. doi: 10.3390/medicina55070361
10. Siris, SG. Suicide and schizophrenia. J Psychopharmacol. (2001) 15:127–35. doi: 10.1177/026988110101500209
11. Kim, SW, Kim, SJ, Mun, JW, Bae, KY, Kim, JM, Kim, SY, et al. Psychosocial factors contributing to suicidal ideation in hospitalized schizophrenia patients in Korea. Psychiatry Investig. (2010) 7:79–85. doi: 10.4306/pi.2010.7.2.79
12. Oexle, N, Waldmann, T, Staiger, T, Xu, Z, and Rüsch, N. Mental illness stigma and suicidality: the role of public and individual stigma. Epidemiol Psychiatr Sci. (2018) 27:169–75. doi: 10.1017/S2045796016000949
13. Yoo, T, Kim, SW, Kim, SY, Lee, JY, Kang, HJ, Bae, KY, et al. Relationship between suicidality and low self-esteem in patients with schizophrenia. Clin Psychopharmacol Neurosci. (2015) 13:296–301. doi: 10.9758/cpn.2015.13.3.296
14. Baek, SH, Kim, H, Kim, JW, Ryu, S, Lee, JY, Kim, JM, et al. Association between peripheral inflammatory cytokines and cognitive function in patients with first-episode schizophrenia. J Pers Med. (2022) 12:1137. doi: 10.3390/jpm12071137
15. Bowie, CR, and Harvey, PD. Cognitive deficits and functional outcome in schizophrenia. Neuropsychiatr Dis Treat. (2006) 2:531–6. doi: 10.2147/nedt.2006.2.4.531
16. Villa, J, Choi, J, Kangas, JL, Kaufmann, CN, Harvey, PD, and Depp, CA. Associations of suicidality with cognitive ability and cognitive insight in outpatients with schizophrenia. Schizophr Res. (2018) 192:340–4. doi: 10.1016/j.schres.2017.06.013
17. Delaney, C, McGrane, J, Cummings, E, Morris, DW, Tropea, D, Gill, M, et al. Preserved cognitive function is associated with suicidal ideation and single suicide attempts in schizophrenia. Schizophr Res. (2012) 140:232–6. doi: 10.1016/j.schres.2012.06.017
18. Pompili, M, Amador, XF, Girardi, P, Harkavy-Friedman, J, Harrow, M, Kaplan, K, et al. Suicide risk in schizophrenia: learning from the past to change the future. Ann General Psychiatry. (2007) 6:10. doi: 10.1186/1744-859X-6-10
19. Clapham, E, Bodén, R, Brandt, L, Jönsson, EG, Bahmanyar, S, Ekbom, A, et al. Suicide ideation and behavior as risk factors for subsequent suicide in schizophrenia: a nested case-control study. Suicide Life Threat Behav. (2019) 49:996–1005. doi: 10.1111/sltb.12499
20. Chapman, CL, Mullin, K, Ryan, CJ, Kuffel, A, Nielssen, O, and Large, MM. Meta-analysis of the association between suicidal ideation and later suicide among patients with either a schizophrenia spectrum psychosis or a mood disorder. Acta Psychiatr Scand. (2015) 131:162–73. doi: 10.1111/acps.12359
21. Bertelsen, M, Jeppesen, P, Petersen, L, Thorup, A, ⊘hlenschlæger, J, le Quach, P, et al. Suicidal behaviour and mortality in first-episode psychosis: the OPUS trial. Br J Psychiatry Suppl. (2007) 191:s140–6. doi: 10.1192/bjp.191.51.s140
22. Barrett, EA, Sundet, K, Faerden, A, Nesvåg, R, Agartz, I, Fosse, R, et al. Suicidality before and in the early phases of first episode psychosis. Schizophr Res. (2010) 119:11–7. doi: 10.1016/j.schres.2010.03.022
23. Ventriglio, A, Gentile, A, Bonfitto, I, Stella, E, Mari, M, Steardo, L, et al. Suicide in the early stage of schizophrenia. Front Psych. (2016) 7:116. doi: 10.3389/fpsyt.2016.00116
24. Fleischhacker, WW, Kane, JM, Geier, J, Karayal, O, Kolluri, S, Eng, SM, et al. Completed and attempted suicides among 18,154 subjects with schizophrenia included in a large simple trial. J Clin Psychiatry. (2014) 75:e184–90. doi: 10.4088/JCP.13m08563
25. Jo, A, Kim, H, Lee, JY, Kim, JM, Jeong, MH, Chung, YC, et al. The effects of patient personality traits and family cohesion on the treatment delay for patients with first-episode schizophrenia spectrum disorder. Early Interv Psychiatry. (2021) 15:889–95. doi: 10.1111/eip.13029
26. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 5th ed. Arlington, VA, USA: American Psychiatric Publishing (2013).
27. Harris, MG, Henry, LP, Harrigan, SM, Purcell, R, Schwartz, OS, Farrelly, SE, et al. The relationship between duration of untreated psychosis and outcome: an eight-year prospective study. Schizophr Res. (2005) 79:85–93. doi: 10.1016/j.schres.2005.05.024
28. Woods, SW. Chlorpromazine equivalent doses for the newer atypical antipsychotics. J Clin Psychiatry. (2003) 64:663–7. doi: 10.4088/jcp.v64n0607
29. Jang, HA, Park, E, Jon, DI, Park, HJ, Hong, HJ, Jung, MH, et al. Validation of the Columbia suicide severity rating scale in depression patients. Korean J Clin Psychol. (2014) 33:799–814. doi: 10.15842/kjcp.2014.33.4.008
30. Posner, K, Brown, GK, Stanley, B, Brent, DA, Yershova, KV, Oquendo, MA, et al. The Columbia-suicide severity rating scale: initial validity and internal consistency findings from three multisite studies with adolescents and adults. Am J Psychiatry. (2011) 168:1266–77. doi: 10.1176/appi.ajp.2011.10111704
31. Kay, SR, Fiszbein, A, and Opler, LA. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr Bull. (1987) 13:261–76. doi: 10.1093/schbul/13.2.261
32. Yi, JS, Ahn, YM, Shin, HK, An, SK, Joo, YH, Kim, YS, et al. Reliability and validity of the Korean version of the positive and negative syndrome scale. J Korean Neuropsychiatr Assoc. (2001) 40:1090–105.
33. Morosini, PL, Magliano, L, Brambilla, L, Ugolini, S, and Pioli, R. Development, reliability and acceptability of a new version of the DSM-IV social and occupational functioning assessment scale (SOFAS) to assess routine social functioning. Acta Psychiatr Scand. (2000) 101:323–9. doi: 10.1111/j.1600-0447.2000.tb10933.x
34. Addington, D, Addington, J, and Schissel, B. A depression rating scale for schizophrenics. Schizophr Res. (1990) 3:247–51. doi: 10.1016/0920-9964(90)90005-r
35. Kim, YK, Won, SD, Lee, KM, Choi, HS, Jang, HS, Han, CS, et al. A study on the reliability and validity of the Korean version of the Calgary depression scale for schizophrenia(K-CDSS). J Korean Neuropsychiatr Assoc. (2005) 44:446–55.
36. Beck, AT, Ward, CH, Mendelson, M, Mock, J, and Erbaugh, J. An inventory for measuring depression. Arch Gen Psychiatry. (1961) 4:561–71. doi: 10.1001/archpsyc.1961.01710120031004
37. Hahn, HM, Yum, TH, Shin, YW, Kim, KH, Yoon, DJ, and Chung, KJ. A standardization study of Beck depression inventory in Korea. J Korean Neuropsychiatr Assoc. (1986) 25:487–502.
38. Beck, AT, Weissman, A, Lester, D, and Trexler, L. The measurement of pessimism: the hopelessness scale. J Consult Clin Psychol. (1974) 42:861–5. doi: 10.1037/h0037562
39. Kim, S, Lee, EH, Hwang, ST, Hong, SH, Lee, K, and Kim, JH. Reliability and validity of the Korean version of the Beck hopelessness scale. J Korean Neuropsychiatr Assoc. (2015) 54:84–90. doi: 10.4306/jknpa.2015.54.1.84
40. Cohen, S, Kamarck, T, and Mermelstein, R. A global measure of perceived stress. J Health Social Behav. (1983) 24:385–96. doi: 10.2307/2136404
41. Park, JO, and Seo, YS. Validation of the perceived stress scale (PSS) on samples of Korean university students. Korean J Psychol. (2010) 29:611–29.
42. Smith, BW, Dalen, J, Wiggins, K, Tooley, E, Christopher, P, and Bernard, J. The brief resilience scale: assessing the ability to bounce back. Int J Behav Med. (2008) 15:194–200. doi: 10.1080/10705500802222972
43. Kim, SW, Shin, IS, Kim, JM, Yoo, JA, Ahn, YM, Kwon, JS, et al. A validation study of the Korean version of the subjective well-being under neuroleptic treatment scale-short form. Korean J Psychopharmacol. (2007) 18:221–30.
44. Miller, GA. The magical number seven plus or minus two: some limits on our capacity for processing information. Psychol Rev. (1956) 63:81–97. doi: 10.1037/h0043158
45. Richardson, JT. Measures of short-term memory: a historical review. Cortex. (2007) 43:635–50. doi: 10.1016/s0010-9452(08)70493-3
46. Kwon, JS, Lyoo, IK, Hong, KS, Yeon, BK, and Ha, KS. Development and standardization of the computerized memory assessment for Korean adults. J Korean Neuropsychiatr Assoc. (2002) 41:347–58.
47. Rey, A. L’examen clinique en psychologie (the clinical psychological examination). Paris: Presse Universitaires de France (1964).
48. Salthouse, TA, Babcock, RL, and Shaw, RJ. Effects of adult age on structural and operational capacities in working memory. Psychol Aging. (1991) 6:118–27. doi: 10.1037/0882-7974.6.1.118
49. Milner, B. Effects of different brain lesions on card sorting. Arch Neurol. (1963) 9:90–100. doi: 10.1001/archneur.1963.00460070100010
50. Heaton, RK, Chelune, GJ, Talley, JL, Kay, GG, and Curtis, G. Wisconsin card sorting test manual. FL: Odessa: Psychological Assessment Resources (1993).
51. Miles, S, Howlett, CA, Berryman, C, Nedeljkovic, M, Moseley, GL, and Phillipou, A. Considerations for using the Wisconsin card sorting test to assess cognitive flexibility. Behav Res Methods. (2021) 53:2083–91. doi: 10.3758/s13428-021-01551-3
52. Rosvold, HE, Mirsky, AF, Sarason, I, Bransome, ED Jr, and Beck, LH. A continuous performance test of brain damage. J Consult Psychol. (1956) 20:343–50. doi: 10.1037/h0043220
53. Riccio, CA, Reynolds, CR, Lowe, P, and Moore, JJ. The continuous performance test: a window on the neural substrates for attention? Arch Clin Neuropsychol. (2002) 17:235–72. doi: 10.1093/arclin/17.3.235
54. Ha, KS, Kwon, JS, and Lyoo, IK. Development and standardization of the computerized attention assessment for Korean adults. J Korean Neuropsychiatr Assoc. (2002) 41:335–46.
56. Llinàs-Reglà, J, Vilalta-Franch, J, López-Pousa, S, Calvó-Perxas, L, Torrents Rodas, D, and Garre-Olmo, J. The trail making test. Assessment. (2017) 24:183–96. doi: 10.1177/1073191115602552
57. Folstein, MF, Folstein, SE, and McHugh, PR. Mini-mental state. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. (1975) 12:189–98. doi: 10.1016/0022-3956(75)90026-6
58. Harvey, PD, White, L, Parrella, M, Putnam, KM, Kincaid, MM, Davidson, M, et al. The longitudinal stability of cognitive impairment in schizophrenia. Mini-mental state scores at one-and two-year follow-ups in geriatric in-patients. Br J Psychiatry. (1995) 166:630–3. doi: 10.1192/bjp.166.5.630
59. Kang, YW, Na, DL, and Han, SH. A validity study on the korean mini-mental state examination (K-MMSE) in dementia patients. J Korean Neurol Assoc. (1997) 15:300–8.
60. Benton, AL, and Hamscher, K. Multilingual aphasia examination manual, revised. Iowa City: University of Iowa (1978).
61. van Beilen, M, Pijnenborg, M, van Zomeren, EH, van den Bosch, RJ, Withaar, FK, and Bouma, A. What is measured by verbal fluency tests in schizophrenia? Schizophr Res. (2004) 69:267–76. doi: 10.1016/j.schres.2003.09.007
62. Wimmer, H, and Perner, J. Beliefs about beliefs: representation and constraining function of wrong beliefs in young children's understanding of deception. Cognition. (1983) 13:103–28. doi: 10.1016/0010-0277(83)90004-5
63. Na, MH, Oh, JE, Shin, YW, Ha, TH, Lee, KJ, Kwon, JS, et al. “Theory of mind” deficits in schizophrenia. Korean J Schizophr Res. (2005) 8:17–24.
64. Brüne, M. Social cognition and behaviour in schizophrenia In: M Brüne, H Ribbert, and W Schiefenhövel, editors. The social brain: Evolution and pathology. Chichester: John Wiley (2003). 277–313. doi: 10.1002/0470867221.ch13
65. Lee, KM, Kim, SW, Yoon, JS, Hong, CH, Yeum, SH, Bae, A, et al. The relationship between theory of mind and suicide attempts in patients with schizophrenia. Korean J Schizophr Res. (2011) 14:105–11.
66. Lewis, L. Mourning, insight, and reduction of suicide risk in schizophrenia. Bull Menn Clin. (2004) 68:231–44. doi: 10.1521/bumc.68.3.231.40405
67. Perkins, DO, Gu, H, Boteva, K, and Lieberman, JA. Relationship between duration of untreated psychosis and outcome in first-episode schizophrenia: a critical review and meta-analysis. Am J Psychiatry. (2005) 162:1785–804. doi: 10.1176/appi.ajp.162.10.1785
68. Marshall, M, Lewis, S, Lockwood, A, Drake, R, Jones, P, and Croudace, T. Association between duration of untreated psychosis and outcome in cohorts of first-episode patients: a systematic review. Arch Gen Psychiatry. (2005) 62:975–83. doi: 10.1001/archpsyc.62.9.975
69. Clarke, M, Whitty, P, Browne, S, Mc Tigue, O, Kinsella, A, O'Callaghan, E, et al. Suicidality in first episode psychosis. Schizophr Res. (2006) 86:221–5. doi: 10.1016/j.schres.2006.05.026
70. Mitter, N, Subramaniam, M, Abdin, E, Poon, LY, and Verma, S. Predictors of suicide in Asian patients with first episode psychosis. Schizophr Res. (2013) 151:274–8. doi: 10.1016/j.schres.2013.10.006
71. Sönmez, N, Romm, KL, Andreasssen, OA, Melle, I, and Røssberg, JI. Depressive symptoms in first episode psychosis: a one-year follow-up study. BMC Psychiatry. (2013) 13:106. doi: 10.1186/1471-244X-13-106
72. Upthegrove, R, Birchwood, M, Ross, K, Brunett, K, McCollum, R, and Jones, L. The evolution of depression and suicidality in first episode psychosis. Acta Psychiatr Scand. (2010) 122:211–8. doi: 10.1111/j.1600-0447.2009.01506.x
73. Drake, RE, and Cotton, PG. Depression, hopelessness and suicide in chronic schizophrenia. Br J Psychiatry. (1986) 148:554–9. doi: 10.1192/bjp.148.5.554
74. Ribeiro, JD, Huang, X, Fox, KR, and Franklin, JC. Depression and hopelessness as risk factors for suicide ideation, attempts and death: meta-analysis of longitudinal studies. Br J Psychiatry. (2018) 212:279–86. doi: 10.1192/bjp.2018.27
75. Kim, SW, Kim, SY, Ryu, S, Lee, JY, Shin, IS, Kim, JM, et al. Development of a checklist for predicting suicidality based on risk and protective factors: the Gwangju checklist for evaluation of suicidality. Psychiatry Investig. (2022) 19:470–9. doi: 10.30773/pi.2022.0063
76. Kim, SW, Kim, JJ, Lee, BJ, Lee, JY, Kim, JM, Chung, YC, et al. Clinical and psychosocial factors associated with depression in patients with psychosis according to stage of illness. Early Interv Psychiatry. (2020) 14:44–52. doi: 10.1111/eip.12806
77. Li, W, Yang, Y, An, FR, Zhang, L, Ungvari, GS, Xiang, YT, et al. Prevalence of comorbid depression in schizophrenia: a meta-analysis of observational studies. J Affect Disord. (2020) 273:524–31. doi: 10.1016/j.jad.2020.04.056
78. Roy, A, and Pompili, M. Management of schizophrenia with suicide risk. Psychiatr Clin North Am. (2009) 32:863–83. doi: 10.1016/j.psc.2009.08.005
79. Berardelli, I, Sarubbi, S, Rogante, E, Hawkins, M, Cocco, G, Pompili, M, et al. The role of demoralization and hopelessness in suicide risk in schizophrenia: a review of the literature. Medicina (Kaunas). (2019) 55:200. doi: 10.3390/medicina55050200
80. Diago, M, Vila-Badia, R, Serra-Arumí, C, Butjosa, A, Del Cacho, N, Esteban Sanjusto, M, et al. Emotional abuse and perceived stress: the most relevant factors in suicide behavior in first-episode psychosis patients. Psychiatry Res. (2022) 315:114699. doi: 10.1016/j.psychres.2022.114699
81. Vila-Badia, R, Kaplan, M, Butjosa, A, Del Cacho, N, Serra-Arumí, C, Usall, J, et al. Suicidal behaviour in first-episode psychosis: the relevance of age, perceived stress and depressive symptoms. Clin Psychol Psychother. (2022) 29:1364–73. doi: 10.1002/cpp.2716
82. Yeo, JJ, Chew, QH, and Sim, K. Resilience and its inter-relationship with symptomatology, illness course, psychosocial functioning, and mediational roles in schizophrenia: a systematic review. Asia Pac Psychiatry. (2022) 14:e12486. doi: 10.1111/appy.12486
83. Premack, D, and Woodruff, G. Does the chimpanzee have a theory of mind? Behav Brain Sci. (1978) 1:515–26. doi: 10.1017/S0140525X00076512
84. Champagne-Lavau, M, Charest, A, Anselmo, K, Rodriguez, JP, and Blouin, G. Theory of mind and context processing in schizophrenia: the role of cognitive flexibility. Psychiatry Res. (2012) 200:184–92. doi: 10.1016/j.psychres.2012.06.011
85. Sami, H, Tei, S, Takahashi, H, and Fujino, J. Association of cognitive flexibility with neural activation during the theory of mind processing. Behav Brain Res. (2023) 443:114332. doi: 10.1016/j.bbr.2023.114332
86. Novak, LA, Carter, SP, LaCroix, JM, Perera, KU, Neely, LL, Soumoff, A, et al. Cognitive flexibility and suicide risk indicators among psychiatric inpatients. Psychiatry Res. (2022) 313:114594. doi: 10.1016/j.psychres.2022.114594
87. Chung, DT, Ryan, CJ, Hadzi-Pavlovic, D, Singh, SP, Stanton, C, and Large, MM. Suicide rates after discharge from psychiatric facilities: a systematic review and Meta-analysis. JAMA Psychiatry. (2017) 74:694–702. doi: 10.1001/jamapsychiatry.2017.1044
88. Ng, R, Fish, S, and Granholm, E. Insight and theory of mind in schizophrenia. Psychiatry Res. (2015) 225:169–74. doi: 10.1016/j.psychres.2014.11.010
89. López-Moríñigo, JD, Wiffen, B, O'Connor, J, Dutta, R, di Forti, M, Murray, RM, et al. Insight and suicidality in first-episode psychosis: understanding the influence of suicidal history on insight dimensions at first presentation. Early Interv Psychiatry. (2014) 8:113–21. doi: 10.1111/eip.12042
Keywords: suicide, cognitive function, schizophrenia, early psychosis, depression
Citation: Kim JS, Baek SH, Kim H, Kim JW, Kang HJ, Ryu S, Lee JY, Kim JM and Kim SW (2023) Association between suicidal ideation and cognitive function in young patients with schizophrenia spectrum disorder. Front. Psychiatry. 14:1276511. doi: 10.3389/fpsyt.2023.1276511
Edited by:
Takahiro Nemoto, Toho University, JapanReviewed by:
Chen Zhu, Shenzhen University, ChinaPadmavati Ramachandran, Schizophrenia Research Foundation, India
Copyright © 2023 Kim, Baek, Kim, Kim, Kang, Ryu, Lee, Kim and Kim. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Sung-Wan Kim, c3draW1AY2hvbm5hbS5hYy5rcg==
 Ji-Su Kim1
Ji-Su Kim1 Seon-Hwa Baek
Seon-Hwa Baek Honey Kim
Honey Kim Seunghyong Ryu
Seunghyong Ryu Ju-Yeon Lee
Ju-Yeon Lee Jae-Min Kim
Jae-Min Kim Sung-Wan Kim
Sung-Wan Kim