
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Pharmacol. , 01 April 2025
Sec. Neuropharmacology
Volume 16 - 2025 | https://doi.org/10.3389/fphar.2025.1571376
Introduction: Cenobamate is a new antiseizure medication approved for polytherapy of focal epilepsy with complex hepatic metabolism and effects on liver enzymes. So far, data are limited with regard to possible interactions with other antiseizure medications. We here report effects of Cenobamate on serum levels of Brivaracetam, a SV2-agent modulating presynaptic neurotransmitter release.
Methods: Retrospective analysis of Brivaracetam serum concentrations with new introduction of Cenobamate with Brivaracetam as a constant baseline antiseizure medication in 19 patients with focal epilepsy. Statistical analysis using paired Fisher´s exact t-Test.
Results: New introduction of Cenobamate lead to a statistically significant increase in Brivaracetam serum concentrations with a mean increase by 27%. This was infrequently accompanied by adverse effects.
Discussion: New introduction of Cenobamate to a pre-existing antiseizure regimen containing Brivaracetam leads to considerably increases in Brivaracetam, probably related to inhibition of CYP2C19. This needs to be taken into account when interpreting changes in treatment efficacy, but also when relating potential adverse effects to baseline vs. newly introduced treatment.
Focal epilepsies account for 61% of epilepsies worldwide. Even though antiseizure treatment has been significantly optimized in recent years through the introduction of new antiseizure medication with extended and partially new mechanisms of action, up to 31% (Janmohamed et al., 2023) of all patients with focal epilepsy remain refractory to pharmacological treatment. Polytherapy, the use of new ASM and the understanding of its pharmacokinetics are necessary to achieve satisfactory results in the majority of patients (Operto et al., 2023). The resulting drug load may contribute to the burden of epilepsy in this difficult-to-treat population, and drug interactions may contribute to this (Operto et al., 2023).
Having been approved by the US Food and Drug Administration in November 2019 and by the European Medicines Agency in March 2021 for the adjunctive treatment of focal onset seizures in adults, Cenobamate (Ontozry, Angelini) plays a pivotal role in the treatment of difficult to treat and pharmacorefractory focal epilepsy. According to real life studies, Cenobamate (CNB) can achieve a >50% seizure reduction in 55%–63%, and a >75% reduction in 27,9%–35% (Novitskaya et al., 2024; Villanueva et al., 2023), while 13,3% (Villanueva et al., 2023) and 14% (Steinhoff et al., 2024) of patients with focal epilepsy obtain seizure freedom. Furthermore CNB contributes to a significant reduction of concomitant ASMs (Roberti et al., 2024). Assenza et al. even suggest the use of CNB as a therapeutic response biomarker as they provide evidence of qEEG modulations which correlate with CNB induced changes in seizure frequency (Assenza et al., 2025).
CNB is a tetrazole carbamate derivate. The favourable effects on seizure outcome are attributed to its dual complementary mechanism of action with blockade of voltage-gated sodium channels (VGSCs) (Keam, 2020; Löscher et al., 2020) and allosteric modulation of synaptic and extrasynaptic γ-aminobutyric acid type A receptors (GABA-A- receptors) on the other side.
The absorption rate after oral administration is almost 90% (Steinhoff et al., 2024). The maximum serum concentration (Cmax) is reached after 0.8–3.5 h and a plateau for 6–12 h after administration. The elimination half-life time (t ½) diverges between 30 and 76 h (Vernillet et al., 2020). The steady-state serum concentration is reached after 2 weeks of daily dosing.
CNB is metabolized to a major amount in the liver through glucuronidation (via UGT2B7 and UGT2B4) and oxidation (via CYP2E1, CYP2A6, CYP2B6), and to a lesser extent through hydroxilation (via CYP2C19 and CYP3A4/5) (Vernillet et al., 2020). In the first 24 h the parent drug is the predominant circulating moiety.
The concentration-time profile shows a non-linear multiphase elimination. with the parent drug and its metabolites being eliminated by a distinct mechanism. The main route of excretion is renally (>80%). CNB is a CYP2C19-inhibitor, and a CYP2C8- and CYP2B6-inductor. Furthermore it exhibits a dose-dependent induction of CYP3A4-activity and has a minor effect on CYP2C9 activity (Greene et al., 2022). By inhibiting CYP2C19 CNB leads to an increase of the serum level of PHY and PB (84% and 37%) (Roberti et al., 2021) while its own AUC diminishes up to 28% vs. 15%. Likewise an increase of the active metabolite of clobazam with concomitant CNB therapy is observed due to CYP2C19-inhibition. A dose reduction is to be considered. In contrast, the blood level of Lamotrigine is reduced by 21%–52% (Roberti et al., 2021). Roberti et al. (2021) postulated potential interactions between CNB and Brivaracetam (BRV) in an increase of the BRV serum level through CYP2C19-inhibition with a consecutive need of dose-adaption of BRV. BRV is thought to reduce the release of neurotransmitters by serving as a ligand to synaptic glycoprotein SV2A in the brain with a 15–30 times higher selective affinity than its analogue Levetiracetam. This may contribute to a more favourable profile of side effects with comparable antiseizure effect to Levetiracetam (Khaleghi and Nemec, 2017). Hirsch et al. (2018) could demonstrate that in 57.1% of patients that switched from Levetiracetam to BRV because of affective side effects a better tolerability was achieved.
BRV is completely absorbed after oral administration and has a linear pharmacokinetic profile. The plasma protein binding is low. It underlies a high amount of biotransformation processes through different metabolic pathways and over 90% are eliminated renally (Laura et al., 2008).
The three main metabolites are formed by amidase-mediated hydrolysis of the acetamide group (60%), CYP-mediated hydroxylation on the propyl side chain (30%) (Dean et al., 2012), and a combination of the two. The metabolites are not pharmacologically active. In vitro inhibition assays and the result of a gemfibrozil clinical trial demonstrated that CYP2C8 and CYP2C9 were not involved, but CYP2C19 is predominantly mediating the hydroxylation pathway (Molteni et al., 2024).
This results in a significant decrease of the hydroxyl metabolite (2–10 fold) in people with genetic CYP2C19-variations, in whom BRV blood level can increase between 22% and 42% depending on the genetic variant (Dean et al., 2012), or patients on a therapeutic regime with CYP2C19-inhibitors. Compensatory dose adaptations have been discussed to compensate for this effect.
We here, for the first time provide data of the pharmacokinetic interactions resulting from Co-administration of the CYP2C19-inhibitor CNB to BRV as a CYP2C19-substrate, and possible clinical correlates thereof.
Between June 2021 and October 2023 112 adult patients with refractory focal epilepsy were started on CNB as adjunctive treatment as part of a real-world, long-term, prospective, open-label trial (Novitskaya et al., 2024) at the tertiary epilepsy centre at the university clinic in Freiburg. For the analysis of potential pharmacokinetic effects of CNB on BRV, we included all patients fulfilling the following criteria: unchanged baseline medication including BRV, at least 2 determinations of serum concentrations of BRV at the time of introduction and with uptitrated CNB to at least 100 mg/day, available documentation of dosages of CNB and BRV, and a stable BRV dosage through time of follow up.
Our aim was to compare the changes in serum concentrations of BRV in the initial phase of CNB-titration (group 1) with the concentrations in the further course of treatment (group 2).
Group 1 consisted of 19 patients (group 1, n = 19) in the initial titration phase, with a CNB dosage of 0–12.5 mg/day at first assessment (baseline dosage, t1) and re-assessment after introduction of CNB to 100–350 mg/day (t2). Group 2 consisted of 11 patients (group 2, n = 11) who were already under a stable CNB dose of 50–200 mg/d at first assessment (t3) and in whom the CNB dosage was further increased until the second assessment (t4) (Table 1.; Table 2.; Table 3). Patients with dose adaptions of BRV in the titration phase of CNB or in the further course of treatment were excluded from the analysis. Adverse events were noted. In case of occurrence the correlation with the BRV dosage, BRV concentration, and CNB dosage was investigated (Table 4). CNB concentrations were not tested.
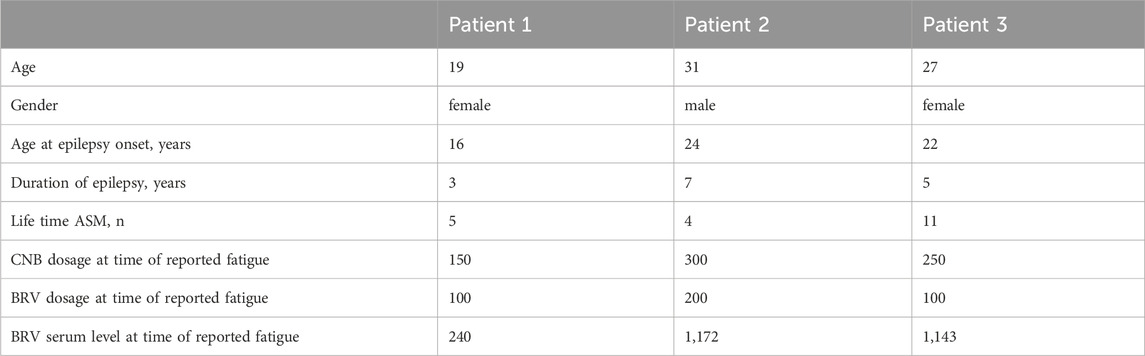
Table 4. Patients with minor adverse events: demographics, BRV and CNB dosages, and BRV serum level.
Whereas more recent studies proved Ultra-High Performance Liquid Chromatography–Tandem Mass Spectrometry as a highly sensitive and selective method to quantify CNB in plasma (Molteni et al., 2024), in our study BRV serum concentration was maintained by LC-MS (Liquid Chromatography-Mass Spectrometry) according to the latest ICH Guideline M10 for Bioanalytical Method Validation. (Stockis et al., 2014; European Medicines Agency, 2025).
No genetic testing on CYP-characteristics was performed.
To investigate the effect of CNB dose changes on the BRV serum concentration a two-sided Fisher’s exact test was applied in R and Excel.
The study included 30 adult patients with refractory focal epilepsy, aged between 21 and 69 years (M = 41,26), 14 males and 16 females. There were no differences in gender or age distribution between group 1 (21–69 years, females 9, males 10), and group 2 (23–60 years, females 6, males 5).
In group 1 (n = 19) the results of the BRV serum concentration at CNB doses of 0/12,5 mg/d (t1) showed a mean of 1562,3 μg/L (±748,29 g/L SD); the mean BRV serum concentration after the initial titration (t2) was 1963,47 μg/L (±712,24 μg/L SD) as shown in Figure 2a. 16/19 patients (84,21%) patients showed an increase of BRV serum concentrations at stable daily dosages of BRV as demonstrated in Figure 1a. The results were highly significant (p < 0.005). On average the concentration increased by 27%.
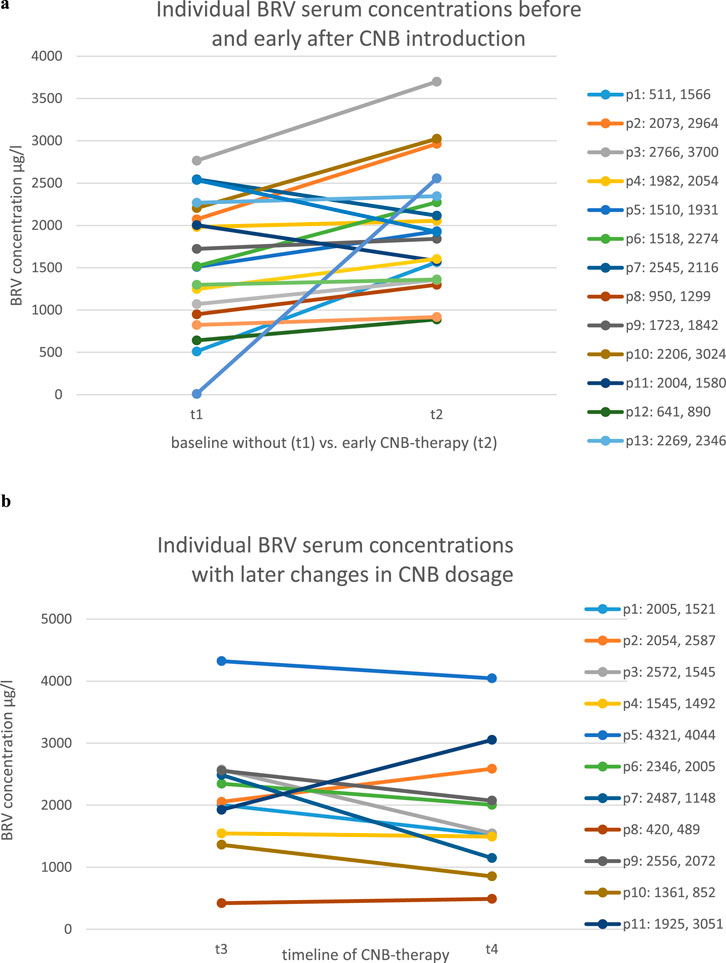
Figure 1. (a) Brivaracetam serum concentrations prior to CNB introduction (t1; CNB dosage 0–12.5 mg/day) vs. after introduction by at least 100 mg/day (t2) on a per-patient basis. (b) Brivaracetam serum concentrations with established CNB treatment (t1: CNB dosage >100 mg/day) later in the course of treatment (t2: 100–400 mg/day) on a per-patient basis.
In contrast, there were no significant changes in BRV concentrations after completed titration phase of CNB (t3, t4, >100–400 mg/d) as shown in Figure 1b. The results of the BRV serum concentration after completed titration (t3) showed a mean of 2144,73 μg/L (±918 μg/L SD) vs. 1891,45 μg/L (±978,13 μg/L SD) at a second time of comparison in the further course of CNB-treatment (t4) demonstrated in Figure 2b. 3/11 patients (27,3%) showed an increase of the BRV serum level while 8/11 (72,73%) did not (differences n. s.).
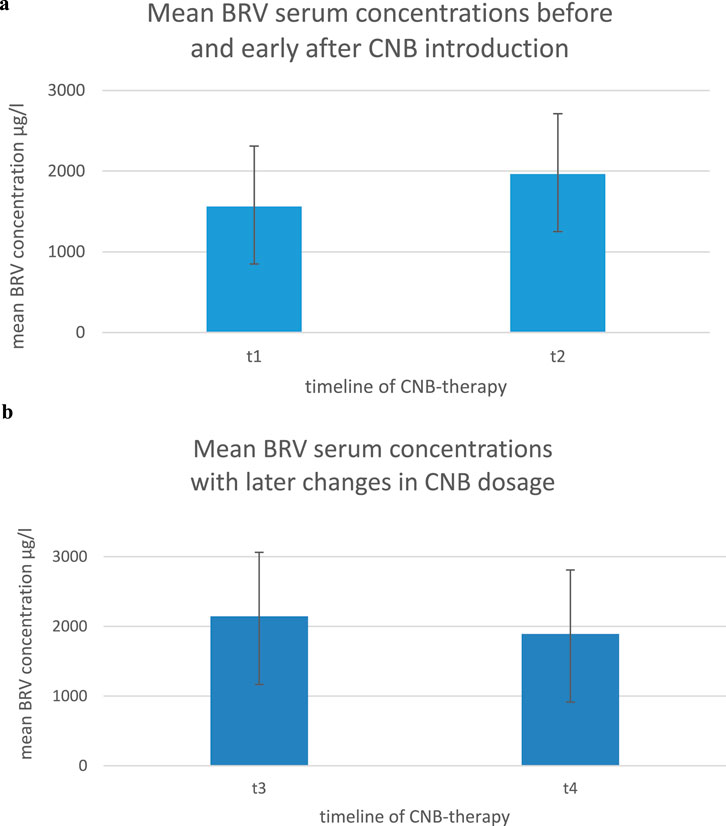
Figure 2. (a) Brivaracetam serum concentrations prior to CNB introduction (t1; CNB dosage 0–12.5 mg/day) vs. after introduction by at least 100 mg/day (t2) as means ± standard deviation. (b) Brivaracetam serum concentrations with established CNB treatment (t1: CNB dosage >100 mg/day) later in the course of treatment (t2: 100–400 mg/day) on a per-patient basis as means ± standard deviation.
The two-sided Fisher’s exact test revealed a significant difference between the distribution of slopes (p < 0.005).
The overall tolerability of the combined therapy with BRV and CNB was good. There was no report of major adverse events associated with increasing drug level of BRV, however, three patients complained about a transient fatigue after increase of CNB-dosage with consecutive reduction of BRV dosage and clinical improvements thereafter. Only in one patient with constant BRV dosage, fatigue was accompanied by an increase in BRV serum concentration as shown in Table 2.
We here found a statistically significant, yet clinically mostly asymptomatic increase of BRV levels with new introduction of CNB to a pre-existing treatment with BRV. By inhibiting CYP2C19 CNB is known to increase the serum level of Phenytoin and Phenobarbital while its own serum concentration decreases when being part of a polytherapy regime that includes other enzyme-inducers. In addition, CNB has similar pharmacodynamic properties with certain ASM, thus co-administration is more likely to cause additive adverse effects, such as in combination with i.e., Lacosamide. A potential pharmacokinetic effect of CNB in BRV shown here had been postulated in a review of pharmacokinetic properties of CNB by Roberti et al. (2021), suggesting that an increase due to inhibition of CYP2C19 might necessitate a dose reduction of BRV. We could confirm the pharmacokinetic interaction, yet with minor pharmacodynamics consequences. This may well reflect the high therapeutic index of SV2A blockers (Schulze-Bonhage, 2011).
Whereas we found significant changes of BRV serum concentrations with new introduction of CNB, dose modifications in the further course of combined treatment were no longer significant. This suggests that relevant inhibition of CYP2C19 takes place already at lower dosages, e.g., in the range of 50–100 mg CNB/day, with minor effects of further increases in dosages. This resembles other inhibitory pharmacokinetic interactions, as e.g., seen with valproate and lamotrigine (May et al., 1996). Certainly this findings needs to be confirmed in larger patient populations.
Adverse effects were limited, however, with rare increases in fatigue reported. The finding that reductions in Brivaracetam dosage lead to the cessation of this adverse effects may point to both, pharmacodynamics and pharmacokinetic interactions of the two drugs. Similarly, in the few patients reporting daytime fatigue, reduction of BRV dosage was effective to ameliorate this symptom of combined administration of the two antiseizure medications and thus may not only be indicative of dose-related adverse effects of CNB administration.
The sample size of 30 patients and the retrospective design are limitations of this study. Thus larger prospective studies are needed to confirm the reported pharmacokinetic interaction. Furthermore a detailed CYP-assessment may provide additional information about the interactions between the two drugs across the spectrum of applied dosages.
Our findings provide first evidence that in the initial titration phase of CNB, serum concentrations of co-administered BRV increase in the majority of patients, whereas there is no significant increase in the course of combined therapy with CNB and BRV with further up-titration of CNB. This reflects an expected effect on CYP enzymes already at low dosages of an enzyme inhibiting drug, and less systematic effects once enzyme inhibition has occurred and dosages of the inhibitor are changed.
Changes in Brivaracetam serum concentrations may thus contribute to an increased efficacy observed with add-on treatment of CNB to a preixisting treatment with BRV. Similarly, potential clinical adverse effects may be related either to CNB or to BRV in this titration phase. Interestingly, despite of high serum concentrations of BRV throughout the titration phase of CNB only few substance-related adverse events were reported by patients. This may reflect the known high therapeutic index in SV2A ligands (Matagne et al., 2008). Nevertheless, there was a small number of patients reporting sleepiness without a direct correlation with elevated drug levels of BRV.
The original contributions presented in the study are included in the article/supplementary material, further inquiries can be directed to the corresponding author.
The studies involving humans were approved by Ethics committeeof the University of Freiburg, Germany (reference number 21–1505). The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
LB: Conceptualization, Investigation, Visualization, Writing – original draft, Writing – review and editing. MH: Data curation, Writing – review and editing. AS-B: Conceptualization, Supervision, Writing – review and editing.
The author(s) declare that no financial support was received for the research and/or publication of this article.
MH. has received lecture fees or grants from, UCB, Angelini Pharma and UNEEG. AS-B. has received honoraria for lectures or consulting fees from Angelini Pharma, Bial, Desitin, Eisai, GW Pharmaceuticals, Jazz Pharmaceuticals, and UCB Pharma outside the submitted work. We confirm that we have read the Journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
The remaining author declares that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The author(s) declare that no Generative AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Assenza, G., Sancetta, B., Ricci, L., Vico, C., Narducci, F., Boscarino, M., et al. (2025). Cenobamate modulates EEG cortical activity and connectivity in individuals with drug-resistant epilepsy: a pharmaco-EEG study; Front. Neurol. 15, 1502668–2024. doi:10.3389/fneur.2024.1502668
Dean, L. (2012). “Brivaracetam therapy and CYP2C19 genotype. 2018 may 15,” in Medical genetics summaries. V. M. Pratt, S. A. Scott, and M. Pirmohamed (Bethesda: National Center for Biotechnology Information US). Available online at: https://www.ncbi.nlm.nih.gov/books/NBK500036/.
Greene, S. A., Kwak, C., Kamin, M., Vernillet, L., Glenn, K. J., Gabriel, L., et al. (2022). Effect of cenobamate on the single-dose pharmacokinetics of multiple cytochrome P450 probes using a cocktail approach in healthy subjects. Clin. Transl. Sci. 15 (4), 899–911. doi:10.1111/cts.13204
Hirsch, M., Hintz, M., Specht, A., and Schulze-Bonhage, A. (2018). Tolerability, efficacy and retention rate of Brivaracetam in patients previously treated with Levetiracetam: a monocenter retrospective outcome analysis. Seizure 61, 98–103. doi:10.1016/j.seizure.2018.07.017
European Medicines Agency (2025). ICH guideline M10 on bioanalytical method validation and study sample analysis-Questions and Answers-EMA/CHMP/ICH/660315/2022. Available online at: https://www.ema.europa.eu/en/ich-m10-bioanalytical-method-validation-scientific-guideline. (Accessed March 25, 2025).
Janmohamed, M., Hakeem, H., Ooi, S., Hakami, S., Vu, L., Perucca, P., et al. (2023). Treatment outcomes of newly diagnosed epilepsy: a systematic review and meta-analysis. CNS Drugs 37 (1), 13–30. doi:10.1007/s40263-022-00979-1
Khaleghi, F., and Nemec, E. C. (2017). Brivaracetam (Briviact): A novel adjunctive therapy for partial-onset seizures. P T 42 (2), 92–96.
Laura, S.-M. M., Espié, P., Coquette, A., and Stockis, A. (2008). “Pharmacokinetics and metabolism of 14C-brivaracetam, a novel SV2A ligand, in healthy subjects,”. Editor H. Subjects, Drug Metabolism Dispos 36, 36–45. doi:10.1124/dmd.107.017129
Löscher, W., Potschka, H., Sisodiya, S. M., and Vezzani, A. (2020). Drug resistance in epilepsy: clinical impact, potential mechanisms, and new innovative treatment options. Pharmacol. Rev. 72 (3), 606–638. doi:10.1124/pr.120.019539
Matagne, A., Margineanu, D., Kenda, B., Michel, P., and Klitgaard, H. (2008). Anti-convulsive and anti-epileptic properties of brivaracetam (ucb 34714), a high-affinity ligand for the synaptic vesicle protein SV2A. Br. J. Pharmacol. 154, 1541662–1541671. doi:10.1038/bjp.2008.198
May, T. W., Rambeck, B., and Jürgens, U. (1996). Serum concentrations of lamotrigine in epileptic patients: the influence of dose and comedication. Ther. Drug Monit. 18 (5), 523–531. doi:10.1097/00007691-199610000-00001
Molteni, L., Charlier, B., Coglianese, A., Izzo, V., Assenza, G., Menna, P., et al. (2024). Quantitative analysis of cenobamate and concomitant anti-seizure medications in human plasma via ultra-high performance Liquid chromatography-tandem Mass Spectrometry. Molecules 29 (4), 884. doi:10.3390/molecules29040884
Novitskaya, Y., Schütz, E., Metternich, B., Schulze-Bonhage, A., and Hirsch, M. (2024). Add-on treatment with cenobamate is already effective at low doses in refractory focal epilepsy: a prospective observational study. Epilepsia 65, 630–640. doi:10.1111/epi.17874
Operto, F. F., Pastorino, G. M. G., Viggiano, A., Dell'Isola, G. B., Dini, G., Verrotti, A., et al. (2023). Epilepsy and cognitive impairment in childhood and adolescence: a mini-review. Curr. Neuropharmacol. 21 (8), 1646–1665. doi:10.2174/1570159X20666220706102708
Roberti, R., Assenza, G., Bisulli, F., Boero, G., Canafoglia, L., Chiesa, V., et al. (2024). Adjunctive cenobamate in people with focal onset seizures: insights from the Italian Expanded Access Program. Epilepsia 65 (10), 2909–2922. doi:10.1111/epi.18091
Roberti, R., De Caro, C., Iannone, L. F., Zaccara, G., Lattanzi, S., and Russo, E. (2021). Pharmacology of cenobamate: mechanism of action, pharmacokinetics, drug-drug interactions and tolerability. CNS Drugs 35 (6), 609–618. doi:10.1007/s40263-021-00819-8
Schulze-Bonhage, A. (2011). Brivaracetam for the treatment of epilepsy. Expert Opin. Pharmacother. 12 (12), 1959–1966. doi:10.1517/14656566.2011.591380
Steinhoff, B. J., Georgiou, D., Dietmann, D., and Intravooth, T. (2024). Cenobamate plasma levels in patients with epilepsy: correlation with efficacy and tolerability? J. Clin. Med. 13 (10), 2757. doi:10.3390/jcm13102757
Stockis, A., Watanabe, S., Rouits, E., Matsuguma, K., and Irie, S. (2014). Brivaracetam single and multiple rising oral dose study in healthy Japanese participants: influence of CYP2C19 genotype. Drug Metab. Pharmacokinet. 29 (5), 394–399. doi:10.2133/dmpk.dmpk-14-rg-010
Vernillet, L., Greene, S. A., Kim, H. W., Melnick, S. M., and Glenn, K. (2020). Mass balance, metabolism, and excretion of cenobamate, a new antiepileptic drug, after a single oral administration in healthy male subjects. Eur. J. Drug Metab. Pharmacokinet. 45 (4), 513–522. doi:10.1007/s13318-020-00615-7
Villanueva, V., Santos-Carrasco, D., Cabezudo-García, P., Gómez-Ibáñez, A., Garcés, M., Serrano-Castro, P., et al. (2023). Real-world safety and effectiveness of cenobamate in patients with focal onset seizures: outcomes from an Expanded Access Program. Epilepsia Open 8 (3), 918–929. doi:10.1002/epi4.12757
Keywords: antiseizure medication, epilepsy, brivaracetam, cenobamate, interaction, hepatic enzyme inhibition, serum levels
Citation: Bender L, Hirsch M and Schulze-Bonhage A (2025) Increase of Brivaracetam serum concentration with introduction of Cenobamate. Front. Pharmacol. 16:1571376. doi: 10.3389/fphar.2025.1571376
Received: 05 February 2025; Accepted: 24 March 2025;
Published: 01 April 2025.
Edited by:
Emilio Russo, Magna Græcia University, ItalyReviewed by:
Giovanni Assenza, Campus Bio-Medico University, ItalyCopyright © 2025 Bender, Hirsch, Schulze-Bonhage. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Lena Bender, bGVuYS5iZW5kZXJAdW5pa2xpbmlrLWZyZWlidXJnLmRl
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.