
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
SYSTEMATIC REVIEW article
Front. Neurol. , 02 April 2025
Sec. Experimental Therapeutics
Volume 16 - 2025 | https://doi.org/10.3389/fneur.2025.1488767
Background: Shoulder-hand syndrome (SHS) is one of the common sequelae after stroke, which not only hinders the recovery of patients, but also increases the economic burden of the family. In the absence of effective treatment measures, acupuncture treatment has been widely used in China to treat post-stroke shoulder-hand syndrome, but the details are unclear. Therefore, this review aims to evaluate the true efficacy of acupuncture in patients with SHS.
Methods: We searched eight databases [PubMed, Embase, Web of Science, Cochrane library, China Biomedical Literature Database (CBM), China Science and Technology Journal (VIP) database, the China National Knowledge Infrastructure (CNKI) database, and Wan fang database] from its inception to March 2025, randomized controlled trials (RCTs) of SHS acupuncture treatment combined with rehabilitation (Rehab). Two investigators independently used pre-designed forms to extract valid data from eligible randomized controlled trials. Meta-analysis was implemented through the Rev. Man software (version 5.4). The strength of the evidence obtained was implemented using the GRADE profiler software. Adverse events (AEs) were collected by reading the full text and used to evaluate the safety of acupuncture treatment.
Results: Forty-seven studies, involving 4,129 participants, met the eligibility criteria, and were included in the review. Overall meta-analysis showed that combined acupuncture rehabilitation significantly improved motor function (upper-limb Fugl-Meyer Assessment (FMA): 41 studies, mean difference (MD) 9.50, 95% confidence interval (CI) [8.47, 10.53]) and pain reduction (visual analog score (VAS): 37 studies, MD: −1.49, 95% CI [−1.66, −1.33]). It also improved activities of daily living (ADL) compared to rehabilitation alone (ADL: 17 studies, MD: 11.94, 95% CI [8.26, 13.63]). There was no significant difference in the occurrence of adverse events (AEs) between acupuncture treatment combined with Rehab and Rehab alone (p > 0.05). The certainty of the evidence was rated low level because of flaws in the study design and considerable heterogeneity among the included studies.
Conclusion: This review found that acupuncture treatment combined with Rehab treatment may have a positive promoting effect on improving motor function, reducing pain, and improving daily living ability in SHS patients. However, due to the existing methodological quality issues, our findings should be treated with caution. Future high-quality studies are urgently needed to validate our findings.
Systematic review registration: https://www.crd.york.ac.uk/PROSPERO/view/CRD42024536169.
Stroke is the second largest cause of death worldwide and the first leading cause of acquired long-term disability, leading to an annual global economic burden (1). Post-stroke shoulder hand syndrome (PS-SHS), also known as post-stroke complex regional pain syndrome, is experienced by more than 50% of stroke patients (2), it usually occurs between 2 and 3 months of an acute event and usually presents with pain, hyperalgesia, joint swelling, and limited range of motion (3). Post-stroke shoulder hand syndrome is difficult to treat, and its symptoms may persist for a long time, resulting in limited upper limb function or even irreversible permanent apraxia (4, 5). In addition, SHS may hinder the overall recovery, prolong hospitalization, limit the patients’ activities of daily living (ADL), reduce the quality of life, and bring heavy economic burden on the patients and their families (6). Currently, commonly used treatments for post-stroke SHS include drug therapy, soaking in cold water, physical therapy (PT), occupational therapy (OT), psychotherapy, and sympathetic block (7, 8). Although these conventional treatments were initially found to be effective, their adverse effects cannot be ignored. Low-dose oral steroids are effective in improving the SHS after stroke (9), for example, to avoid adverse effects associated with long-term drug use, steroids are only indicated for short-term treatment and are considered a difficult factor for long-term post-stroke SHS (5), early referral to PT, OT, and psychotherapy may prevent the progression of symptoms (10). However, the disadvantages of these approaches, such as high healthcare costs, increased workforce investment, and increased demands for patient collaboration, have also received attention. In addition, the expertise of rehabilitation therapists varies from different regions, which will affect the treatment effect. The incidence of SHS after stroke remains high and is a challenging problem to be addressed. To date, consistently effective and good patient compliance methods are still lacking (11).
As a basic therapy for the prevention and treatment of traditional Chinese medicine (TCM), acupuncture has been used in clinical practice in China for thousands of years (12). According to the site of application, acupuncture can be divided into abdominal acupuncture (AA) and scalp acupuncture (SA). In addition, according to the surgical method, acupuncture can be divided into manual needle (MA), electro-acupuncture (EA), and warm acupuncture (WA) has been proved to have the advantages of low price, good effect and simple operation (13). Moreover, as a non-pharmacological intervention, acupuncture has better efficacy on chronic diseases difficult to treat with traditional treatment methods, such as low back pain and renal disease (14, 15). As a result of these advantages, acupuncture has received continued interest from the general public and health professionals (16). Furthermore, more medical institutions are using acupuncture clinically and show that acupuncture can be used as a prospective therapeutic measure to improve motor function in patients with SHS (6, 17).
In the last few years, three reviews have been published on acupuncture for SHS. The meta-analysis published in 2018 (18) only evaluated the effect of manual acupuncture on the treatment efficacy in patients with SHS, and manual acupuncture represented only one acupuncture form, and the findings were necessarily limited. The meta-analysis published in 2019 (19) included only 13 studies totaling 1,040 patients, an insufficient sample size, and only evaluated the effect of electroacupuncture effects in SHS patients, and the findings were limited. The meta-analysis, published in 2019 (20), selected FMA, VAS and ADL as outcome measures. The results showed that acupuncture treatment had excellent efficacy in relieving the symptoms of SHS. However, the intervention did not involve warm acupuncture. Therefore, we conducted a systematic review of the latest evidence on acupuncture (including warm acupuncture) as an add-on treatment for the clinical treatment of post-stroke SHS. Furthermore, with the widespread use of acupuncture treatment, more research is published in recent years (17, 21). Therefore, the aim of this review was to explore the effect of acupuncture treatment on the relief of clinical symptoms in patients with SHS and to update previous published reviews.
The detailed protocol of this systematic review and meta-analysis has been registered on the international systematic review registration platform (PROSPERO) with the registration number is CRD42024536169 (22).
Randomized controlled trials (RCTs) on acupuncture treatment SHS from establishment to March 2025 in 8 databases including Web of Science, Embase, PubMed, Cochrane Liberary, Chinese Biomedical Literature Database (CBM), Chinese Science and technology Journal (VIP) database, China National Knowledge Infrastructure (CNKI) database and Wanfang database. Meanwhile, the reference lists of the identified included articles were screened to identify as many relevant articles as possible. No language restrictions were used during the search process. Search terms included “acupuncture treatment,” “electro-acupuncture,” “warm acupuncture,” “shoulder hand syndrome,” “SHS,” “stroke,” “cerebrovascular accident,” “acupuncture,” and “Hao zhen.” The specific search strategies are described in the Supplementary Material.
Two researchers independently screened and checked the titles and abstracts of the literature to be initially included based on the PICOS principles (patient, intervention, control, outcome, and study). The PICOS criteria used for literature screening were detailed as follows: (a) Type of participant: (1) The patient was diagnosed with stroke with no restrictions on age, sex and duration of disease. (2) Their condition was confirmed by magnetic resonance imaging (MRI) or electronic computed tomography (CT) scan. (3) Shoulder hand syndrome is caused by stroke, rather than by other diseases, such as trauma, periarthritis of shoulder, cervical spondylosis; (b) Type of intervention: the experimental group was treated with manual acupuncture (MA), electric acupuncture (EA) or warm acupuncture (WA), with or without the same treatment as the control group. For the control group, rehabilitation (Rehab) must be used and all other types of interventions should be excluded; (c) Type of outcome: Primary outcome measures: (1) motor function: upper limb Fugl-Meyer assessment (FMA) and (2) pain assessment using the visual analog scale (VAS). Secondary outcome measures: (1) Barthel index (BI) or modified Barthel index (MBI) for self-care and activities of daily living; (2) Edema and (3) adverse events. (d) Study type: Randomized Controlled Trial (RCT). The safety of acupuncture treatment was assessed by the severity and number of adverse events (AEs). The language types of these documents are limited to either the Chinese or English language.
Meanwhile, we excluded literature that met the following criteria: (1) Duplication of publications; (2) Studies compared different acupuncture therapies; (3) Full text is not available; (4) Lack of effective outcome measures; (5) Conferences; (6) The types of studies are reviews, animal experiments, conference articles, and case reports.
Two researchers independently used pre-designed forms to retrieve useful information from qualified studies, including publication year, first author, sample size, mean age and method used in experimental groups (e.g., acupuncture modality and acupoint selection), and duration and frequency of treatment. Any inconsistencies in information extraction could be resolved by consulting corresponding author. After data extraction was completed, researchers assessed the safety of acupuncture treatment by collecting adverse event reports from the included articles.
The risk of bias in the included randomized controlled trials was assessed using the revised Cochrane Risk of Bias Tool (RoB-2) (23). This evaluation addressed several key aspects: random sequence generation and allocation concealment (both related to selection bias), blinding of participants and personnel (performance bias), blinding of outcome assessment (detection bias), incomplete outcome data (attrition bias), selective reporting (reporting bias), and other potential biases. Each aspect was categorized based on the level of bias risk: low, unclear (indicating some concerns), or high. The findings from this comprehensive bias assessment were then visually represented using Revman 5.4 software, offering a clear graphical depiction of the potential biases within these trials.
Two researchers (JY-S and Y-L) assessed the quality of evidence for each outcome indicator by using the Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) system (24). When disagreements arose, they could be resolved through consultation or by consulting a third researcher. The quality of evidence for each outcome is displayed in the form of a GRADE evidence profile to determine the certainty of all pooled outcomes. The GRADE system includes five downgrading factors and three escalating factors, five downgrading factors consisting of risk of bias, inconsistency, indirectness, uncertainty, and publication bias, and three escalating factors consisting of larger effect values, dose effect relationships, and negative bias. The quality of evidence for each outcome was assessed by the eight factors mentioned above, which ultimately resulted in a high, moderate, low, or very low evidence level.
After data extraction was completed, Rev. Man 5.4 software (Cochrane Collaboration, Oxford, United Kingdom) was selected for statistical analysis. If the outcome indicator was a continuous variable, mean difference (MD) or standardized mean difference (SMD) and 95% confidence interval (CI) were selected for calculation. If the outcome indicator was a dichotomous variable, the risk ratio (RR) and 95% CI were selected for calculation. Heterogeneity between included studies was assessed using Q-tests (p-values) and the I2 statistic, and effect models were selected accordingly. If p < 0.1 and I2 > 50%, statistically significant heterogeneity among the included studies was detected and a random effects model was selected to calculate the effect size. Conversely, if p ≥ 0.1 and I2 ≤ 50%, the heterogeneity among the included studies was regarded as tolerable and we selected the fixed effects model to merge the data. This meta-analysis assessed the significance of the pooled results by Z-test, with p < 0.05 being a statistically significant difference.
We categorized the included studies according to different acupuncture types and treatment duration, which were MA, EA, WA, 0–4 weeks, and > 4 weeks. Subgroup analysis was attempted to account for possible heterogeneity under the stratification factors of different acupuncture types and treatment cycles. Sensitivity analyses were used to validate the robustness of the meta-analysis results and to explore potential sources of heterogeneity by excluding each individual study in the original analysis. For FMA, VAS, ADL, we used funnel plots and Egger’s tests to evaluate publication bias in the included studies.
Using a pre-defined search strategy, we initially retrieved 4,606 relevant records from eight databases. A total of 4,356 duplicate and irrelevant studies were excluded by screening titles and abstracts. Subsequently, the full texts of the remaining studies were reviewed, resulting in the exclusion of 203 records. Finally, 47 studies were included in the qualitative analysis (25–71). All included studies were conducted in China, consisting of 46 RCTs published in Chinese and 1 RCT in English. These studies were published between 2008 and 2025. Figure 1 shows the flow chart of the literature screening process for the systematic review and meta-analysis.
A total of 4,129 participants were included, with 2,068 in the experimental group and 2,061 in the control group. The sample size per study ranged from 40 to 178. The proportion of males was higher than that of females. The mean age of patients was similar in both groups. Among the studies, 29 reported SHS staging, including 21 studies on stage I (25, 26, 29, 31, 33, 35, 38, 40, 43, 44, 46, 49–52, 59, 60, 65, 66, 69, 70). Two studies (65, 70) reported participant dropouts (3 and 5 cases, respectively) with corresponding reasons provided. Details of the 47 included RCTs are summarized in Table 1.
In the included studies, manual acupuncture was the most frequently used intervention (59.57%), followed by electroacupuncture (25.53%) and warm acupuncture (14.89%). All included studies used Rehab as a control measure. The retention time ranged from 15 to 40 min, with 30 min being the most common duration (n = 35). The treatment frequency ranged from 3 to 7 times per week, with 5 times weekly being the most common pattern (n = 13). The treatment duration varied widely across studies, ranging from 2 to 8 weeks, where a 4-week treatment period was the most common (n = 21). Through analysis of acupoint selection patterns, we found that acupuncture points for SHS were primarily located in the shoulder and arm regions. The most frequently used acupoints were Wai-guan (SJ5) (63.83%), Jian-yu (LI15) (63.83%), He-gu (LI4) (61.70%), Qu-chi (LI11) (61.07%), Jian-liao (SJ14) (38.30%), Shou-san-li (LI10) (38.30%) and Jian-zhen (SI9) (31.91%). Table 2 details the intervention characteristics of the included studies.
The results of the methodological assessment are shown in Figure 2. Twenty-eight studies (25–27, 29–33, 38–42, 47, 51, 52, 54, 57–60, 62–64, 66, 68–70), were rated as low risk due to the use of random number tables or computer-generated randomization for sequence generation, while the remaining 19 studies (28, 34–37, 43–46, 48–50, 53, 55, 56, 61, 65, 67, 71) were classified as having unclear risk of bias due to insufficient information. None of the 47 studies described the allocation concealment process in sufficient detail, resulting in an unclear risk of bias judgment. Blinding of participants or personnel could not be implemented in any of the 47 studies because of significant differences in acupuncture treatment protocols between the intervention and control groups. The two studies (65, 70) were rated as high risk because they did not conduct appropriate intention-to-treat analysis in the context of the dropout situation. Forty-five studies were categorized as low risk of selective reporting bias because all pre-specified endpoints were reported, while two studies (27, 61) were rated as high risk of selective reporting bias due to incomplete endpoint reporting. For the remaining 47 studies, insufficient data were available to assess other potential sources of bias.
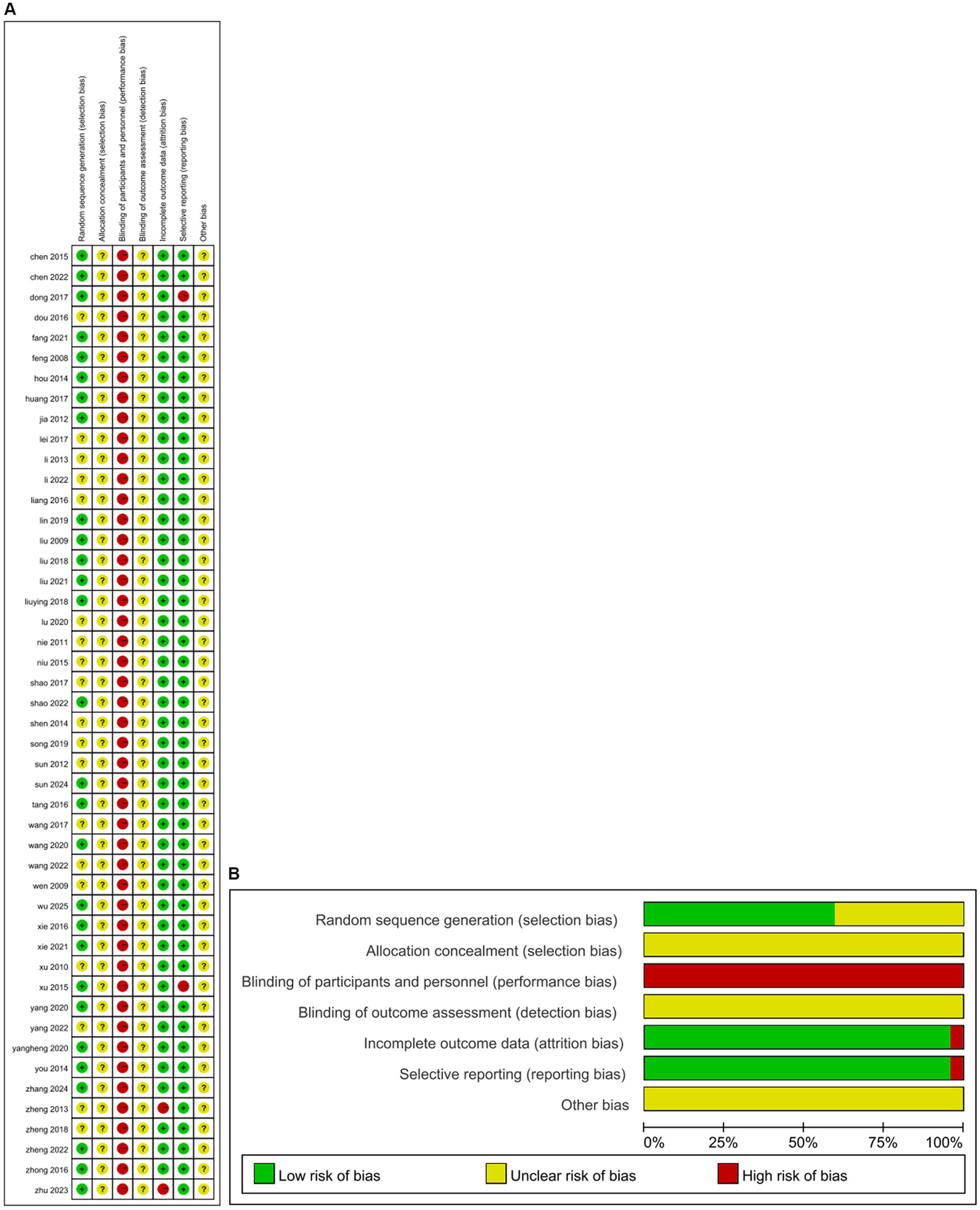
Figure 2. The figure represents the risk of bias assessment for the studies selected in the meta-analysis. (A) ROB graph. (B) ROB summary.
Forty-one studies (25–27, 29, 31, 33–46, 48–62, 64–71) involving 3,614 patients reported increased FMA scores with acupuncture combined with Rehab compared to Rehab alone. These studies showed significant statistical heterogeneity in FMA outcomes (p < 0.00001, I2 = 83%). Using a random-effects model, the pooled MD was 9.50 (95% CI: 8.47, 10.53). The results demonstrated a statistically significant difference between combined therapy and Rehab alone in the overall effect size (Z = 18.12, p < 0.00001; see Figure 3).
To evaluate the effects of acupuncture type and treatment duration on combined data, subgroup analyses were conducted. Acupuncture type subgroups included MA, EA, and WA. No significant differences were observed between subgroups (p = 0.99, I2 = 0%). WA combined with Rehab showed reduced heterogeneity and significant motor function improvement (MD: 9.48, 95% CI: [8.28, 10.67], p < 0.00001; Figure 4). Eleven studies (31, 33–37, 40, 49, 58, 64, 66) comparing EA plus Rehab with Rehab alone demonstrated significant motor function enhancement (MD: 9.64, 95% CI: [7.64, 11.64], p < 0.00001; Figure 4). Similarly, 22 studies (25–27, 38, 39, 41, 43, 45, 46, 48, 50–54, 56, 57, 60, 61, 65, 67, 69, 70) comparing MA plus Rehab with Rehab alone also showed significant improvement (MD: 9.44, 95% CI: [8.01, 10.87], p < 0.00001; Figure 4). For treatment duration subgroups (0–4 weeks vs. >4 weeks), no significant differences were found (p = 0.91, I2 = 0%). Both intervals improved motor function compared to controls (0–4 weeks: MD 9.54, 95% CI: [8.13, 10.95], p < 0.00001; >4 weeks: MD 9.43, 95% CI: [8.07, 10.77], p < 0.000001; Figure 5). Sensitivity analysis by removing high-weight studies identified Wang (54) in the >4 weeks subgroup as a potential heterogeneity source, likely due to its extended treatment duration. Exclusion of this study stabilized results with reduced heterogeneity (Supplementary Table 1). In acupuncture-type subgroup sensitivity analyses, no individual study significantly influenced MD values or heterogeneity.

Figure 4. Forest plot of the intervention subgroup of acupuncture treatment combined with Rehab vs. Rehab on FMA.
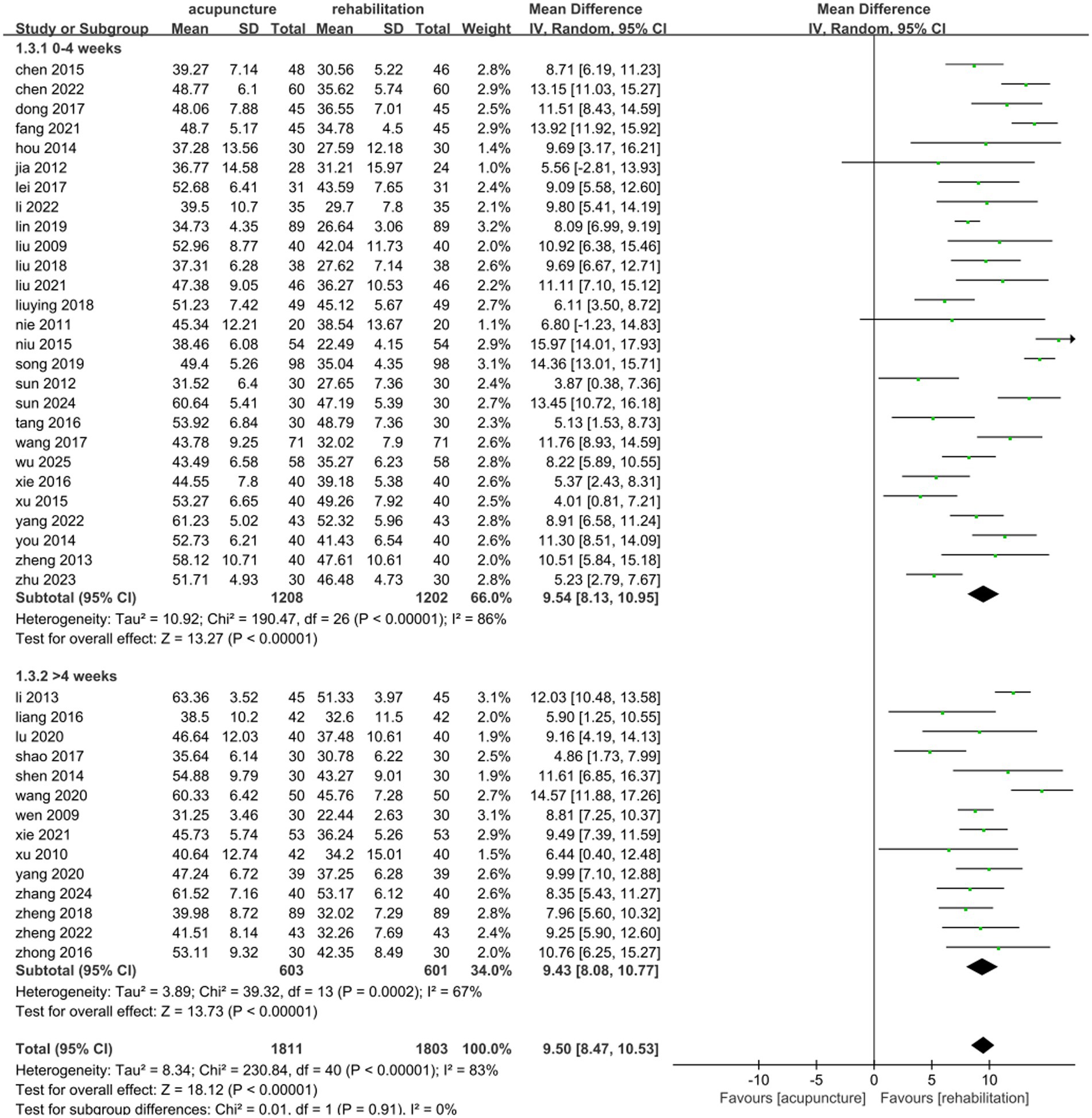
Figure 5. Forest plot of the treatment duration subgroup of acupuncture treatment combined with Rehab vs. on FMA.
Thirty-seven studies (25, 26, 31, 33–41, 43–47, 49–52, 54, 55, 57–65, 67, 69–71) involving 3,228 patients demonstrated that acupuncture combined with Rehab significantly reduced VAS scores compared to Rehab alone, with a pooled MD of −1.49 (95% CI: [−1.66, −1.33]; Z = 17.69, p < 0.00001) using a random-effects model. Substantial heterogeneity was observed (p < 0.00001, I2 = 86%)(Figure 6). Subgroup analyses by acupuncture type and treatment duration showed no significant inter-subgroup differences (acupuncture method: p = 0.38, I2 = 0%; duration: p = 0.24, I2 = 26.3%). Both EA + Rehab (MD: −1.57, 95% CI: [−1.78, −1.37], p < 0.0001) and WA + Rehab (MD: −1.65, 95% CI: [−1.85, −1.45]) exhibited reduced heterogeneity, while MA + Rehab also showed significant improvement (MD: −1.43, 95% CI: [−1.67, −1.19], p < 0.00001) (Figure 7). Treatment durations of 0–4 weeks (MD: −1.54, 95% CI: [−1.74, −1.34]) and > 4 weeks (MD: −1.35, 95% CI: [−1.67, −1.19]) both achieved statistical significance (p < 0.00001) (Figure 8). Sensitivity analysis excluding Li 2013 (35) mitigated heterogeneity in the EA + Rehab subgroup, possibly due to variations in disease duration and acupoint selection, though results remained favorable for combination therapy (Supplementary Table 1).
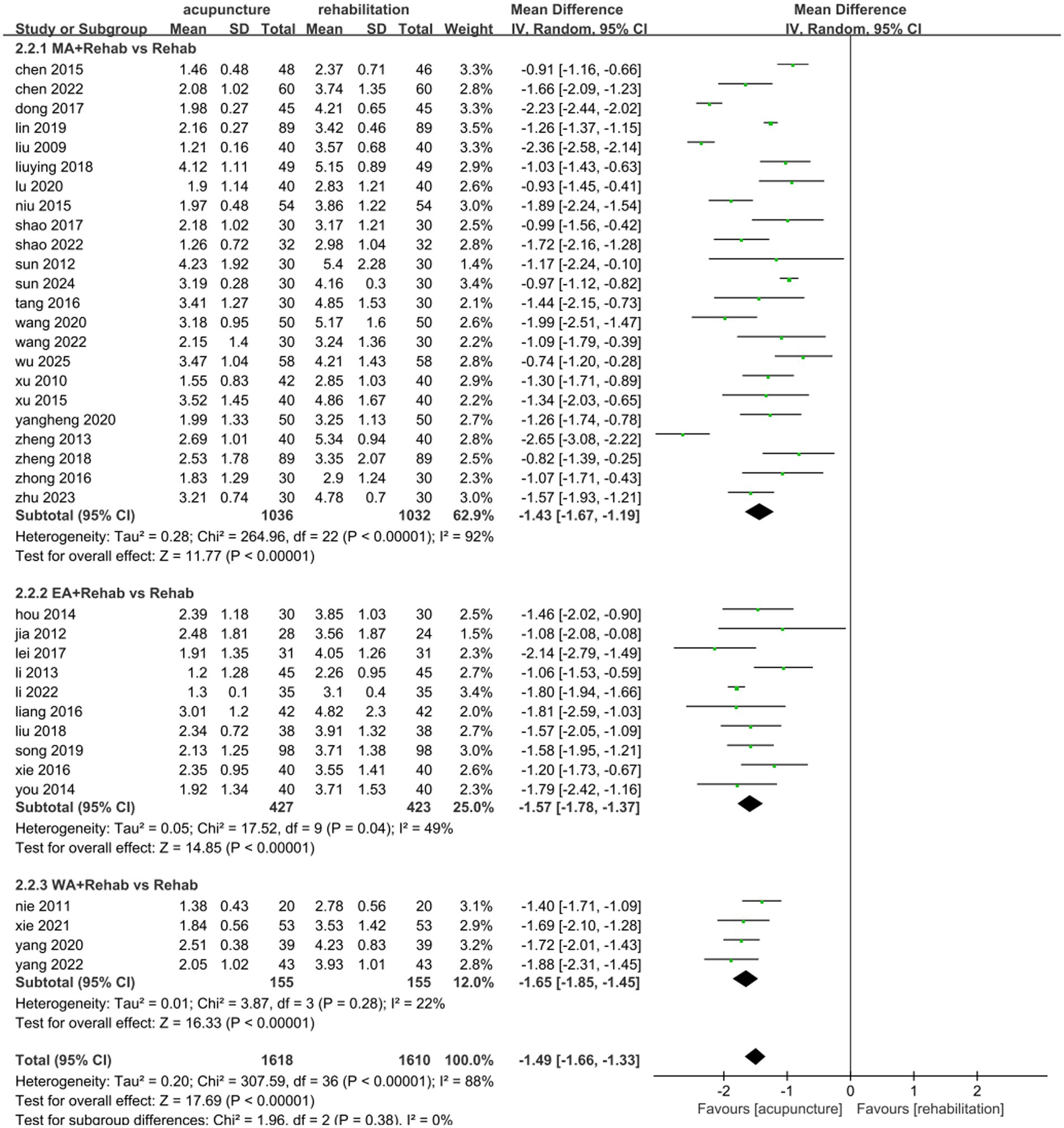
Figure 7. Forest plot of the intervention subgroup of acupuncture treatment combined with Rehab vs. Rehab on VAS.
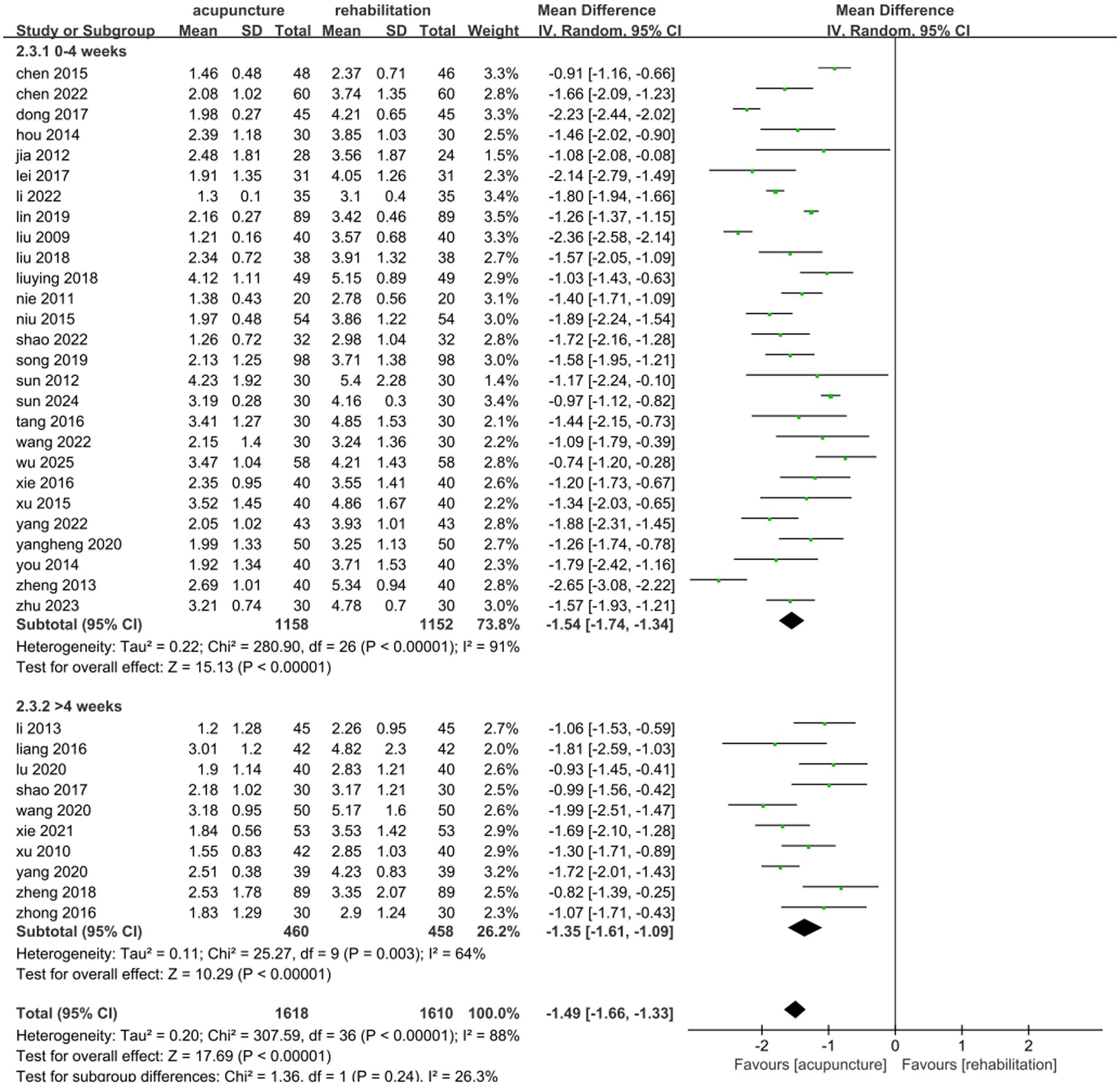
Figure 8. Forest plot of the treatment duration subgroup of acupuncture treatment combined with Rehab vs. on VAS.
A total of 1,585 patients across 17 studies (25, 28, 30, 35, 36, 38, 45, 47, 51, 53, 54, 57, 63–65, 68, 71) evaluated the effects of acupuncture combined with Rehab on ADL using the Barthel Index (BI) or modified Barthel Index (MBI). A random-effects model was applied due to significant heterogeneity (p < 0.00001, I2 = 94%). The meta-analysis demonstrated that acupuncture combined with Rehab significantly improved self-care ability compared to controls (MD: 10.94, 95% CI: 8.26–13.63, p < 0.00001, see Figure 9). Subgroup analyses by acupuncture modality revealed superior outcomes for manual acupuncture + Rehab (MD: 11.10, 95% CI: 7.20–15.00, p < 0.00001), electroacupuncture + Rehab (MD: 10.34, 95% CI: 4.93–15.74, p = 0.0002), and warm acupuncture + Rehab (MD: 11.55, 95% CI: 8.97–14.12, p < 0.00001, see Figure 10) over Rehab alone. Treatment duration subgroup analyses showed consistent benefits for acupuncture + Rehab across both short-term (0–4 weeks: MD: 10.19, 95% CI: 6.10–14.28, p < 0.0001) and extended periods (>4 weeks: MD: 12.37, 95% CI: 8.31–16.42, p < 0.0001, see Figure 11). The results of the sensitivity analysis showed that the exclusion of either study had little effect on the MD values of the pooled data, and we were unable to find a clear reason for the heterogeneity. Differences in acupoint selection, acupuncture retention time, and treatment frequency in the included studies may be potential reasons for the heterogeneity.
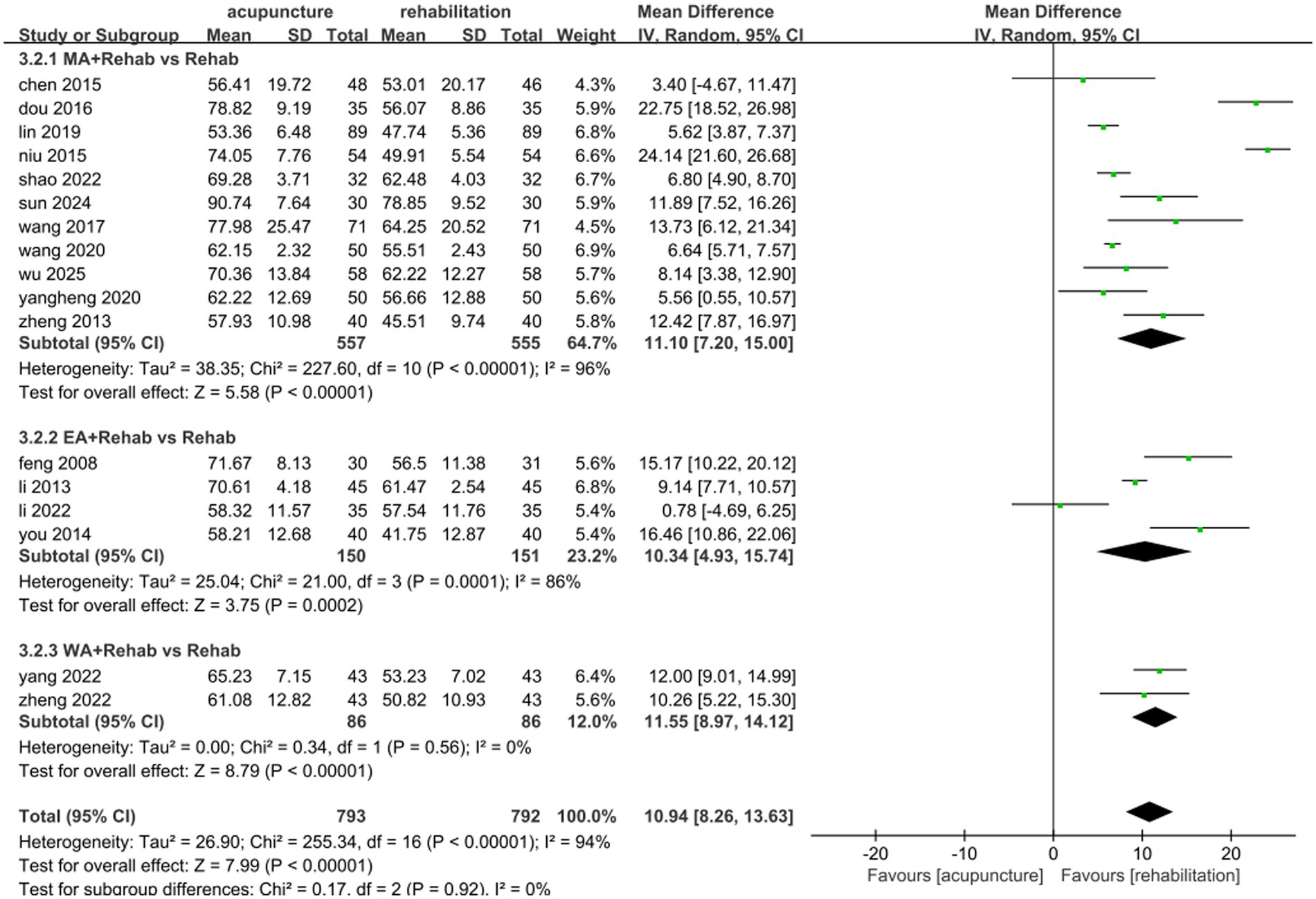
Figure 10. Forest plot of the intervention subgroup of acupuncture treatment combined with Rehab vs. Rehab on ADL. MA, manual acupuncture; Ea, electro-acupuncture; MA, warm acupuncture; Rehab, rehabilitation.
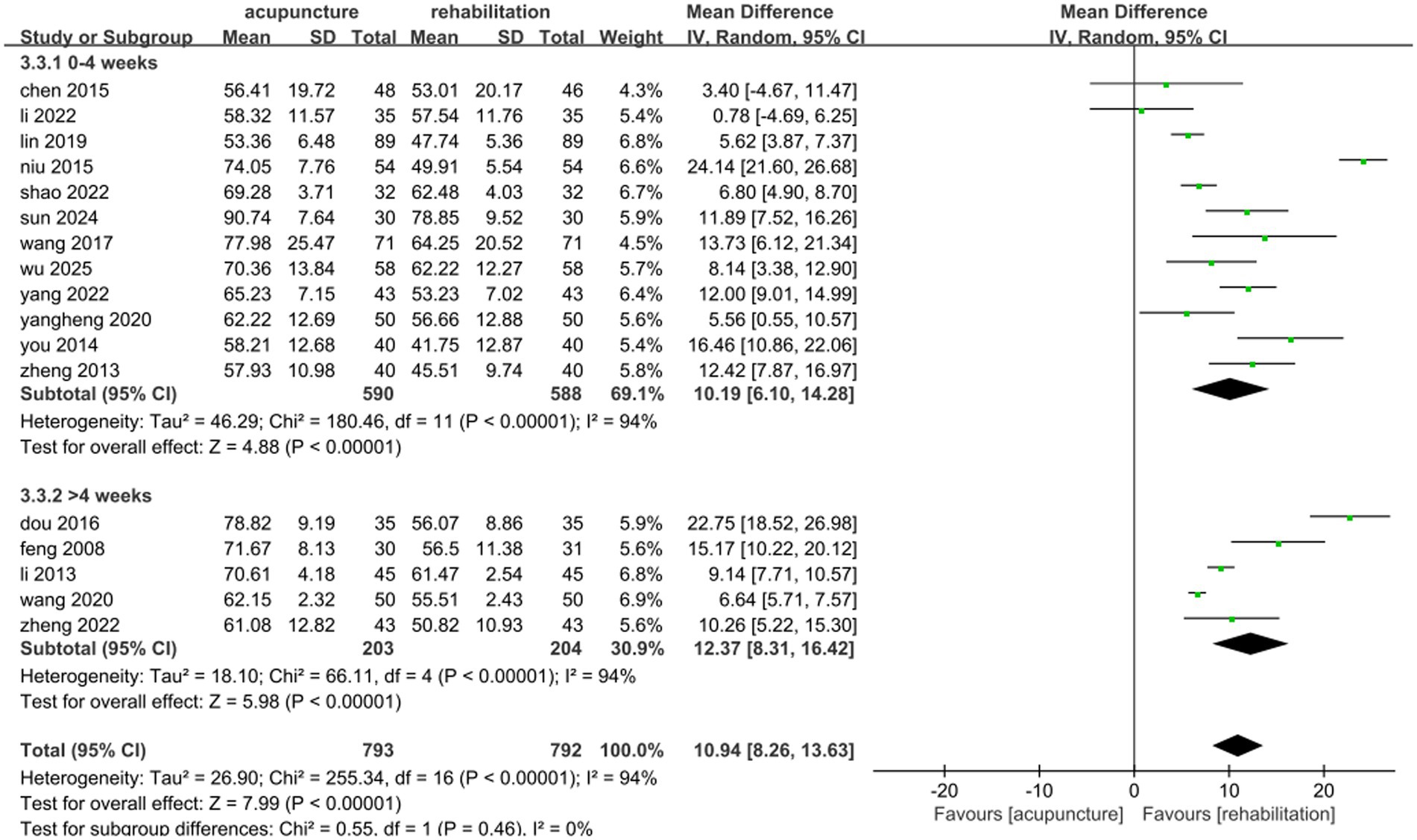
Figure 11. Forest plot of the treatment duration subgroup of acupuncture treatment combined with Rehab vs. on ADL.
Sufficient information on edema was detected in 476 patients with SHS across 4 studies (26, 43, 49, 61). A random-effects model analysis revealed a statistically significant difference between acupuncture therapy combined with Rehab and Rehab alone (MD: −0.65, 95% CI: [−0.93, −0.38], p < 0.00001; see Supplementary Figure 1). Subgroup analysis based on acupuncture methods demonstrated that MA combined with Rehab significantly reduced edema (MD: −0.55, 95% CI: [−0.94, −0.16], p < 0.00001; see Supplementary Figure 2). Further subgroup analysis stratified by treatment duration (0–4 weeks) showed similar results (MD: −0.76, 95% CI: [−1.52, −1.01], p < 0.00001; see Supplementary Figure 3). Heterogeneity in the MA + Rehab subgroup was notably reduced after excluding Chen (26), potentially attributed to variations in disease duration and acupoint selection. Xu (61) was a key source of heterogeneity in the 0–4 week subgroup, likely attributed to older participants and longer disease duration. After excluding this study, pooled results remained significantly in favor of acupuncture combined with Rehab (Supplementary Table 1).
By scanning 47 studies, we found that the majority of patients with adverse events were able to recover spontaneously without medical intervention. The verse events are described as follows: Three studies (26, 45, 60) reported no adverse events during the treatment period. Two studies (36, 54) reported two patients with subcutaneous hemorrhage, compression relief, and pain 5, redness 4, and pruritus 3. No adverse events were mentioned in the remaining studies. The data combined by fixed effects model showed that there was no significant difference in the occurrence of adverse reactions and Rehab (RR: 1.15, 95% CI:[0.42, 3.14], I2 = 0%, p = 0.78, see Supplementary Figure 4).
Funnel plot and Egger’s test were used to evaluate publication bias based on the FMA, VAS and ADL scales. The distribution of the funnel plot is asymmetric, with some studies exceeding the 95% confidence interval (see Supplementary Figures 5–7). Egger’s test showed no publication bias in the FMA (p = 0.126), VAS (p = 0.896), and ADL scales (p = 0.133) (see Supplementary Tables 2–4). The test results of the funnel plot show potential publication bias.
The strength of evidence for the above four scales was assessed as a ‘low’ level of certainty. Defects in the study design and considerable statistical heterogeneity were the main reasons for reduced evidence certainty (see Table 3).
In this systematic review, 47 randomized controlled trials involving 4,129 patients were included. Our findings from this review suggest that acupuncture therapy combined with Rehab benefits motor function (FMA), pain (VAS), and activities of daily living (ADL) in SHS patients. The subgroup analysis results showed no difference in the upper limb motor function improvement by manual acupuncture, electric acupuncture, and warm acupuncture (measured by FMA, VAS, and ADL). In terms of treatment duration, the results did not change with increasing treatment duration (as measured by FMA, VAS, and ADL). Two studies (36, 54) (4%) reported AEs related to acupuncture treatment, with the main AEs including subcutaneous hemorrhage, pain, itching, and redness. Sensitivity analysis showed that the effect of acupuncture combined with Rehab was robust to improving motor function, reducing pain and improving daily living ability in SHS patients. The included studies had methodological flaws and high heterogeneity, giving a “low” level of certainty of evidence.
The mechanism of acupuncture to relieve pain have been extensively studied. Modern neurological studies believe that the analgesic effect of acupuncture is mainly based on the effect of acupuncture on the nervous system and neurotransmitters. Acupuncture at acupuncture points plays an important role in the release of pain-reducing signaling molecules such as opioid peptides, glutamate and calcium adenosine (72). Acupuncture treatment can effectively regulate the levels of pro-inflammatory and anti-inflammatory factors TNF-A, IL-13 and IL-6, and can also reduce the inflammatory immune response and effectively relieve pain by inhibiting the NLRP 3 inflammasome and its inflammatory factors Caspase-1 and IL-13 (73, 74). Numerous studies have shown that phosphorylation of ipsilateral extracellular signal-regulated kinases (ERKs) and subsequent CREB activation, and various calmodulin kinases such as CamKV and cAMP/protein kinase A (PKA) transfer to neurons and regulate the activity of transcriptional regulators. It is suggested that acupuncture may lead to changes in neuronal and synaptic morphological structures that may affect the plasticity of hippocampal synapses (75). In motor function, acupuncture mainly by adjusting the bilateral motor cortex, auxiliary motor area, central back, the pole, lingual gyrus, cerebellum, frontal gyrus, and the precuneus area function connection, adjust the left prefrontal network, default mode network and sensorimotor network connection conduction mode, change the network between information input and output way, thus improving patients motor function (76–78). Currently, there is no consensus on the mechanism of action of acupuncture for SHS or CRPS, so how acupuncture affects sympathetic/somatic nervous system dysfunction needs further investigation.
However, before applying the study results to clinical practice, we must consider some of the limitations in this review. First, although 47 RCTs items were ultimately included in the mate analysis, the random sequence generation method for most studies was ambiguous, the lack of blindness among participants and operators, and blind uncertainty among outcome assessors. Specifically, 40.4% of the studies did not explicitly address the method for random sequence generation. None of the RCTs implemented allocation concealment. Participants and acupuncturists were not blinded in any of the studies. Blinding of outcome assessors in all studies was assessed as an “unclear” risk of bias because of a lack of information. These factors will inevitably lead to a degree of selection bias, detection bias, and reporting bias. Second, another limitation is the high degree of heterogeneity between the included studies. Although we sought to identify the cause of high heterogeneity by subgroup analysis and sensitivity analysis, acupuncture, as a complex treatment, may itself be a source of heterogeneity. In order to maximize the benefits from acupuncture treatment, we need to consider a combination of factors such as the choice and combination of acupuncture points, the depth and retention time of needles, and the duration and frequency of treatment. Although we grouped the studies by acupuncture modality and treatment duration, these parameters were still variable, and we were unable to accurately and reliably determine the reasons for the significant heterogeneity. Therefore, future experimental studies should elaborate on the acupuncture protocol to further improve the reporting completeness. Furthermore, variability in the skill level of acupuncture therapists can also have an impact on treatment outcomes. The variability of these factors may be responsible for the high heterogeneity. These two limitations are the main reasons for the lower level of evidence in this review. Furthermore, most of the studies in this review were published and only one study was published in the English database. Therefore, the superior efficacy of acupuncture for SHS over rehabilitation needs to be interpreted cautiously in China. Patients with SHS have a long-term recovery period, but all studies used short-term prognostic indicators and lack long-term follow-up of patients. Therefore, the long-term efficacy of acupuncture for SHS needs to be further explored. Furthermore, we should note that in this review, outcome measures such as FMA, VAS and ADL were used as screening tools for recovery in SHS patients rather than as a comprehensive assessment of symptom relief. A further limitation is that the severity of SHS patient staging was not clearly defined according to the inclusion criteria. Therefore, it is suggested that future studies can be conducted in specific areas to provide more definite and high-quality evidence for the efficacy of acupuncture for SHS. Finally, among the 47 included studies, three studies reported no adverse events during acupuncture treatment, and two studies reported mild adverse events in 16 patients. Acupuncture treatment appears to be relatively safe and does not cause serious AEs.
Due to the unique geographical characteristics of acupuncture treatment, we had to look for RCTs related to acupuncture treatment as comprehensively as possible in Chinese journals. All of the studies included in this review were conducted at the Chinese mainland. Further studies should be conducted around the world to involve more ethnic and culturally diverse populations. However, we note that the vast majority of studies published in Chinese databases suffer from experimental design flaws. In order to truly effectively evaluate the efficacy of acupuncture for SHS and to provide high quality evidence for clinical practice, future studies need to be more rigorous in experimental design and methodology. As a non-pharmacological intervention, acupuncture therapists need to choose different acupoints for treatment in clinical practice, which makes it difficult to achieve operator blinding. However, we could achieve blinding to participants by sham or placebo acupuncture to reduce the occurrence of bias. Furthermore, blinding of the outcome assessors is also feasible and necessary.
This systematic review suggests that the addition of acupuncture treatment in rehabilitation training may have a positive effect on improving motor function, reducing pain and improving daily life in SHS patients with SHS. However, due to the methodological limitations of the included studies, this evidence was graded as “low ‘, and the results should be treated with caution. Future clinical studies should use a high-quality randomized, double-blind controlled trial design. Meanwhile, long-term follow-up and efficacy assessment and clinical studies with large-scale multicenter sample sizes are highly desirable.
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding author.
JS: Data curation, Writing – original draft. FC: Methodology, Writing – review & editing. YL: Resources, Writing – review & editing. MB: Conceptualization, Writing – original draft. XS: Supervision, Writing – original draft. RR: Investigation, Writing – original draft. SL: Software, Writing – review & editing.
The author(s) declare that financial support was received for the research and/or publication of this article. This work was supported by the Qinghai Provincial Health Commission Guidance Plan Research Project (No. 2024-wjzdx-24).
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
The authors declare that no Gen AI was used in the creation of this manuscript.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
The Supplementary material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fneur.2025.1488767/full#supplementary-material
SUPPLEMENTARY FIGURE 1 | Forest plot of acupuncture treatment combined with Rehab vs. Rehab on Edema.
SUPPLEMENTARY FIGURE 2 | Forest plot of the intervention subgroup of acupuncture treatment combined with Rehab vs. Rehab on Edema MA, manual acupuncture; EA, electro-acupuncture; Rehab, rehabilitation.
SUPPLEMENTARY FIGURE 3 | Forest plot of the treatment duration subgroup of acupuncture treatment combined with Rehab vs. on Edema.
SUPPLEMENTARY FIGURE 4 | The forest plot of acupuncture treatment combined with Rehab vs. Rehab on the incidence of adverse events.
SUPPLEMENTARY FIGURE 5 | The funnel plot of FMA.
SUPPLEMENTARY FIGURE 6 | The funnel plot of VAS.
SUPPLEMENTARY FIGURE 7 | The funnel plot of ADL.
1. Herpich, F, and Rincon, F. Management of acute ischemic stroke. Crit Care Med. (2020) 48:1654–63. doi: 10.1097/CCM.0000000000004597
2. Kim, JY, Yoon, SY, Kim, J, Jeong, YH, and Kim, YW. Neural substrates for poststroke complex regional pain syndrome type I: a retrospective case-control study using voxel-based lesion symptom mapping analysis. Pain. (2020) 161:1311–20. doi: 10.1097/j.pain.0000000000001816
3. Pertoldi, S, and Di Benedetto, P. Shoulder-hand syndrome after stroke. A complex regional pain syndrome. Eura Medicophys. (2005) 41:283–92.
4. Misidou, C, and Papagoras, C. Complex regional pain syndrome: an update. Mediterr J Rheumatol. (2019) 30:16–25. doi: 10.31138/mjr.30.1.16
5. Matayoshi, S, Shimodozono, M, Hirata, Y, Ueda, T, Horio, S, and Kawahira, K. Use of calcitonin to prevent complex regional pain syndrome type I in severe hemiplegic patients after stroke. Disabil Rehabil. (2009) 31:1773–9. doi: 10.1080/09638280902795573
6. Zhan, J, Ai, Y, Zhan, L, Pan, R, Wang, Y, Dong, C, et al. Effect of abdominal acupuncture combined with routine rehabilitation training on shoulder-hand syndrome after stroke: a randomized controlled trial. Integr Med Res. (2022) 11:100805. doi: 10.1016/j.imr.2021.100805
7. Zhang, XL, Tang, CZ, and Jia, J. Analysis of the current status of Chinese and Western medical treatment of post-stroke shoulder-hand syndrome. Chin J Rehabil Med. (2015) 30:294–8.
8. Turner-Stokes, L, and Goebel, A. Complex regional pain syndrome in adults: concise guidance. Clin Med. (2011) 11:596–600. doi: 10.7861/clinmedicine.11-6-596
9. Kalita, J, Vajpayee, A, and Misra, UK. Comparison of prednisolone with piroxicam in complex regional pain syndrome following stroke: a randomized controlled trial. QJM. (2006) 99:89–95. doi: 10.1093/qjmed/hcl004
10. O'Connell, NE, Wand, BM, McAuley, J, Marston, L, and Moseley, GL. Interventions for treating pain and disability in adults with complex regional pain syndrome. Cochrane Database Syst Rev. (2013) 2013:CD009416. doi: 10.1002/14651858.CD009416.pub2
11. Forouzanfar, T, Köke, AJ, van Kleef, M, and Weber, WE. Treatment of complex regional pain syndrome type I. Eur J Pain. (2002) 6:105–22. doi: 10.1053/eujp.2001.0304
12. Zhuang, Y, Xing, JJ, Li, J, Zeng, BY, and Liang, FR. History of acupuncture research. Int Rev Neurobiol. (2013) 111:1–23. doi: 10.1016/b978-0-12-411545-3.00001-8
13. Witt, CM, Pach, D, Reinhold, T, Wruck, K, Brinkhaus, B, Mank, S, et al. Treatment of the adverse effects from acupuncture and their economic impact: a prospective study in 73,406 patients with low back or neck pain. Eur J Pain. (2011) 15:193–7. doi: 10.1016/j.ejpain.2010.06.008
14. Berman, BM, Langevin, HM, Witt, CM, and Dubner, R. Acupuncture for chronic low back pain. N Engl J Med. (2010) 363:454–61. doi: 10.1056/NEJMct0806114
15. Kim, KH, Lee, MS, Kim, TH, Kang, JW, Choi, TY, and Lee, JD. Acupuncture and related interventions for symptoms of chronic kidney disease. Cochrane Database Syst Rev. (2016) 2016:CD009440. doi: 10.1002/14651858.CD009440.pub2
16. Burke, A, Upchurch, DM, Dye, C, and Chyu, L. Acupuncture use in the United States: findings from the National Health Interview Survey. J Altern Complement Med. (2006) 12:639–48. doi: 10.1089/acm.2006.12.639
17. Li, L, Li, J, and He, M. Treatment outcomes in post-stroke shoulder-hand syndrome: the role of combined acupuncture, traditional Chinese herb hot compress and rehabilitation training. J Back Musculoskelet Rehabil. (2024) 37:1023–30. doi: 10.3233/BMR-230267
18. Peng, L, Zhang, C, Zhou, L, Zuo, HX, He, XK, and Niu, YM. Traditional manual acupuncture combined with rehabilitation therapy for shoulder hand syndrome after stroke within the Chinese healthcare system: a systematic review and meta-analysis. Clin Rehabil. (2018) 32:429–39. doi: 10.1177/0269215517729528
19. Wei, X, He, L, Liu, J, Ai, Y, Liu, Y, Yang, Y, et al. Electroacupuncture for reflex sympathetic dystrophy after stroke: a Meta-analysis. J Stroke Cerebrovasc Dis. (2019) 28:1388–99. doi: 10.1016/j.jstrokecerebrovasdis.2019.02.010
20. Liu, S, Zhang, CS, Cai, Y, Guo, X, Zhang, AL, Xue, CC, et al. Acupuncture for post-stroke shoulder-hand syndrome: a systematic review and Meta-analysis. Front Neurol. (2019) 10:433. doi: 10.3389/fneur.2019.00433
21. Wang, M, Wang, PQ, Yu, LH, Wang, CY, and Shao, Y. Post-stroke shoulder-hand syndrome of phlegm-stasis obstruction treated with the combined therapy of eye acupuncture, Tengliao and rehabilitation training: a multi-central randomized controlled trial. Zhongguo Zhen Jiu. (2022) 42:385–9. doi: 10.13703/j.0255-2930.20210426-0003
22. Moher, D, Liberati, A, Tetzlaff, J, and Altman, DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. (2009) 6:e1000097. doi: 10.1371/journal.pmed.1000097
23. Sterne, JAC, Savović, J, Page, MJ, Elbers, RG, Blencowe, NS, Boutron, I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. (2019) 366:l4898. doi: 10.1136/bmj.l4898
24. Guyatt, GH, Oxman, AD, Vist, GE, Kunz, R, Falck-Ytter, Y, Alonso-Coello, P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. (2008) 336:924–6. doi: 10.1136/bmj.39489.470347.AD
25. Chen, Y, Huang, T, and Liu, K. Acupuncture combined with rehabilitation training in the treatment of shoulder-hand syndrome after stroke: a phase I clinical study. J Sichuan Tradit Chin Med. (2015) 33:150–2.
26. Chen, H, and Guan, F. Clinical effect of acupuncture combined with rehabilitation therapy in the treatment of shoulder-hand syndrome after ischemic stroke. Chin Med Herald. (2022) 19:27. doi: 10.20047/j.issn1673-7210.2022.02.027
27. Dong, J, Yang, X, Zheng, D, Li, D, and Xue, X. A randomized controlled study of cephalic and somatic needle mu-prick method combined with rehabilitation training in the treatment of post-stroke shoulder-hand syndrome. J Chengdu Univ Tradit Chin Med. (2017) 40:40–3. doi: 10.13593/j.cnki.51-1501/r.2017.01.040
28. Dou, Z . The efficacy of acupuncture with rehabilitation training to improve the pain and edema of shoulder-hand syndrome after stroke. Tradit Chin Med Rehabil. (2016) 7:29–30.
29. Fang, T, and Cao, X. Clinical study on 45 cases of phase I shoulder-hand syndrome after stroke treated with head acupuncture plus body acupuncture penetration method. J Shaanxi Univ Chin Med. (2021) 44:89–92. doi: 10.13424/j.cnki.jsctcm.2021.01.015
30. Feng, X . Clinical efficacy of integrated therapy on 60 cases of patients with shoulder-hand syndrome after stroke. Chin J Pract Nerv Dis. (2008) 2008:76–7. doi: 10.3969/j.issn.1673-5110.2008.04.041
31. Hou, Z . Evaluation of the efficacy of rehabilitation training combined with acupuncture in the treatment of post-stroke shoulder-hand syndrome stage I. J Clin Med Pract. (2014) 18:2018. doi: 10.7619/jcmp.201405018
32. Huang, L, Qian, L, and Li, J. Clinical observation on 80 cases of shoulder-hand syndrome after stroke treated with warm acupuncture and moxibustion combined with exercise therapy. Chin J Tradit Med Sci Technol. (2017) 24:328–9.
33. Jia, C, Ni, G, Tan, H, and Zhang, X. Clinical efficacy of rehabilitation training combined with acupuncture in the treatment of post-stroke shoulder-hand syndrome in stage I. J Changchun Univ Chin Med. (2012) 28:711–2. doi: 10.13463/j.cnki.cczyy.2012.04.084
34. Lei, B, Zhang, J, and Qin, G. Therapeutic effect of electroacupuncture combined with rehabilitation training in the treatment of shoulder-hand syndrome after stroke. Tradit Chin Med Rehabil. (2017) 8:24. doi: 10.19787/j.issn.1008-1879.2017.08.010
35. Li, F, and Tu, M. Observations on the efficacy of occupational therapy with electroacupuncture in the treatment of phase I shoulder-hand syndrome after stroke. Chin J Pharm Econ. (2013) 2013:370–1.
36. Li, S, and Li, F. The efficacy of electroacupuncture combined with upper limb rehabilitation training in the treatment of post-stroke shoulder-hand syndrome. Clin J Chin Med. (2022) 14:58–62. doi: 10.3969/j.issn.1674-7860.2022.16.017
37. Liang, N, and Liu, X. Clinical efficacy of electroacupuncture combined with rehabilitation training in the treatment of shoulder-hand syndrome after stroke. Guide Chin Med. (2016) 14:200–1. doi: 10.15912/j.cnki.gocm.2016.25.163
38. Lin, B . Observation on the therapeutic effect of eight-evil penetration with systematic rehabilitation training in the treatment of shoulder-hand syndrome after hemiplegia with stroke. West J Tradit Chin Med. (2019) 32:108–12. doi: 10.3969/j.issn.1004-6852.2019.05.031
39. Liu, Y . Clinical study on the treatment of shoulder-hand syndrome by mu-pricking shoulder pain points combined with rehabilitation training. Gansu Med J. (2009) 28:176–8. doi: 10.15975/j.cnki.gsyy.2009.03.002
40. Liu, H . Clinical efficacy of rehabilitation training combined with acupuncture in the treatment of post-stroke shoulder-hand syndrome stage I. Guide Chin Med. (2018) 16:147–8. doi: 10.15912/j.cnki.gocm.2018.16.107
41. Liu, Y, and Jiao, H. Study on the efficacy of acupuncture combined with rehabilitation training in patients with acute phase of shoulder-hand syndrome after stroke. J Hunan Univ Chin Med. (2018) 38:546–9. doi: 10.3969/j.issn.1674-070X.2018.05.015
42. Liu, X . Effects of acupuncture and moxibustion adjuvant therapy on limb function and psychological status of patients with shoulder-hand syndrome due to stroke. Psychol Mon. (2021) 16:34. doi: 10.19738/j.cnki.psy.2021.13.034
43. Lu, M, Liu, L, Wang, P, and Zhuang, C. Xingnao Kaiqiao acupuncture combined with rehabilitation training for post-stroke shoulder-hand syndrome: a clinical study of 40 cases. Tradit Chin Med Res. (2020) 33:51–4. doi: 10.3969/j.issn.1001-6910.2020.07.19
44. Nie, W, and Zhao, H. Clinical observation of warming and unblocking the triple burner method combined with rehabilitation training for shoulder-hand syndrome. Shanghai J Acupunct Moxibust. (2011) 30:217–9. doi: 10.3969/j.issn.1005-0957.2011.04.217
45. Niu, G . Clinical study of rehabilitation training combined with acupuncture for shoulder-hand syndrome. Henan Tradit Chin Med. (2015) 35:2846–7. doi: 10.16367/j.issn.1003-5028.2015.11.1220
46. Shao, Y, Tan, T, Zhang, P, and Yang, T. Efficacy observation of shoulder three-needle therapy combined with Bobath therapy for post-stroke shoulder-hand syndrome. Zhejiang J Integr Tradit West Med. (2017) 27:584–6. doi: 10.3969/j.issn.1005-4561.2017.07.015
47. Shao, B, Wang, J, Jin, X, Chen, L, Zhang, D, and Chen, J. Clinical observation of "Fuzheng Butu" acupuncture combined with conventional rehabilitation training for post-stroke shoulder-hand syndrome with qi deficiency pattern: a study of 32 cases. J Gansu Univ Chin Med. (2022) 29:82–7. doi: 10.16841/j.issn1003-8450.2022.04.15
48. Shen, Z . Efficacy observation of acupuncture combined with rehabilitation training for shoulder-hand syndrome. Shenzhen J Integr Tradit West Med. (2014) 24:56–8. doi: 10.16458/j.cnki.1007-0893.2014.08.007
49. Song, Y, and Xie, G. Efficacy observation of Electroacupuncture combined with Tuina rehabilitation training for stage I shoulder-hand syndrome after ischemic stroke. Shanghai J Acupunct Moxibust. (2019) 38:487–91. doi: 10.13460/j.issn.1005-0957.2019.05.0487
50. Sun, Y, Wang, Y, Wang, W, and Hong, Y. Effect of acupuncture plus rehabilitation training on shoulder-hand syndrome due to ischemic stroke. J Acupunct Tuina Sci. (2012) 10:109–13. doi: 10.1007/s11726-012-0583-z
51. Sun, H, and Tu, Q. Clinical observation of Xingnao Kaiqiao acupuncture combined with comprehensive rehabilitation training for stage I shoulder-hand syndrome after ischemic stroke. J Pract Tradit Chin Med. (2024) 40:355–8.
52. Tang, D, Wu, W, and Sun, X. Randomized controlled trial of Meridian-unblocking acupuncture combined with functional training for post-cerebral infarction shoulder-hand syndrome. J Clin Acupunct Moxibust. (2016) 32:26–9. doi: 10.19917/j.cnki.1005-0779.2016.01.009
53. Wang, X, Gao, Y, and Gao, S. Effects of acupuncture combined with rehabilitation training on PRI, FMA, and MBI scores in patients with post-stroke shoulder-hand syndrome. Glob Tradit Chin Med. (2017) 10:361–3. doi: 10.3969/j.issn.1674-1749.2017.03.033
54. Wang, L, Wang, K, Wang, F, Li, R, Wang, J, and Li, Y. Effects of comprehensive rehabilitation training combined with acupuncture at Yanglao (SI6) on Hemorheology and activities of daily living in post-stroke shoulder-hand syndrome patients with yin deficiency and Yang hyperactivity syndrome and Meridian stasis pattern. Hebei. J Tradit Chin Med. (2020) 42:21. doi: 10.3969/j.issn.1002-2619.2020.07.021
55. Wang, Q, and Li, H. The impact of acupuncture on pain and comprehensive function in patients with post-stroke shoulder-hand syndrome. J Hubei Univ Chin Med. (2022) 24:94–6. doi: 10.3969/j.issn.1008-987x.2022.04.27
56. Wen, J, and Zhang, L. Observation on the clinical treatment of 30 cases with post-stroke shoulder-hand syndrome using the method of regulating Spirit and unblocking meridians combined with rehabilitation training. Jiangsu J Tradit Chin Med. (2009) 41:55–6. doi: 10.3969/j.issn.1672-397X.2009.08.037
57. Wu, R, Huang, F, Liu, C, and Jiang, Z. The impact of Acupoint needling in awakening brain, initiating opening and closing, and adjusting pivot method on upper limb functional recovery and VAS, MBI scores in elderly patients with shoulder-hand syndrome after stroke. Chin J Gerontol. (2025) 45:85–8.
58. Xie, J, and Li, J. Observation on the efficacy of Electroacupuncture combined with rehabilitation training in the treatment of shoulder-hand syndrome after stroke. Shanghai J Acupunct Moxibust. (2016) 35:1423–5. doi: 10.13460/j.issn.1005-0957.2016.12.1423
59. Xie, Y, Cao, Y, Su, T, and Yang, W. Clinical observation on the treatment of shoulder-hand syndrome after stroke using warm acupuncture combined with rehabilitation therapy. Mod Chin Med. (2021) 41:103–7. doi: 10.13424/j.cnki.mtcm.2021.04.024
60. Xu, S, Zhuang, L, Jia, C, Xu, D, and Pan, C. Clinical observation on the treatment of shoulder-hand syndrome following hemiplegia after stroke using the Jin's three needle therapy combined with functional training. J Guangzhou Univ Tradit Chin Med. (2010) 27:19–22. doi: 10.13359/j.cnki.gzxbtcm.2010.01.009
61. Xu, F, Li, H, and Zhang, Q. Randomized controlled study on the treatment of shoulder-hand syndrome after ischemic stroke using acupuncture combined with rehabilitation training. Chin J Trauma Disabil Med. (2015) 23:141–2. doi: 10.13214/j.cnki.cjotadm.2015.16.107
62. Yang, X, Tian, F, Ying, Q, and Zheng, Q. Observation on the efficacy of Electroacupuncture combined with warm acupuncture in the treatment of shoulder-hand syndrome after stroke. J Emerg Tradit Chin Med. (2020) 29:329–32. doi: 10.3969/j.issn.1004-745X.2020.02.041
63. Yang, H . Intervention study of acupuncture combined with rehabilitation training on pain and edema in post-stroke shoulder-hand syndrome. Reflexol Rehabil Med. (2020) 2020:60–2.
64. You, Y . Observation on the efficacy of Electroacupuncture sparse-dense wave combined with occupational therapy for shoulder-hand syndrome after stroke. Chin J Convalescent Med. (2014) 23:509–11. doi: 10.13517/j.cnki.ccm.2014.06.016
65. Zheng, S, Wu, Y, Chang, J, Cui, S, Xu, M, Lian, J, et al. Efficacy observation of Chifeng Yingyuan acupuncture for post-stroke shoulder-hand syndrome. Chin J Rehabil. (2013) 28:40–1. doi: 10.3870/zgkf.2013.01.015
66. Zhang, Z, Tao, L, Ma, X, Zeng, M, and Zhu, M. Clinical study on the treatment of stage I shoulder-hand syndrome after stroke using Electroacupuncture combined with upper limb rehabilitation training. New Chin Med. (2024) 56:125–8. doi: 10.13457/j.cnki.jncm.2024.07.025
67. Zheng, J, Wu, Q, Wang, L, and Guo, T. A clinical study on acupuncture in combination with routine rehabilitation therapy for early pain recovery of post-stroke shoulder-hand syndrome. Exp Ther Med. (2018) 15:2049–53. doi: 10.3892/etm.2017.5659
68. Zheng, C . The impact of warm acupuncture combined with massage techniques on clinical efficacy and upper limb function in patients with shoulder-hand syndrome after stroke. Smart Health. (2022) 8:186–9. doi: 10.19335/j.cnki.2096-1219.2022.35.043
69. Zhong, C, Ni, D, Lin, W, and Chen, F. Observation on the efficacy of acupuncture combined with rehabilitation training in the treatment of shoulder-hand syndrome after stroke. Hainan Med J. (2016) 27:1687–8. doi: 10.3969/j.issn.1003-6350.2016.10.048
70. Zhu, Z, and Zhou, W. Clinical observation of Canggui Tanxue acupuncture combined with rehabilitation training for stage I post-stroke shoulder-hand syndrome. Guangzhou Med J. (2023) 54:25–9.
71. Yang, C . Study on the therapeutic effects of acupuncture treatment combined with rehabilitation training on shoulder-hand syndrome following hemiplegia. Med Health. (2022) 2022:296–9.
72. Yang, ES, Li, PW, Nilius, B, and Li, G. Ancient Chinese medicine and mechanistic evidence of acupuncture physiology. Pflugers Arch. (2011) 462:645–53. doi: 10.1007/s00424-011-1017-3
73. Li, N, Guo, Y, Gong, Y, Zhang, Y, Fan, W, Yao, K, et al. The anti-inflammatory actions and mechanisms of acupuncture from Acupoint to target organs via neuro-immune regulation. J Inflamm Res. (2021) 14:7191–224. doi: 10.2147/JIR.S341581
74. Wu, Z, and Liu, Q. Effects of repetitive transcranial magnetic stimulation combined with acupuncture on NLRP3 inflammasome and protease levels in patients with neuropathic pain. Am J Transl Res. (2023) 15:4699–708.
75. Tyrtyshnaia, A, and Manzhulo, I. Neuropathic pain causes memory deficits and dendrite tree morphology changes in mouse Hippocampus. J Pain Res. (2020) 13:345–54. doi: 10.2147/JPR.S238458
76. Li, Y, Wang, Y, Liao, C, Huang, W, and Wu, P. Longitudinal brain functional connectivity changes of the cortical motor-related network in subcortical stroke patients with acupuncture treatment. Neural Plast. (2017) 2017:5816263–9. doi: 10.1155/2017/5816263
77. Chen, X, Zhang, H, and Zou, Y. A functional magnetic resonance imaging study on the effect of acupuncture at GB34 (Yanglingquan) on motor-related network in hemiplegic patients. Brain Res. (2015) 1601:64–72. doi: 10.1016/j.brainres.2015.01.011
Keywords: acupuncture treatment, post-stroke shoulder-hand syndrome, meta-analysis, rehabilitation, non-pharmacological
Citation: Shi J, Chen F, Liu Y, Bian M, Sun X, Rong R and Liu S (2025) Acupuncture versus rehabilitation for post-stroke shoulder-hand syndrome: a systematic review and meta-analysis of randomized controlled trials. Front. Neurol. 16:1488767. doi: 10.3389/fneur.2025.1488767
Received: 20 November 2024; Accepted: 18 March 2025;
Published: 02 April 2025.
Edited by:
Leonardo Pellicciari, IRCCS Institute of Neurological Sciences of Bologna (ISNB), ItalyReviewed by:
Xun Luo, Kerry Rehabilitation Medicine Research Institute, ChinaCopyright © 2025 Shi, Chen, Liu, Bian, Sun, Rong and Liu. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Fuyan Chen, ZWNmeV8yMDA1QDE2My5jb20=
‡Present address: Fuyan Chen,Qinghai Provincial Hospital of Traditional Chinese Medicine, Xining, China
†These authors have contributed equally to this work and share first authorship
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.