
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
CASE REPORT article
Front. Med. , 11 March 2025
Sec. Infectious Diseases: Pathogenesis and Therapy
Volume 12 - 2025 | https://doi.org/10.3389/fmed.2025.1496961
 Yudai Tanaka1,2†
Yudai Tanaka1,2† Koji Hayashi1*†
Koji Hayashi1*† Ei Kawahara3
Ei Kawahara3 Shin-Ichiro Azuma4
Shin-Ichiro Azuma4 Maho Hayashi4
Maho Hayashi4 Yuka Nakaya1
Yuka Nakaya1 Asuka Suzuki1
Asuka Suzuki1 Midori Ueda1
Midori Ueda1 Rei Asano1
Rei Asano1 Hiromi Hayashi1
Hiromi Hayashi1 Toyoaki Miura1
Toyoaki Miura1 Kouji Hayashi5
Kouji Hayashi5 Mamiko Sato1,5
Mamiko Sato1,5 Yasutaka Kobayashi5
Yasutaka Kobayashi5Background: Sepsis can lead to life-threatening complications such as hemophagocytic lymphohistiocytosis (HLH) and bilateral adrenal hemorrhage (BAH), commonly known as Waterhouse-Friderichsen syndrome. HLH involves severe inflammation and organ damage, often linked with infections and autoimmune diseases, while BAH leads to adrenal insufficiency, typically caused by Neisseria meningitidis, though Escherichia coli (E. coli) is a rare cause.
Case presentation: A 27-year-old Japanese woman, with a history of diabetes mellitus and obesity, presented with a complicated urinary tract infection. She commenced oral levofloxacin treatment five days before hospital admission. Her medications included prednisolone 5 mg/day, trimethoprim-sulfamethoxazole for pyoderma gangrenosum, and oral hypoglycemic agents. Upon admission, her vital signs, including body temperature and blood pressure, were stable, and her body mass index was recorded at 49.8. Laboratory tests indicated elevated white blood cell count and C-reactive protein. She was diagnosed with a urinary tract infection and was treated with levofloxacin and trimethoprim-sulfamethoxazole. On day 16 of hospitalization, her general condition rapidly worsened, leading to her sudden death on day 18. Premortem blood tests showed cytopenia, and blood cultures tested positive for E. coli. Autopsy imaging using computed tomography revealed enlargement and high density of the left adrenal gland. Postmortem pathology identified bilateral adrenal hemorrhages with focal necrosis. Extensive erythrophagocytic macrophages were observed in the bone marrow, spleen, and liver. Disseminated intravascular coagulopathy was confirmed through the detection of a renal glomerular fibrin thrombus.
Conclusion: We concluded that E. coli infection had caused multiple fatal conditions, such as disseminated intravascular coagulopathy, bilateral adrenal hemorrhage, and suspected hemophagocytic lymphohistiocytosis leading to the death of the young woman.
Sepsis, recognized as a life-threatening organ dysfunction, arises from a dysregulated host response to infection (1). This condition can lead to a range of severe complications, one notable example being hemophagocytic lymphohistiocytosis (HLH). HLH is a fatal inflammatory syndrome that is pathologically characterized by extensive hemophagocytic activity by macrophages in various organs (2–4). While HLH in children predominantly occurs as a familial disorder, adult-onset HLH is typically associated with various underlying conditions such as viral infections, lymphoproliferative diseases, and autoimmune disorders (5, 6). HLH caused by bacterial infection is less common (5, 6), and HLH secondary to Escherichia coli (E. coli) infection is rarely reported (7, 8).
Bilateral adrenal hemorrhage (BAH), classically known as Waterhouse-Friderichsen syndrome, was initially described by Rupert Waterhouse in 1911 and Carl Friderichsen in 1918 (9). BAH is a rare syndrome associated with adrenal insufficiency that can occasionally become life-threatening. It is linked to a spectrum of infectious and non-infectious conditions (9, 10). The most commonly identified infectious agent is Neisseria meningitidis (10), as initially noted by Friderichsen (9). Nonetheless, a variety of bacteria have been implicated in the etiology of this syndrome (9), with E. coli-related instances being notably rare (11, 12).
In the present case, we report that the postmortem pathological examinations show the unusual co-occurrence of BAH and hemophagocytosis in the reticuloendothelial system as complications in the progression of sepsis, instigated by an infection with the widely encountered bacterium, E. coli.
A 27-year-old Japanese woman, with a history of diabetes mellitus and obesity, and previous diagnosis of a complicated urinary tract infection (UTI) based on an elevated serum inflammatory response and bacteriuria, was prescribed oral levofloxacin, which had been initiated 5 days prior to admission. Her medical history included long-term treatment with prednisolone, trimethoprim-sulfamethoxazole for pyoderma gangrenosum and oral hypoglycemic agents such as biguanides, SGLT2 inhibitors, and GLP-1 receptor agonists for latent autoimmune diabetes started 8 years ago. Pyoderma gangrenosum developed one year before admission, and she was started on 50 mg/day of prednisolone, which was tapered to 5 mg/day to account for the effect on her underlying diabetes mellitus, while she had recurrent refractory leg ulcers and skin and soft tissue infections that were repeatedly treated with antibacterial agents. Five days before her admission, blood tests revealed HbA1c level of 6.9%, C-peptide immunoreactivity (CPR) level of 7.2 ng/mL, triglycerides (TG) of 192 mg/dL, HDL cholesterol of 66 mg/dL, and LDL cholesterol of 137 mg/dL. Three days before her admission, she developed anorexia and headache. Upon admission, her vital signs, including body temperature and blood pressure, were within normal ranges, while her body mass index was recorded at 49.8. There were no abnormal findings in the chest or abdomen, and the neurological evaluation was unremarkable. Laboratory investigations revealed an elevated white blood cell count and increased CRP levels (Table 1). Urinary analysis showed the presence of ketones and bacteria; however, pyuria was not detected (Table 1). Her venous blood gas analysis showed a pH of 7.360 and HCO3- of 20.5. Although the urinary analysis results were atypical, she was diagnosed with a complicated UTI based on her clinical history of recurrent UTIs and treated with levofloxacin and trimethoprim-sulfamethoxazole. In addition, prednisolone was dosed up to 6 mg per day. She was not eating enough and was admitted to the hospital for intravenous therapy and blood glucose monitoring. Despite the ongoing treatment and an initial improvement in her symptoms during the course of hospitalization, her condition deteriorated rapidly on day 16 of hospitalization, leading to her sudden death on day 18. She presented with nausea and vomiting, with complaints of diarrhea and decreased urinary output before her death. Premortem blood tests indicated bicytopenia (Table 2), and two sets of blood cultures yielded positive results for E. coli using the BD BACTEC™ bottle.
Autopsy imaging using computed tomography (CT) showed enlargement and high density of the left adrenal glands compared to its normal appearance on images taken 5 months prior (Figure 1). Postmortem anatomical examinations revealed the presence of an accumulation of inflammatory cells in the renal pelvis and renal medulla. Despite the absence of bacteriological evidence, the pathology report indicated the presence of pyelonephritis (Figure 2). They also revealed an adrenal hemorrhage and necrosis (Figure 3), with the left adrenal gland showing more severe hemorrhage and necrosis compared to the right. Numerous erythrophagocytic macrophages were observed in the bone marrow (Figure 4), spleen (Figure 5), and liver. Acute splenitis with neutrophil infiltration, indicative of sepsis, was also observed in the spleen (Figure 5). The renal glomerular fibrin thrombus, confirming disseminated intravascular coagulopathy (DIC), was identified (Figure 6). Hemorrhagic diathesis secondary to DIC was evident with intra-alveolar, subpleural, subperitoneal, and ileal mucosal bleeding. The likely source of the E. coli leading to sepsis was identified as pyelonephritis. The autopsy concluded that the cause of death was acute adrenal insufficiency due to BAH and hemophagocytosis associated with sepsis caused by E. coli.
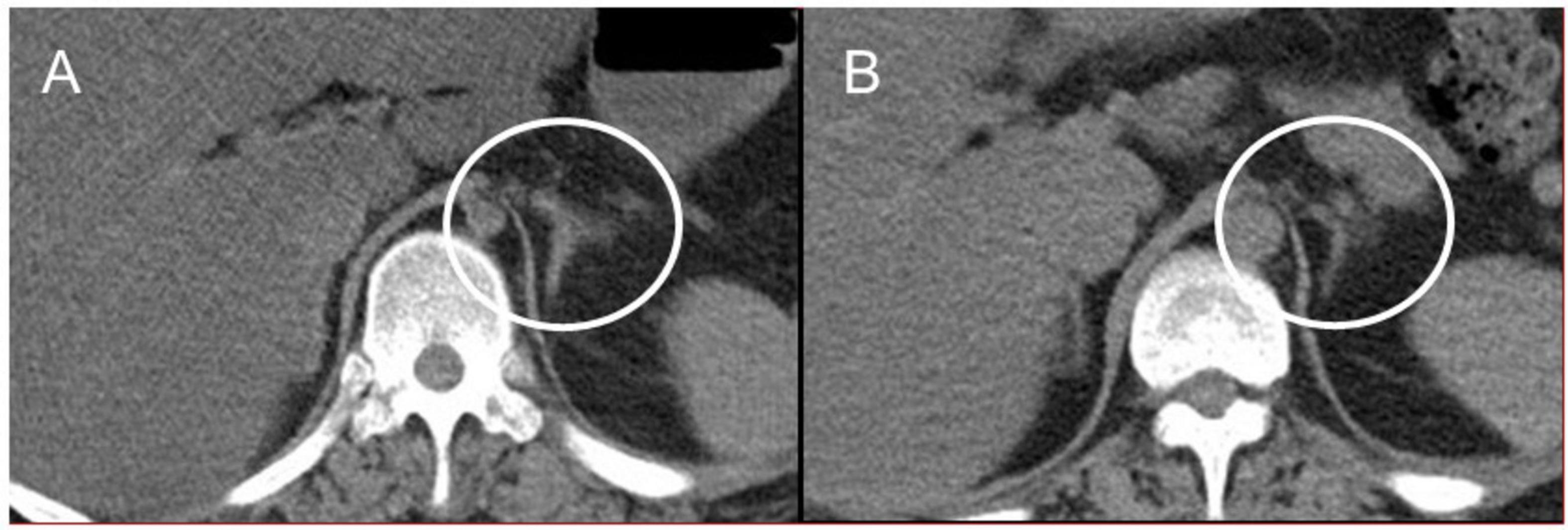
Figure 1. Abdominal CT images. (A) Postmortem CT imaging reveals hyperdensity in the left adrenal gland (indicated by a circle), suggestive of adrenal hemorrhage. (B) A CT scan performed 5 months prior to admission shows no abnormalities in the left adrenal gland (indicated by a circle). CT, computed tomography.
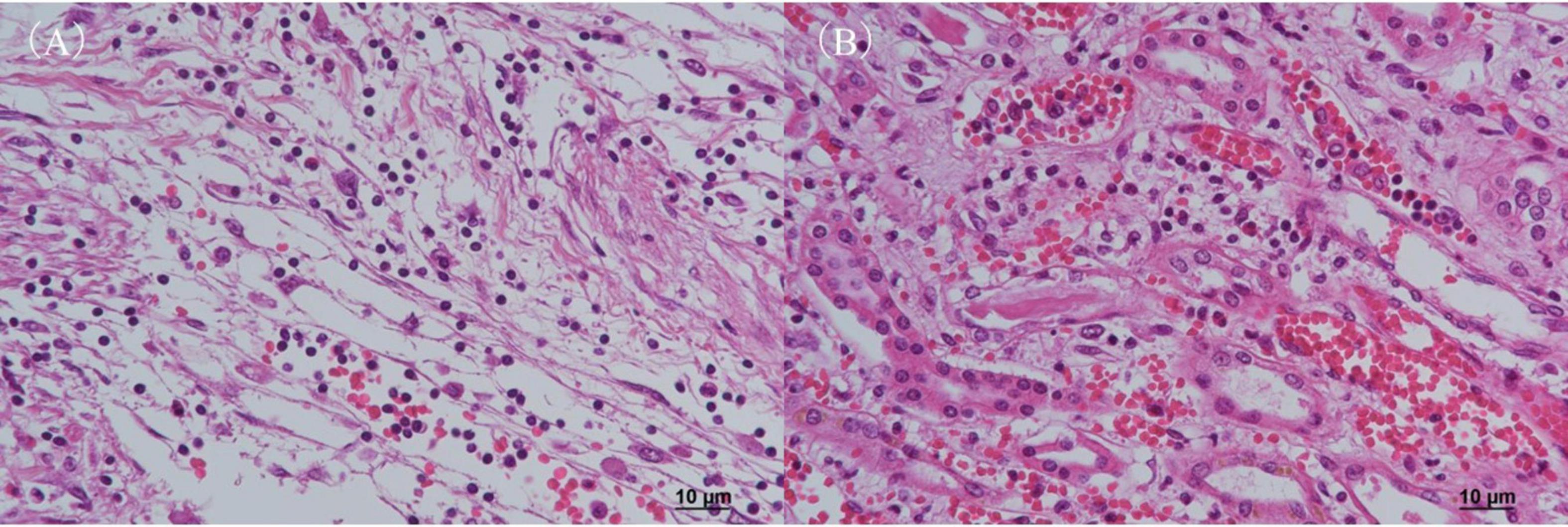
Figure 2. Histopathological examination of the kidney with H&E staining. (A) Renal pelvis and (B) renal medulla. Both regions show infiltration of inflammatory cells, predominantly neutrophils, along with evidence of hemorrhage, consistent with pyelonephritis. H&E, hematoxylin and eosin.
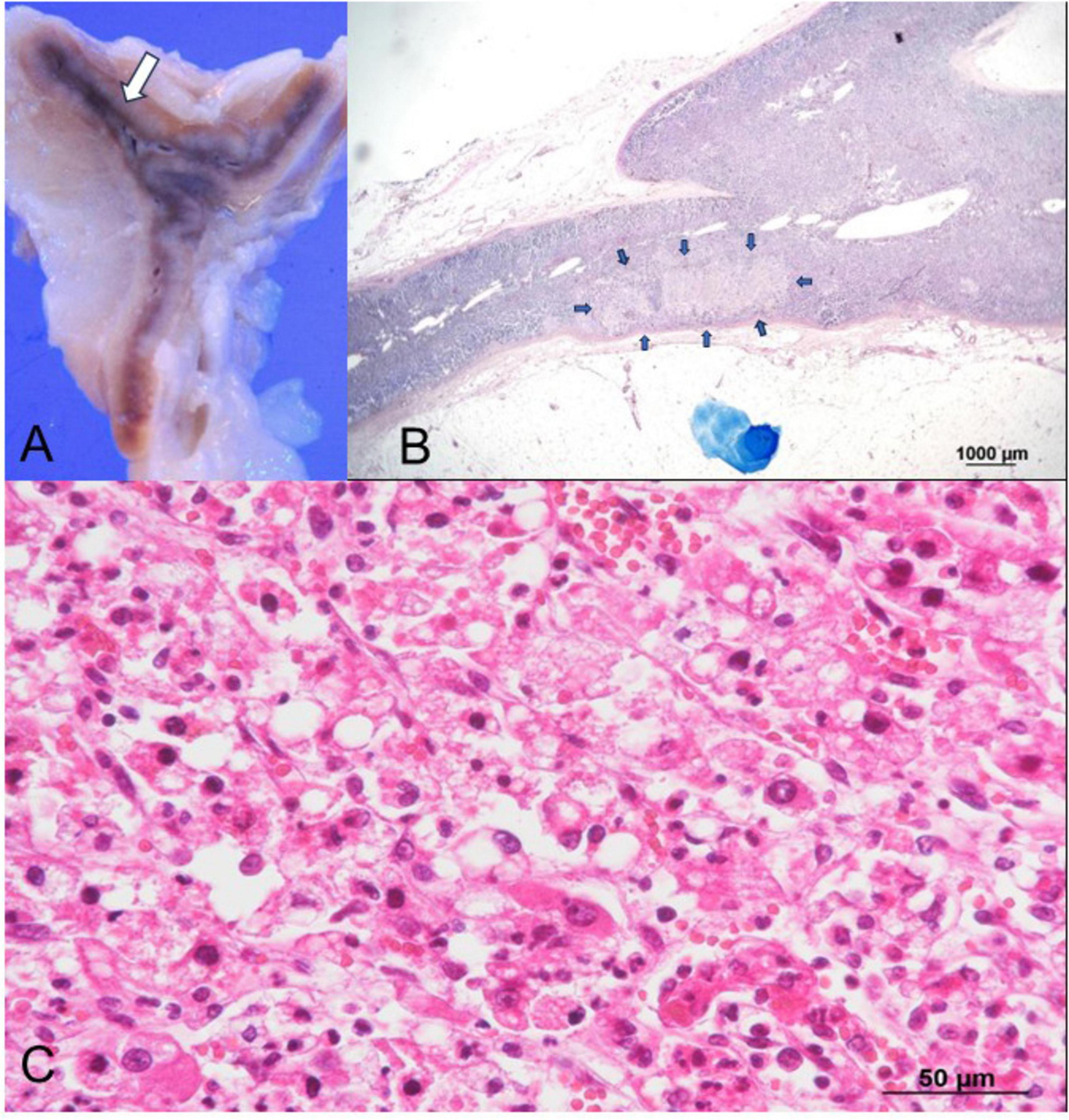
Figure 3. Histopathological findings of the left adrenal gland. (A) Gross examination reveals hemorrhage (arrow) in the left adrenal gland. (B) Low-magnification Giemsa staining highlights a weakly stained area (arrows) consistent with necrosis, with no bacteria observed. (C) Higher magnification of the weakly stained area in (B), examined under H&E staining, reveals extravascular erythrocytes and necrotic cells surrounded by neutrophils, indicating extensive hemorrhages and necrosis. H&E, hematoxylin and eosin.
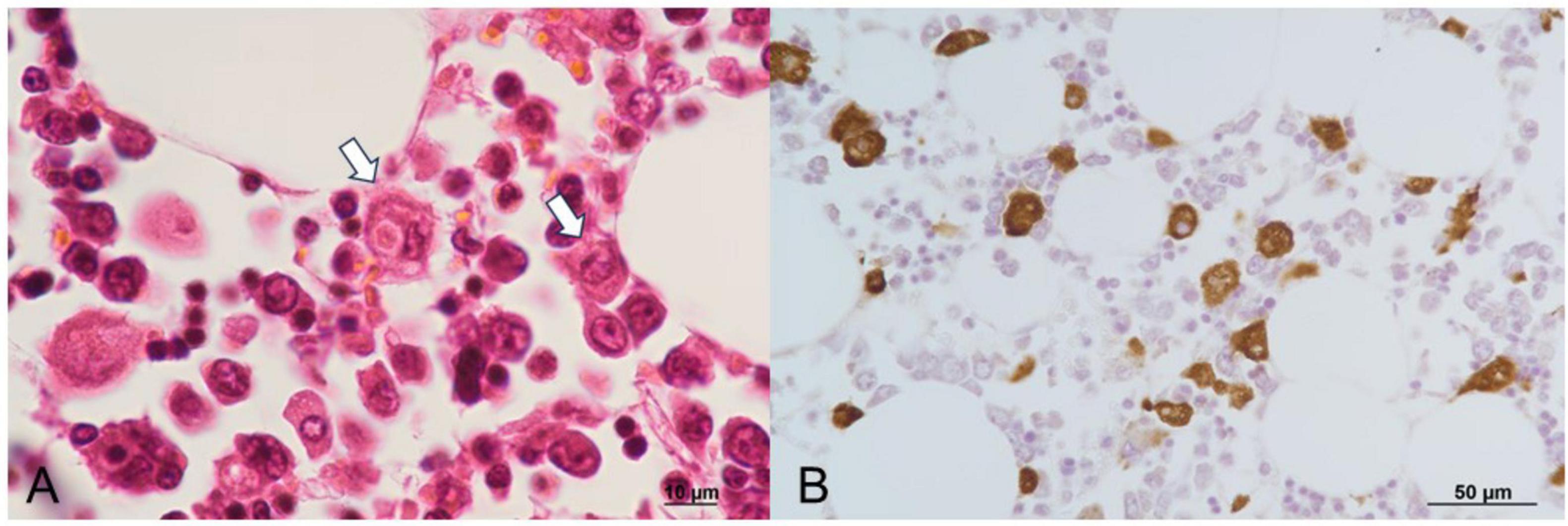
Figure 4. Histopathological findings of the bone marrow. (A) Macrophages engulfing erythrocytes, observed with H&E staining. (B) Erythrophagocytic macrophages demonstrate CD68 positivity on immunoperoxidase staining. H&E, hematoxylin and eosin.
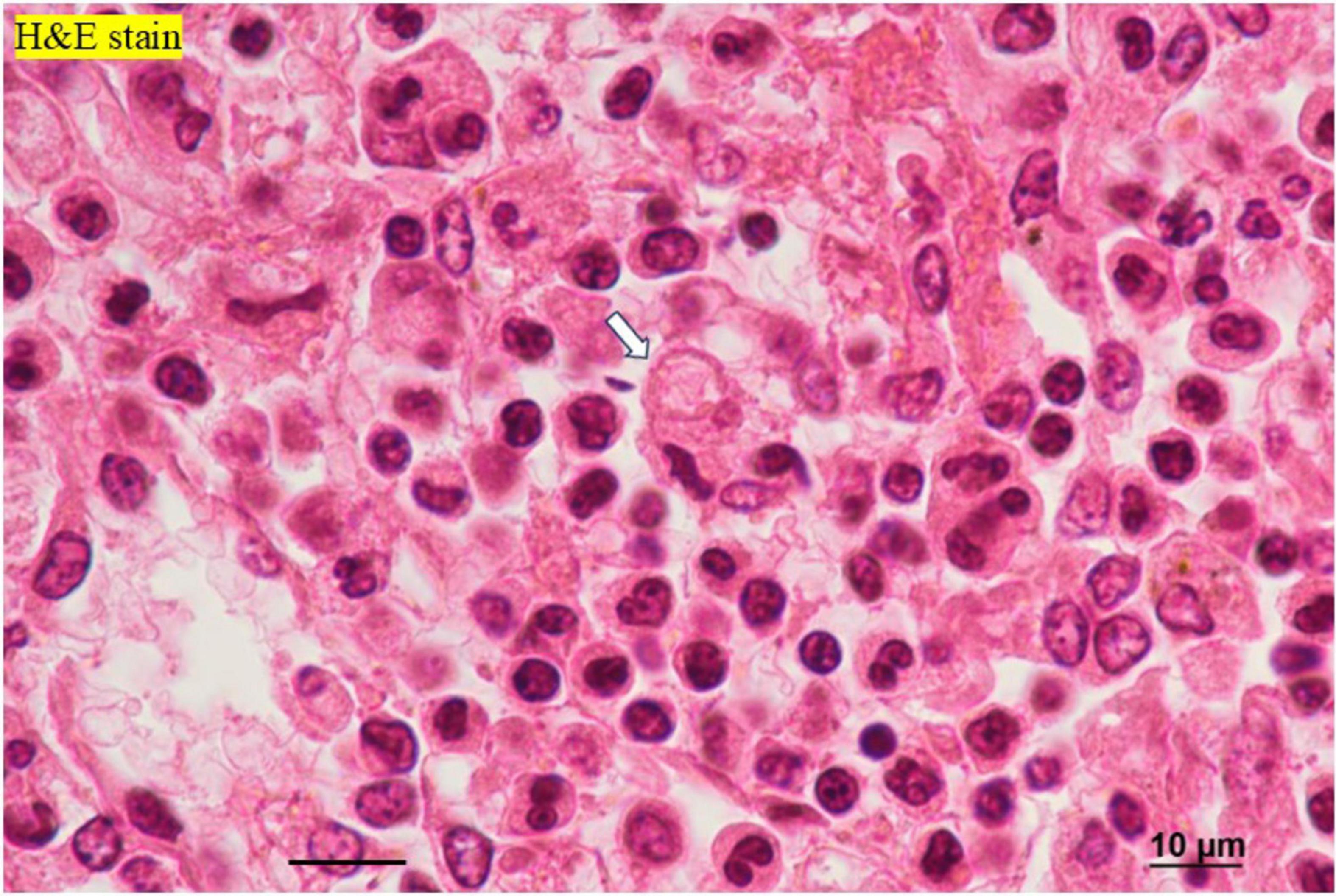
Figure 5. Histopathological findings of the spleen. H&E staining reveals neutrophils (black arrows) and erythrophagocytosis by macrophages (white arrow). H&E, hematoxylin and eosin.

Figure 6. Histopathological findings of the kidney. Phosphotungstic acid-hematoxylin staining reveals a fibrin thrombus (arrow) within the glomerular capillary, indicative of disseminated intravascular coagulopathy (DIC).
This case report details the autopsy findings of a young woman who succumbed to both BAH and suspected HLH secondary to an E. coli infection. HLH is characterized by a wide range of symptoms including fever, organomegaly, hepatomegaly, splenomegaly, lymphadenopathy, liver injury, consumptive coagulopathy, hypertriglyceridemia, pancytopenia, neurologic dysfunction, dermatologic abnormalities, and increased acute-phase reactants, especially serum ferritin (2). Due to the variability of these symptoms, HLH diagnosis can be challenging. According to the HLH-2004 diagnostic guidelines, primarily developed for pediatric cases, clinical diagnosis of HLH should fulfill five out of the following eight criteria: fever, splenomegaly, cytopenias (affecting at least two of three lineages), hypertriglyceridemia and/or hypofibrinogenemia, hemophagocytosis in bone marrow, spleen, or lymph nodes, ferritin ≥ 500 ng/mL, low or absent NK-cell activity, soluble CD25 > 2,400 U/mL (13). However, these criteria have not been validated for secondary HLH (14), making its diagnosis during sepsis particularly difficult. In cases of infection, organomegaly, cytopenia, and elevated serum ferritin levels are indicative of HLH, as they reflect erythrophagocytosis in the lymphoreticular system. In our case, we were unable to test for triglyceride, fibrinogen, ferritin, NK cell activity, or soluble CD25 because the patient died suddenly, and we did not suspect HLH in the premortem phase. In addition, hepatosplenomegaly was not discernible due to significant obesity and concurrent fatty liver. Although a definitive diagnosis of HLH could not be made due to a lack of testing, we actively suspected the possibility of HLH because blood test data showed bicytopenia, pathological findings indicated signs of hemophagocytosis, and there have been reports of HLH in patients with bacterial infections, including E. coli (5–8).
Suspecting acute adrenal insufficiency, including classical Waterhouse-Friderichsen syndrome, but constrained by the rapid clinical progression, we could not perform some tests including endocrinological tests. Autopsy findings revealed an enlarged left adrenal gland and bilateral hemorrhage with necrosis of the adrenal cortices. Over the years, there have been reports of BAH related to multiple etiologies, including various systemic bacterial and viral infections (9, 10), with Neisseria meningitidis as a notable causative agent of BAH. However, cases of BAH resulting from E. coli infection are rare (11–13). Although E. coli is a common microorganism, many internists may overlook the complications associated with BAH. BAH, leading to adrenal insufficiency (15, 16), is often predisposed by DIC (17, 18). While antemortem diagnosis of BAH is challenging, serial CT imaging of the abdomen is valuable (15, 16), as confirmed by our autopsy imaging.
As far as we know, there is no previous report regarding the combination of BAH and HLH. However, both conditions are fatal and can be caused by severe infections, including sepsis. Additionally, radiological diagnosis has limitations for both conditions, and several tests are often required, including genetic and pathological tests. In fact, in our case, the diagnosis was made after evidence of these diseases was collected through a postmortem pathological autopsy. Based on these findings, we speculated that the lack of previous reports may be due to underdiagnosis.
The patient had multiple risk factors including diabetes mellitus, severe obesity, and chronic oral corticosteroid use. Although we could not determine her immune status before death, it was likely insufficient due to her history of recurrent infections, including skin and soft tissue infections. In addition, although we did not diagnose pyelonephritis during her pre-mortem phase, we observed evidence of it during the postmortem autopsy. The rapid progression of the infection leading to her death may have been due to her immunocompromised status. The sepsis, secondary to E. coli infection from pyelonephritis, likely increased her body’s demand for steroids, and persistent infection-related hypercytokinemia may have ensued. We concluded that the E. coli infection precipitated multiple fatal conditions such as DIC, BAH and conditions in which HLH may be suspected, culminating in the young woman’s death.
This study has some limitations: the course of events leading up to her death was so rapid that there were only limited test results available. Specifically, the complications of HLH and BAH were not recognized during her life, and the necessary tests for diagnosing HLH, including hypercytokinemia, were not conducted, which prevented a definitive diagnosis. Additionally, the possibility of familial HLH could not be ruled out. Although fibrin thrombi in the renal glomeruli demonstrated pathomorphological findings consistent with DIC, coagulability studies to confirm DIC could not be performed. Antimicrobial susceptibility testing of the E. coli identified postmortem was not performed, so the effectiveness of the levofloxacin and trimethoprim-sulfamethoxazole treatments administered during her illness could not be evaluated. In addition, urine culture was not performed at the time of death, and bacteriological E. coli urinary tract infection could not be proven. However, because we found evidence of adrenal hemorrhage, pyelonephritis, and hemophagocytosis in the reticuloendothelial system at autopsy, we believe this is an important case report, despite the limitations mentioned above.
We presented an autopsy case of a young woman with bilateral adrenal hemorrhage (BAH) and hemophagocytosis in the reticuloendothelial system associated with Escherichia coli infection. Although E. coli is a common bacterium, it can cause serious complications such as BAH and hemophagocytosis, even in young adults, particularly when the patient is immunocompromised due to steroid therapy or other conditions, potentially leading to death. To our knowledge, there have been no previous reports of simultaneous adrenal hemorrhage and hemophagocytosis induced by E. coli, making this a valuable case report.
The original contributions presented in this study are included in this article/supplementary material, further inquiries can be directed to the corresponding author.
The requirement for ethical approval was waived by the Ethics Committee of Nittazuka Medical Welfare Center in accordance with the local legislation and institutional requirements. Written informed consent was obtained from the individual’s next of kin/legal guardians for the publication of any potentially identifiable images or data included in this article. Written informed consent was obtained from the patient’s family for the publication of this case report.
YT: Conceptualization, Data curation, Formal Analysis, Investigation, Validation, Writing – original draft, Writing – review and editing. KojH: Conceptualization, Data curation, Formal Analysis, Investigation, Methodology, Resources, Supervision, Validation, Visualization, Writing – original draft, Writing – review and editing. EK: Conceptualization, Formal Analysis, Investigation, Supervision, Validation, Writing – original draft, Writing – review and editing. S-IA: Conceptualization, Data curation, Formal Analysis, Investigation, Methodology, Validation, Writing – original draft, Writing – review and editing. MH: Conceptualization, Data curation, Investigation, Supervision, Validation, Writing – original draft, Writing – review and editing. YN: Conceptualization, Data curation, Investigation, Methodology, Validation, Writing – original draft, Writing – review and editing. AS: Data curation, Formal Analysis, Methodology, Validation, Writing – original draft, Writing – review and editing. MU: Data curation, Formal Analysis, Investigation, Validation, Writing – original draft, Writing – review and editing. RA: Data curation, Investigation, Supervision, Validation, Writing – original draft, Writing – review and editing. HH: Data curation, Investigation, Supervision, Writing – original draft, Writing – review and editing. TM: Formal Analysis, Investigation, Supervision, Writing – original draft, Writing – review and editing. KouH: Data curation, Investigation, Supervision, Writing – original draft, Writing – review and editing. MS: Data curation, Formal Analysis, Investigation, Supervision, Writing – original draft, Writing – review and editing. YK: Data curation, Investigation, Supervision, Validation, Writing – original draft, Writing – review and editing.
The authors declare that no financial support was received for the research, authorship, and/or publication of this article.
We would like to express our gratitude to Professor Ippei Sakamaki, the Department of Infectious Diseases at the University of Fukui, for his invaluable guidance on infectious diseases and hematology.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
BAH, bilateral adrenal hemorrhage; CT, computed tomography; DIC, disseminated intravascular coagulopathy; E. coli, Escherichia coli; HLH, hemophagocytic lymphohistiocytosis; UTI, urinary tract infection.
1. Singer M, Deutschman C, Seymour C, Shankar-Hari M, Annane D, Bauer M, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA. (2016) 315:801–10. doi: 10.1001/jama.2016.0287
2. Al-Samkari H, Berliner N. Hemophagocytic lymphohistiocytosis. Annu Rev Pathol. (2018) 13:27–49. doi: 10.1146/annurev-pathol-020117-043625
4. Fisman D. Hemophagocytic syndromes and infection. Emerg Infect Dis. (2000) 6:601–8. doi: 10.3201/eid0606.000608
5. Oda Y, Urushidani Y, Ooi S, Endoh A, Nakamura R, Adachi K, et al. Hemophagocytic lymphohistiocytosis in a rheumatoid arthritis patient treated with infliximab. Intern Med. (2012) 51:655–7. doi: 10.2169/internalmedicine.51.5687
6. Ishii E, Ohga S, Imashuku S, Yasukawa M, Tsuda H, Miura I, et al. Nationwide survey of hemophagocytic lymphohistiocytosis in Japan. Int J Hematol. (2007) 86:58–65. doi: 10.1532/IJH97.07012
7. Chang K, Tang L, Lyu R. Spontaneous Escherichia coli meningitis associated with hemophagocytic lymphohistiocytosis. J Formos Med Assoc. (2006) 105:756–9. doi: 10.1016/S0929-6646(09)60204-7
8. Risdall R, Brunning R, Hernandez J, Gordon D. Bacteria-associated hemophagocytic syndrome. Cancer. (1984) 54:2968–72. doi: 10.1002/1097-0142(19841215)54:12
9. D’Agati M, Major B, Marangoni M. The waterhouse-friderichsen syndrome. N Engl J Med. (1945) 232:1–7. doi: 10.1056/NEJM194501042320101
10. Guarner J, Paddock C, Bartlett J, Zaki S. Adrenal gland hemorrhage in patients with fatal bacterial infections. Mod Pathol. (2008) 21:1113–20. doi: 10.1038/modpathol.2008.98
11. Khwaja J. Bilateral adrenal hemorrhage in the background of Escherichia coli sepsis: A case report. J Med Case Rep. (2017) 11:72. doi: 10.1186/s13256-017-1236-0
12. Yokoyama S, Sekioka A, Utsunomiya H, Hara S, Takahashi T, Yoshida A. Adrenal abscess as a complication of Escherichia coli sepsis in neonates: A case report. J Pediatr Surg Case Rep. (2013) 1:328–30. doi: 10.1016/j.epsc.2013.09.001
13. Henter J, Horne A, Aricó M, Egeler R, Filipovich A, Imashuku S, et al. HLH-2004: diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer. (2007) 48:124–31. doi: 10.1002/pbc.21039
14. Otrock Z, Daver N, Kantarjian H, Eby C. Diagnostic challenges of hemophagocytic lymphohistiocytosis. Clin Lymphoma Myeloma Leuk. (2017) 17S:S105–10. doi: 10.1016/j.clml.2017.02.017
15. Siu S, Kitzman D, Sheedy P, Northcutt R. Adrenal insufficiency from bilateral adrenal hemorrhage. Mayo Clin Proc. (1990) 65:664–70. doi: 10.1016/S0025-6196(12)65129-5
16. Vella A, Nippoldt T, Morris J. Adrenal hemorrhage: A 25-year experience at the Mayo clinic. Mayo Clin Proc. (2001) 76:161–8. doi: 10.4065/76.2.161
17. Mutlu M, Karagüzel G, Aslan Y, Cansu A, Ökten A. Adrenal hemorrhage in newborns: A retrospective study. World J Pediatr. (2011) 7:355–7. doi: 10.1007/s12519-011-0259-7
Keywords: bilateral adrenal hemorrhage, hemophagocytic lymphohistiocytosis, disseminated intravascular coagulopathy, sepsis, Escherichia coli
Citation: Tanaka Y, Hayashi K, Kawahara E, Azuma S-I, Hayashi M, Nakaya Y, Suzuki A, Ueda M, Asano R, Hayashi H, Miura T, Hayashi K, Sato M and Kobayashi Y (2025) Case Report: Bilateral adrenal hemorrhage and hemophagocytosis in the reticuloendothelial system caused by Escherichia coli in a young woman: an autopsy case. Front. Med. 12:1496961. doi: 10.3389/fmed.2025.1496961
Received: 16 September 2024; Accepted: 24 February 2025;
Published: 11 March 2025.
Edited by:
Shisan (Bob) Bao, The University of Sydney, AustraliaReviewed by:
Abhilasha Kandahalli Venkataranga Nayaka, National Cancer Institute at Frederick (NIH), United StatesCopyright © 2025 Tanaka, Hayashi, Kawahara, Azuma, Hayashi, Nakaya, Suzuki, Ueda, Asano, Hayashi, Miura, Hayashi, Sato and Kobayashi. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Koji Hayashi, a2poYXlhc2hpQGYtZ2guanA=
†These authors have contributed equally to this work and share first authorship
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.