
94% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Med. , 16 September 2021
Sec. Intensive Care Medicine and Anesthesiology
Volume 8 - 2021 | https://doi.org/10.3389/fmed.2021.716086
 Xuyan Li1†
Xuyan Li1† Ming Hu2†
Ming Hu2† Ruiqiang Zheng3†
Ruiqiang Zheng3† Yishan Wang1†
Yishan Wang1† Hanyujie Kang1†
Hanyujie Kang1† Li Jiang4
Li Jiang4 Ming Zhong5
Ming Zhong5 Ling Sang6
Ling Sang6 Xia Zheng7
Xia Zheng7 Chun Pan8
Chun Pan8 Wei Zhang9
Wei Zhang9 Haibo Qiu8*
Haibo Qiu8* Bin Du10*
Bin Du10* Zhaohui Tong1*
Zhaohui Tong1*Background: Extracorporeal membrane oxygenation (ECMO) is a rapidly evolving therapy for acute lung and/or heart failure. However, the information on the application of ECMO in severe coronavirus disease 2019 (COVID-19) is limited, such as the initiation time. Especially in the period and regions of ECMO instrument shortage, not all the listed patients could be treated with ECMO in time. This study aimed to investigate and clarify the timing of ECMO initiation related to the outcomes of severe patients with COVID-19. The results show that ECMO should be initiated within 24 h after the criteria are met.
Methods: In this retrospective, multicenter cohort study, we enrolled all ECMO patients with confirmed COVID-19 at the three hospitals between December 29, 2019 and April 5, 2020. Data on the demographics, clinical presentation, laboratory profile, clinical course, treatments, complications, and outcomes were collected. The primary outcomes were successful ECMO weaning rate and 60-day mortality after ECMO. Successful weaning from ECMO means that the condition of patients improved with adequate oxygenation and gas exchange, as shown by the vital signs, blood gases, and chest X-ray, and the patient was weaned from ECMO for at least 48 h.
Results: A total of 31 patients were included in the analysis. The 60-day mortality rate after ECMO was 71%, and the ECMO weaning rate was 26%. Patients were divided into a delayed ECMO group [3 (interquartile range (IQR), 2–5) days] and an early ECMO group [0.5 (IQR, 0–1) days] based on the time between meeting the ECMO criteria and ECMO initiation. In this study, 14 and 17 patients were included in the early and delayed treatment groups, respectively. Early initiation of ECMO was associated with decreased 60-day mortality after ECMO (50 vs. 88%, P = 0.044) and an increased ECMO weaning rate (50 vs. 6%, P = 0.011).
Conclusions: In ECMO-supported patients with COVID-19, delayed initiation of ECMO is a risk factor associated with a poorer outcome.
Trial Registration: Clinical trial submission: March 19, 2020. Registry name: A medical records-based study for the clinical application of extracorporeal membrane oxygenation in the treatment of severe respiratory failure patients with novel coronavirus pneumonia (COVID-19). Chinese Clinical Trial Registry: https://www.chictr.org.cn/showproj.aspx?proj=51267,identifier:~ChiCTR2000030947.
Severe acute respiratory syndrome coronavirus (SARS-CoV) and Middle East respiratory syndrome coronavirus (MERS-CoV) were responsible for the first two pandemics at the beginning of the Twenty-first century. The ongoing SARS-CoV-2 pandemic was the third coronavirus pandemic of this century (1). Coronaviruses are enveloped ribonucleic acid (RNA) viruses that represent relevant pathogens in the respiratory tract and lung infections (2, 3). Coronavirus disease 2019 (COVID-19) caused by SARS-CoV-2 was identified in Wuhan, China, in December 2019 (4), and it has become a global health concern. The number of cases of COVID-19 is increasing substantially worldwide.
However, the mortality rate of critically ill patients with COVID-19 was 61.5%, and patients who developed acute respiratory distress syndrome (ARDS) have been at high risk of dying from refractory hypoxemia, even with timely and standardized invasive mechanical ventilation (IMV) (5). The mortality rate has even reached 97% in patients receiving invasive ventilation (6). As the ultimate means of respiratory support, extracorporeal membrane oxygenation (ECMO) can maintain oxygenation and effectively implement a “lung protective ventilation strategy” (7). Previous studies have shown that ECMO could reduce the mortality of patients with severe ARDS in the influenza A (H1N1) outbreak of 2009 (8), avian influenza A (H7N9) viral pneumonia (9), and MERS (10). Therefore, we believe that ECMO could also be effective for other types of severe viral pneumonia (11). A recent descriptive study that compared the outcomes of patients on ECMO with mechanical ventilation to patients without ECMO but with mechanical ventilation also indicated that ECMO might be an effective salvage treatment for severe patients infected with COVID-19 (12).
Studies have shown that the mortality of severe COVID-19 patients treated with ECMO was relatively high, ranging from 57.1 to 100%, although the sample sizes of these studies were all relatively small (5, 12, 13). A large sample study in patients suffering from COVID-19 who were treated with ECMO found a 90-day mortality rate of 39% (14). Recently, several multicenter studies found that the mortality of patients with COVID-19 managed with ECMO ranged from 33.2 to 54.3% (15–17). The effect of ECMO on the outcome of patients with severe COVID-19 remains uncertain. The feasibility of launching randomized clinical trials to verify the efficacy of ECMO in this population is affected by many difficulties in patient recruitment, study design, and ethical concerns. Therefore, an observational research is a reasonable alternative. In this study, we expect to compare the effect of early and delayed initiation of ECMO on the outcomes of patients with severe ARDS related to COVID-19.
This is a retrospective, multicenter cohort study. All the adult severe patients with COVID-19 treated with ECMO in Jinyintan Hospital, Wuhan Pulmonary Hospital, and Wuhan Asian General Hospital between December 29, 2019 and April 5, 2020 at Wuhan, China, were enrolled in this study. According to the time between meeting the ECMO criteria and the initiation of ECMO, the included patients were divided into two groups, namely, the “early ECMO group” and “delayed ECMO group.” The former refers to the group of patients who began ECMO within 24 h of meeting the ECMO to Rescue Lung Injury in Severe ARDS (EOLIA) trial criteria (7), as indicated by one of the following three criteria: Partial pressure of arterial oxygen [PaO2]/fraction of inspired oxygen [FiO2] ratio of <50 mmHg for more than 3 h; PaO2/FiO2 ratio of <80 mmHg for more than 6 h; or an arterial blood pH of <7.25 with a partial pressure of arterial carbon dioxide of at least 60 mmHg for more than 6 h. The “delayed ECMO group” refers to the group of patients that did not begin ECMO until more than 24 h after meeting one of the first indications for ECMO initiation. The effect of the timing of ECMO initiation on the outcomes of patients was investigated by comparing the groups.
The study was approved by the Jinyintan Hospital ethics board (KY-2020-10.02). Informed consent was waived since we collected and analyzed all data from the patients according to the policy for public health outbreak investigation of emerging infectious diseases issued by the National Health Commission of the People's Republic of China.
The inclusion criteria were the adult patients with ARDS (≥18 years old) who had laboratory-confirmed COVID-19 and were given veno-venous ECMO (VV-ECMO) support because of refractory hypoxemia (PaO2/FiO2 ratio <50 mmHg for 3 h and PaO2/FiO2 ratio <80 mmHg for 6 h). The diagnosis of ARDS was made according to the Berlin definition (18). The confirmed diagnosis of COVID-19 was established according to the definition established by the WHO interim guidance with positive SARS-CoV-2 nucleic acid test results in throat swab specimens (19).
Due to the limitations of the resources and professional staffing for ECMO during the early stage of the pandemic, only three representative hospitals were included in this study. The exclusion criteria were an age of more than 75 years; receipt of mechanical ventilation >7 days; and multiple organ failure (such as severe liver failure, massive upper gastrointestinal hemorrhage, and disseminated intravascular coagulation). Given the poorer outcome with age, the balance between resource availability and the potential to improve outcomes should be considered. Because the outcome worsens with time on invasive mechanical ventilation (IMV), patients on mechanical ventilation >7 days should also be excluded (note: this is a general guideline that may not apply to specific patients with COVID-19 depending on the local circumstances). In addition, the use of ECMO in patients with a combination of advanced age, multiple comorbidities, or multiple organ failure should be rare, and no such patients were included in the study.
In this study, we retrospectively collected data on the demographics, clinical presentation, laboratory results, time from onset to ICU admission, duration of high-flow nasal cannula (HFNC) therapy before ECMO, duration of non-invasive ventilation (NIV) before ECMO, duration of IMV before ECMO, implementation of rescue ventilation strategies (such as prone-position ventilation) before ECMO, disease severity score, total duration of ECMO and IMV, and treatments and complications during ECMO. The primary outcomes were successful ECMO weaning rate and 60-day mortality after ECMO. Successful weaning refers to a group of patients whose condition improved with adequate oxygenation and gas exchange, as shown based on the vital signs, blood gases, and chest x-ray results, and who were weaned from ECMO for at least 48 h. All included patients were followed up until intensive care unit (ICU) discharge or death, or up to June 15, 2020. Two researchers independently reviewed the case report form to double check and input the collected data.
Descriptive data were presented as frequencies (percentages) for discrete variables and as the means (SDs) or medians [interquartile ranges (IQRs)] for continuous variables. Comparisons were determined by Student's t-test and the Mann–Whitney test for continuous variables and by the use of Fisher's exact test for categorical variables. Repeated measured data were compared by repeated measured ANOVA. The Kaplan–Meier curves between groups were compared by the log-rank test. The statistical significance level was set at 0.05 (two-tailed). All the analyses were conducted with SPSS version 23.0 (SPSS Inc., Chicago, IL, USA) and GraphPad Prism 8 (San Diego, CA, USA).
Finally, 31 patients who received VV-ECMO support at the three hospitals were included in the analysis. Fourteen patients were assigned to the early ECMO group, and 17 patients were assigned to the delayed ECMO group. The flowchart of the study population is shown in Figure 1.
Among the 31 patients included in the analysis, the median age was 58 years (IQR, 46–64.5 years), and 19 (61%) were men. The recorded comorbidities included hypertension n = 7 (23%) and diabetes n = 5 (16%), and no difference between the two groups was observed. The Acute Physiology and Chronic Health Evaluation (APACHE II) scores of the patients were not significantly different between the groups both on ICU admission and before ECMO application. The Sequential Organ Failure Assessment (SOFA) score before ECMO application was not significantly different between the groups (P > 0.999). The median length from symptom onset to hospital admission was 11 days (IQR, 6–17 days), and the median time from symptom onset to ICU admission, to IMV and to ECMO were 15 days (IQR, 9–20 days), 19 days (IQR, 12–23.5 days), and 22 days (IQR, 16.5–26 days), respectively. The clinical course is shown in Figure 2. Patients in the early ECMO group had a significantly shorter duration of IMV before ECMO, duration of mechanical ventilation (MV) before ECMO, and duration of HFNC and MV before ECMO than the values in the delayed ECMO group (Table 1). The time between meeting the ECMO criteria and the initiation of ECMO was significantly longer in the delayed ECMO group (P < 0.001). Regarding the outcomes, delayed initiation of ECMO was associated with increased 60-day mortality after ECMO compared with the early ECMO group (88 vs. 50%, P = 0.044). The ICU mortality was also increased in the delayed ECMO group (94 vs. 57%, P=0.026). Kaplan–Meier survival estimates during the 60 days after ECMO onset and ICU stay showed statistical significance between the groups (P = 0.0426 and 0.0253, respectively) (Table 1, Figure 3). Fewer patients in the delayed ECMO group were successfully weaned from ECMO than in the early ECMO group (6 vs. 50%, P = 0.011). The median duration of ECMO was 14 days (IQR, 4.5–35 days). The total viral nucleic acid negative conversion ratio and viral shedding days were similar between the groups.
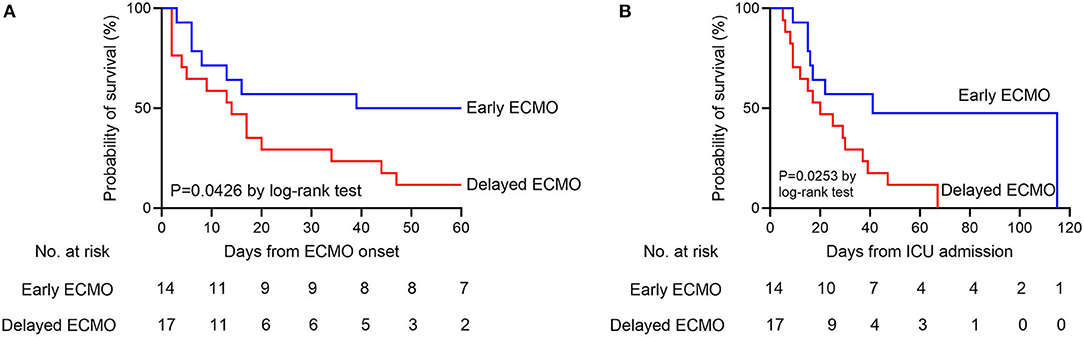
Figure 3. (A) Kaplan–Meier survival estimates of the early ECMO group and delayed ECMO group during the 60 days after ECMO onset. (B) Kaplan–Meier survival estimates of the early ECMO group and delayed ECMO group during the ICU stay. ECMO, extracorporeal membrane oxygenation; ICU, intensive care unit.
Patients receiving ECMO treatment were followed for 6 h before ECMO application and 24 and 72 h after ECMO. Three patients died between 24 and 72 h after ECMO application; thus, their data are missing from the 72 h follow-up. The respiratory rate improved after ECMO application, dropping from 30 ± 14 to 25 ±8 beats/min (bpm) 24 h after ECMO and 22 ± 7 bpm 72 h after ECMO (Table 2). The mean arterial blood pressure (MAP) was rather steady at >75 mmHg. The initial tidal volume (Vt/predicted body weight) was 5.2 ± 1.0 ml/kg before ECMO onset and was reduced to 3.2 ± 0.9 ml/kg after ECMO onset, in compliance with the “lung protective ventilation strategy.” A relatively high positive end expiratory pressure (PEEP) was seen before and after ECMO application, although the differences were not observed between each time point. Patient oxygenation was significantly improved after the onset of ECMO. The PaO2 was 66 ± 19 mmHg before ECMO onset and 89 ± 31 and 82 ± 23 mmHg at each time point after ECMO onset, and both were significantly improved compared with 6 h pre-ECMO (P = 0.003). The PaO2/FiO2 ratio was 76 ± 29 before ECMO, 146 ± 70 at 24 h, and 163 ± 92 at 72 h (P < 0.001). Carbon dioxide (CO2) clearance was also significantly improved (6 h pre-ECMO 56 ± 20 mmHg vs. 24 h on ECMO 43 ± 12 mmHg vs. 72 h on ECMO 41 ± 6 mmHg, P=0.001).
Routine blood tests showed a trend of decreased total white blood cell count but were not significantly different between each time point. The lymphocyte count was 0.5 × 109/L (0.3–0.7) before ECMO and 0.6 × 109/L (0.5–1.1) 72 h after ECMO (Supplementary Table 1). Although blood transfusion was actively implemented in most of the patients, hemoglobin showed a sequential downward trend. A significant reduction was observed in the level of platelets at 72 h on ECMO (P < 0.001). A mildly elevated total bilirubin (TBIL) level was also observed. The creatinine level was slightly elevated after ECMO but was not significantly different between timepoints. Regarding laboratory findings on coagulopathy, a significantly prolonged activated partial thromboplastin time (APTT) was noticed after ECMO initiation due to the continuous infusion of heparin. APTT was continuously monitored and was fluttered from 51.8 ± 20.2 to 54.4 ± 16.0 s after ECMO. The decreased fibrinogen (FIB) was also observed in patients after ECMO initiation (2.8 ± 1.7 g/L at 24 h on ECMO; 3.0 ± 1.9 g/L at 72 h on ECMO). D-dimer was not significantly different among the timepoints (Supplementary Table 2).
In the total 31 patients, more than half of the patients received antiviral treatment [21 (68%)] (Table 3). A continuous renal replacement therapy (CRRT) was applied 27 times for the clearance of inflammatory mediators and renal function protection. Four (16%) patients received tracheotomy. Significant differences were not observed between the groups.
In total, ventilation-associated pneumonia (VAP) occurred in 22 (71%) patients (Table 4). Catheter-related bloodstream infection (CRBSI) occurred in eight (26%) patients. Nine patients had hemorrhage onset during the clinical course, and one patient had bleeding at multiple sites. Barotrauma occurred in eight (26%) patients and was related to IMV. Hemolysis was seen in one patient related to ECMO. The ECMO mechanical complications were seen in six patients.
Eight patients were successfully weaned off ECMO, and among them, one patient died 10 days after weaning because of severe infection due to invasive pulmonary aspergillosis (IPA). Seven (88%) of these patients were men, with a median age of 44.5 years (IQR, 41–63 years) (Supplementary Table 4). The pre-ECMO APACHE II score and SOFA score were 12.6 ± 4.4 and 7.9 ± 3.0, respectively. Median ECMO duration was 26 days (IQR, 17–38 days). All patients received IMV before ECMO. The PaO2/FiO2 ratio was 219 ± 93 mmHg, and the partial pressure of arterial carbon dioxide (PaCO2) was 41 ± 9 mm Hg before weaning (Supplementary Table 3).
This study descriptively discussed and elaborated on the efficacy and safety of ECMO in patients with COVID-19 with severe ARDS. We found that the outcome was related to the timing of ECMO initiation, and patients in the early initiation group had an increased ECMO successful weaning rate and decreased 60-day mortality after ECMO compared to the delayed ECMO patients.
A majority (67–85%) of critically ill patients admitted to ICUs with confirmed COVID-19 developed ARDS (5, 20). Although the Extracorporeal Life Support Organization (ELSO) issued guidance on the use of ECMO in patients with COVID-19 (21), ECMO should be considered according to the standard management algorithm for ARDS in supporting patients with viral lower respiratory tract infection. Many studies also recommend ECMO as a standard strategy in experienced ECMO centers for patients meeting EOLIA criteria (22). However, the worldwide experience with using ECMO to support patients with COVID-19 is limited. Therefore, we conducted this study to report on the efficacy and safety of ECMO in patients with severe ARDS related to COVID-19.
The application of ECMO could improve oxygenation, reduce carbon dioxide, and stabilize the vital signs of patients. However, the 60-day mortality after ECMO was 71% in this study, which was higher than the mortality of H1N1-induced ARDS following the ECMO treatment (8, 23) and even slightly higher than the mortality of severe MERS-CoV and H7N9 pneumonia patients treated by ECMO (9, 10). The main reason was the controversial results regarding the timing of ECMO initiation.
Although patients may meet the EOLIA criteria, which are widely used, ECMO support may not be initiated in time (7, 24). The COVID-19 pandemic has greatly strained the critical care resources of hospitals in Wuhan, especially if they were not adequately resourced or staffed (5). In the early stage of the outbreak, we focused on increasing the number of beds, ventilators, and ICU clinicians to address the problems. This study found that 55% of the patients were in the delayed ECMO group, and ECMO support was established at a median of 4 days after meeting the EOLIA criteria. They had higher 60-day mortality after ECMO and a lower successful weaning rate. Compared to the early group, they had a longer duration of IMV before ECMO. The duration of IMV before ECMO of more than 7 days was an important prognostic factor for death (25). Although the IMV duration of all patients pre-ECMO in our study was <7 days, the delayed group had a significantly longer duration, with a median of 4 days before ECMO. However, ECMO was started at 2 h (1–5 h) after IMV among the patients with H1N1, with a lower ICU mortality of 23% in Australia and New Zealand in 2009 (8). Therefore, we emphasize the importance of early implementation of ECMO in patients with severe ARDS related to COVID-19.
The past experience with the self-limited disease H1N1 or H7N9 virus-induced ARDS indicated that the median duration of ECMO support was 8–10 days (8, 9, 26). For all types of ARDS, the EOLIA study showed that the median duration was 15 days (7). However, the median duration was 26 days in successfully weaned COVID-19 patients, which was partially related to the prolonged viral shedding and lack of a clear antiviral therapy in SARS-CoV-2 (13). ELSO-issued guidance showed that ~21 days on ECMO could be considered futile, and this study indicated that extending the duration of ECMO should be considered for the patients infected with COVID-19 (21).
The hospital-level volume of ECMO cases was related to the outcomes of patients (27), and VV-ECMO for respiratory support in Wuhan was not at the leading level before this outbreak in China. Despite the support of medical staff from national high-level ECMO treatment centers, management problems were still one of the risk factors leading to high mortality. Nosocomial infections during ECMO were associated with longer duration (28, 29), and VAP was the most common nosocomial infection in this study. According to the autopsy results for COVID-19 (30), SARS-CoV-2 seldom infiltrates the lungs with lymphocytes, which is different from influenza virus pneumonia. SARS-CoV-2 invades the lungs, hearts, kidneys, and other organs, while immune organs, such as the spleen, show “desolation.” Immunological status should be considered when selecting candidates for ECMO. The incidence of nosocomial infection was above the normal level because of damage to the immune function of the patients and inadequate prevention due to the state of the COVID-19 outbreak. Therefore, intensification of airway management and reasonable management of catheters, such as deep vein catheters, are of vital importance.
The incidence of hemorrhage and oxygenator thrombus was high, which suggested that some problems existed in our anticoagulation management and organ supportive treatment of ECMO (31). Thus, coagulation tests, such as the activated clotting time (ACT) or APTT, should be regularly monitored to avoid large fluctuations, and invasive operations, such as tracheotomy, should be performed in the early stage of ECMO to prevent fatal factors, such as intratracheal massive hemorrhage.
In addition to the “lung protective ventilation strategy” (32), patients with severe COVID-19-related ARDS are often given higher PEEP (33) and placed in the prone position (34). The effects of lung recruitment and titrated PEEP are still unclear in patients with pulmonary endogenous ARDS caused by pneumonia (35). During ECMO support, the “lung rest strategy” was mainly used (36, 37) due to the high clinical workload and constrained environment. An individual patient data meta-analysis of observational studies in ventilated patients with ARDS receiving ECMO for refractory hypoxemia showed that the driving pressure during ECMO was the only ventilator setting that showed an independent association with in-hospital mortality (38). Unfortunately, some specific information from the ICU was missing, and many patients did not have driving pressure measurements. There were four pneumothorax patients during ECMO support. Perhaps due to the special respiratory mechanics of patients with COVID-19, the main findings were low respiratory system compliance and poor reactivity to recruitment maneuvers with high PEEP in a single-center observational study (39). Therefore, the optimal ventilation strategy is still unclear.
This study has several limitations. First, only 31 ECMO patients were included in this study. All ECMO patients cared for in the ICU of three hospitals who met the inclusion criteria were included. With the increased number of patients with COVID-19, we hope that these findings presented here will promote a larger cohort study or potentially some randomized controlled trials. Second, the data collected were only from the ICUs of three hospitals, which may not reflect the treatment of severe ECMO patients in the whole region of Wuhan, thereby resulting in the data selection bias. Third, this is a retrospective study, and the number of subjects was too small to perform a multiple regression analysis to identify the risk factors for unsuccessful weaning from ECMO. Therefore, further studies are still needed.
Extracorporeal membrane oxygenation is effective at improving oxygenation and ventilation of patients with severe ARDS related to COVID-19, and early application successfully improves weaning and increases survival compared with the delayed initiation of ECMO. As the duration of ECMO in successfully weaned patients was prolonged, it was necessary to prevent and control complications, such as nosocomial infection and hemorrhage, to generate appropriate conditions for lung recovery.
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
The study was approved by Jinyintan Hospital ethics board. Informed consent was waived since we collected and analyzed all data from the patients according to the policy for public health outbreak investigation of emerging infectious diseases issued by the National Health Commission of the People's Republic of China.
XL, MH, RZ, HQ, BD, and ZT: conception, design, and administrative support. XL, MH, RZ, LJ, MZ, LS, XZ, CP, WZ, HQ, BD, and ZT: provision of study materials or patients. XL, YW, HK, LJ, MZ, LS, XZ, CP, and WZ: collection and assembly of data. XL, MH, RZ, YW, and HK: data analysis and interpretation. All authors manuscript writing and final approval of manuscript.
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
We thank all the doctors, nurses, and clinical scientists who worked in the hospital during the period of patient recruitment as well as all the patients and their families who were involved in the study.
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fmed.2021.716086/full#supplementary-material
ECMO, extracorporeal membrane oxygenation; COVID-19, coronavirus disease 2019; IMV, invasive mechanical ventilation; SARS-CoV, severe acute respiratory syndrome coronavirus; MERS-CoV, Middle East respiratory syndrome coronavirus; RNA, ribonucleic acid; ARDS, acute respiratory distress syndrome; H1N1, influenza A; H7N9, avian influenza A; VV-ECMO, veno-venous ECMO; WHO, World Health Organization; ICU, intensive care unit; HFNC, high-flow nasal cannula oxygen therapy; NIV, non-invasive ventilation; PaO2, partial pressure of arterial oxygen; FiO2, fraction of inspired oxygen; SD, standard deviation; IQR, interquartile range; ANOVA, analysis of variance; APACHE II, Acute Physiology and Chronic Health Evaluation; SOFA, Sequential Organ Failure Assessment; MV, mechanical ventilation; MAP, mean arterial blood pressure; Vt, tidal volume; PEEP, positive end expiratory pressure; CO2, carbon dioxide; TBIL, total bilirubin; APTT, activated partial thromboplastin time; FIB, fibrinogen; CRRT, continuous renal replacement therapy; VAP, ventilation associated pneumonia; CRBSI, catheter related blood stream infection; IPA, invasive pulmonary aspergillosis; PaCO2, partial pressure of arterial carbon dioxide; ELSO, Extracorporeal Life Support Organization; ACT, activated clotting time.
1. Munster VJ, Koopmans M, van Doremalen N, van Riel D, de Wit E. A novel coronavirus emerging in china - key questions for impact assessment. N Engl J Med. (2020) 382:692–4. doi: 10.1056/NEJMp2000929
2. Cui J, Li F, Shi ZL. Origin and evolution of pathogenic coronaviruses. Nat Rev Microbiol. (2019) 17:181–92. doi: 10.1038/s41579-018-0118-9
3. Wu F, Zhao S, Yu B, Chen YM, Wang W, Song ZG, et al. A new coronavirus associated with human respiratory disease in China. Nature. (2020) 579:265–9. doi: 10.1038/s41586-020-2008-3
4. Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, et al. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med. (2020) 382:727–33. doi: 10.1056/NEJMoa2001017
5. Yang X, Yu Y, Xu J, Shu H, Xia J, Liu H, et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med. (2020) 8:475–81. doi: 10.1016/S2213-2600(20)30079-5
6. Wang Y, Lu X, Li Y, Chen H, Chen T, Su N, et al. Clinical course and outcomes of 344 intensive care patients with COVID-19. Am J Respir Crit Care Med. (2020) 201:1430–4. doi: 10.1164/rccm.202003-0736LE
7. Combes A, Hajage D, Capellier G, Demoule A, Lavoue S, Guervilly C, et al. Extracorporeal membrane oxygenation for severe acute respiratory distress syndrome. N Engl J Med. (2018) 378:1965–75. doi: 10.1056/NEJMoa1800385
8. Australia New Zealand Extracorporeal Membrane Oxygenation Influenza I, Davies A, Jones D, Bailey M, Beca J, et al. Extracorporeal membrane oxygenation for 2009 influenza A(H1N1) acute respiratory distress syndrome. JAMA. (2009) 302:1888–95. doi: 10.1001/jama.2009.1535
9. Huang L, Zhang W, Yang Y, Wu W, Lu W, Xue H, et al. Application of extracorporeal membrane oxygenation in patients with severe acute respiratory distress syndrome induced by avian influenza A (H7N9) viral pneumonia: national data from the Chinese multicentre collaboration. BMC Infect Dis. (2018) 18:23. doi: 10.1186/s12879-017-2903-x
10. Alshahrani MS, Sindi A, Alshamsi F, Al-Omari A, El Tahan M, Alahmadi B, et al. Extracorporeal membrane oxygenation for severe middle east respiratory syndrome coronavirus. Ann Intensive Care. (2018) 8:3. doi: 10.1186/s13613-017-0350-x
11. Ramanathan K, Antognini D, Combes A, Paden M, Zakhary B, Ogino M, et al. Planning and provision of ECMO services for severe ARDS during the COVID-19 pandemic and other outbreaks of emerging infectious diseases. Lancet Respir Med. (2020) 8:518–26. doi: 10.1016/S2213-2600(20)30121-1
12. Yang X, Cai S, Luo Y, Zhu F, Hu M, Zhao Y, et al. Extracorporeal membrane oxygenation for coronavirus disease 2019-induced acute respiratory distress syndrome: a multicenter descriptive study. Crit Care Med. (2020) 48:1289–95. doi: 10.1097/CCM.0000000000004447
13. Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. (2020) 385:1054–62. doi: 10.1016/S0140-6736(20)30566-3
14. Barbaro RP, MacLaren G, Boonstra PS, Iwashyna TJ, Slutsky AS, Fan E, et al. Extracorporeal membrane oxygenation support in COVID-19: an international cohort study of the extracorporeal life support organization registry. Lancet. (2020) 396:1071–8. doi: 10.1016/S0140-6736(20)32008-0
15. Lebreton G, Schmidt M, Ponnaiah M, Folliguet T, Para M, Guihaire J, et al. Extracorporeal membrane oxygenation network organisation and clinical outcomes during the COVID-19 pandemic in greater Paris, France: a multicentre cohort study. Lancet Respir Med. (2021) 9:851–62. doi: 10.1016/S2213-2600(21)00096-5
16. Rabie AA, Azzam MH, Al-Fares AA, Abdelbary A, Mufti HN, Hassan IF, et al. Implementation of new ECMO centers during the COVID-19 pandemic: experience and results from the middle east and India. Intensive Care Med. (2021) 47:887–95. doi: 10.1007/s00134-021-06451-w
17. Shaefi S, Brenner SK, Gupta S, O'Gara BP, Krajewski ML, Charytan DM, et al. Extracorporeal membrane oxygenation in patients with severe respiratory failure from COVID-19. Intensive Care Med. (2021) 47:208–21. doi: 10.1007/s00134-020-06331-9
18. Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, et al. Acute respiratory distress syndrome: the Berlin definition. JAMA. (2012) 307:2526–33. doi: 10.1001/jama.2012.5669
19. WHO. Clinical Management of Severe Acute Respiratory Infection When Novel Coronavirus (nCoV) Infection is Suspected. Available online at: https://www.who.int/publications-detail/clinical-management-of-severe-acute-respiratory-infection-when-novel-coronavirus-(ncov)-infection-is-suspected (accessed March 23, 2020).
20. Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. (2020) 395:497–506. doi: 10.1016/S0140-6736(20)30183-5
21. Organization TELS. ELSO Guidance Document: ECMO for COVID-19 Patients with Severe Cardiopulmonary Failure. (2020). Available online: https://www.elso.org/Portals/0/Files/pdf/ECMO%20for%20COVID%2019%20Guidance%20Document.Final%2003.24.2020.pdf (accessed March 27, 2020).
22. Brodie D, Slutsky AS, Combes A. Extracorporeal life support for adults with respiratory failure and related indications: a review. JAMA. (2019) 322:557–68. doi: 10.1001/jama.2019.9302
23. Noah MA, Peek GJ, Finney SJ, Griffiths MJ, Harrison DA, Grieve R, et al. Referral to an extracorporeal membrane oxygenation center and mortality among patients with severe 2009 influenza A(H1N1). JAMA. (2011) 306:1659–68. doi: 10.1001/jama.2011.1471
24. Li M, Gu SC, Wu XJ, Xia JG, Zhang Y, Zhan QY. Extracorporeal membrane oxygenation support in 2019 novel coronavirus disease: indications, timing, and implementation. Chin Med J. (2020) 133:1115–7. doi: 10.1097/CM9.0000000000000778
25. Hemmila MR, Rowe SA, Boules TN, Miskulin J, McGillicuddy JW, Schuerer DJ, et al. Extracorporeal life support for severe acute respiratory distress syndrome in adults. Ann Surg. (2004) 240:595–605; discussion 605–7. doi: 10.1097/01.sla.0000141159.90676.2d
26. Kulkarni T, Sharma NS, Diaz-Guzman E. Extracorporeal membrane oxygenation in adults: a practical guide for internists. Cleve Clin J Med. (2016) 83:373–84. doi: 10.3949/ccjm.83a.15021
27. Barbaro RP, Odetola FO, Kidwell KM, Paden ML, Bartlett RH, Davis MM, et al. Association of hospital-level volume of extracorporeal membrane oxygenation cases and mortality. Analysis of the extracorporeal life support organization registry. Am J Respir Crit Care Med. (2015) 191:894–901. doi: 10.1164/rccm.201409-1634OC
28. Franchineau G, Luyt CE, Combes A, Schmidt M. Ventilator-associated pneumonia in extracorporeal membrane oxygenation-assisted patients. Ann Transl Med. (2018) 6:427. doi: 10.21037/atm.2018.10.18
29. MacLaren G, Schlapbach LJ, Aiken AM. Nosocomial infections during extracorporeal membrane oxygenation in neonatal, pediatric, and adult patients: a comprehensive narrative review. Pediatr Crit Care Med. (2020) 21:283–90. doi: 10.1097/PCC.0000000000002190
30. Liu Q, Wang RS, Qu GQ, Wang YY, Liu P, Zhu YZ, et al. Gross examination report of a COVID-19 death autopsy. Fa Yi Xue Za Zhi. (2020) 36:21–3. doi: 10.12116/j.issn.1004-5619.2020.01.005
31. Fang ZA, Navaei AH, Hensch L, Hui SR, Teruya J. Hemostatic management of extracorporeal circuits including cardiopulmonary bypass and extracorporeal membrane oxygenation. Semin Thromb Hemost. (2020) 46:62–72. doi: 10.1055/s-0039-3400273
32. Acute Respiratory Distress Syndrome N, Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT, et al. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. (2000) 342:1301–8. doi: 10.1056/NEJM200005043421801
33. Mercat A, Richard JC, Vielle B, Jaber S, Osman D, Diehl JL, et al. Positive end-expiratory pressure setting in adults with acute lung injury and acute respiratory distress syndrome: a randomized controlled trial. JAMA. (2008) 299:646–55. doi: 10.1001/jama.299.6.646
34. Munshi L, Del Sorbo L, Adhikari NKJ, Hodgson CL, Wunsch H, Meade MO, et al. Prone Position for Acute Respiratory Distress Syndrome. A systematic review and meta-analysis. Ann Am Thorac Soc. (2017) 14:S280–8. doi: 10.1513/AnnalsATS.201704-343OT
35. Writing Group for the Alveolar Recruitment for Acute Respiratory Distress Syndrome Trial I Cavalcanti AB Suzumura EA Laranjeira LN Paisani DM Damiani LP . Effect of lung recruitment and titrated positive end-expiratory pressure (PEEP) vs low PEEP on mortality in patients with acute respiratory distress syndrome: a randomized clinical trial. JAMA. (2017) 318:1335–45. doi: 10.1001/jama.2017.14171
36. ELSO. Guidelines for Adult Respiratory Failure. Available online at: https://www.elso.org/Portals/0/ELSO%20Guidelines%20For%20Adult%20Respiratory%20Failure%201_4.pdf (accessed April 9, 2020).
37. Patel B, Arcaro M, Chatterjee S. Bedside troubleshooting during venovenous extracorporeal membrane oxygenation (ECMO). J Thorac Dis. (2019) 11 (Suppl. 14):S1698–S707. doi: 10.21037/jtd.2019.04.81
38. Serpa Neto A, Schmidt M, Azevedo LC, Bein T, Brochard L, Beutel G, et al. Associations between ventilator settings during extracorporeal membrane oxygenation for refractory hypoxemia and outcome in patients with acute respiratory distress syndrome: a pooled individual patient data analysis : mechanical ventilation during ECMO. Intensive Care Med. (2016) 42:1672–84. doi: 10.1007/s00134-016-4507-0
Keywords: coronavirus disease 2019, respiratory failure, acute respiratory distress syndrome, extracorporeal membrane oxygenation, outcome
Citation: Li X, Hu M, Zheng R, Wang Y, Kang H, Jiang L, Zhong M, Sang L, Zheng X, Pan C, Zhang W, Qiu H, Du B and Tong Z (2021) Delayed Initiation of ECMO Is Associated With Poor Outcomes in Patients With Severe COVID-19: A Multicenter Retrospective Cohort Study. Front. Med. 8:716086. doi: 10.3389/fmed.2021.716086
Received: 11 June 2021; Accepted: 20 August 2021;
Published: 16 September 2021.
Edited by:
Somchai Amornyotin, Mahidol University, ThailandReviewed by:
Laura Borgstedt, Technical University of Munich, GermanyCopyright © 2021 Li, Hu, Zheng, Wang, Kang, Jiang, Zhong, Sang, Zheng, Pan, Zhang, Qiu, Du and Tong. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Zhaohui Tong, dG9uZ3poYW9odWljeUBzaW5hLmNvbQ==; Bin Du, ZHViaW45OEBnbWFpbC5jb20=; Haibo Qiu, aGFpYm9xMjAwMEAxNjMuY29t
†These authors have contributed equally to this work
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.