
95% of researchers rate our articles as excellent or good
Learn more about the work of our research integrity team to safeguard the quality of each article we publish.
Find out more
ORIGINAL RESEARCH article
Front. Cardiovasc. Med. , 13 February 2025
Sec. General Cardiovascular Medicine
Volume 12 - 2025 | https://doi.org/10.3389/fcvm.2025.1476053
This article is part of the Research Topic Immune Cell Dynamics and Biomarkers in Cardiac Surgery-Induced Systemic Inflammatory Response View all 4 articles
Background: A pathological decrease in the serum prealbumin level is closely associated with the severity of various diseases and complications after surgery. Many patients suffer from a systemic inflammatory response and local myocardial ischemia after off-pump coronary artery bypass grafting, which is related to an adverse prognosis. This study aimed to explore the relationship between the serum prealbumin level and early complications following off-pump coronary artery bypass grafting, in addition to its predictive value.
Methods: Data were retrospectively collected on patients undergoing off-pump coronary artery bypass grafting from January 2014 to July 2019. The serum prealbumin level was assessed within 6–12 h after the operation. Patients were classified into two groups: the “normal” level group (≥17 mg/dl) and the “low” level group (<17 mg/dl). Univariate and multivariable analyses were performed to evaluate the predictive value of a low serum prealbumin level.
Results: Of the 1,002 patients, 553 (55.2%) had a low serum prealbumin level. The rate of pulmonary infection in the low group was significantly higher than in the normal group. Univariate analysis and multivariable analysis indicated that a low serum prealbumin level was associated with the increased incidence of postoperative pulmonary infection, pleural effusion, and new-onset atrial fibrillation.
Conclusion: The serum prealbumin level following off-pump coronary artery bypass grafting serves as a crucial predictor for early major postoperative complications, such as pulmonary complications and new-onset atrial fibrillation. Early identification of high-risk patients by assessing serum prealbumin levels, in addition to the timely adjustment of treatment and care strategies, can improve patient prognosis, shorten hospital stays, and reduce healthcare expenses.
It has recently been revealed that in pathological states, such as inflammation and stress, reduced serum prealbumin (PA) levels are closely associated with the severity of several diseases and postoperative complications, and can even serve as a vital indicator for the stratification of surgically critically ill patients (1–6). Therefore, PA is not only a nutritional indicator, but also acts as an independent risk factor in certain pathological states, predicting or even influencing the disease regression. However, in the cardiovascular field, few reports on the relationship between PA levels and disease progression, particularly its role in the postoperative assessment following cardiac surgery, are available.
Therefore, this large-sample, retrospective study aimed to investigate the relationship between the PA level and early-stage complications following off-pump coronary artery bypass grafting (OPCAB), in addition to its predictive value. These findings may help to guide perioperative treatment and promptly adjust care strategies to help patients' postoperative recovery, which has great clinical significance.
Data were collected retrospectively from 1,485 patients who had undergone OPCAB surgery at a single institution between June 2014 and July 2019. The study was approved by the Institutional Review Board of our hospital. The data are anonymous, and the requirement for informed consent was therefore waived.
Inclusion criteria for patients were as follows. (1) Age >18 years old. (2) Isolated first-time OPCAB surgery. (3) Normal liver and kidney function before operation.
The exclusion criteria were as follows: (1) Missing clinical data (n = 87). (2) Poor preoperative clinical status (e.g., hepatic or renal insufficiency, malignancies with low life expectancy, chronic inflammatory disease, active infection, preoperative inotropic agents and/or intra-aortic balloon pump (IABP) requirement, history of cardiopulmonary resuscitation within last 4 weeks) (n = 117). (3) Redo coronary surgery, emergency surgery, and concomitant valve surgery, left ventricular surgery, or other surgical procedures than isolated OPCAB (total n = 279). The remaining 1,002 patients were include in our final analysis (Figure 1).
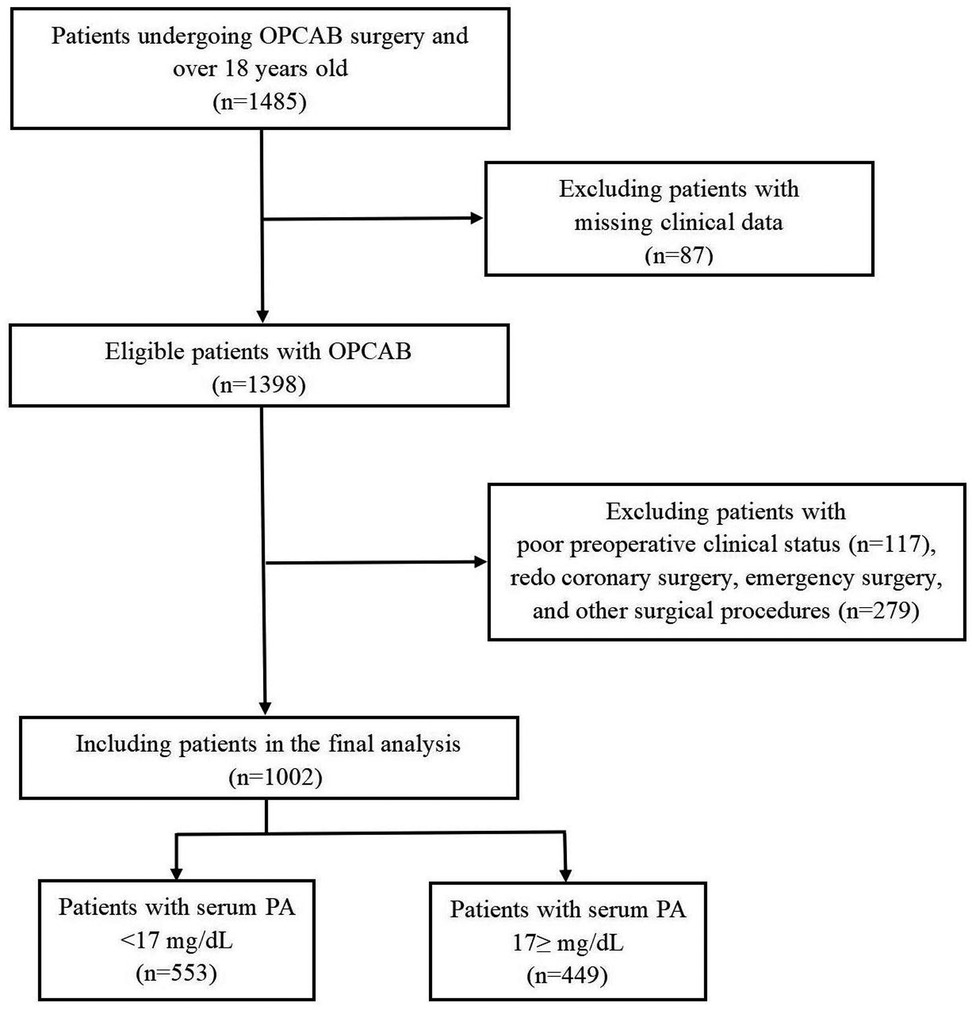
Figure 1. Flowchart depicting patients selection in the study. OPCAB, off-pump coronary artery bypass grafting; PA, prealbumin.
Fasting venous blood samples were collected from all patients within 6–12 h after surgery. Data on the patient's characteristics were collected retrospectively, and preoperative demographics and clinical features, intraoperative data, and postoperative outcomes were all recorded and then analyzed. In the present study, we have used PA 17 mg/dl as the cut-off point, which is the most widely reported value used in the literature (7–10). Accordingly, patients were divided into two groups: serum PA <17 mg/dl (“low” level group) and serum PA ≥17 mg/dl (“normal” level group).
Clinical and procedural data were recorded retrospectively on standardized forms by trained medical personnel. Medical records were reviewed to obtain information regarding patient demographics and comorbidities, operative techniques, postoperative management, complications, and outcomes. The primary outcomes of this study were as follows: extubation time; intensive care unit (ICU) length of stay; postoperative hospital stay; the necessity of inotropic support and IABP; postoperative complications including pulmonary infection, pleural effusion, new-onset atrial fibrillation (AF), hepatic dysfunction, cerebrovascular event (CVE), incision problem, respiratory failure, perioperative myocardial infarction (MI), low left ventricular ejection fraction (LVEF), and acute renal failure (ARF) requiring hemodialysis; and in-hospital mortality.
Pulmonary infection was defined as the presence of purulent sputum associated with fever or requiring antibiotic therapy according to a positive sputum culture. Pleural effusion was defined as middle-to-large pleural effusion confirmed by ultrasound or x-ray. New-onset AF was defined as a new-onset AF during the postoperative hospitalization that required treatment and was diagnosed based on 12-lead ECG findings. Hepatic dysfunction was an elevated postoperative alanine transaminase (ALT) level >100 U/L or an elevated serum bilirubin level >3 mg/dl.
CVE was confirmed by computed tomography and a neurologic consultation. An incision problem was defined as any impaired wound healing, including superficial and deep wound infection. Respiratory failure was defined as the requirement for the continuation of mechanical ventilation beyond 48 h after surgery. A diagnosis of perioperative MI was confirmed by the following events: an elevation in the plasma level of cardiac troponin I (cTnI) >10 times the upper limit of normal in addition to the development of new pathological Q waves or echocardiographic evidence of new-onset regional left ventricular wall motion abnormalities. A low LVEF was defined as <50%. ARF was defined as the requirement for renal replacement therapy after the operation. Hospital mortality was defined as any-cause mortality in the hospital after the surgery.
Preoperative, operative, and postoperative variables were compared between the two groups by adopting different statistical tests. Categorical variables were analyzed using the Chi-square test or Fisher's exact test. For the analyses of normally distributed continuous variables, independent samples t-tests were used. The nonparametric Mann–Whitney test was used for nonnormal data. While continuous variables were expressed as median with interquartile ranges, categorical variables were presented as frequency and percentage for each group. Correlations between continuous variables were determined using Spearman's correlation coefficient.
Univariate logistic regression was used to analyze the prognosis-related factors; those with predictive value were subjected to the multivariate logistic regression analysis. Factors with confounding effects or interactions were excluded to clarify the predictive value of PA. Subsequently, the screened independent predictors were used to plot the receiver operating characteristic (ROC) curves and calculate the area under the curve (AUC). Finally, an AUC comparison between the two groups was performed by the Z-test to evaluate the predictive performance of PA.
All statistical analyses were performed using GraphPad Prism 9.0 (© GraphPad Software, Inc., La Jolla, CA, USA). In addition, the statistical tests were two-sided with a P-value <0.05 considered statistically significant.
Of the 1,002 patients, 553 (55.2%) had a PA level <17 mg/dl. There were no differences in demographics, comorbidities, clinical characteristics, echocardiographic data, and surgical data between the two groups (Table 1). The correlation analysis indicated extremely weak correlations between the postoperative levels of PA and the preoperative levels of albumin (r = 0.117, P = 0.0002) and body mass index (r = 0.0665, P = 0.0352).
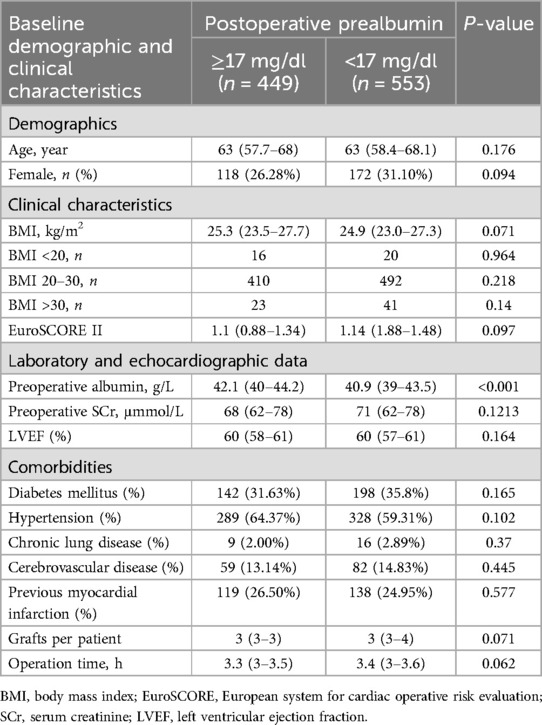
Table 1. Baseline demographic and clinical characteristics between the normal and low postoperative serum prealbumin groups.
In the low-level group, the ICU length of stay, length of postoperative hospital stay, and extubation time were significantly longer, and the proportion of inotropic support, pulmonary infection, pleural effusion, new-onset AF, incision problems, and respiratory failure were higher than those in the normal-level group. However, there was no significant difference between the two groups regarding perioperative MI, hepatic dysfunction, CVE, low LVEF, necessity of IABP, ARF requiring hemodialysis, and in-hospital mortality (Table 2).
The univariate analysis of the postoperative PA levels and postoperative pulmonary infections revealed that low PA levels were associated with an increased incidence of pulmonary infections (P < 0.0001). Other risk factors for pulmonary infections were female sex, concurrent chronic lung disease, older age, longer surgery duration, longer extubation time, higher neutrophil count, and lower albumin level.
Furthermore, we conducted a multivariate logistic regression analysis of the significant factors. The result suggested that a lower preoperative PA level was an independent risk factor for postoperative pulmonary infection [adjusted odds ratio (OR): 1.5, 95% confidence interval (CI): 1.324–1.704, P < 0.0001]. Other independent risk factors included older age, longer operation time, longer extubation time, higher neutrophil count, and lower albumin level (Table 3). According to the ROC curves in Figure 2 and calculations in Table 4, the predictive power of the postoperative PA level was significantly stronger than other variables and decreased PA levels had a greater predictive value for postoperative pulmonary infection.
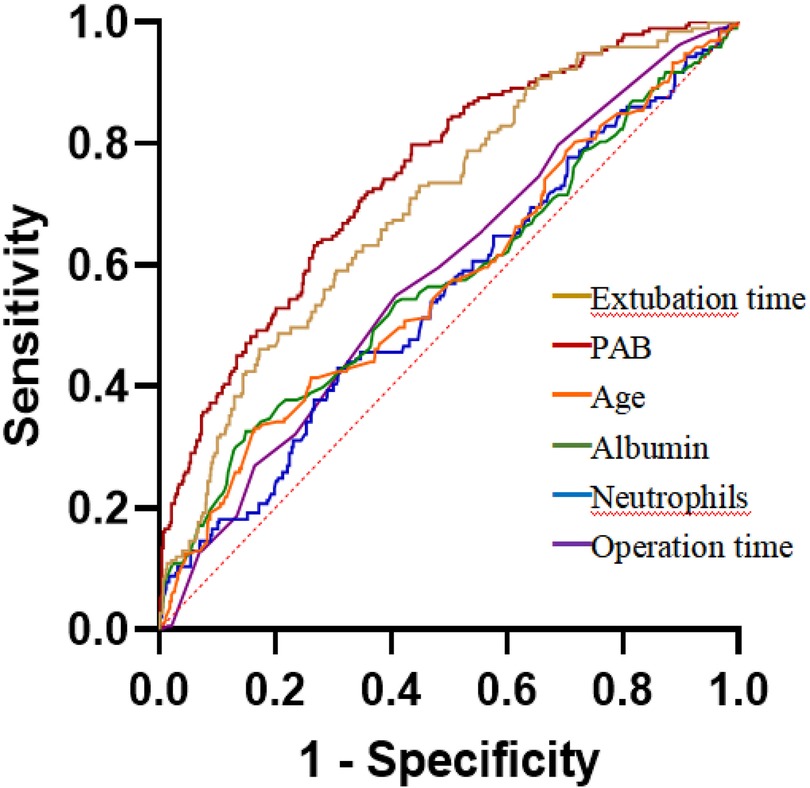
Figure 2. Receiver operating characteristics curves of PA and other variables in predicting postoperative pulmonary infection. The area under the curve of the PA and extubation time is 0.742 (95% CI: 0.704–0.781) and 0.684 (95% CI: 0.648–0.730), respectively (P = 0.043).
The inflammatory response following cardiac surgery is an integrated process that includes endothelial dysfunction, platelet activation, and activation of multiple complementary components. OPCAB avoids the exacerbating factors encountered in cardiopulmonary bypass (CPB); however, in previous studies, patients who underwent OPCAB still exhibited a widespread perioperative inflammatory response in the absence of CPB (11–22), which can influence the clinical outcomes, particularly early complications. Therefore, it is theoretically possible that some rapid-response inflammatory indicators are associated with the early prognosis of OPCAB patients.
PA is a transport protein synthesized by hepatocytes; it is more sensitive than albumin due to its short half-life, rapid renewal, and minimal influence on liver disease and blood product transfusions (23). Phillip et al. (24) induced an inflammatory response in rats by subcutaneous injection of turpentine and reported a faster and more significant decrease in PA than in albumin during the acute phase of inflammation. Recent research also shows that decreased PA levels during periods of the inflammatory response are often not the result of calorie or protein deficiency, but are negatively correlated with inflammatory biomarkers, indicating that they are likely to signal an inflammatory response and poor prognosis (25).
Based on previous studies (1–6), we selected the early postoperative PA level of OPCAB patients as an observation indicator to predict postoperative complications.
As an inflammatory response signal, PA is theoretically predictive of the frequency of postoperative pulmonary injuries. Pulmonary complications after cardiac surgery include atelectasis, pleural effusion, pneumonia, pulmonary edema, acute respiratory distress syndrome, pulmonary embolism, aerothorax, and sternal wound infections. Pulmonary complications are the most prevalent and unavoidable of all postoperative cardiac complications.
This study primarily includes postoperative pulmonary infection, pleural effusion, incision problems, and respiratory failure from any cause. These complications were significantly more prevalent in the low PA group than in the normal group. Pulmonary infection is the most common nosocomial infection in the postoperative period, with a reported incidence of postoperative pneumonia ranging from 6.37% to 35.2% in high-risk groups and a mortality rate of up to 42% at 30 days postoperatively (26, 27). We discovered a statistically significant difference in the incidence of postoperative lung infection in the low PA group. Subsequently, postoperative pulmonary infection was made the study subject, and we introduced numerous potentially significant factors for correction analyses. The results demonstrated that decreased postoperative PA, advanced age, prolonged operative time, prolonged extubation time, elevated postoperative neutrophils, and decreased albumin levels were independent risk factors for postoperative pulmonary infections. Some previously mentioned significant factors, such as gender, diabetes, and comorbid chronic pulmonary diseases, were excluded, probably due to differences in care strategies. Furthermore, due to the limitations of retrospective research, not all influencing factors have been validated (Table 3).
Using ROC curve analysis, we discovered that PA and extubation time had the highest AUCs of 0.742 and 0.684, respectively, with ideal cut-off values of PA <179.5 g/L and extubation time >8.9 h, respectively, while the other predictors are less effective. When compared by the Z-test, PA is the strongest predictor of postoperative pulmonary infection, and we found that by combining PA and extubation time in a ROC curve (AUC = 0.807), the predictive efficacy is further improved, which was significantly higher than the individual index (Table 4, Figure 2). In previous studies, many risk factors for postoperative infectious complications after coronary artery bypass grafting have been identified. The importance of our study is that we have shown, for the first time, that PA is an independent predictor of postoperative pulmonary infection after OPCAB, and its predictive efficacy is significantly higher than other variables, signifying that PA levels <179.5 g/L result in a greater potential for early infection.
AF is one of the most common cardiac arrhythmias after cardiac surgery, and its prevalence is rising with the aging population. Despite advances in anesthesia and surgical techniques, which have reduced the risk of postoperative complications in patients undergoing cardiac surgery, AF remains the most common complication, with a prevalence ranging between 10% and 50%. However, the mechanism for AF after cardiac surgery is uncertain, and inflammation is assumed to be the primary pathophysiology (28–31).
In our study, PA was found to be closely associated with the incidence of new-onset postoperative AF in OPCAB patients as an indicator of inflammation, with a considerably higher incidence of AF in the low PA group than in the normal group (Table 2). However, regression analysis and the ROC curve show that although the PA level is an independent influential factor for new-onset postoperative AF after surgery, the prediction efficacy is not high. Therefore, new-onset postoperative AF after OPCAB may be influenced by a combination of the perioperative inflammatory response and preoperative high-risk factors. Furthermore, the mechanism may be complex, restricting its ability to be predicted by a single factor.
This study has several limitations that are worth noting. First, it is a single center, retrospective, non-randomized controlled study. The acquisition of statistical data has limitations and is unable to obtain all potentially meaningful indicators for the analysis. Therefore, the retrospective nature of this study could have inevitably contained a certain level of selection bias. Second, due to the limitation of the research method, PA was measured after surgery; the blood collection time was within 6–12 h after surgery, not at the same time. As a result, the data lacks certain homogeneity. Third, the division of normal PA and low PA groups is based on the common criteria used in previous studies, which may have some influence on the differential analysis results of some prognosis indicators. Fourth, only short-term studies of prognosis indicators during the postoperative hospitalization period were conducted, with no long-term follow-up; therefore, the impact of changes in the PA level on the medium and long-term prognosis after OPCAB is unclear. Last, on-pump cases means that there will be more influencing factors during the surgical process, so our results may not be fully applicable to on pump cases. As a result, the specific influencing factors and the role of PA may necessitate the accumulation of more cases and further classification studies.
In conclusion, the PA level after OPCAB serves as a crucial predictor for early major postoperative complications, such as pulmonary complications and new-onset AF. The early identification of high-risk patients by PA levels, in addition to the timely adjustment of treatment and care strategies, can improve patient prognosis, shorten the hospital stay, and reduce healthcare expenses. Further studies are needed to better determine the effect of PA on the long-term prognosis of OPCAB patients in the future.
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
The studies involving humans were approved by Medical Ethics Committee of Shandong Provincial Hospital Affiliated to Shandong University. The studies were conducted in accordance with the local legislation and institutional requirements. The participants provided their written informed consent to participate in this study.
YJ: Conceptualization, Data curation, Formal Analysis, Investigation, Methodology, Writing – original draft. JZ: Data curation, Resources, Supervision, Writing – original draft. LC: Investigation, Validation, Visualization, Writing – review & editing.
The author(s) declare financial support was received for the research, authorship, and/or publication of this article. This work was supported by the Natural Science Foundation of Shandong Province, China (Grant No. ZR2023MH289).
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
1. Kudsk KA, Tolley EA, DeWitt RC, Janu PG, Blackwell AP, Yeary S, et al. Preoperative albumin and surgical site identify surgical risk for major postoperative complications. JPEN J Parenter Enteral Nutr. (2003) 27(1):1–9. doi: 10.1177/014860710302700101
2. Huang J, Wang Y, Yuan Y, Chen Y, Kong W, Chen H, et al. Preoperative serum pre-albumin as an independent prognostic indicator in patients with localized upper tract urothelial carcinoma after radical nephroureterectomy. Oncotarget. (2017) 8(22):36772–9. doi: 10.18632/oncotarget.13694
3. Roche M, Law TY, Kurowicki J, Sodhi N, Rosas S, Elson L, et al. Albumin, prealbumin, and transferrin may be predictive of wound complications following total knee arthroplasty. J Knee Surg. (2018) 31(10):946–51. doi: 10.1055/s-0038-1672122
4. Li L, Dai L, Wang X, Wang Y, Zhou L, Chen M, et al. Predictive value of the C-reactive protein-to-prealbumin ratio in medical ICU patients. Biomark Med. (2017) 11(4):329–37. doi: 10.2217/bmm-2016-0266
5. Harriman S, Rodych N, Hayes P, Moser MA. The C-reactive protein-to-prealbumin ratio predicts fistula closure. Am J Surg. (2011) 202(2):175–8. doi: 10.1016/j.amjsurg.2010.06.021
6. Dellière S, Cynober L. Is transthyretin a good marker of nutritional status? Clin Nutr. (2017) 36(2):364–70. doi: 10.1016/j.clnu.2016.06.004
7. Wang W, Wang CS, Ren D, Li T, Yao HC, Ma SJ. Low serum prealbumin levels on admission can independently predict in-hospital adverse cardiac events in patients with acute coronary syndrome. Medicine (Baltimore). (2018) 97(30):e11740. doi: 10.1097/MD.0000000000011740
8. Li JD, Diao YK, Li J, Wu H, Sun LY, Gu WM, et al. Association between preoperative prealbumin level and postoperative mortality and morbidity after hepatic resection for hepatocellular carcinoma: a multicenter study from a HBV-endemic area. Am J Surg. (2021) 221(5):1024–32. doi: 10.1016/j.amjsurg.2020.08.036
9. Devakonda A, George L, Raoof S, Esan A, Saleh A, Bernstein LH. Transthyretin as a marker to predict outcome in critically ill patients. Clin Biochem. (2008) 41(14-15):1126–30. doi: 10.1016/j.clinbiochem.2008.06.016
10. Bonilla-Palomas JL, Gámez-López AL, Anguita-Sánchez MP, Castillo-Domínguez JC, García-Fuertes D, Crespin-Crespin M, et al. Influencia de la desnutrición en la mortalidad a largo plazo de pacientes hospitalizados por insuficiencia cardiaca [impact of malnutrition on long-term mortality in hospitalized patients with heart failure]. Rev Esp Cardiol. (2011) 64(9):752–8. doi: 10.1016/j.recesp.2011.03.009
11. Velioglu Y, Isik M. Early-term outcomes of off-pump versus on-pump beating-heart coronary artery bypass surgery. Thorac Cardiovasc Surg. (2019) 67(7):546–53. doi: 10.1055/s-0039-1679923
12. Li Z, Yeo KK, Parker JP, Mahendra G, Young JN, Amsterdam EA. Off-pump coronary artery bypass graft surgery in California, 2003–2005. Am Heart J. (2008) 156(6):1095–102. doi: 10.1016/j.ahj.2008.07.020
13. Mack MJ, Pfister A, Bachand D, Emery R, Magee MJ, Connolly M, et al. Comparison of coronary bypass surgery with and without cardiopulmonary bypass in patients with multivessel disease. J Thorac Cardiovasc Surg. (2004) 127(1):167–73. doi: 10.1016/j.jtcvs.2003.08.032
14. Puskas JD, Edwards FH, Pappas PA, O'Brien S, Peterson ED, Kilgo P, et al. Off-pump techniques benefit men and women and narrow the disparity in mortality after coronary bypass grafting. Ann Thorac Surg. (2007) 84(5):1447–54; discussion 1454–6. doi: 10.1016/j.athoracsur.2007.06.104
15. Gerola LR, Buffolo E, Jasbik W, Botelho B, Bosco J, Brasil LA, et al. Off-pump versus on-pump myocardial revascularization in low-risk patients with one or two vessel disease: perioperative results in a multicenter randomized controlled trial. Ann Thorac Surg. (2004) 77(2):569–73. doi: 10.1016/S0003-4975(03)01353-5
16. Shroyer AL, Grover FL, Hattler B, Collins JF, McDonald GO, Kozora E, et al. On-pump versus off-pump coronary-artery bypass surgery. N Engl J Med. (2009) 361(19):1827–37. doi: 10.1056/NEJMoa0902905
17. Shroyer AL, Hattler B, Wagner TH, Collins JF, Baltz JH, Quin JA, et al. Five-year outcomes after on-pump and off-pump coronary-artery bypass. N Engl J Med. (2017) 377(7):623–32. doi: 10.1056/NEJMoa1614341
18. Lamy A, Devereaux PJ, Prabhakaran D, Taggart DP, Hu S, Paolasso E, et al. Off-pump or on-pump coronary-artery bypass grafting at 30 days. N Engl J Med. (2012) 366(16):1489–97. doi: 10.1056/NEJMoa1200388
19. Lamy A, Devereaux PJ, Prabhakaran D, Taggart DP, Hu S, Paolasso E, et al. Effects of off-pump and on-pump coronary-artery bypass grafting at 1 year. N Engl J Med. (2013) 368(13):1179–88. doi: 10.1056/NEJMoa1301228
20. Lamy A, Devereaux PJ, Prabhakaran D, Taggart DP, Hu S, Straka Z, et al. Five-year outcomes after off-pump or on-pump coronary-artery bypass grafting. N Engl J Med. (2016) 375(24):2359–68. doi: 10.1056/NEJMoa1601564
21. Wijeysundera DN, Beattie WS, Djaiani G, Rao V, Borger MA, Karkouti K, et al. Off-pump coronary artery surgery for reducing mortality and morbidity: meta-analysis of randomized and observational studies. J Am Coll Cardiol. (2005) 46(5):872–82. doi: 10.1016/j.jacc.2005.05.064
22. Smart NA, Dieberg G, King N. Long-term outcomes of on- versus off-pump coronary artery bypass grafting. J Am Coll Cardiol. (2018) 71(9):983–91. doi: 10.1016/j.jacc.2017.12.049
23. Collins N. The difference between albumin and prealbumin. Adv Skin Wound Care. (2001) 14(5):235–6. doi: 10.1097/00129334-200109000-00009
24. Dickson PW, Howlett GJ, Schreiber G. Metabolism of prealbumin in rats and changes induced by acute inflammation. Eur J Biochem. (1982) 129(2):289–93. doi: 10.1111/j.1432-1033.1982.tb07051.x
25. Yeh DD, Johnson E, Harrison T, Kaafarani HMA, Lee J, Fagenholz P, et al. Serum levels of albumin and prealbumin do not correlate with nutrient delivery in surgical intensive care unit patients. Nutr Clin Pract. (2018) 33(3):419–25. doi: 10.1002/ncp.10087
26. He S, Chen B, Li W, Yan J, Chen L, Wang X, et al. Ventilator-associated pneumonia after cardiac surgery: a meta-analysis and systematic review. J Thorac Cardiovasc Surg. (2014) 148(6):3148–55.e1−5. doi: 10.1016/j.jtcvs.2014.07.107
27. Allou N, Allyn J, Snauwaert A, Welsch C, Lucet JC, Kortbaoui R, et al. Postoperative pneumonia following cardiac surgery in non-ventilated patients versus mechanically ventilated patients: is there any difference? Crit Care. (2015) 19(1):116. doi: 10.1186/s13054-015-0845-5
28. Filardo G, Damiano RJ Jr, Ailawadi G, Thourani VH, Pollock BD, Sass DM, et al. Epidemiology of new-onset atrial fibrillation following coronary artery bypass graft surgery. Heart. (2018) 104(12):985–92. doi: 10.1136/heartjnl-2017-312150
29. Lowres N, Mulcahy G, Jin K, Gallagher R, Neubeck L, Freedman B. Incidence of postoperative atrial fibrillation recurrence in patients discharged in sinus rhythm after cardiac surgery: a systematic review and meta-analysis. Interact Cardiovasc Thorac Surg. (2018) 26(3):504–11. doi: 10.1093/icvts/ivx348
30. Eikelboom R, Sanjanwala R, Le ML, Yamashita MH, Arora RC. Postoperative atrial fibrillation after cardiac surgery: a systematic review and meta-analysis. Ann Thorac Surg. (2021) 111(2):544–54. doi: 10.1016/j.athoracsur.2020.05.104
Keywords: atrial fibrillation, complications, inflammatory response, off-pump coronary artery bypass grafting, prealbumin
Citation: Jia Y, Zhang J, Chen L and Zhu Y (2025) Predictive value of postoperative prealbumin levels for detecting early-stage complications following off-pump coronary artery bypass grafting. Front. Cardiovasc. Med. 12:1476053. doi: 10.3389/fcvm.2025.1476053
Received: 5 August 2024; Accepted: 3 February 2025;
Published: 13 February 2025.
Edited by:
Wataru Takayama, Kawasaki Saiwai Hostpital, JapanReviewed by:
Georgia Damoraki, National and Kapodistrian University of Athens, GreeceCopyright: © 2025 Jia, Zhang, Chen and Zhu. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: Yanhui Zhu, emh1eWFuaHVpQHNwaC5jb20uY24=; MTIzODAzMzM4QHFxLmNvbQ==
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Research integrity at Frontiers

Learn more about the work of our research integrity team to safeguard the quality of each article we publish.